Abstract
Purpose
This study aims to determine the influence of significant weight loss on parameters of skeletal muscle function in a population of advanced cancer patients with fatigue.
Methods
A cross-sectional and comparative study was designed between two arms of advanced cancer patients with fatigue (fatigue numeral scale (FNS) ≥4). A arm (n = 27) with ≥5 % weight loss in the last 6 months, and B arm (n = 22) without weight loss. Muscle strength was examined by hand grip technique and measurements of body composition by bioimpedance analysis (BIA), values of hemoglobin, albumin, lactic dehydrogenase (LDH), c-reactive protein (CRP), urine creatinine, and FNS. These variables were compared between both groups and correlated within each group.
Results
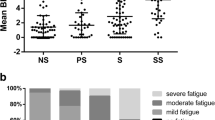
here were no differences concerning parameters of muscle strength between both arms. A arm had values of CRP ≥10 ug/dl in 77 % compared with 38.5 % of B arm (p = 0.004). A arm showed a higher percentage of body cell mass (%BCM) than B arm (p = 0.005). The A arm also showed a lower percentage of fat mass (%FM) (p = 0.014) when compared to the B arm. FNS was higher in A arm (median 7 vs 5; p = 0.047). All the variables of muscle strength had a significant positive correlation. In A arm, BCM had a negative significant correlation with CRP (p = 0.021).
Conclusions
In this study, significant weight loss and high CRP did not have influence on parameters of skeletal muscular function. We consider that further studies should be necessary, preferably with longitudinal designs to evaluate these findings.
Similar content being viewed by others
References
National Comprehensive Cancer Network. Clinical practice guidelines in oncology. Cancer-related fatigue (version 2. 2015) http.//www.nccn.org/professionals physician –gls/pdf/fatigue.pdf. Accessed May 21, 2015.
Partridge A, Jacobsen P, Andersen B (2015) Challenges to standardizing the care for adult cancer survivors: highlighting ASCO’s fatigue and anxiety and depression guidelines. Am Soc Clin Oncol Educ Book: 188-194.
Luthy C, Cedraschi C, Pugliesi A, Di Silvestro K, Mugnier-Konrad B, Rapiti E, Allaz AF (2011) Patients ‘views about causes and preferences for the management of cancer-related fatigue—a case for non congruence with physicians? Support Care Cancer 19:363–370
Dy SM, Lorenz KA, Naem A, Sanati H, Walling A, Asch SM (2008) Evidence-based recommendations for cancer fatigue, anorexia, depression and dyspnea. J Clin Oncol 26:3886–3895
Kisiel-Sajewicz K, Mellar PD, Siemionov V, Sediyova-Khoshknabi D, Wyant A, Walsh D et al (2012) Lack of muscle contractile property changes at the time of perceived physical exhaustion suggests central mechanisms contributing to early motor task failure in cancer-related fatigue. J Pain Symptom Manag 44:351–361
Campos MP, Hassan BJ, Riechelman R, Del Giglio A (2011) Cancer-related fatigue: a practical review. Ann Oncol 22:1273–1279
Capuano G, Pavese I, Satta F, Tosti M, Palladino A, Del Grosso A, Di Palma M (2008) Correlation between anemia, unintentional weight loss and inflammatory status on cancer-related fatigue and quality of life before chemo and radiotherapy. Eur J Clin Nutr Metab 3:147–151
Saligan LN, Olson K, Filler K, Larkin D, Cramp F et al (2015) The biology of cancer-related fatigue: a review of the literature. Support Care Cancer 23:2461–2478
Evans WJ, Morley JE, Argilés J, Bales C, Baracos V et al (2008) Cachexia: a new definition. Clin Nutr 27:793–799
Stasi R, Abriani L, Beccaglia P, Terzoli E, Amadori S (2003) Cancer-related fatigue: evolving concepts in evaluation and treatment. Cancer 98(9):1786–1801
Minton O, Strasser F, Radbruch L, Stone P (2012) Identification of factors associated with fatigue in advanced cancer: a subset analysis of the European palliative care research collaborative computerized symptom assessment date set. J Pain Symptom Manage 43:226–235
