Abstract
Objectives
To reduce the technical challenges of a totally minimally invasive approach (TMA) and to decrease the morbidity associated with open surgery, a hybrid minimally invasive/open approach (HMOA) has been introduced as a surgical technique for rectal cancer. The aim of this study was to compare postoperative results and long-term oncologic outcomes between hybrid minimally invasive/open approach and totally minimally invasive approach in patients who underwent rectal resection for cancer.
Methods
All patients with rectal cancer undergoing a totally minimally invasive approach or hybrid minimally invasive/open approach proctectomy between 2012 and 2016 were analyzed. Preoperative and postoperative outcomes were collected from a prospectively maintained institutional database.
Results
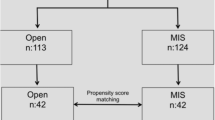
Among 283 patients, 138 (48.8%) underwent a hybrid minimally invasive/open approach and 145 (51.2%) a totally minimally invasive approach. Preoperative characteristics were similar between groups except for distance from the anal verge, which was lower in totally minimally invasive approach group (50.7% vs 29%; p = 0.0008). Length of stay (LOS) was significantly longer in the hybrid minimally invasive/open approach group (6.4 vs 4.3; p = < 0.0001). The median follow-up was 29.6 (14–40.6) months. Overall survival and disease-free survival were not significantly different between groups.
Conclusions
Compared with a hybrid minimally invasive/open approach, a totally minimally invasive approach has a shorter length of stay and may improve short-term outcomes in patients undergoing proctectomy for cancer.


Similar content being viewed by others
References
Heald RJ, Husband EM, Ryall RDH (1982) The mesorectum in rectal cancer surgery—the clue to pelvic recurrence? Br J Surg 69:613–616. https://doi.org/10.1002/bjs.1800691019
Heald RJ, Karanjia ND (1992) Results of radical surgery for rectal cancer. World J Surg 16:848–857
Chessin DB, Enker W, Cohen AM, Paty PB, Weiser MR, Saltz L, Minsky BD, Wong WD, Guillem JG (2005) Complications after preoperative combined modality therapy and radical resection of locally advanced rectal cancer: a 14-year experience from a specialty service. J Am Coll Surg 200:876–882. https://doi.org/10.1016/j.jamcollsurg.2005.02.027
Noel JK, Fahrbach K, Estok R, Cella C, Frame D, Linz H, Cima RR, Dozois EJ, Senagore AJ (2007) Minimally invasive colorectal resection outcomes: short-term comparison with open procedures. J Am Coll Surg 204:291–307
Jayne DG, Thorpe HC, Copeland J, Quirke P, Brown JM, Guillou PJ (2010) Five-year follow-up of the Medical Research Council CLASICC trial of laparoscopically assisted versus open surgery for colorectal cancer. Br J Surg 97:1638–1645. https://doi.org/10.1002/bjs.7160
van der Pas MHGM, Haglind E, Cuesta MA, Fürst A, Lacy AM, Hop WCJ, Bonjer HJ (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14:210–218. https://doi.org/10.1016/S1470-2045(13)70016-0
Bonjer HJ, Deijen CL, Abis GA, Cuesta MA, van der Pas MHGM, de Langedeklerk ESM, Lacy AM, Bemelman WA, Andersson J, Angenete E, Rosenberg J, Fuerst A, Haglind E (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372:1324–1332. https://doi.org/10.1056/NEJMoa1414882
Stevenson ARL, Solomon MJ, Lumley JW, Hewett P, Clouston AD, Gebski VJ, Davies L, Wilson K, Hague W, Simes J (2015) Effect of laparoscopic-assisted resection vs open resection on pathological outcomes in rectal cancer: the ALaCaRT randomized clinical trial. JAMA J Am Med Assoc 314:1356–1363. https://doi.org/10.1001/jama.2015.12009
Fleshman J, Branda M, Sargent DJ, Boller AM, George V, Abbas M, Peters WR, Maun D, Chang G, Herline A, Fichera A, Mutch M, Wexner S, Whiteford M, Marks J, Birnbaum E, Margolin D, Larson D, Marcello P, Posner M, Read T, Monson J, Wren SM, Pisters PWT, Nelson H (2015) Effect of laparoscopic-assisted resection vs open resection of stage II or III rectal cancer on pathologic outcomes the ACOSOG Z6051 randomized clinical trial. JAMA J Am Med Assoc 314:1346–1355. https://doi.org/10.1001/jama.2015.10529
Vithiananthan S, Cooper Z, Betten K, Stapleton GS, Carter J, Huang EH, Whelan RL (2001) Hybrid laparoscopic flexure takedown and open procedure for rectal resection is associated with significantly shorter length of stay than equivalent open resection. Dis Colon Rectum 44:927–935. https://doi.org/10.1007/BF02235478
Guend H, Lee DY, Myers EA, Gandhi ND, Cekic V, Whelan RL (2015) Technique of last resort: characteristics of patients undergoing open surgery in the laparoscopic era. Surg Endosc Other Interv Tech 29:2763–2769. https://doi.org/10.1007/s00464-014-4007-7
Larson DW, Lovely JK, Cima RR, Dozois EJ, Chua H, Wolff BG, Pemberton JH, Devine RR, Huebner M (2014) Outcomes after implementation of a multimodal standard care pathway for laparoscopic colorectal surgery. Br J Surg 101:1023–1030. https://doi.org/10.1002/bjs.9534
