Abstract
Introduction
The Serbian National Training Programme for minimally invasive colorectal surgery (LapSerb) was introduced to implement laparoscopic colorectal surgery across Serbia. The programme aimed to accelerate training of established colorectal surgeons through a competency-based programme. This involved knowledge assessment, workshops, live operating, and competency-based assessment of unedited videos. The aim of this study is to report the outcomes of laparoscopic colorectal resection performed by LapSerb certified surgeons.
Methods
LapSerb prospectively maintained multicentred database was analysed for laparoscopic colorectal resections from January 2015 to February 2021. Data collected included patient demographics, indications for surgery, perioperative data, and 30-day outcomes.
Results
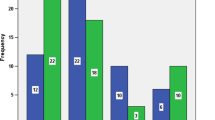
A total of 1456 laparoscopic colectomies by 24 certified surgeons were included in the final analysis. Mean age was 67 (± 12) years old and male to female ratio was 1:1.5. 83.1% of the colectomies were malignant, mainly due to adenocarcinoma. Anterior resection was the most common procedure with 699 (48%) cases, followed by right and left colectomies with 357 (24.5%) and 303 (21%) procedure respectively. 4.8% of patients required conversion to open surgery. Thirty-day readmission and reoperation rates were 2.3% and 4.7%, respectively. Overall mortality in all cases was 1.1% and R0 resections were achieved in 97.8% of malignant colectomies.
Conclusion
The LapSerb programme successfully and safely established laparoscopic colorectal surgery across the country with comparable and acceptable short-term clinical outcomes.
Similar content being viewed by others
References
Nelson H et al (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 350(20):2050–2059
Buunen M et al (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10(1):44–52
Stefanidis D, Heniford BT (2009) The formula for a successful laparoscopic skills curriculum. Arch Surg 144(1):77–82; discussion 82.
Hanna GB et al (2022) Laparoscopic colorectal surgery outcomes improved after National Training Program (LAPCO) for Specialists in England. Ann Surg 275(6):1149–1155
Penna M et al (2016) First international training and assessment consensus workshop on transanal total mesorectal excision (taTME). Tech Coloproctol 20(6):343–352
Miskovic D et al (2013) Is competency assessment at the specialist level achievable? A study for the national training programme in laparoscopic colorectal surgery in England. Ann Surg 257(3):476–482
Mihajlović J et al (2013) Cancer incidence and mortality in Serbia 1999–2009. BMC Cancer 13(1):18
Nikolic A et al (2019) Colorectal cancer surgery in Serbia 2010–2014: evaluation of a multicenter registry. Vojnosanit Pregl 78:80–80
Choy I et al (2013) Barriers to the uptake of laparoscopic surgery in a lower-middle-income country. Surg Endosc 27(11):4009–4015
Heemskerk J et al (2006) Advantages of advanced laparoscopic systems. Surg Endosc 20(5):730–733
Miskovic D et al (2012) Learning curve and case selection in laparoscopic colorectal surgery: systematic review and international multicenter analysis of 4852 cases. Dis Colon Rectum 55(12):1300–1310
Goldwag J et al (2019) The impact of decision aids in patients with colorectal cancer: a systematic review. BMJ Open 9(9):e028379
Ugwumadu L et al (2017) The role of the multidisciplinary team in the management of deep infiltrating endometriosis. Gynecol Surg 14(1):15–15
Jenkins JT et al (2016) A multi-modal approach to training in laparoscopic colorectal surgery accelerates proficiency gain. Surg Endosc 30(7):3007–3013
Acknowledgements
Many thanks and appreciations to LapSerb Collaborative; Pavlov M, Latincic S, Vasiljevic J, Spica B, Gunjic D, Tesic N, Bacevic R, Maric S, Resanovic A, Milev B, Neskovic B, Slavkovic D, Dragovic S, Kenić M, Janic M, Veljanovic O, Maricic A, Stojanovic N, Popovic I, Jovanovic V, Zunjic S, Lazarevic J, Arpad K, Mrksic M, Tamas K, Andras K, Lehel B, Vasic D, Ivanovic P, Stojkovic V, Ivanovic A, Ivanov D, Korica M, Stanojevic M, Tosovic G, Tosovic D, Obucina S, Varnicic V, Golubovic A, Milacević T, Djokovic V, Milosavljevic I, Sutic P, Lazic A, Dabic D, Zarev I, Kosanin Z, Ljubisavljevic R, Kosanovic D, Zaric S, Stojiljkovic M, Zdravkovic R, Petrovic L, Lazarevic M, Djenadic J, Mihajlov V, Ognjenovic A, Popov D, Filko R.
Funding
None to disclose.
Author information
Authors and Affiliations
Contributions
CM and AG equally share the contribution to the first authorship of the manuscript.
Corresponding author
Ethics declarations
Disclosure
Ceranic Miljan, Ahmed Gendia,Masood UR Rehman, Djukanovic Blagoje, Janic Mladen, Krdzic Igor, Stojakovic Nebojsa,Gluhovic Aleksandar, Loncar Zlatibor, Jamil Ahmed, Parvaiz Amjad have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Miljan, C., Gendia, A., Rehman, M.U.R. et al. Serbian National Training Programme for minimally invasive colorectal surgery (LapSerb): short-term clinical outcomes of over 1400 colorectal resections. Surg Endosc 37, 2943–2948 (2023). https://doi.org/10.1007/s00464-022-09795-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09795-6