Abstract
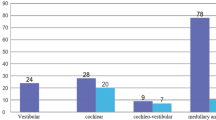
Inner ear decompression sickness (IEDCS) in scuba divers is increasingly observed, but epidemiological data are limited to small case series and the pathogenesis remains elusive. We report our experience over a 13-year period. We also thought to demonstrate that the development of this injury is mainly attributed to a mechanism of vascular origin. Diving information, clinical data, presence of circulatory right-to-left shunt (RLS), and laboratory investigations of 115 recreational divers were retrospectively analyzed. A follow-up study at 3 months was possible with the last 50 consecutive cases. IEDCS (99 males, 44 ± 11 years) represented 24 % of all the patients treated. The median delay of onset of symptoms after surfacing was 20 min. Violation of decompression procedure was recorded in 3 % while repetitive dives were observed in 33 %. The median time to hyperbaric treatment was 180 min. Pure vestibular disorders were observed in 76.5 %, cochlear deficit in 6 % and combination of symptoms in 17.5 %. Additional skin and neurological disorders were reported in 15 % of cases. In 77 %, a large RLS was detected with a preponderant right-sided lateralization of IEDCS (80 %, P < 0.001). Incomplete recovery was found in 68 % of the followed patients. Time to recompression did not seem to influence the clinical outcome. IEDCS is a common presentation of decompression sickness following an uneventful scuba dive, but the therapeutic response remains poor. The high prevalence of RLS combined with a right-sided predominance of inner ear dysfunction suggests a preferential mechanism of paradoxical arterial gas emboli through a vascular anatomical selectivity.

Similar content being viewed by others
References
Vann RD, Butler FK, Mitchell SJ, Moon RE (2011) Decompression illness. Lancet 377:153–164
Smerz RW (2007) A descriptive epidemiological analysis of isolated inner ear decompression illness in recreational divers in Hawaii. Diving Hyperb Med 37:2–9
Edmonds C (2004) Diving and inner ear damage. SPUMS J 34:2–4
Nachum Z, Shupak A, Spitzer O, Sharoni Z, Doweck I, Gordon CR (2001) Inner ear decompression sickness in sport compressed-air diving. Laryngoscope 111:851–856
Cantais E, Louge P, Suppini A, Foster PP, Palmier B (2003) Right-to-left shunt and risk of decompression illness with cochleovestibular and cerebral symptoms in divers: case control study in 101 consecutive dive accidents. Crit Care Med 31:84–88
Money KE, Buckingham IP, Calder IM, Johnson WH, King JD, Landolt JP (1985) Damage to the middle ear and the inner ear in underwater divers. Undersea Biomed Res 12:77–84
Klingmann C, Benton PB, Ringleb PA, Knauth M (2003) Embolic inner ear decompression illness: correlation with right-to-left shunt. Laryngoscope 113:1356–1361
Leverment J, Wolfers D, Kertesz T (2003) Isolated inner ear decompression illness following a nitrogen/oxygen dive: the difficulty in differentiating inner ear decompression illness and inner ear barotrauma. SPUMS J 33:2–5
Reissman P, Shupak A, Nachum Z, Melamed Y (1990) Inner ear decompression sickness following a shallow scuba dive. Aviat Space Environ Med 61:563–566
Wong RM, Walker MB (2004) Diagnostic dilemmas in inner ear decompression illness. SPUMS J 34:5–10
Farmer JC, Thomas WG, Youngblood DG, Bennett PB (1976) Inner ear decompression sickness. Laryngoscope 86:1315–1327
Shupak A, Gil A, Nachum Z, Miller S, Gordon CR, Tal D (2003) Inner ear decompression sickness and inner ear barotraumas in recreational divers: a long-term follow-up. Laryngoscope 113:2141–2147
Klingmann C, Praetorius M, Baumann I, Plinkert PK (2007) Barotrauma and decompression illness of the inner ear: 46 cases during treatment and follow-up. Otol Neurotol 28:447–454
