Abstract
Introduction
Dynamic stabilization of the spine was developed as an alternative to rigid fusion in chronic back pain to reduce the risk of adjacent segment degeneration. Dynamic neutralization system (Dynesys, Zimmer CH) is one of the most popular systems available, but some midterm studies show revision rates as high as 30 %. Some late infectious complications in our patients prompted us to review them systematically. Propionibacterium recently has been shown to cause subtle infections of prosthetic material.
Materials and methods
Here, we report on a consecutive series of 50 Dynesys implants. In a median follow-up of 51 months (range 0–91), we identified 12 infectious and 11 non-infectious complications necessitating reoperation or removal of the implant in 17 patients.
Results
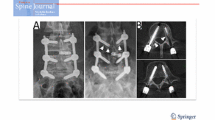
Material infections occurred after a median of 52 months (2–77) and were due to Propionibacterium alone (n = 4) or in combination (n = 3) in seven out of 11 patients. Clinical presentation combines new or increasing pain associated with signs of screw loosening on conventional X-rays; however, as many as 73.5 % of patients present some degree of screw loosening without being at all symptomatic of infection.
Conclusion
The high rate of late infections with low-grade germs and the frequency of screw loosening signs made us suspect a lack of integration at the bone-screw interface. Surgeons should be suspicious if the patient presents a combination of new or increasing pain and signs of screw loosening, and aggressive revision is recommended in these cases.


Similar content being viewed by others
References
Beastall J, Karadimas E, Siddiqui M, Nicol M, Hughes J, Smith F, Wardlaw D (2007) The Dynesys lumbar spinal stabilization system: a preliminary report on positional magnetic resonance imaging findings. Spine (Phila Pa 1976) 32:685–690
Benezech J, Mitulescu A (2007) Retrospective patient outcome evaluation after semi-rigid stabilization without fusion for degenerative lumbar instability. Eur J Orthop Surg Traumatol 17:227–234
Bothmann M, Kast E, Boldt GJ, Oberle J (2008) Dynesys fixation for lumbar spine degeneration. Neurosurg Rev 31:189–196
Collins I, Wilson-MacDonald J, Chami G, Burgoyne W, Vineyakam P, Berendt T, Fairbank J (2008) The diagnosis and management of infection following instrumented spinal fusion. Eur Spine J 17:445–450
Dakhil-Jerew F, Jadeja H, Cohen A, Shepperd JAN (2009) Inter-observer reliability of detecting Dynesys pedicle screw using plain X-rays: a study on 50 post-operative patients. Eur Spine J 18:1486–1493
Davis R, Delamarter R, Maxwell J, Welch W, Wingate J, Sherman J (2009) Preliminary 3-year results from a prospective, randomized, controlled IDE study of the Dynesys dynamic stabilization system. In: Abstracts of the 24th annual meeting of the North American spine society, San Francisco, 10–17 Nov 2009, The Spine J, 86S
Faundez AA, Schwender JD, Safriel Y, Gilbert ThJ, Mehbod AA, Denis F, Transfeldt EE, Wroblewski JM (2009) Clinical and radiological outcome of anterior-posterior fusion versus trans-foraminal lumbar interbody fusion for symptomatic disc degeneration: a retrospective comparative study of 133 patients. Eur Spine J 18:203–211
Grob D, Benini A, Junge A, Mannion AF (2005) Clinical experience with the Dynesys semirigid fixation system for the lumbar spine. Spine 30:324–331
Lee ChS, Hwang ChJ, Lee SW, Ahn YJ, Kim YT, Lee DH, Lee MY (2009) Risk factors for adjacent segment disease after lumbar fusion. Eur Spine J 18:1637–1643
Mannion AF, Elfering A (2006) Predictors of surgical outcome and their assessment. Eur Spine J 15:S93–S108
Mullholland RC, Sengupta DK (2002) Rationale, principles and experimental evaluation of the concept of soft stabilization. Eur Spine J 11:S198–S205
Mullholland RC (2008) The myth of lumbar instability: the importance of abnormal loading as a cause of low back pain. Eur Spine J 17:619–625
Putzier M, Hoff E, Tohtz S, Gross C, Perka C, Strube P (2010) Dynamic stabilization adjacent to single-level fusion: part II. No clinical benefit for asymptomatic, initially degenerated adjacent segments after 6 years follow-up. Eur Spine J 19(12):2181–2189. doi:10.1007/s00586-010-1517-4
Reyes-Sánchez A, Zárate-Kalfópulos B, Ramírez-Mora I, Rosales-Olivarez LM, Alpizar-Aguirre A, Sánchez-Bringas G (2010) Posterior dynamic stabilization of the lumbar spine with the Accuflex rod system as a stand-alone device: experience in 20 patients with 2-year follow-up. Eur Spine J. doi:10-1007/s00586-010-1417-7
St Schaeren, Broger I, Jeanneret B (2008) Minimum 4-year follow-up of spinal stenosis with degenerative spondylolisthesis treated with decompression and dynamic stabilization. Spine 33:E636–E642
Schimmel JJP, Horsting PP, de Kleuver M, Wonders G, van Limbeck J (2010) Risk factors for deep surgical site infections after spinal fusion. Eur Spine J 19:1711–1719
Schwarzenbach O, Berlemann U, Stoll ThM, Dubois G (2005) Posterior dynamic stabilization systems: Dynesys. Orthop Clin N Am 36:363–372
Schwarzenbach O, Rohrbach N, Berlemann U (2010) Segment-by-segment stabilization for degenerative disc disease: a hybrid technique. Eur Spine J 19:1010–1020
Stoll ThM, Dubois G, Schwarzenbach O (2002) The dynamic neutralization system for the spine: a multi-center study of a novel non-fusion system. Eur Spine J 11:S170–S178
Strube P, S Tohtz, Hoff E, Gross C, Perka C, Putzier M (2010) Dynamic stabilization adjacent to single-level fusion: part I. Biomechanical effects on lumbar spinal motion. Eur Spine J. doi:10.1007/s00586-010-1549-9
Würgler-Hauri CC, Kalbarczyk A, Wiesli M, Landolt H, Fandino J (2008) Dynamic neutralization of the lumbar spine after microsurgical decompression in acquired lumbar spinal stenosis and segmental instability. Spine 33:E66–E72
Zappe B, Graf S, Ochsner PE, Zimmerli W, Sendi P (2008) Propionibacterium spp. in prosthetic joint infections: a diagnostic challenge. Arch Orthop Trauma Surg 128:1039–1046
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lutz, J.A., Otten, P. & Maestretti, G. Late infections after dynamic stabilization of the lumbar spine with Dynesys. Eur Spine J 21, 2573–2579 (2012). https://doi.org/10.1007/s00586-012-2366-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-012-2366-0