Abstract
Introduction
The utility of routine upper gastrointestinal (UGI) evaluations after laparoscopic Roux-Y gastric bypass (LRYGB) has yet to be determined, primarily being used to rule out a gastrojejunal leak. Additional information can be assessed with these studies, including the rate of contrast emptying from the pouch; some patients show no or very slow emptying while others show a faster rate of emptying. No or slow emptying is likely due to anastomotic edema and/or a small initial stomal diameter. The aim of this study is to ascertain whether initial pouch emptying (or lack thereof) predicts postoperative weight loss.
Methods
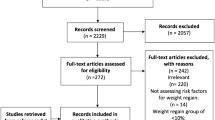
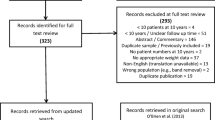
Between August 2002 and July 2006, 405 LRYGB were performed by a single surgeon using a linear stapler technique. Patient demographics were entered into a longitudinal, prospective database. All patients had an UGI study on postoperative day 1. At 1-year follow-up, 304 patients were available for analysis. The patients were divided into two groups: group A, 188 patients with normal gastric emptying, and group B, 116 patients with very slow or no emptying of contrast. Analysis of covariance (ANCOVA) was used to compare weight loss between the two groups. The following covariates were considered in all analyses: age, sex, length of stay, and operative time.
Results
There was a statistically significant difference in weight loss between the two gastric emptying groups adjusting for age, sex, and operative time (p = 0.007). Subjects with prompt gastric emptying (group A) showed more weight loss (50.6 kg versus 47.3 kg) and greater body mass index (BMI) loss (mean loss of 18.1 versus mean loss of 16.6 kg/m2) when compared with group B patients with slow or no emptying of the gastric pouch.
Conclusions
Many factors (psychosocial, behavioral, hormonal, and anatomical) influence weight loss after LRYGB. Although we are uncertain of the mechanism, patients with normal initial pouch emptying tend to lose more weight than patients who initially exhibit slow or no emptying of the gastric pouch.


Similar content being viewed by others
References
Schauer PR, Ikramuddin S (2001) Laparoscopic surgery for morbid obesity. Surg Clin North Am 81:1145–1179
Capella JF, Capella RF (1996) The weight reduction operation of choice: vertical banded gastroplasty or gastric bypass? Am J Surg 171:74–79
Fobi MA, Lee H, Holness R et al (1998) Gastric bypass operation for obesity. World J Surg 22:925–935
Hall JC, Watts JM, O’Brien PE et al (1990) Gastric surgery for morbid obesity. The Adelaide Study. Ann Surg 211:419–427
Nguyen NT, Goldman C, Rosenquist CJ et al (2001) Laparoscopic versus open gastric bypass: a randomized study of outcomes, quality of life, and costs. Ann Surg 234:279–289
Lee S, Carmody B, Wolfe L et al (2007) Effect of location and speed of diagnosis on anastomotic leak outcomes in 3828 gastric bypass cases. J Gastrointest Surg 11(6):708–13
Doraiswamy A, Rasmussen JJ, Pierce J et al (2007) The utility of routine postoperative upper GI series following laparoscopic gastric bypass. Surg Endosc 21:2159–2162
Dixon JB, Pories WJ, O’Brien PE et al (2005) Surgery as an effective early intervention for diabesity: why the reluctance? Diabetes Care 28:472–474
Santry HP, Gillen DL, Lauderdale DS (2005) Trends in bariatric surgical procedures. JAMA 294:1909–1917
Hildebrandt SE (1998) Effects of participation in bariatric support group after Roux-en-Y gastric bypass. Obes Surg 8:535–542
Ma Y, Pagoto SL, Olendzki BC et al (2006) Predictors of weight status following laparoscopic gastric bypass. Obes Surg 16:1227–1231
Elakkary E, Elhorr A, Aziz F et al (2006) Do support groups play a role in weight loss after laparoscopic adjustable gastric banding? Obes Surg 16:331–334
Serafini F, Anderson W, Ghassemi P et al (2002) The utility of contrast studies and drains in the management of patients after Roux-en-Y gastric bypass. Obes Surg 12:34–38
