Abstract
Introduction
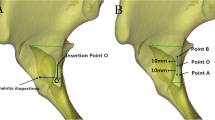
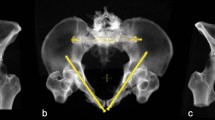
Typical stabilisation of pelvic open book injuries consists of plate fixation of the symphysis. No previous literature has been published about the evaluation of screw placement and their trajectory with four oblique 4.5 mm screws using a four-hole plate in symphysis diastasis. The aim of this study was to define insertion points and angles of trajectory for crossed screw placement regardless of any plate design based on an analysis of three-dimensional computed tomography data sets.
Methods
One hundred human pelvic CT data sets were collected. Unilateral and bilateral placements of crossed 4.5 mm screws were simulated. Primary outcome measure was successful simulated screw placement without cortical breach. Secondary outcome measures included the anatomical measurements of the screw positions.
Results
Simulated screw placement of two oblique screws on each side of the pubic symphysis without cortical breach was achieved in all (100 %) cases. There were a total of 400 screw simulations. Medial screws were longer, lateral screws had higher coronal angles, and the distance between both screws was higher on the right side (p < 0.001 each). The lengths of the right lateral, right medial, left lateral, and left medial screws were 44.9, 65.8, 45.4, and 67.4 mm, respectively. The sagittal angles to the dorsal surface area of the pubic rami were 10.5°, 11.1°, 9.0°, and 11.0°. The coronal angles to the vertical axis of the symphysis measured 39.5°, 16.0°, 33.8°, and 16.8°. The distances between these screws and the medial edge of the pubic crest were 33.5, 8.6, 29.5, and 7.3 mm. Furthermore, certain sex- and side-related differences were noted.
Conclusions
This series provides results about the feasibility and a detailed anatomical description of crossed screw placement. This is of special interest in pelvic surgery for choosing the entry points, safe screw channel parameters, and trajectories.






Similar content being viewed by others
References
Balogh Z, King KL, Mackay P, McDougall D, Mackenzie S, Evans J, Lyons T, Deane S (2007) The epidemiology of pelvic ring fractures: a population-based study. J Trauma 63:1066–1073. doi:10.1097/TA.0b013e3181589fa4
Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: a review. Injury 37:691–697. doi:10.1016/j.injury.2006.04.130
Demetriades D, Karaiskakis M, Toutouzas K, Alo K, Velmahos G, Chan L (2002) Pelvic fractures: epidemiology and predictors of associated abdominal injuries and outcomes. J Am Coll Surg 195:1–10. doi:10.1016/S1072-7515(02)01197-3
Giannoudis P, Grotz M, Tzioupis C, Dinopoulos H, Wells G, Bouamra O, Lecky F (2007) Prevalence of pelvic fractures, associated injuries, and mortality: the United Kingdom perspective. J Trauma 63:875–883. doi:10.1097/01.ta.0000242259.67486.15
Burgess AR, Eastridge BJ, Young JW et al (1990) Pelvic ring disruptions: effective classification systems and treatment protocols. J Trauma 30:022–5282/90/3007–0848
Young J, Burgess A, Brumback R, Poka A (1986) Pelvic fractures: value of plain radiography in early assessment and management. Radiology 160:445–451
Meissner A, Fell M, Wilk R, Boenick U, Rahmanzadeh R (1996) Biomechanics of the pubic symphysis. Which forces lead to mobility of the symphysis in physiological conditions? Unfallchirurg 99:415–421
Walheim G, Selvik G (1984) Mobility of the pubic symphysis. In vivo measurements with an electromechanic method and a roentgen stereophotogrammetric method. Clin Orthop Relat Res. doi:10.1097/00003086-198412000-00016
Barei DP, Bellabarba C, Mills WJ, Routt ML (2001) Percutaneous management of unstable pelvic ring disruptions. Injury 32(Suppl 1):SA33–SA44. doi:10.1016/S0020-1383(01)00059-6
