Abstract
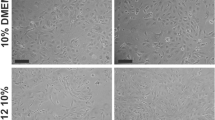
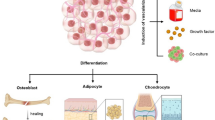
Proliferative or synthetic vascular smooth muscle cells (VSMCs) are widely accepted to be mainly derived from the dedifferentiation or phenotypic modulation of mature contractile VSMCs, i.e., a phenotype switch from a normally quiescent and contractile type into a proliferative or synthetic form. However, this theory has been challenged by recent evidence that synthetic VSMCs predominantly originate instead from media-derived multipotent vascular stem cells (MVSCs). To test these hypotheses further, we re-examine whether the conventional rat aortic SMC (RASMC) culture involves the VSMC differentiation of MVSCs or the dedifferentiation of mature VSMCs and the potential mechanism for controlling the synthetic phenotype of RASMCs. We enzymatically isolated RASMCs and cultured the cells in both a regular growth medium (RGM) and a stem cell growth medium (SCGM). Regardless of culture conditions, only a small portion of freshly isolated RASMCs attaches, survives and grows slowly during the first 7 days of primary culture, while expressing both SMC- and MVSC-specific markers. RGM-cultured cells undergo a process of synthetic SMC differentiation, whereas SCGM-cultured cells can be differentiated into not only synthetic SMCs but also other somatic cells. Notably, compared with the RGM-cultured differentiated RASMCs, the SCGM-cultured undifferentiated cells exhibit the phenotype of MVSCs and generate greater amounts of reactive oxygen species (ROS) that act as a negative regulator of differentiation into synthetic VSMCs. Knockdown of phospholipase A2, group 7 (Pla2g7) suppresses ROS formation in the MVSCs while enhancing SMC differentiation of MVSCs. These results suggest that cultured synthetic VSMCs can be derived from the SMC differentiation of MVSCs with ROS as a negative regulator.







Similar content being viewed by others
References
Atkinson C, Horsley J, Rhind-Tutt S, Charman S, Phillpotts CJ, Wallwork J, Goddard MJ (2004) Neointimal smooth muscle cells in human cardiac allograft coronary artery vasculopathy are of donor origin. J Heart Lung Transplant 23:427–435
Bautch VL (2011) Stem cells and the vasculature. Nat Med 17:1437–1443
Chen Y, Wong MM, Campagnolo P, Simpson R, Winkler B, Margariti A, Hu Y, Xu Q (2013) Adventitial stem cells in vein grafts display multilineage potential that contributes to neointimal formation. Arterioscler Thromb Vasc Biol 33:1844–1851
Ciceri P, Volpi E, Brenna I, Arnaboldi L, Neri L, Brancaccio D, Cozzolino M (2012) Combined effects of ascorbic acid and phosphate on rat VSMC osteoblastic differentiation. Nephrol Dial Transplant 27:122–127
Clempus RE, Sorescu D, Dikalova AE, Pounkova L, Jo P, Sorescu GP, Schmidt HH, Lassegue B, Griendling KK (2007) Nox4 is required for maintenance of the differentiated vascular smooth muscle cell phenotype. Arterioscler Thromb Vasc Biol 27:42–48
Dalle Carbonare L, Innamorati G, Valenti MT (2012) Transcription factor Runx2 and its application to bone tissue engineering. Stem Cell Rev 8:891–897
Dandre F, Owens GK (2004) Platelet-derived growth factor-BB and Ets-1 transcription factor negatively regulate transcription of multiple smooth muscle cell differentiation marker genes. Am J Physiol Heart Circ Physiol 286:H2042–H2051
Daniel JM, Bielenberg W, Stieger P, Weinert S, Tillmanns H, Sedding DG (2010) Time-course analysis on the differentiation of bone marrow-derived progenitor cells into smooth muscle cells during neointima formation. Arterioscler Thromb Vasc Biol 30:1890–1896
