Abstract
Introduction
Personal protective equipment (PPE) inhibits heat dissipation and elevates heat strain. Impaired cooling with PPE warrants investigation into practical strategies to improve work capacity and mitigate exertional heat illness.
Purpose
Examine physiological and subjective effects of forearm immersion (FC), fan mist (MC), and passive cooling (PC) following three intermittent treadmill bouts while wearing PPE.
Methods
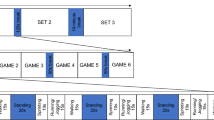
Twelve males (27 ± 6 years; 57.6 ± 6.2 ml/kg/min; 78.3 ± 8.1 kg; 183.1 ± 7.2 cm) performed three 50-min (10 min of 40%, 70%, 40%, 60%, 50% vVO2max) treadmill bouts in the heat (36 °C, 30% relative humidity). Thirty minutes of cooling followed each bout, using one of the three strategies per trial. Rectal temperature (Tcore), skin temperature (Tsk), heart rate (HR), heart rate recovery (HRR), rating of perceived exertion (RPE), thirst, thermal sensation (TS), and fatigue were obtained. Repeated-measures analysis of variance (condition x time) detected differences between interventions.
Results
Final Tcore was similar between trials (P > .05). Cooling rates were larger in FC and MC vs PC following bout one (P < .05). HRR was greatest in FC following bouts two (P = .013) and three (P < .001). Tsk, fluid consumption, and sweat rate were similar between all trials (P > .05). TS and fatigue during bout three were lower in MC, despite similar Tcore and HR.
Conclusion
Utilizing FC and MC during intermittent work in the heat with PPE yields some thermoregulatory and cardiovascular benefit, but military health and safety personnel should explore new and novel strategies to mitigate risk and maximize performance under hot conditions while wearing PPE.




Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
Abbreviations
- ACU:
-
Army combat uniform
- FC:
-
Forearm cooling
- HR:
-
Heart rate
- HRR:
-
Heart rate recovery
- HRV:
-
Heart rate variability
- MC:
-
Fan-mist cooling
- NBC:
-
Nuclear, biological, or chemical
- NBM:
-
Nude body mass
- PC:
-
Passive cooling
- PPE:
-
Personal protective gear
- ANOVA:
-
Analysis of variance
- RPE:
-
Rate of perceived exertion
- SD:
-
Standard deviation
- Tcore :
-
Rectal temperature
- Tsk :
-
Mean skin temperature
- TS:
-
Thermal sensation
- USG:
-
Urine-specific gravity
- VO2max:
-
Maximal volume of oxygen uptake
- VO2peak:
-
Peak value of oxygen uptake
References
Al Haddad H, Laursen PB, Ahmaidi S, Buchheit M (2010) Influence of cold water face immersion on post-exercise parasympathetic reactivation. Eur J Appl Physiol 108(3):599–606. https://doi.org/10.1007/s00421-009-1253-9
Amorim FT, Yamada PM, Robergs RA, Schneider SM (2010) Palm cooling does not reduce heat strain during exercise in a hot, dry environment. Appl Physiol Nutr Metab 35(4):480–489. https://doi.org/10.1139/H10-040
Baker LB (2019) Physiology of sweat gland function: The roles of sweating and sweat composition in human health. Temperature (austin) 6(3):211–259. https://doi.org/10.1080/23328940.2019.1632145
Barr D, Reilly T, Gregson W (2011) The impact of different cooling modalities on the physiological responses in firefighters during strenuous work performed in high environmental temperatures. Eur J Appl Physiol 111(6):959–967. https://doi.org/10.1007/s00421-010-1714-1
Buchheit M, Peiffer JJ, Abbiss CR, Laursen PB (2009) Effect of cold water immersion on postexercise parasympathetic reactivation. Am J Physiol Heart Circ Physiol 296(2):H421-427. https://doi.org/10.1152/ajpheart.01017.2008
Casa DJ, McDermott BP, Lee EC, Yeargin SW, Armstrong LE, Maresh CM (2007) Cold water immersion: the gold standard for exertional heatstroke treatment. Exerc Sport Sci Rev 35(3):141–149. https://doi.org/10.1097/jes.0b013e3180a02bec
Casa DJ, DeMartini JK, Bergeron MF, Csillan D, Eichner ER, Lopez RM, Ferrara MS, Miller KC, O’Connor F, Sawka MN, Yeargin SW (2015) National athletic trainers’ association position statement: exertional heat illnesses. J Athl Train 50(9):986–1000. https://doi.org/10.4085/1062-6050-50.9.07
Chou TH, Akins JD, Crawford CK, Allen JR, Coyle EF (2019) Low stroke volume during exercise with hot skin is due to elevated heart rate. Med Sci Sports Exerc 51(10):2025–2032. https://doi.org/10.1249/MSS.0000000000002029
Cleary MA, Toy MG, Lopez RM (2014) Thermoregulatory, cardiovascular, and perceptual responses to intermittent cooling during exercise in a hot, humid outdoor environment. J Strength Cond Res 28(3):792–806. https://doi.org/10.1519/JSC.0b013e3182a20f57