Goldstein A, Phillips T, Sclafani SJ, Scalea T, Duncan A, Goldstein J, Panetta T, Shaftan G (1986) Early open reduction and internal fixation of the disrupted pelvic ring. J Trauma 26:325–333
Latenser BA, Gentilello LM, Tarver AA, Thalgott JS, Batdorf JW (1991) Improved outcome with early fixation of skeletally unstable pelvic fractures. J Trauma 31:28–31. doi:10.1097/00005373-199101000-00006
Matta JM (1996) Indications for anterior fixation of pelvic fractures. Clin Orthop Relat Res. doi:10.1097/00003086-199608000-00011
Tile M (1996) Acute pelvic fractures: II. Principles of management. J Am Acad Orthop Surg 4:152–161
Webb LX, Gristina AG, Wilson JR, Rhyne AL, Meredith JH, Hansen ST (1988) Two-hole plate fixation for traumatic symphysis pubis diastasis. J Trauma 28:813–817. doi:10.1097/00005373-198806000-00016
Simonian PT, Schwappach JR, Routt ML, Agnew SG, Harrington RM, Tencer AF (1996) Evaluation of new plate designs for symphysis pubis internal fixation. J Trauma 41:498–502. doi:10.1097/00005373-199609000-00019
Varga E, Hearn T, Powell J, Tile M (1995) Effects of method of internal fixation of symphyseal disruptions on stability of the pelvic ring. Injury 26:75–80
Wen Y, Liu X, Ge B, Liu Z, Shiji Z (1998) A newer plate system for internal fixation of unstable pelvic fractures. Int Surg 83:88–90
Simonian PT, Routt ML, Harrington RM, Tencer AF (1994) Box plate fixation of the symphysis pubis: biomechanical evaluation of a new technique. J Orthop Trauma 8:483–489. doi:10.1097/00005131-199412000-00005
Hamad A, Pavlou G, Dwyer J, Lim J (2013) Management of pubic symphysis diastasis with locking plates: a report of 11 cases. Injury 44:947–951. doi:10.1016/j.injury.2012.12.018
Moed BR, O’Boynick CP, Bledsoe JG (2014) Locked versus standard unlocked plating of the symphysis pubis in a Type-C pelvic injury: a cadaver biomechanical study. Injury 45:748–751. doi:10.1016/j.injury.2013.11.017
Simonian PT, Routt ML, Harrington RM, Tencer AF (1994) Internal fixation of the unstable anterior pelvic ring: a biomechanical comparison of standard plating techniques and the retrograde medullary superior pubic ramus screw. J Orthop Trauma 8:476–482. doi:10.1097/00005131-199412000-00004
Stuart PR, Talbot D, Milne DD (1990) Internal fixation of pubic symphysis diastasis with a tension banding technique. Injury 21:223–224. doi:10.1016/0020-1383(90)90007-H
Leighton RK, Waddell JP, Bray TJ, Chapman MW, Simpson L, Martin RB, Sharkey NA (1991) Biomechanical testing of new and old fixation devices for vertical shear fractures of the pelvis. J Orthop Trauma 5:313–317. doi:10.1097/00005131-199109000-00010
Oh CW, Kim PT, Kim JW, Min WK, Kyuung HS, Kim SY, Oh SH, Ihn JC (2008) Anterior plating and percutaneous iliosacral screwing in an unstable pelvic ring injury. J Orthop Sci 13:107–115. doi:10.1007/s00776-007-1201-7
Pohlemann T, Gänsslen A (1999) Die Operation der Symphysensprengung. Operative Orthopädie und Traumatologie 59:149–159
Putnis SE, Pearce R, Wali UJ, Bircher MD, Rickman MS (2011) Open reduction and internal fixation of a traumatic diastasis of the pubic symphysis: one-year radiological and functional outcomes. J Bone Joint Surg Br 93:78–84. doi:10.1302/0301-620X.93B1.23941
Giannoudis PV, Chalidis BE, Roberts CS (2008) Internal fixation of traumatic diastasis of pubic symphysis: is plate removal essential? Arch Orthop Trauma Surg 128:325–331. doi:10.1007/s00402-007-0429-1
Routt M, Simonian P (1996) Internal fixation in pelvic fractures and primary repairs of associated genitourinary disruptions: a team approach. J Trauma 40:784–790. doi:10.1097/00005373-199605000-00018
Karadeniz E, Balcik BC, Demirors H, Tuncay IC (2011) Biomechanical comparison of conventional technique versus oblique screw placement in plate fixation. J Trauma 70:E84–E87. doi:10.1097/TA.0b013e318214094d