Diehn M, Cho RW, Lobo NA, Kalisky T, Dorie MJ, Kulp AN, Qian D, Lam JS, Ailles LE, Wong M, Joshua B, Kaplan MJ, Wapnir I, Dirbas FM, Somlo G, Garberoglio C, Paz B, Shen J, Lau SK, Quake SR, Brown JM, Weissman IL, Clark MF (2009) Association of reactive oxygen species levels and radioresistance in cancer stem cells. Nature 458:780–783
Downs CA, Kumar A, Kreiner LH, Johnson NM, Helms MN (2013) H2O2 regulates lung epithelial sodium channel (ENaC) via ubiquitin-like protein Nedd8. J Biol Chem 288:8136–8145
Dzau VJ, Braun-Dullaeus RC, Sedding DG (2002) Vascular proliferation and atherosclerosis: new perspectives and therapeutic strategies. Nat Med 8:1249–1256
Gomez D, Owens GK (2012) Smooth muscle cell phenotypic switching in atherosclerosis. Cardiovasc Res 95:156–164
Grudzinska MK, Kurzejamska E, Bojakowski K, Soin J, Lehmann MH, Reinecke H, Murry CE, Soderberg-Naucler C, Religa P (2013) Monocyte chemoattractant protein 1-mediated migration of mesenchymal stem cells is a source of intimal hyperplasia. Arterioscler Thromb Vasc Biol 33:1271–1279
Herring BP, Hoggatt AM, Burlak C, Offermanns S (2014) Previously differentiated medial vascular smooth muscle cells contribute to neointima formation following vascular injury. Vasc Cell 6:21
Hu Y, Zhang Z, Torsney E, Afzal AR, Davison F, Metzler B, Xu Q (2004) Abundant progenitor cells in the adventitia contribute to atherosclerosis of vein grafts in ApoE-deficient mice. J Clin Invest 113:1258–1265
Hynes RO (2009) The extracellular matrix: not just pretty fibrils. Science 326:1216–1219
Ito K, Hirao A, Arai F, Takubo K, Matsuoka S, Miyamoto K, Ohmura M, Naka K, Hosokawa K, Ikeda Y, Suda T (2006) Reactive oxygen species act through p38 MAPK to limit the lifespan of hematopoietic stem cells. Nat Med 12:446–451
Jevon M, Ansari TI, Finch J, Zakkar M, Evans PC, Shurey S, Sibbons PD, Hornick P, Haskard DO, Dorling A (2011) Smooth muscle cells in porcine vein graft intimal hyperplasia are derived from the local vessel wall. Cardiovasc Pathol 20:e91–e94
Kennedy E, Hakimjavadi R, Greene C, Mooney CJ, Fitzpatrick E, Collins LE, Loscher CE, Guha S, Morrow D, Redmond EM, Cahill PA (2014) Embryonic rat vascular smooth muscle cells revisited—a model for neonatal, neointimal SMC or differentiated vascular stem cells? Vasc Cell 6:6
Kumar MS, Owens GK (2003) Combinatorial control of smooth muscle-specific gene expression. Arterioscler Thromb Vasc Biol 23:737–747
Lee G, Kim H, Elkabetz Y, Al Shamy G, Panagiotakos G, Barberi T, Tabar V, Studer L (2007) Isolation and directed differentiation of neural crest stem cells derived from human embryonic stem cells. Nat Biotechnol 25:1468–1475
Li J, Ichikawa T, Villacorta L, Janicki JS, Brower GL, Yamamoto M, Cui T (2009) Nrf2 protects against maladaptive cardiac responses to hemodynamic stress. Arterioscler Thromb Vasc Biol 29:1843–1850
Liao XB, Zhang ZY, Yuan K, Liu Y, Feng X, Cui RR, Hu YR, Yuan ZS, Gu L, Li SJ, Mao DA, Lu Q, Zhou XM, Jesus Perez VA de, Yuan LQ (2013) MiR-133a modulates osteogenic differentiation of vascular smooth muscle cells. Endocrinology 154:3344–3352
Libby P, Ridker PM, Hansson GK (2011) Progress and challenges in translating the biology of atherosclerosis. Nature 473:317–325
Lu P, Takai K, Weaver VM, Werb Z (2011) Extracellular matrix degradation and remodeling in development and disease. Cold Spring Harb Perspect Biol 3:pii:a005058
