Abstract
Purpose
There are few prospective studies on surgical outcomes and survival in patients with metastatic disease to the spine. The magnitude and duration of effect of surgery on pain relief and quality of life remains uncertain. Therefore, the aim of this clinical study was to prospectively evaluate clinical, functional, quality of life and survival outcomes after palliative surgery for vertebral metastases.
Methods
118 consecutive patients who underwent spinal surgery for symptomatic vertebral metastases were prospectively followed up for 12 months or until death. Clinical data and data from the European Organization for Research and Treatment of Cancer (EORTC) QLQ-C30 questionnaire were obtained pre- and post-operatively and at regular follow-up intervals.
Results
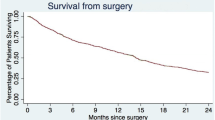
Surgery was effective in achieving rapid improvement in axial and radicular pain, neurological deficit, sphincteric dysfunction and ambulatory status, with a complication rate of 26% and a 12 month mortality rate of 48%. Almost 50% of patients had complete resolution of back pain, radiculopathy and neurological deficit. Of the patients who were non-ambulant and incontinent, over 50% regained ambulatory ability and recovered urinary continence. The overall incidence of wound infection or breakdown was 6.8% and the local recurrence rate was 8.5%. There was a highly significant improvement in physical, role, cognitive and emotional functioning and global health status post-operatively. Greatest improvement in pain, function and overall quality of life occurred in the early post-operative period and was maintained until death or during the 12 month prospective follow-up period.
Conclusion
The potential for immediate and prolonged improvement in pain, function and quality of life in patients with symptomatic vertebral metastases should be considered during the decision-making process when selecting and counselling patients for surgery.





Similar content being viewed by others
References
Harrington K (1993) Metastatic tumors of the spine: diagnosis and treatment. J Am Acad Orthop Surg 1:76–86
Bohm P, Huber J (2002) The surgical treatment of bony metastases of the spine and limbs. J Bone Joint Surg Br 84:521–529
Wong DA, Fornasier VL, MacNab I (1990) Spinal metastases: the obvious, the occult, and the impostors. Spine 15:1–4
Klimo P, Schmidt MH (2004) Surgical management of spinal metastases. Oncologist 9:188–196
Witham TF, Khavkin YA, Gallia GL, Wolinsky JP, Gokaslan ZL (2006) Surgery insight: current management of epidural spinal cord compression from metastatic spine disease. Nat Clin Pract Neurol 2:87–94
Bartels RH, van der Linden YM, van der Graaf WT (2008) Spinal extradural metastasis: review of current treatment options. CA Cancer J Clin 58:245–259
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ (2009) Cancer statistics, 2009. CA Cancer J Clin 59:225–249
Jansson K, Bauer HC (2006) Survival, complications and outcome in 282 patients operated for neurological deficit due to thoracic or lumbar spinal metastases. Eur Spine J 15:196–202
Aebi M (2003) Spinal metastasis in the elderly. Eur Spine J 12:S202–S213
Patchell RA, Tibbs PA, Regine WF, Payne R, Saris S, Hrysio RJ, Mohiuddin M, Young B (2005) Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: a randomized trial. Lancet 66:643–648
Ibrahim A, Crockard A, Antonietti P et al (2008) Does spinal surgery improve the quality of life for those with extradural (spinal) osseous metastases? An international multicenter prospective observational study of 223 patients. J Neurosurg Spine 8:271–278
Tokuhashi Y, Ajiro Y, Umezawa N (2008) Outcome of treatment for spinal metastases using scoring system for preoperative evaluation of prognosis. Spine 34:69–73
Falicov A, Fisher CG, Sparkes J, Boyd MC, Wing PC, Dvorak MF (2006) Impact of surgical intervention on quality of life in patients with spinal metastases. Spine 31:2849–2856
Chi JH, Gokaslan Z, McCormick P, Tibbs PA, Krysio RJ, Patchell RA (2009) Selecting treatment for patients with malignant epidural spinal cord compression—does age matter? Results from a randomized clinical trial. Spine 34:431–435
Vrionis FD, Small J (2003) Surgical management of metastatic spinal neoplasms. Neurosurg Focus 15:1–8
Tokuhashi Y, Matsuzaki H, Toriyama S, Kawano H, Ohsaka S (1990) Scoring system for the preoperative evaluation of metastatic spine tumor prognosis. Spine 15:1110–1113
Tomita K, Kawahara N, Kobayashi T, Yoshida A, Murakami H, Akamaru T (2001) Surgical strategy for spinal metastases. Spine 26:298–306
Tokuhashi Y, Matsuzaki H, Oda H, Oshima M, Ryu J (2005) A revised scoring system for properative evaluation of metastatic spine tumor prognosis. Spine 30:2186–2191
Aaronson NK, Ahmedzai S, Bergman B et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–376
Fayers P, Bottomley A (2002) Quality of life research within the EORTC–the EORTC QLQ-C30. European Organisation for Research and Treatment of Cancer. Eur J Cancer 38:S125–S133
Fayers P, Aaronson NK, Bjordal K, Curran D, Groenvold M (2001) On behalf of the EORTC Quality of Life Study Group. The EORTC QLQ-C30 scoring manual, 3rd edn. European Organisation for Research and Treatment of Cancer, Brussels