Kuzhupilly R, Lieberman I, McLain R (2002) In vitro stability of FRA spacers with integrated crossed screws for anterior lumbar interbody fusion. Spine (Phila Pa 1976) 27:923–928. doi:10.1097/00007632-200205010-00007
Nasson S, Shuff C, Palmer D (2001) Biomechanical comparison of ankle arthrodesis techniques: crossed screws vs. blade plate. Foot Ankle Int 22:575–580
Robert K, Chandler R (2003) The effect of divergent screw placement on the initial strength of plate-to-bone fixation. J Trauma 55:1139–1144. doi:10.1097/01.TA.0000031103.15337.CA
Stoffel K, Stachowiak G (2004) Oblique screws at the plate ends increase the fixation strength in synthetic bone test medium. J Orthop Trauma 18:611–616. doi:10.1097/00005131-200410000-00006
Chen L, Zhang G, Song D, Guo X, Yuan W (2012) A comparison of percutaneous reduction and screw fixation versus open reduction and plate fixation of traumatic symphysis pubis diastasis. Arch Orthop Trauma Surg 132:265–270. doi:10.1007/s00402-011-1414-2
Yu K, Hong J, Sun Y, Shi C, Guo X, Zhou D (2014) Anatomical measurement and finite element study on screw channel parameter in percutaneous fixation of canulated screw for symphyseolysis. Cell Biochem Biophys. doi:10.1007/s12013-014-0335-4
Mu W, Wang H (2009) Computer navigated percutaneous screw fixation for traumatic pubic symphysis diastasis of unstable pelvic ring injuries. Chin Med J 122:1699–1703. doi:10.3760/cma.j.issn.0366-6999.2009.14.017
Whiston G (1953) Internal fixation for fractures and dislocations of the pelvis. J Bone Jt Surg Am 53:701–706
Sharp IK (1973) Plate fixation of disrupted symphysis pubis: preliminary report. J Bone Jt Surg Br 55:618–620
Fabian TC, McKinnon WM, Moskowitz MS, Stone HH (1980) Techniques for operative reduction of pubic symphysis disruptions. Surg Gynecol Obstet 151:549–551
Jenkins DH, Young MH (1978) The operative treatment of sacro-iliac subluxation and disruption of the symphysis pubis. Injury 10:139–141. doi:10.1016/S0020-1383(79)80079-0
Culemann U, Scola A, Tosounidis G, Pohlemann T, Gebhard F (2010) Concept for treatment of pelvic ring injuries in elderly patients. A challenge. Unfallchirurg 113:258–271. doi:10.1007/s00113-010-1762-3
Pizanis A, Garcia P, Santelmann M, Culemann U, Pohlemann T (2013) Reduction and fixation capabilities of different plate designs for pubic symphysis disruption: a biomechanical comparison. Injury 44:183–188. doi:10.1016/j.injury.2012.09.023
Rommens PM, Gercek E, Hansen M, Hessmann MH (2003) Mortality, morbidity and functional outcome after open book and lateral compression lesions of the pelvic ring. A retrospective analysis of 100 type B pelvic ring lesions according to Tile’s classification. Unfallchirurg 106:542–549. doi:10.1007/s00113-003-0619-4
Sagi HC, Papp S (2008) Comparative radiographic and clinical outcome of two-hole and multi-hole symphyseal plating. J Orthop Trauma 22:373–378
Jentzsch T, Pietsch CM, Stigler B, Ramseier LE, Seifert B, Werner CML (2015) The compliance with and knowledge about radiation protection in operating room personnel: a cross-sectional study with a questionnaire. Arch Orthop Trauma Surg 135:1233–1240. doi:10.1007/s00402-015-2257-z
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors confirm that there are no financial and personal relationships with any other people or organizations that could inappropriately influence the content or the statements of the submitted article.
Rights and permissions
About this article
Cite this article
Michelitsch, C., Nguyen-Kim, T.D.L., Jentzsch, T. et al. Computed tomography-based three-dimensional visualisation of bone corridors and trajectories for screws in open reduction and internal fixation of symphysis diastasis: a retrospective radiological study. Arch Orthop Trauma Surg 136, 1673–1681 (2016). https://doi.org/10.1007/s00402-016-2568-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-016-2568-8