Sims TL, Mullican MA, Hamilton EC et al (2003) Routine upper gastrointestinal Gastrografin swallow after laparoscopic Roux-en-Y gastric bypass. Obes Surg 13:66–72
Toppino M, Cesarani F, Comba A et al (2001) The role of early radiological studies after gastric bariatric surgery. Obes Surg 11:447–454
Raman R, Raman B, Raman P et al (2007) Abnormal findings on routine upper GI series following laparoscopic Roux-en-Y gastric bypass. Obes Surg 17:311–316
Lyass S, Khalili TM, Cunneen S et al (2004) Radiological studies after laparoscopic Roux-en-Y gastric bypass: routine or selective? Am Surg 70:918–921
Singh R, Fisher BL (2003) Sensitivity and specificity of postoperative upper GI series following gastric bypass. Obes Surg 13:73–75
Carter JT, Tafreshian S, Campos GM et al (2007) Routine upper GI series after gastric bypass does not reliably identify anastomotic leaks or predict stricture formation. Surg Endosc 21:2172–2177
Brolin RE (2002) Bariatric surgery and long-term control of morbid obesity. JAMA 288:2793–2796
Buchwald H, Avidor Y, Braunwald E et al (2004) Bariatric surgery: a systematic review and meta-analysis. JAMA 292:1724–1737
Meguid MM, Ramos EJ, Suzuki S et al (2004) A surgical rat model of human Roux-en-Y gastric bypass. J Gastrointest Surg 8:621–630
Xu Y, Ohinata K, Meguid MM et al (2002) Gastric bypass model in the obese rat to study metabolic mechanisms of weight loss. J Surg Res 107:56–63
Pories WJ, Swanson MS, MacDonald KG et al (1995) Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg 222:339–350
Adrian TE, Ferri GL, Bacarese-Hamilton AJ et al (1985) Human distribution and release of a putative new gut hormone, peptide YY. Gastroenterology 89:1070–1077
Savage AP, Adrian TE, Carolan G et al (1987) Effects of peptide YY (PYY) on mouth to caecum intestinal transit time and on the rate of gastric emptying in healthy volunteers. Gut 28:166–170
Batterham RL, Cowley MA, Small CJ et al (2002) Gut hormone PYY(3–36) physiologically inhibits food intake. Nature 418:650–654
Wynne K, Bloom SR (2006) The role of oxyntomodulin and peptide tyrosine-tyrosine (PYY) in appetite control. Nat Clin Pract Endocrinol Metab 2:612–620
Batterham RL, Cohen MA, Ellis SM et al (2003) Inhibition of food intake in obese subjects by peptide YY3–36. N Engl J Med 349:941–948
Le Roux CW, Batterham RL, Aylwin SJ et al (2006) Attenuated peptide YY release in obese subjects is associated with reduced satiety. Endocrinology 147:3–8
Chan JL, Mun EC, Stoyneva V et al (2006) Peptide YY levels are elevated after gastric bypass surgery. Obesity 14:194–198
Korner J, Bessler M, Cirilo LJ et al (2005) Effects of Roux-en-Y gastric bypass surgery on fasting and postprandial concentrations of plasma ghrelin, peptide YY, and insulin. J Clin Endocrinol Metab 90:359–365
Korner J, Inabnet W, Conwell IM et al (2006) Differential effects of gastric bypass and banding on circulating gut hormone and leptin levels. Obesity 14:1553–1561
Morinigo R, Moize V, Musri M et al (2006) Glucagon-like peptide-1, peptide YY, hunger, and satiety after gastric bypass surgery in morbidly obese subjects. J Clin Endocrinol Metab 91:1735–1740
Suzuki S, Ramos E, Concalves C et al (2005) Changes in GI hormones and their effect on gastric emptying and transit times after Roux-en-Y gastric bypass in rat model. Surgery 138(2):283–290
Morinigo R, Vidal J, Lacy AM et al (2008) Circulating peptide YY, weight loss, and glucose homeostasis after gastric bypass surgery in morbidly obese subjects. Ann Surg 247:270–275
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Akkary, E., Sidani, S., Boonsiri, J. et al. The paradox of the pouch: prompt emptying predicts improved weight loss after laparoscopic Roux-Y gastric bypass. Surg Endosc 23, 790–794 (2009). https://doi.org/10.1007/s00464-008-0069-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-008-0069-8