Clavien PA, Barkun J, De Oliveira ML, Vauthey JN, Dindo D, Schulick RD, De Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Merchea A, Ali SM, Kelley SR, Duchalais E, Alabbad JY, Dozois EJ, Larson DW (2018) Long-term oncologic outcomes of minimally invasive proctectomy for rectal adenocarcinoma. J Gastrointest Surg:1–6
Trastulli S, Cirocchi R, Listorti C, Cavaliere D, Avenia N, Gulla N, Giustozzi G, Sciannameo F, Noya G, Boselli C (2012) Laparoscopic vs open resection for rectal cancer: a meta-analysis of randomized clinical trials. Color Dis 14:e277–e296. https://doi.org/10.1111/j.1463-1318.2012.02985.x
Trastulli S, Farinella E, Cirocchi R, Cavaliere D, Avenia N, Sciannameo F, Gullà N, Noya G, Boselli C (2012) Robotic resection compared with laparoscopic rectal resection for cancer: systematic review and meta-analysis of short-term outcome. Color Dis 14:e134–e156. https://doi.org/10.1111/j.1463-1318.2011.02907.x
Akiyoshi T, Ueno M, Fukunaga Y, Nagayama S, Fujimoto Y, Konishi T, Kuroyanagi H, Yamaguchi T (2011) Effect of body mass index on short-term outcomes of patients undergoing laparoscopic resection for colorectal cancer: a single institution experience in Japan. Surg Laparosc Endosc Percutan Tech 21:409–414. https://doi.org/10.1097/SLE.0b013e31822e5fdc
Park JW, Lim SW, Choi HS, Jeong SY, Oh JH, Lim SB (2010) The impact of obesity on outcomes of laparoscopic surgery for colorectal cancer in Asians. Surg Endosc 24:1679–1685. https://doi.org/10.1007/s00464-009-0829-0
Baukloh JK, Reeh M, Spinoglio G, Corratti A, Bartolini I, Mirasolo VM, Priora F, Izbicki JR, Gomez Fleitas M, Gomez Ruiz M, Perez DR (2017) Evaluation of the robotic approach concerning pitfalls in rectal surgery. Eur J Surg Oncol 43:1304–1311. https://doi.org/10.1016/j.ejso.2016.12.014
Denost Q, Quintane L, Buscail E, Martenot M, Laurent C, Rullier E (2013) Short- and long-term impact of body mass index on laparoscopic rectal cancer surgery. Color Dis 15:463–469. https://doi.org/10.1111/codi.12026
Karahasanoglu T, Hamzaoglu I, Baca B, Aytac E, Kirbiyik E (2011) Impact of increased body mass index on laparoscopic surgery for rectal cancer. Eur Surg Res Eur Chir Forschung Rech Chir Eur 46:87–93. https://doi.org/10.1159/000321360
Oyasiji T, Baldwin K, Katz SC, Espat NJ, Somasundar P (2012) Feasibility of purely laparoscopic resection of locally advanced rectal cancer in obese patients. World J Surg Oncol 10:147. https://doi.org/10.1186/1477-7819-10-147
Makino T, Trencheva K, Shukla PJ, Rubino F, Zhuo C, Pavoor RS (2014) The influence of obesity on short- and long-term outcomes after laparoscopic surgery for colon cancer: a case-matched study of 152 patients. Surgery (United States) 156:661–668
Gorgun E, Ozben V, Costedio M, Stocchi L, Kalady M, Remzi F (2016) Robotic versus conventional laparoscopic rectal cancer surgery in obese patients. Color Dis 18:1063–1071. https://doi.org/10.1111/codi.13374
Vargas GM, Sieloff EP, Parmar AD, Tamirisa NP, Mehta HB, Riall TS (2016) Laparoscopy decreases complications for obese patients undergoing elective rectal surgery. Surg Endosc Other Interv Tech 30:1826–1832. https://doi.org/10.1007/s00464-015-4463-8
Jiménez Rodríguez RM, Díaz Pavón JM, de La Portilla de Juan F, Prendes Sillero E, Hisnard Cadet Dussort JM, Padillo J (2011) Prospective randomised study: robotic-assisted versus conventional laparoscopic surgery in colorectal cancer resection. Cirugía Española 89:432–438. https://doi.org/10.1016/j.ciresp.2011.01.017
Duchalais E, Machairas N, Kelley SR, Landmann RG, Merchea A, Colibaseanu DT, Mathis KL, Dozois EJ, Larson DW (2018) Does prolonged operative time impact postoperative morbidity in patients undergoing robotic-assisted rectal resection for cancer? Surg Endosc 32:3659–3666. https://doi.org/10.1007/s00464-018-6098-z
Fleshman J, Branda ME, Sargent DJ, Boller AM, George VV, Abbas MA, Peters WRJ, Maun DC, Chang GJ, Herline A, Fichera A, Mutch MG, Wexner SD, Whiteford MH, Marks J, Birnbaum E, Margolin DA, Larson DW, Marcello PW, Posner MC, Read TE, Monson JRT, Wren SM, Pisters PWT, Nelson H (2018) Disease-free survival and local recurrence for laparoscopic resection compared with open resection of stage II to III rectal Cancer: follow-up results of the ACOSOG Z6051 randomized controlled trial. Ann Surg 269:589–595. https://doi.org/10.1097/SLA.0000000000003002
Quiram BJ, Crippa J, Grass F, Lovely JK, Behm KT, Colibaseanu DT, Merchea A, Kelley SR, Harmsen WS, Larson DW (2019) Impact of enhanced recovery on oncological outcomes following minimally invasive surgery for rectal cancer. Br J Surg. https://doi.org/10.1002/bjs.11131
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The Mayo Clinic Review Board approved this study. Mayo Clinic was the sole support for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Deidda, S., Crippa, J., Duchalais, E. et al. Hybrid minimally invasive/open approach versus total minimally invasive approach for rectal cancer resection: short- and long-term results. Int J Colorectal Dis 34, 1251–1258 (2019). https://doi.org/10.1007/s00384-019-03311-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-019-03311-4