Coote JH (2010) Recovery of heart rate following intense dynamic exercise. Exp Physiol 95(3):431–440. https://doi.org/10.1113/expphysiol.2009.047548
DeGroot DW, Kenefick RW, Sawka MN (2015) Impact of arm immersion cooling during ranger training on exertional heat illness and treatment costs. Mil Med 180(11):1178–1183. https://doi.org/10.7205/MILMED-D-14-00727
DeMartini JK, Ranalli GF, Casa DJ, Lopez RM, Ganio MS, Stearns RL, McDermott BP, Armstrong LE, Maresh CM (2011) Comparison of body cooling methods on physiological and perceptual measures of mildly hyperthermic athletes. J Strength Cond Res 25(8):2065–2074. https://doi.org/10.1519/JSC.0b013e3182259b1d
Giesbrecht GG, Jamieson C, Cahill F (2007) Cooling hyperthermic firefighters by immersing forearms and hands in 10 degrees C and 20 degrees C water. Aviat Space Environ Med 78(6):561–567
Gonzalez-Alonso J, Calbet JA, Nielsen B (1998) Muscle blood flow is reduced with dehydration during prolonged exercise in humans. J Physiol 513(Pt 3):895–905. https://doi.org/10.1111/j.1469-7793.1998.895ba.x
Grahn DA, Dillon JL, Heller HC (2009) Heat loss through the glabrous skin surfaces of heavily insulated, heat-stressed individuals. J Biomech Eng 131(7):071005
Grahn D, Makam M, Craig Heller H (2018) A method to reduce heat strain while clad in encapsulating outerwear. J Occup Environ Hyg 15(8):573–579. https://doi.org/10.1080/15459624.2018.1470635
Imai K, Sato H, Hori M, Kusuoka H, Ozaki H, Yokoyama H, Takeda H, Inoue M, Kamada T (1994) Vagally mediated heart rate recovery after exercise is accelerated in athletes but blunted in patients with chronic heart failure. J Am Coll Cardiol 24(6):1529–1535. https://doi.org/10.1016/0735-1097(94)90150-3
Kenney WL, Munce TA (2003) Invited review: aging and human temperature regulation. J Appl Physiol (1985) 95(6):2598–2603. https://doi.org/10.1152/japplphysiol.00202.2003
Khomenok GA, Hadid A, Preiss-Bloom O, Yanovich R, Erlich T, Ron-Tal O, Peled A, Epstein Y, Moran DS (2008) Hand immersion in cold water alleviating physiological strain and increasing tolerance to uncompensable heat stress. Eur J Appl Physiol 104(2):303–309. https://doi.org/10.1007/s00421-008-0693-y
Macartney MJ, Meade RD, Notley SR, Herry CL, Seely AJE, Kenny GP (2020) Fluid loss during exercise-heat stress reduces cardiac vagal autonomic modulation. Med Sci Sports Exerc 52(2):362–369. https://doi.org/10.1249/MSS.0000000000002136
Mitchell JB, McFarlin BK, Dugas JP (2003) The effect of pre-exercise cooling on high intensity running performance in the heat. Int J Sports Med 24(2):118–124. https://doi.org/10.1055/s-2003-38203
Morrissey MC, Scarneo-Miller SE, Giersch GEW, Jardine JF, Casa DJ (2021) Assessing the validity of aural thermometry for measuring internal temperature in patients with exertional heat stroke. J Athl Train. https://doi.org/10.4085/1062-6050-0449.19
Nakamura D, Muraishi K, Hasegawa H, Yasumatsu M, Takahashi H (2020) Effect of a cooling strategy combining forearm water immersion and a low dose of ice slurry ingestion on physiological response and subsequent exercise performance in the heat. J Therm Biol 89:102530
Nindl BC, Castellani JW, Warr BJ, Sharp MA, Henning PC, Spiering BA, Scofield DE (2013) Physiological employment standards III: physiological challenges and consequences encountered during international military deployments. Eur J Appl Physiol 113(11):2655–2672. https://doi.org/10.1007/s00421-013-2591-1
Payne S, Macintosh A, Stock J (2018) The thermoregulatory function of the human hand: How do palm and digit proportions affect heat loss? Am J Phys Anthropol 166(4):803–811. https://doi.org/10.1002/ajpa.23469
Perini R, Orizio C, Comande A, Castellano M, Beschi M, Veicsteinas A (1989) Plasma norepinephrine and heart rate dynamics during recovery from submaximal exercise in man. Eur J Appl Physiol Occup Physiol 58(8):879–883. https://doi.org/10.1007/BF02332222
Ranalli GF, Demartini JK, Casa DJ, McDermott BP, Armstrong LE, Maresh CM (2010) Effect of body cooling on subsequent aerobic and anaerobic exercise performance: a systematic review. J Strength Cond Res 24(12):3488–3496. https://doi.org/10.1519/JSC.0b013e3181fb3e15
Rowell LB (1974) Human cardiovascular adjustments to exercise and thermal stress. Physiol Rev 54(1):75–159. https://doi.org/10.1152/physrev.1974.54.1.75
Rowell LB (1990) Hyperthermia: a hyperadrenergic state. Hypertension 15(5):505–507. https://doi.org/10.1161/01.hyp.15.5.505
