Abstract
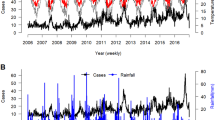
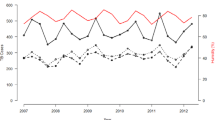
Available evidence is limited on the association between weather factors and childhood pneumonia, especially in developing countries. This study examined the effects of weather variability on childhood pneumonia after the introduction of pneumococcal conjugate vaccines (PCV) intervention in rural Bangladesh. Data on pneumonia cases and weather variables (temperature and relative humidity) between the 1st January 2012 and the 31st December 2016 were collected from Matlab Hospital, International Centre for Diarrhoeal Disease Research, Bangladesh, and Bangladesh Meteorological Department, respectively. Time series cross-correlation functions were applied to identify the time lags of the effect of each weather factor on pneumonia. Generalized linear regression model with Poisson link was used to quantify the association between weather factors and childhood pneumonia after adjustment of PCV intervention. The annual incidence rate of pneumonia reduced from 5691/100,000 to 2000/100,000 after PCV intervention. Generalized linear regression model suggested that temperature had a negative association with childhood pneumonia (relative risk, 0.985; 95% confidence interval (CI), 0.974–0.997), and PCV intervention was a protective factor with the relative risk estimate of 0.489 (95% CI, 0.435–0.551). However, no substantial association was found with relative humidity. PCV intervention appeared protective against childhood pneumonia, and temperature might be associated with this disease in children. Our findings may help inform public health policy, including the potential of development of early warning systems based on weather factors and PCV for the control and prevention of pneumonia in lower middle-income country like Bangladesh.




Similar content being viewed by others
References
Alam N, Chowdhury HR, Ahmed A, Rahman M, Streatfield PK (2014) Distribution of cause of death in rural Bangladesh during 2003-2010: evidence from two rural areas within Matlab health and demographic surveillance site. Glob Health Action 7:25510
Baqui AH, El Arifeen S, Saha SK, Persson L, Zaman K, Gessner BD et al (2007) Effectiveness of Haemophilus influenzae type b conjugate vaccine on prevention of pneumonia and meningitis in Bangladeshi children: a case–control study. Pediatr Infect Dis J 26:565–571
Box GE, Jenkins GM, Reinsel GC, Ljung GM (2015) Time series analysis:forecasting and control. (https://books.google.com.au/books?hl=en&lr=&id=rNt5CgAAQBAJ&oi=fnd&pg=PR7&dq=Time+series+analysis:+forecasting+and+control&ots=DJ73uMoZRB&sig=8eu5VdNL_gdkEoFtpvkaYCmet-o#v=onepage&q=Time series analysis A forecasting and control&f=false)
CDC (2017) Pneumococcal disease. (https://www.cdc.gov/pneumococcal/clinicians/clinical-features.html). Accessed on September 2018
Chowdhury FR, Ibrahim QSU, Bari MS, Alam MMJ, Dunachie SJ, Rodriguez-Morales AJ et al (2018) The association between temperature, rainfall and humidity with common climate-sensitive infectious diseases in Bangladesh. PLoS One 13:e0199579
Cleveland RB, Cleveland WS, McRae JE, Terpenning I (1990) Stl: a seasonal-trend decomposition. J Off Stat 6:3–73
D’Amato M, Molino A, Calabrese G, Cecchi L, Annesi-Maesano I, D’Amato G (2018) The impact of cold on the respiratory tract and its consequences to respiratory health. Clin Transl Allergy 8:20
De Souza A, Fernandes WA, Pavão HG, Lastoria G, Albrez EA (2012) Potential impacts of climate variability on respiratory morbidity in children, infants, and adults. J Brazil J Pulmonol 38:708–715
DeAntonio R, Yarzabal JP, Cruz JP, Schmidt JE, Kleijnen J (2016) Epidemiology of community-acquired pneumonia and implications for vaccination of children living in developing and newly industrialized countries: a systematic literature review. Hum Vaccin Immunother 12:2422–2440
Eccles R (2002) An explanation for the seasonality of acute upper respiratory tract viral infections. Acta Otolaryngol 122:183–191
Fullman N, Yearwood J, Abay SM, Abbafati C, Abd-Allah F, Abdela J et al (2018) Measuring performance on the healthcare access and quality index for 195 countries and territories and selected subnational locations: a systematic analysis from the global burden of disease study 2016. Lancet 391:2236–2271
Glass RI, Becker S, Huq MI, Stoll BJ, Khan M, Merson MH, Lee JV, Black RE (1982) Endemic cholera in rural Bangladesh, 1966–1980. Am J Epidemiol 116:959–970
Guisan A, Edwards TC Jr, Hastie T (2002) Generalized linear and generalized additive models in studies of species distributions: setting the scene. Ecol Model 157:89–100
Harvell CD, Mitchell CE, Ward JR, Altizer S, Dobson AP, Ostfeld RS et al (2002) Climate warming and disease risks for terrestrial and marine biota. Science (New York, NY) 296:2158–2162
