Abstract
Purpose
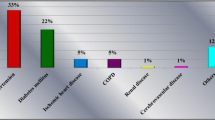
Postoperative wound infection (WI) is a main complication after head and neck surgery. Poor oral health may be a risk factor for WI. We therefore assessed the contribution of oral health care in preventing postoperative WI in patients with oral squamous cell carcinoma (OSCC).
Methods
A total of 66 consecutive inpatients with OSCC (mean age, 68 years) was divided into two groups that did or did not receive oral health care. There were no significant between group differences in gender, age, or T-, N-, or clinical stage. Patients in the care group were given oral health care plans by doctors of oral medicine, whereas patients in the control group were not. Twenty-three variables were recorded for each patient.
Results
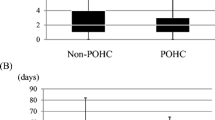
WI was observed in 14/66 patients (21%), three (3/33 = 9%) in the care group and 11 (11/33 = 33%) in the control group (p < 0.025). Univariate statistical analysis showed that 11 factors correlated with WI significantly: T-stage, clinical stage, wearing of dentures, tracheostomy, neck dissection, tissue transplantation, oral health care, preoperative radiation, blood transfusion, operation time, and blood loss. In multiple logistic regression analysis, only two factors were significant independent risk factors for WI: tissue transplantation (p = 0.01; odds ratio, 24.5) and lack of oral health care (p = 0.04; odds ratio, 6.0).
Conclusion
Oral health care may reduce the risk of postoperative WI in patients with OSCC.
Similar content being viewed by others
References
Abe S, Ishihara K, Okuda K (2001) Prevalence of potential respiratory pathogens in the mouths of elderly patients and effects of professional oral care. Arch Gerontol Geriatr 32(1):45–55
Blumberg N, Heal JM (1989) Transfusion and recipient immune function. Arch Pathol Lab Med 113(3):246–253
Brailo V, Vučićević-Boras V, Cekić-Arambašin A, Alajbeg IŽ, Milenović A, Lukač J (2006) The significance of salivary interleukin 6 and tumor necrosis factor alpha in patients with oral leukoplakia. Oral Oncol 42:370–373
Brown BM, Johnson JT, Wagner RL (1987) Etiologic factors in head and neck wound infections. Laryngoscope 97(5):587–590
Coskun H, Erisen L, Basut O (2000) Factors affection wound infection rates in head and neck surgery. Otolaryngol Head Neck Surg 123(3):328–333
de Melo GM, Ribeiro KCB, Kowalski LP, Deheinzelin D (2001) Risk factors for postoperative complications in oral cancer and their prognostic implications. Arch Otolaryngol Head Neck Surg 12(7):828–833
Epstein JB, Emerton S, Le ND, Steveson-Moore P (1999) A double-blind crossover trial of Oral Balance gel and Biotene® toothpaste versus placebo in patients with xerostomia following radiation therapy. Oral Oncol 35:132–137
Grandis JR, Snyderman CH, Johnson JY, Yu VL, D’Amico F (1992) Postoperative wound infection. A poor prognostic sign for patients with head and neck cancer. Cancer 70(8):2166–2170
Johnson JT (1983) Prophylaxis in surgical procedures. Am J Otolaryngol 4(6):433–434
Joyce LD, McQuarrie DG (1976) Applications of contemporary reconstructive techniques in head and neck surgery for anterior oral-facial cancers. Surgery 80(3):373–378
Kowalski LP, Alcantara PSM, Magrin J, Parise Junior O (1994) A case-control study on complications and survival in elderly patients undergoing major head and neck surgery. Am J Surg 168(5):485–490
Matsunaga K, Oobu K, Yoshikawa H, Sasaguri M, Takeda E, Tauchi A, Kawano S, Nagata T, Ohishi M (2002) A clinical study of postoperative infection in oral and maxillofacial surgery. J Jpn Stomatol Soc 51(1):62–68
Ogihara H, Takeuchi K, Yuta A, Majima Y (2005) Analysis of risk factors of postoperative infection in head and neck surgery. J Jpn Soc Infect Dis in Otolaryngol 23(1):116–118
Penel N, Lefebvre D, Fournier C, Sarini J, Kara A, Lefebvre JL (2001) Risk factors for wound infection in head and neck cancer surgery: a prospective study. Head Neck 23(6):447–455
Rhys Evans PH (1989) Complications in head and neck surgery and how to avoid trouble. J Laryngol Otol 103(10):926–929
Seiwert TY, Cohen EEW (2005) State-of-the-art management of locally advanced head and neck cancer. Br J Cancer 92(8):1341–1348
Suzuki K (2004) Prevention of respiratory infections in the elderly. Jpn J Gerodontol 18(4):301–308
Warde P, Kroll B, O’Sullivan B, Aslanidis J, Tew-George E, Waldron J, Maxymiw W, Liu FF, Payne D, Cummings B (2000) A phase II study of Biotene in the treatment of postradiation xerostomia in patients with head and neck cancer. Support Care Cancer 8:203–208
Weber RS, Hankins P, Rosenbaum B, Raad I (1993) Nonwound infections following head and neck oncologic surgery. Laryngoscope 103(1):22–27
World Health Organization (1997) Oral health surveys. Basic methods. Geneva, World Health Organization
Yoneyama K, Yoshida M, Matsui T, Sasaki H, Oral Care Working Group (1999) Oral care and pneumonia. Lancet 354(9177):515
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Additional Table 1
Correlations between the dental status and WI (PPT 94 kb)
Rights and permissions
About this article
Cite this article
Sato, J., Goto, J., Harahashi, A. et al. Oral health care reduces the risk of postoperative surgical site infection in inpatients with oral squamous cell carcinoma. Support Care Cancer 19, 409–416 (2011). https://doi.org/10.1007/s00520-010-0853-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-010-0853-6