Sawka MN, Young AJ, Francesconi RP, Muza SR (1985) Pandolf KB (1985) Thermoregulatory and blood responses during exercise at graded hypohydration levels. J Appl Physiol 59(5):1394–1401. https://doi.org/10.1152/jappl.1985.59.5.1394
Sawka MN, Cheuvront SN, Kenefick RW (2012) High skin temperature and hypohydration impair aerobic performance. Exp Physiol 97(3):327–332. https://doi.org/10.1113/expphysiol.2011.061002
Sefton JM, McAdam JS, Pascoe DD, Lohse KR, Banda RL, Henault CB, Cherrington AR, Adams NE (2016) Evaluation of 2 Heat-mitigation methods in army trainees. J Athl Train 51(11):936–945. https://doi.org/10.4085/1062-6050-51.10.13
Selkirk GA, McLellan TM, Wong J (2004) Active versus passive cooling during work in warm environments while wearing firefighting protective clothing. J Occup Environ Hyg 1(8):521–531. https://doi.org/10.1080/15459620490475216
Tokizawa K, Sawada S, Oka T, Yasuda A, Tai T, Ida H, Nakayama K (2014) Fan-precooling effect on heat strain while wearing protective clothing. Int J Biometeorol 58(9):1919–1925. https://doi.org/10.1007/s00484-014-0794-8
Walloe L (2016) Arterio-venous anastomoses in the human skin and their role in temperature control. Temperature (austin) 3(1):92–103. https://doi.org/10.1080/23328940.2015.1088502
Watanabe K, Stohr EJ, Akiyama K, Watanabe S, Gonzalez-Alonso J (2020) Dehydration reduces stroke volume and cardiac output during exercise because of impaired cardiac filling and venous return, not left ventricular function. Physiol Rep 8(11):e14433
Yeargin S, McKenzie AL, Eberman LE, Kingsley JD, Dziedzicki DJ, Yoder P (2016) Physiological and perceived effects of forearm or head cooling during simulated firefighting activity and rehabilitation. J Athl Train 51(11):927–935. https://doi.org/10.4085/1062-6050-51.10.09
Zhang Y, Davis JK, Casa DJ, Bishop PA (2015) Optimizing cold water immersion for exercise-induced hyperthermia: a meta-analysis. Med Sci Sports Exerc 47(11):2464–2472. https://doi.org/10.1249/MSS.0000000000000693
Acknowledgements
We would like to thank the U.S. Army Medical Research and Development Command for funding this study, as well as those who volunteered to participate.
Funding
This study was sponsored by the U.S. Army Medical Research and Development Command under a research contract with The Henry M. Jackson Foundation for the Advancement of Military Medicine, Inc.; Award No.: W81XWH-17–2-0024. The cooling device used for forearm immersion was developed by First Line Technologies (Chantilly, VA, USA) which is a corporate sponsor of the Korey Stringer Institute, where this project was conducted.
Author information
Authors and Affiliations
Contributions
Conceptualization and design: [Margaret C. Morrissey, Ciara N. Manning, Tushar Gulati, Srinivas Laxminarayan, Jaques Reifman, Douglas J. Casa]; Data collection: [Sean P. Langan, Margaret C. Morrissey, Ciara N. Manning]; Data analysis: [Sean P. Langan]; Writing – original draft preparation: [Sean P. Langan]; Writing – review and editing: [Sean P. Langan, Margaret C. Morrissey, Ciara N. Manning, Tushar Gulati, Srinivas Laxminarayan, Jaques Reifman, Douglas J. Casa]; Funding acquisition: [Douglas J. Casa]; Supervision: [Douglas J. Casa]. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The Korey Stringer Institute focuses on exertional heat illnesses and research aimed at maximizing performance, optimizing safety, and preventing sudden death in athletes, warfighters, and laborers.
Ethics approval
This study was approved by the University of Connecticut Institutional Review Board and all procedures were in accordance with the Declaration of Helsinki. This study was also reviewed and approved by the U.S. Army Human Research Protections Office (Fort Detrick, MD).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Communicated by Narihiko kondo.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The opinions or assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army, the U.S. Department of Defense, or The Henry M. Jackson Foundation for the Advancement of Military Medicine, Inc. This paper has been approved for public release with unlimited distribution.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Langan, S.P., Manning, C.N., Morrissey, M.C. et al. Efficacy of two intermittent cooling strategies during prolonged work-rest intervals in the heat with personal protective gear compared with a control condition. Eur J Appl Physiol 123, 1125–1134 (2023). https://doi.org/10.1007/s00421-023-05139-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-023-05139-x