Weigel B, Maghsudi M, Neumann C, Kretschmer R, Muller FJ, Nerlich M (1999) Surgical management of symptomatic spinal metastases. Spine 24:2240–2246
Hatrick NC, Lucas JD, Timothy AR, Smith MA (2000) The surgical treatment of metastatic disease of the spine. Rad Onc 56:335–339
Fourney DR, Abi-Said D, Lang FF, McCutcheon IE, Gokaslan ZL (2001) Use of pedicle screw fixation in the management of malignant spinal disease: experience in 100 consecutive procedures. J Neurosurg Sp 94:25–37
Hirabayashi H, Ebara S, Kinoshita T, Yuzawa Y, Nakamura I, Takahashi J, Kamimura M, Ohtsuka K, Takaoka K (2003) Clinical outcome and survival after palliative surgery for spinal metastases. Cancer 97:476–484
Wai EK, Finkelstein JA, Tangente RP, Holden L, Chow E, Ford M, Yee A (2003) Quality of life in surgical treatment of metastatic spine disease. Spine 28:508–512
Holman PJ, Suki D, McCutcheon I, Wolinsky JP, Rhines L, Gokaslan ZL (2005) Surgical management of metastatic disease of the lumbar spine; experience with 139 patients. J Neurosurg Sp 2:550–563
Villavicencio AT, Oskouian RJ, Roberson C, Stokes J, Park J, Shaffrey C, Johnson JP (2005) Thoracolumbar vertebral reconstruction after surgery for metastatic spinal tumors: long-term outcomes. Neurosurg Focus 19:1–8
Kondo T, Hozumi T, Goto T, Seichi A, Nakamura K (2008) Intraoperative radiotherapy combined with posterior decompression and stabilization for non-ambulant paralytic patients due to spinal metastasis. Spine 33:1898–1904
Yamashita T, Aota Y, Kushida K, Murayama H, Hiruma T, Takeyama M, Iwamura Y, Saito T (2008) Changes in physical function after palliative surgery for metastatic spinal tumor: association of the Revised Tokuhashi Score with neurologic recovery. Spine 33:2341–2346
Hessler C, Burkhardt T, Raimund F, Regelsberger J, Vettorazzi E, Madert J, Eggers C (2009) Dynamics of neurological deficit after surgical decompression of symptomatic vertebral metastases. Spine 34:566–571
Klimo P, Thompson CJ, Kestle JR, Schmidt MH (2005) A meta-analysis of surgery versus conventional radiotherapy for the treatment of metastatic spinal epidural disease. Neuro Oncol 7:64–76
North RB, Larocca VR, Schwartz J, North CA, Zahurak M, Davis RF, McAfee PC (2005) Surgical management of spinal metastases: analysis of prognostic factors during a 10-year experience. J Neurosurg Sp 2:564–573
Pascal-Moussellard H, Broc G, Pointillart V, Simeon F, Vital JM, Senegas J (1998) Complications of vertebral metastasis surgery. Eur Spine J 7:438–444
Rompe JD, Hopf CG, Eysel P (1999) Outcome after palliative posterior surgery for metastatic disease of the spine—evaluation of 106 consecutive patients after decompression and stabilization with the Cotrel-Dubousset instrumentation. Arch Orthop Trauma Surg 119:394–400
Wise JJ, Fischgrund JS, Herkowitz HN, Montgomery D, Kurz LT (1999) Complication, survival rates, and risk factors of surgery for metastatic disease of the spine. Spine 24:1943–1951
Finkelstein JA, Zaveri G, Wai E, Vidmar M, Kreder H, Chow E (2003) A population-based study of surgery for spinal metastases. Survival rates and complications. J Bone Joint Surg Br 85:1045–1050
Patil CG, Lad SP, Santarelli J, Boakye M (2007) National inpatient complications and outcomes after surgery for spinal metastasis from 1993–2002. Cancer 110:625–630
Ghogwala Z, Mansfield FL, Borges LF (2001) Spinal radiation before surgical decompression adversely affects outcomes of surgery for symptomatic metastatic spinal cord compression. Spine 26:818–824
Sioutos PJ, Arbit E, Meshulam CF, Galicich JH (1995) Spinal metastases from solid tumors. Analysis of factors affecting survival. Cancer 76:1453–1459
Van der Linden YM, Dijkstra SP, Vonk EJ et al (2005) Prediction of survival in patients with metastases in the spinal column. Results based on a randomized trial of radiotherapy. Cancer 103:320–328
Bartels RH, Feuth T, van der Maazen R, Verbeek AL, Kappelle AC, Grotenhuis JA, Leer JW (2007) Development of a model with which to predict the life expectancy of patients with spinal epidural metastases. Cancer 110:2042–2049
Chow E, Abdolell M, Panzarella T, Harris K, Bezjak A, Warde P, Tannock I (2009) Validation of a predictive model for survival in metastatic cancer patients attending an outpatient palliative radiotherapy clinic. Int J Rad Onc Biol Phys 73:280–287
Cella DF (1996) Quality of life outcomes: measurement and validation. Oncology 10:S233–S245
Acknowledgments
This study was part of an approved French National Research and Clinical Hospital Project funded in 2003 by a public national grant. Dr. Quan was supported by a Post-Doctoral Fellowship from the National Health and Medical Research Council of Australia. The authors would like to acknowledge the assistance of the Centre de Recherche Epidémiologie et Biostatistique PU-PH, Service d’information médicale, CHU de Bordeaux Institut de Santé Publique, d’Epidémiologie et de Développement (ISPED) Université de Bordeaux, France.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Quan, G.M.Y., Vital, JM., Aurouer, N. et al. Surgery improves pain, function and quality of life in patients with spinal metastases: a prospective study on 118 patients. Eur Spine J 20, 1970–1978 (2011). https://doi.org/10.1007/s00586-011-1867-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-011-1867-6