Collado-Hidalgo A, Bower JF, Ganz PA, Cole SW, Irwin MR (2006) Inflammatory biomarkers for persistent fatigue in breast cancer survivors. Clin Cancer Res 12:2759–2766
Berger AM, Bruera E, Cimpich B (2010) Recognition and treatment of the symptom of cancer-related fatigue. Am Soc Clin Oncol Educ Book: 350-355
Navigante A, Cresta MP, Casbadien O, López DN, Giglio R, Perman M (2013) Relationship between weakness and phase angle in advanced cancer patients with fatigue. Support Care in Cancer 21(6):1585–1590. doi:10.1007/s00520-012-1774-2
Cerchietti L, Navigante A, Peluffo G, Diament M et al (2004) Effects of celecoxib, medroxyprogesterone, and dietary intervention on systemic syndromes in patients with advanced lung adenocarcinoma: a pilot study. J Pain Symptom Manage 27:85–95
Fearon K, Strasser F, Anker SD, Bosaeus I et al (2011) Definition and classification of cancer cachexia: an international consensus. Lancet Oncol 12:489–503
Kyle UG, Bosaeus I, De Lorenzo AD, Deurenberg P et al (2004) Bioelectrical impedance analysis-part II: utilization in clinical practice. Clin Nutr 23:1430–1453
Beberashvili I, Azar A, Sinuani I, Kadoshi H et al (2014) Longitudinal changes in bioimpedance phase angle reflect inverse changes in serum IL-6 levels in maintenance hemodialysis patients. Nutrition 30:297–304
Hui D, Bansal S, Morgado M, Dev R, Chisholm G, Bruera E (2014) Phase angle for prognostication of survival in patients with advanced cancer: preliminary findings. Cancer 15:2207–2214
Bautmans I, Gorus E, Njemani R, Mets T (2007) Handgrip performance in relation to self perceived-fatigue, physical functioning and circulating IL-6 elderly persons without inflammation. BMC Geriatr 7(5):1–8
Richardson A (1995) Fatigue in cancer patients: a review of the literature. Eur J Cancer Care 4:20–32
Hauser K, Rybicki L, Walsh D (2010) What’s in a name? Word descriptors of cancer-related fatigue. Palliat Med 24(7):724–730
Filler K, Saligan LN (2016) Defining cancer-related fatigue for biomarker discovery. Support Care Cancer 24:5–7
Tisdale MJ (2009) Mechanisms on cancer cachexia. Physiol Rev 89:381–410
Gandevia SC (2001) Spinal and supraspinal factors in human muscle fatigue. Physiol Rev 81(4):1725–1789
Davis MP, Walsh D (2010) Mechanisms of fatigue. J Supp Oncol 8(4):164–174
Jensen GL, Hsiao YP, Wheeler D (2012) Adult nutrition assessment tutorial. JPEN J Parenter Enter Nutr 36:267–274
Scialla SJ, Cole RP, Bednarz L (2006) Redefining cancer-related asthenia-fatigue syndrome. J Palliat Med 5(4):866–872
Fouladiun M, Korner U, Gunnebo L, Sixt-Ammilon P, Bosaeus I, Lundholm K (2007) Daily physical-rest activities in relation to nutritional state, metabolism, and quality of life in cancer patients with progressive cachexia. Clin Cancer Res 13(21):6379–6385
Kyle UG, Bosaeus I, De Lorenzo AD, Deurenberg P et al (2004) Bioelectrical impedance analysis—part I: review of principles and methods. Clin Nutr 23:1226–1243
Argilés JM, Busquets S, Stemmler B, López-Soriano FJ (2014) Cancer cachexia understanding the molecular basis. Nat Rev 14:754–762
Fearon KCH (2011) Cancer cachexia and fat-muscle physiology. N Engl J Med 365(6):565–567
Acknowledgments
The authors thank Lojo, María Laura for the contribution to this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study protocol was approved by the Ethics Committee of the Angel H. Roffo Cancer Institute of the Universidad of Buenos Aires and met the recommendations stated in Helsinki Declaration. All the patients signed an informed consent.
Conflict of interest
None. We do not have any financial relationship with the Institution. We agree to allow the Journal to review this data if requested.
Rights and permissions
About this article
Cite this article
Morgado, P.C., Giorlando, A., Castro, M. et al. Relationship between weight loss and parameters of skeletal muscle function in patients with advanced cancer and fatigue. Support Care Cancer 24, 3961–3966 (2016). https://doi.org/10.1007/s00520-016-3236-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-016-3236-9