Majesky MW (2007) Developmental basis of vascular smooth muscle diversity. Arterioscler Thromb Vasc Biol 27:1248–1258
Nakahara T, Sato H, Shimizu T, Tanaka T, Matsui H, Kawai-Kowase K, Sato M, Iso T, Arai M, Kurabayashi M (2010) Fibroblast growth factor-2 induces osteogenic differentiation through a Runx2 activation in vascular smooth muscle cells. Biochem Biophys Res Commun 394:243–248
Nguyen AT, Gomez D, Bell RD, Campbell JH, Clowes AW, Gabbiani G, Giachelli CM, Parmacek MS, Raines EW, Rusch NJ, Speer MY, Sturek M, Thyberg J, Towler DA, Weiser-Evans MC, Yan C, Miano JM, Owens GK (2013) Smooth muscle cell plasticity: fact or fiction? Circ Res 112:17–22
Orlandi A, Bennett M (2010) Progenitor cell-derived smooth muscle cells in vascular disease. Biochem Pharmacol 79:1706–1713
Owens GK, Loeb A, Gordon D, Thompson MM (1986) Expression of smooth muscle-specific alpha-isoactin in cultured vascular smooth muscle cells: relationship between growth and cytodifferentiation. J Cell Biol 102:343–352
Owens GK, Kumar MS, Wamhoff BR (2004) Molecular regulation of vascular smooth muscle cell differentiation in development and disease. Physiol Rev 84:767–801
Page-McCaw A, Ewald AJ, Werb Z (2007) Matrix metalloproteinases and the regulation of tissue remodelling. Nat Rev Mol Cell Biol 8:221–233
Pan L, Wang S, Lu T, Weng C, Song X, Park JK, Sun J, Yang ZH, Yu J, Tang H, McKearin DM, Chamovitz DA, Ni J, Xie T (2014) Protein competition switches the function of COP9 from self-renewal to differentiation. Nature 514:233–236
Pauly RR, Passaniti A, Crow M, Kinsella JL, Papadopoulos N, Monticone R, Lakatta EG, Martin GR (1992) Experimental models that mimic the differentiation and dedifferentiation of vascular cells. Circulation 86:III68–III73
Ross JJ, Hong Z, Willenbring B, Zeng L, Isenberg B, Lee EH, Reyes M, Keirstead SA, Weir EK, Tranquillo RT, Verfaillie CM (2006) Cytokine-induced differentiation of multipotent adult progenitor cells into functional smooth muscle cells. J Clin Invest 116:3139–3149
Sainz J, Al Haj Zen A, Caligiuri G, Demerens C, Urbain D, Lemitre M, Lafont A (2006) Isolation of “side population” progenitor cells from healthy arteries of adult mice. Arterioscler Thromb Vasc Biol 26:281–286
Tang Z, Wang A, Yuan F, Yan Z, Liu B, Chu JS, Helms JA, Li S (2012) Differentiation of multipotent vascular stem cells contributes to vascular diseases. Nat Commun 3:875
Tintut Y, Alfonso Z, Saini T, Radcliff K, Watson K, Bostrom K, Demer LL (2003) Multilineage potential of cells from the artery wall. Circulation 108:2505–2510
Torsney E, Xu Q (2011) Resident vascular progenitor cells. J Mol Cell Cardiol 50:304–311
Wu Z, Rosen ED, Brun R, Hauser S, Adelmant G, Troy AE, McKeon C, Darlington GJ, Spiegelman BM (1999) Cross-regulation of C/EBP alpha and PPAR gamma controls the transcriptional pathway of adipogenesis and insulin sensitivity. Mol Cell 3:151–158
Xiao Q, Luo Z, Pepe AE, Margariti A, Zeng L, Xu Q (2009) Embryonic stem cell differentiation into smooth muscle cells is mediated by Nox4-produced H2O2. Am J Physiol Cell Physiol 296:C711–C723
Xiao Q, Pepe AE, Wang G, Luo Z, Zhang L, Zeng L, Zhang Z, Hu Y, Ye S, Xu Q (2012) Nrf3-Pla2g7 interaction plays an essential role in smooth muscle differentiation from stem cells. Arterioscler Thromb Vasc Biol 32:730–744
Acknowledgements
This work was supported by the National Institute of Health (KO1 grant 5KO1DK080884-05), the Shandong University National Qianren Scholar Fund, the Taishan Scholar Fund and the National Natural Science Foundation of China (grant no. 81370267).