Heymann DL (2006) Effects of social, environmental and economic factors on current and future patterns of infectious diseases. Interaction between global change and human health 290–299. (http://www.casinapioiv.va/content/dam/accademia/pdf/sv106/sv106.pdf#page=318). Accessed 18 Jan 2019
icddrb (2016) Health and demographic surveillance system-matlab. (http://dspace.icddrb.org/jspui/handle/123456789/6323). Accessed 04 Mar 2019
Khatun MA (2016) Climate of Bangladesh. (https://www.met.no/publikasjoner/met-report/met.../MET-report-08-2016.pdf). Accessed 12 Feb 2019
Kim J, Kim JH, Cheong HK, Kim H, Honda Y, Ha M et al (2016) Effect of climate factors on the childhood pneumonia in Papua New Guinea: a time-series analysis. Int J Environ Res Public Health 13:1–16
Lin HC, Lin HC, Lin CC, Chen CS (2009) Seasonality of pneumonia admissions and its association with climate: an eight-year nationwide population-based study. Chronobiol Int 26:1647–1659
Liu GY, Wang C, Li W, Lu J, Shen S et al (2015a) Association between temperature change and outpatient visits for respiratory tract infections among children in Guangzhou, China. Int J Environ Res Public Health 12:439–454
Liu L, Oza S, Hogan D, Perin J, Rudan I, Lawn JE, Cousens S, Mathers C, Black RE (2015b) Global, regional, and national causes of child mortality in 2000–13, with projections to inform post-2015 priorities: an updated systematic analysis. Lancet 385:430–440
Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V et al (2013) Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the global burden of disease study 2010. Lancet 380:2095–2128
Mirsaeidi M, Motahari H, Taghizadeh Khamesi M, Sharifi A, Campos M, Schraufnagel DE (2016) Climate change and respiratory infections. Ann Am Thorac Soc 13:1223–1230
Omer SB, Sutanto A, Sarwo H, Linehan M, Djelantik IGG, Mercer D, Moniaga V, Moulton LH, Widjaya A, Muljati P, Gessner BD, Steinhoff MC (2008) Climatic, temporal, and geographic characteristics of respiratory syncytial virus disease in a tropical island population. Epidemiol Infect 136:1319–1327
Onozuka D, Hashizume M, Hagihara A (2009) Impact of weather factors on mycoplasma pneumoniae pneumonia. Thorax 64:507–511
Paynter S, Weinstein P, Ware RS, Lucero MG, Tallo V, Nohynek H et al (2013) Sunshine, rainfall, humidity and child pneumonia in the tropics: time-series analyses. Epidemiol Infect 141:1328–1336
Rolfe MD, Rice CJ, Lucchini S, Pin C, Thompson A, Cameron AD et al (2012) Lag phase is a distinct growth phase that prepares bacteria for exponential growth and involves transient metal accumulation. J Bacteriol 194:686–701
Sultana NK, Saha SK, Al-Emran HM, Modak JK, Sharker MY, El-Arifeen S et al (2013) Impact of introduction of the Haemophilus influenzae type b conjugate vaccine into childhood immunization on meningitis in Bangladeshi infants. J Pediatr 163:S73–S78
Swinnen I, Bernaerts K, Dens EJ, Geeraerd AH, Van Impe J (2004) Predictive modelling of the microbial lag phase: a review. Int J Food Microbiol 94:137–159
Tanaka G, Faruque AS, Luby SP, Malek MA, Glass RI, Parashar UD (2007) Deaths from rotavirus disease in Bangladeshi children: estimates from hospital-based surveillance. Pediatr Infect Dis J 26:1014–1018
Tang JW, Loh TP (2014) Correlations between climate factors and incidence--a contributor to rsv seasonality. Rev Med Virol 24:15–34
Tian DD, Jiang R, Chen XJ, Ye Q (2017) Meteorological factors on the incidence of mp and rsv pneumonia in children. PLoS One 12:e0173409
WHO (2014) Revised who classification and treatment of childhood pneumonia at health facilities–evidence summaries. World Health Organization, Geneva
WHO (2016) Pneumonia.(http://www.who.int/mediacentre/factsheets/fs331/en/). Access on June 2019
Winchell MJ (2013) Mycoplasma pneumoniae–a national public health perspective. Curr Pediatr Rev 9:324–333
Wolf T, Lyne K, Martinez GS, Kendrovski V (2015) The health effects of climate change in the WHO European region. Climate 3:901–936
Xu Z, Hu W, Tong S (2014) Temperature variability and childhood pneumonia: an ecological study. Environ Health 13:51
Acknowledgements
The study was supported by the Queensland University of Technology Postgraduate Research Award and Queensland University of Technology Higher Degree Research International Tuition Fee Sponsorship.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
ESM 1
(DOCX 110 kb)
Rights and permissions
About this article
Cite this article
Hossain, M.Z., Tong, S., Bambrick, H. et al. Weather factors, PCV intervention and childhood pneumonia in rural Bangladesh. Int J Biometeorol 64, 561–569 (2020). https://doi.org/10.1007/s00484-019-01842-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-019-01842-7