Abstract
Objectives
The purpose of this study was to investigate the influence of immune deficiency status of HIV-positive patients on postoperative complication such as surgical site infection and nonunions.
Design
Retrospective observational cohort study: Level III.
Setting
Level I trauma center.
Patients/participants
Consecutive adult HIV-positive patients with closed fractures who underwent operative treatment between January 1, 2001 and December 31, 2012.
Main outcome and measurements
postoperative complication including infection and fracture nonunion.
Results
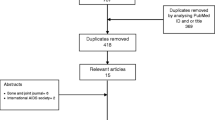
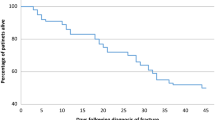
A total of 42 HIV-positive patients with closed fractures who underwent surgical fracture fixation were identified during the 12-year study time window. Of these, 18 patients were excluded due to incomplete medical records (n = 16) or open fractures (n = 2). The remaining 24 patients with closed fracture treated surgically (19 males and 5 females; mean age 45.1 ± 10.5 years; age range 20–67 years) were included in the study. Within a 6-month period from the time of injury, 16 patients had a CD4+ cell count >200 and five patients had a CD4+ cell count <200 (CD4+ cell count was not available in three patients). Twenty-two patients (91.6 %) were on antiretroviral therapy at the time of injury. Only one patient, with associated end-stage renal failure and diabetes mellitus, developed a postoperative infection (4.2 %). All patients achieved fracture union within 180 days postoperatively, without the need for surgical revisions.
Conclusions
Our study suggests that HIV infection does not seem to correlate with a higher risk for the development of postoperative complication related to surgical site infection and fracture nonunions after operative fixation of closed fractures.
Similar content being viewed by others
References
Johnson AS, Hall HI, Hu X, Lansky A, Holtgrave DR, Mermin J (2014) Trends in diagnoses of HIV infection in the United States, 2002–2011. JAMA J Am Med Assoc 312(4):432–434. doi:10.1001/jama.2014.8534
Prevention CfDCa (2013) Monitoring selected national HIV prevention and care objectives by using HIV surveillance data—United States and 6 U.S. dependent areas—2011. HIV Surveillance Supplemental Report 18 (5)
Ball SC (2014) Increased longevity in HIV: caring for older HIV-infected adults. Care Manag J J Case Manag J Long Term Home Health Care 15(2):76–82
Krentz HB, Kliewer G, Gill MJ (2005) Changing mortality rates and causes of death for HIV-infected individuals living in Southern Alberta, Canada from 1984 to 2003. HIV medicine 6(2):99–106. doi:10.1111/j.1468-1293.2005.00271.x
Palella FJ Jr, Baker RK, Moorman AC, Chmiel JS, Wood KC, Brooks JT, Holmberg SD, Investigators HIVOS (2006) Mortality in the highly active antiretroviral therapy era: changing causes of death and disease in the HIV outpatient study. J Acquir Immune Defic Syndr 43(1):27–34. doi:10.1097/01.qai.0000233310.90484.16
Yang CH, Huang YF, Hsiao CF, Yeh YL, Liou HR, Hung CC, Yang SY (2008) Trends of mortality and causes of death among HIV-infected patients in Taiwan, 1984–2005. HIV Med 9(7):535–543. doi:10.1111/j.1468-1293.2008.00600.x
Castronuovo D, Cacopardo B, Pinzone MR, Di Rosa M, Martellotta F, Schioppa O, Moreno S, Nunnari G (2013) Bone disease in the setting of HIV infection: update and review of the literature. Eur Rev Med Pharmacol Sci 17(18):2413–2419
Del Carpio-Cano FE, Dela Cadena RA, Sawaya BE (2013) HIV and bone disease: a perspective of the role of microRNAs in bone biology upon HIV infection. J Osteoporos 2013:571418. doi:10.1155/2013/571418
Mallon PW (2014) Ageing with HIV: osteoporosis and fractures. Curr Opin HIV AIDS. doi:10.1097/COH.0000000000000080
Prieto-Alhambra D, Guerri-Fernandez R, De Vries F, Lalmohamed A, Bazelier M, Starup-Linde J, Diez-Perez A, Cooper C, Vestergaard P (2014) HIV infection and its association with an excess risk of clinical fractures: a nationwide case-control study. J Acquir Immune Defic Syndr 66(1):90–95. doi:10.1097/QAI.0000000000000112
Bates J, Mkandawire N, Harrison WJ (2012) The incidence and consequences of early wound infection after internal fixation for trauma in HIV-positive patients. J Bone Jt Surg Br 94(9):1265–1270. doi:10.1302/0301-620X.94B9.28682
Harrison WJ, Lewis CP, Lavy CB (2002) Wound healing after implant surgery in HIV-positive patients. J Bone Jt Surg Br 84(6):802–806
Richardson J, Hill AM, Johnston CJ, McGregor A, Norrish AR, Eastwood D, Lavy CB (2008) Fracture healing in HIV-positive populations. J Bone Jt Surg Br 90(8):988–994. doi:10.1302/0301-620X.90B8.20861
Gardner RO, Bates JH, Ng’oma E, Harrison WJ (2013) Fracture union following internal fixation in the HIV population. Injury 44(6):830–833. doi:10.1016/j.injury.2012.11.024
Masur H, Ognibene FP, Yarchoan R, Shelhamer JH, Baird BF, Travis W, Suffredini AF, Deyton L, Kovacs JA, Falloon J et al (1989) CD4 counts as predictors of opportunistic pneumonias in human immunodeficiency virus (HIV) infection. Ann Intern Med 111(3):223–231
Vlahov D, Graham N, Hoover D, Flynn C, Bartlett JG, Margolick JB, Lyles CM, Nelson KE, Smith D, Holmberg S, Farzadegan H (1998) Prognostic indicators for AIDS and infectious disease death in HIV-infected injection drug users: plasma viral load and CD4+ cell count. JAMA J Am Med Assoc 279(1):35–40
Conflict of interest
The authors declare no conflict of interest in relation to the preparation of this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hao, J., Herbert, B., Quispe, J.C. et al. An observational case series of HIV-positive patients treated with open reduction internal fixation for a closed lower extremity fracture. Eur J Orthop Surg Traumatol 25, 815–819 (2015). https://doi.org/10.1007/s00590-015-1595-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-015-1595-4