Conflicts of Interest
The authors declare that they have no conflicts of interest with biotech companies, financial foundations, or any other third parties and that no competing interests exist. The funders of this project had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Haibo Song and Hui Wang contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Figure S1
Flow cytometry analysis of CD29, CD90 and CD44H expression in RASMCs cultured in RGM over time. The results are representative of three independent experiments (P passage) (GIF 67 kb)
Figure S2
Adipogenic, chondrogenic and osteogenic differentiation of RASMCs cultured in SCGM. P3 RASMCs grown in SCGM were subjected to adipogenic, chondrogenic and osteogenic differentiation by defined factors as indicated. a Adipogenesis. Oil red staining and qPCR analysis of PPARγ2, LPL and C/EBPα. n=4, *P<0.05 vs. control SCGM. b Chondrogenic differentiation. Alcian blue staining and qPCR analysis of aggrecan and OPN. n=4, *P<0.05 vs. control SCGM. c Osteogenic differentiation. Alizarin red staining and qPCR analysis of Runx2 and Alp. n=4, *P<0.05 vs. control SCGM (GIF 215 kb)
Figure S3
Adipocyte, chondrocyte, or osteocyte differentiation potential of RASMCs cultured in SCGM over time. a Experimental flow chart. RASMCs growth in SCGM at various passages were subjected to adipocyte, chondrocyte, or osteocyte differentiation by defined factors as indicated. b Adipogenesis. qPCR analysis of PPARγ2, LPL and C/EBPα. n=4, *P<0.05 vs. control SCGM. c Chondrogenic differentiation. qPCR analysis of aggrecan and OPN. n=4, *P<0.05 vs. control SCGM. d Osteogenic differentiation. qPCR analysis of Runx2 and Alp. n=4, *P<0.05 vs. control SCGM (GIF 58 kb)
Figure S4
Effect of NEDD8 knockdown on SMC differentiation of RASMCs cultured in SCGM. a Experimental flow chart. P2 RASMCs transfected with control (Ctr) interfering RNA (RNAi) and NEDD8 RNAi were cultured in SCGM, RGM, or RGM with PDGF-BB (50 ng/ml) for 7 days and then subjected to the analysis as indicated. b qPCR analysis of NEDD8 gene mRNA expression in P2 RASMCs grown in SCGM, RGM, or RGM with PDGF-BB (50 ng/ml) for 7 days. n=4, *P<0.05 vs. SCGM. c Representative results of NEDD8 protein expression in P2 RASMCs transfected with Ctr siRNA and NEDD8 siRNA and cultured in SCGM for 24 h. d qPCR analysis of SMC gene mRNA expression. n=4, *P<0.05 vs. SCGM. e Western blot analysis of SMC gene protein expression. The results are representative of four separate experiments (GIF 80 kb)
Rights and permissions
About this article
Cite this article
Song, H., Wang, H., Wu, W. et al. Inhibitory role of reactive oxygen species in the differentiation of multipotent vascular stem cells into vascular smooth muscle cells in rats: a novel aspect of traditional culture of rat aortic smooth muscle cells. Cell Tissue Res 362, 97–113 (2015). https://doi.org/10.1007/s00441-015-2193-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-015-2193-9