Klingmann C (2012) Inner ear decompression sickness in compressed-air diving. Undersea Hyperb Med 39:589–594
Gempp E, Blatteau JE, Stephant E, Louge P (2009) Relation between right-to-left shunts and spinal cord decompression sickness in divers. Int J Sports Med 30:150–153
Sloan MA, Alexandrov AV, Tegeler CH, Spencer MP, Caplan LR, Feldmann E et al (2004) Assessment: transcranial Doppler ultrasonography: report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 62:1468–1481
Torti SR, Billinger M, Schwerzmann M, Vogel R, Zbinden R, Windecker S et al (2004) Risk of decompression illness among 230 divers in relation to the presence and size of patent foramen ovale. Eur Heart J 25:1014–1020
Kerut EK, Norfleet WT, Plotnick GD, Giles TD (2001) Patent foramen ovale: a review of associated conditions and the impact of physiological size. J Am Coll Cardiol 38:613–623
Mitchell SJ, Doolette DJ (2009) Selective vulnerability of the inner ear to decompression sickness in divers with right-to-left shunt: the role of tissue gas supersaturation. J Appl Physiol 106:298–301
Chuang YM, Chern CM, Liao WH, Hsu LC, Lien CF, Lirng JF et al (2001) Contribution of intracranial vertebral artery asymmetry to vestibular neuropathy. J Neurol Neurosurg Psychiatry 82:823–825
Hayashi Y, Nakau H, Shima H, Tohma Y, Kida S, Yamashita J (2003) Infarction in anterior inferior cerebellar artery territory caused by occlusion of vertebral artery. Clin Radiol Extra 56:57–59
Seidel E, Eicke BM, Tettenborn B, Krummenauer F (1999) Reference values for vertebral artery flow volume by duplex sonography in young and elderly adults. Stroke 30:2692–2696
Yuan RY, Yip PK, Liu HM, Hwang BS, Chen RC (1994) The value of duplex and continuous wave Doppler sonography for evaluation of the extracranial vertebral arteries: a prospective comparison with angiography. Chin Med J 53:42–48
Heckmann JG, Lang CJG, Kindler K, Huk W, Erbguth FJ, Neundorfer B (2000) Neurologic manifestations of cerebral air embolism as a complication of central venous catheterization. Crit Care Med 28:1621–1625
Galion A, Do AH, Chang GY (2010) Lateralized infarction in cerebral air embolism due to patient positioning. J Clin Neurosci 17:943–944
Arfel G, Casanova C, Naquet R, Passelecq J, Dubost C (1967) An electro-clinical study of cerebral gas embolism in cardiac surgery. Electroenceph Clin Neurophysiol 23:101–122
Kendy TK, Arikan OK, Koc C (2005) Volume of components of labyrinth: magnetic resonance imaging study. Otol Neurotol 26:778–781
Droste DW, Reisener M, Kemény V, Dittrich R, Schulte-Altedorneburg G, Stypmann J et al (1999) Contrast transcranial Doppler ultrasound in the detection of right-to-left shunts: reproductibility, comparison of 2 agents and distribution of microemboli. Stroke 30:1014–1018
Horner S, Ni XS, Weihs W, Augustin M, Duft M, Niederkorn K (1997) Simultaneous bilateral contrast transcranial Doppler monitoring in patients with intracardiac and intrapulmonary shunts. J Neurol Sci 150:49–57
Acknowledgments
The authors gratefully acknowledge the medical team of the Otorhinolaryngology department of Sainte Anne’s military hospital (Toulon, France) for conducting the laboratory investigations. Additionally, the authors thank Dr P. Constantin, J.E. Blatteau and J.M. Pontier for their participation to this study.
Conflict of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gempp, E., Louge, P. Inner ear decompression sickness in scuba divers: a review of 115 cases. Eur Arch Otorhinolaryngol 270, 1831–1837 (2013). https://doi.org/10.1007/s00405-012-2233-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-012-2233-y