Abstract
Introduction
We investigated the continuous infusion rates of rocuronium necessary to obtain the surgical muscle relaxation before, during, and after the Pringle maneuver on patients who underwent hepatectomy.
Methods
Fifteen patients were induced by total intravenous anesthesia with propofol. After obtaining the calibration of acceleromyography, the patient was intubated with rocuronium 0.6 mg/kg. Fifteen minutes after initial rocuronium injection, the continuous infusion was started at 7.5 µg/kg/min. The infusion rate was adjusted every 15 min so that the first twitch height (% T1) might become from 3 to 10% of control. The infusion rates at the time when the state of surgical muscle relaxation was achieved for more than 15 min were recorded before, during and after the Pringle maneuver. The 25% recovery time was measured after discontinuing the continuous infusion.
Results
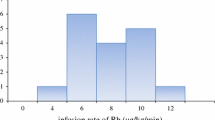
The infusion rate of rocuronium before, during, and after the Pringle maneuver was 7.2 ± 1.8, 4.2 ± 1.4, and 4.7 ± 1.5 µg/kg/min (mean ± SD), respectively. The rocuronium infusion rate during the Pringle maneuver was decreased about 40% compared to that before this maneuver, and that after completion of the Pringle maneuver was not recovered to that before the Pringle maneuver. The 25% recovery time was 20 ± 7 min.
Conclusion
In case of continuous administration of rocuronium during surgery performing the Pringle maneuver, it was considered necessary to regulate the administration of rocuronium using muscle relaxant monitoring in order to deal with the decrease in muscle relaxant requirement by the Pringle maneuver.


Similar content being viewed by others
References
Yamamoto J, Kosuge T, Takayama T, Shimada K, Yamasaki S, Ozaki H, et al. Perioperative blood transfusion promotes recurrence of hepatocellular carcinoma after hepatectomy. Surgery. 1994;115:303–9.
Cata JP, Wang H, Gottumukkala V, Reuben J, Sessler DI. Inflammatory response, immunosuppression, and cancer recurrence after perioperative blood transfusions. Br J Anaesth. 2013;110:690–701.
Luan H, Ye F, Wu L, Zhou Y, Jiang J. Perioperative blood transfusion adversely affects prognosis after resection of lung cancer: a systematic review and a meta-analysis. BMC Surg. 2014;14:34.
Pringle JH. Notes on the arrest of hepatic hemorrhage due to trauma. Ann surg. 1908;48:541–9.
Makuuchi M, Mori T, Gunvén P, Yamazaki S, Hasegawa H. Safety of hemihepatic vascular occlusion during resection of the liver. Surg Gynecol Obstet. 1987;164:155–8.
Wierda JMKH., Kleef UW, Lambalk LM, Kloppenburg WD, Agoston S. The pharmacodynamics and pharmacokinetics of Org 9426; a new non-depolarizing neuromuscular blocking agent, in patients anaesthetized with nitrous oxide, halothane and fentanyl. Can J Anaesth. 1991;38:430–5.
Magorian T, Flannery KB, Miller RD. Comparison of rocuronium, succinylcholine, and vecuronium for rapid sequence induction of anesthesia in adult patients. Anesthesiology. 1993;79:913–8.
McCoy EP, Mirakhur RK, Maddineni VR, Wierda JM, Proost JH. Pharmacokinetics of rocuronium after bolus and continuous infusion during halothane anaesthesia. Br J Anaesth. 1996;76:29–33.
Khuenl-Brady K, Castagnoli KP, Canfell PC, Caldwell JE, Agoston S, Miller RD. The neuromuscular blocking effects and pharmacokinetics of ORG 9426 and ORG 9616 in the cat. Anesthesiology 1990; 72:669–74.
Takagi S, Ozaki M, Iwasaki H, Hatano Y, Takeda J. Effects of sevoflurane and propofol on neuromuscular blocking action of Org 9426 (rocuronium bromide) infused continuously in Japanese patients (in Japanese with English abstract). Masui (Jpn J Anesthesiol) 2006; 55:963–70.
Kajiura A, Nagata O, Takizawa Y, Nakatomi T, Kodera S, Murayama T. A large individual variation in both the infusion rate and the blood concentration of rocuronium necessary for obtain adequate surgical muscle relaxation during total intravenous anesthesia with propofol and remifentanil. J Anesth. 2015;29:9–14.
Gao L, Ramzan I, Baker B. Rocuronium infusion requirements and plasma concentrations at constant levels of neuromuscular paralysis during three phases of liver transplantation. J Clin Anesth 2003; 15:257–66.
Murata F, Iwade M, Hidano G, Tsunoda C, Nagata O, Ozaki M. Recovery from propofol anesthesia is delayed in hepatectomy patients due to altered pharmacodynamics (in Japanese with English abstract). Masui (Jpn J Anesthesiol. 2006;55:150–7.
Funding
This study was funded by departmental funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest.
Additional information
Presented in part at the annual meeting of the 64th Annual Meeting of the Japan Society of Anesthesia, Kobe, Japan, June 2017.
About this article
Cite this article
Kajiura, A., Nagata, O. & Sanui, M. The Pringle maneuver reduces the infusion rate of rocuronium required to maintain surgical muscle relaxation during hepatectomy. J Anesth 32, 409–413 (2018). https://doi.org/10.1007/s00540-018-2498-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-018-2498-4