Abstract
Aims
Pre-operative templating for total hip replacement (THR) surgery leads to more accurate implant sizing and positioning. This study aimed to compare the KingMark™ dual-marker system for magnification calibration to the current gold standard single-marker system in accuracy of predicting implant size and restoration of leg length post-operatively.
Methods
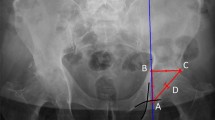
This is a retrospective analysis of patients who had primary THR surgery from 2013 to 2019 by a single surgeon. Patients were in two cohorts whose operations were completed at separate healthcare facilities. Patients in the first cohort had pre-operative templating using the KingMark system; patients in the second cohort had templating using a single-marker. For all patients, pre-operative radiographs were reviewed; predicted implants noted; and leg length discrepancies calculated. These were compared to post-operative data. We then tested the null hypothesis that there was no difference between the templating methods for prediction accuracy of implant size and achieving restoration of leg length.
Results
A total of 121 patients were included in the KingMark cohort, and 104 were included in the single-marker cohort. In the KingMark cohort, 83.5% of patients had implantation of a cup within one size of that predicted, compared to 71.2% of the single-marker cohort. This superiority was statistically significant. There was a greater proportion of exact cup size predictions in the KingMark cohort, but this was not statistically significant. We did not find any significant difference between the cohorts for stem size, or stem placement, or reduction of leg length discrepancy.
Conclusion
We have demonstrated statistically significant superiority of the KingMark over a single-marker templating system for predicting cup size in primary THR surgery. For post-operative restoration of leg length, our study did not show any advantage of KingMark templating compared to single-marker templating.


Similar content being viewed by others
References
Eggli S, Pisan M, Muller ME (1998) The value of preoperative planning for total hip arthroplasty. J Bone Jt Surg 80(3):9
Alnahhal A, Aslam-Pervez N, Sheikh HQ (2019) Templating hip arthroplasty. Open Access Maced J Med Sci 7(4):672–685. https://doi.org/10.3889/oamjms.2019.088
Crooijmans HJA, Laumen AMRP, van Pul C, van Mourik JBA (2009) A new digital preoperative planning method for total hip arthroplasties. Clin Orthop Relat Res 467(4):909–916. https://doi.org/10.1007/s11999-008-0486-y
Conn KS, Clarke MT, Hallett JP (2002) A simple guide to determine the magnification of radiographs and to improve the accuracy of preoperative templating. J Bone Jt Surg 84(2):4
Davila JA, Kransdorf MJ, Duffy GP (2006) Surgical planning of total hip arthroplasty: accuracy of computer-assisted EndoMap software in predicting component size. Skeletal Radiol 35(6):390–393. https://doi.org/10.1007/s00256-006-0106-4
Iorio R, Siegel J, Specht LM, Tilzey JF, Hartman A, Healey WL (2009) A comparison of acetate vs digital templating for preoperative planning of total hip arthroplasty: is digital templating accurate and safe? J Arthroplasty 24(2):175–179. https://doi.org/10.1016/j.arth.2007.11.019
Whiddon DR, Bono JV, Lang JE, Smith ES, Salyapongse AK (2011) Accuracy of digital templating in total hip arthroplasty. Am J Orthop (Belle Mead NJ) 40(8):395–398 (PMID: 22016868)
Gamble P, de Beer J, Petruccelli D, Winemaker M (2010) The accuracy of digital templating in uncemented total hip arthroplasty. J Arthroplasty 25(4):529–532. https://doi.org/10.1016/j.arth.2009.04.011
Si H, Zeng Y, Cao F, Pei F, Shen B (2015) Accuracy of a simple digital templating in primary uncemented total hip arthroplasty. Chin Med Sci J 30(3):150–155. https://doi.org/10.1016/S1001-9294(15)30039-0
Della Valle AG, Comba F, Taveras N, Salvati EA (2008) The utility and precision of analogue and digital preoperative planning for total hip arthroplasty. Int Orthop (SICO) 32(3):289–294. https://doi.org/10.1007/s00264-006-0317-2
Valle AGD, Padgett DE, Salvati EA (2005) Preoperative planning for primary total hip arthroplasty. J Am Acad Orthop Surg 13(7):8
Bayne CO, Krosin M, Barber TC (2009) Evaluation of the accuracy and use of X-ray markers in digital templating for total hip arthroplasty. J Arthroplasty 24(3):407–413. https://doi.org/10.1016/j.arth.2007.11.020
Boese CK, Wilhelm S, Haneder S (2018) Influence of calibration on digital templating of hip arthroplasty. Int Orthop 43(8):1799–1805. https://doi.org/10.1007/s00264-018-4120-7
Archibeck MJ et al (2016) Inaccuracies in the use of magnification markers in digital hip radiographs. Clin Orthop Relat Res 474(8):1812–1817. https://doi.org/10.1007/s11999-016-4704-8
Holzer LA, Scholler G, Wagner S, Friesenbichler J, Maurer-Ertl W, Leithner A (2019) The accuracy of digital templating in uncemented total hip arthroplasty. Arch Orthop Trauma Surg 139(2):263–268. https://doi.org/10.1007/s00402-018-3080-0
Shin JK, Son SM, Kim TW, Shin WC, Lee JS, Suh KT (2016) Accuracy and reliability of preoperative on-screen templating using digital radiographs for total hip arthroplasty. Hip Pelvis 28(4):201. https://doi.org/10.5371/hp.2016.28.4.201
Bertz A, Indrekvam K, Ahmed M, Englund E, Sayed-Noor AS (2012) Validity and reliability of preoperative templating in total hip arthroplasty using a digital templating system. Skeletal Radiol 41(10):1245–1249. https://doi.org/10.1007/s00256-012-1431-4
Shaarani SR, McHugh G, Collins DA (2013) Accuracy of digital preoperative templating in 100 consecutive uncemented total hip arthroplasties. J Arthroplasty 28(2):331–337. https://doi.org/10.1016/j.arth.2012.06.009
Iorio R, Siegel J, Specht LM, Tilzey JF, Hartman A, Healy WL (2009) A comparison of acetate versus digital templating for preoperative planning of total hip arthroplasty. J Arthroplasty 24(2):175–179. https://doi.org/10.1016/j.arth.2007.11.019
Unnanuntana A, Wagner D, Goodman SB (2009) The accuracy of preoperative templating in cementless total hip arthroplasty. J Arthroplasty 24(2):180–186. https://doi.org/10.1016/j.arth.2007.10.032
Warschawski Y et al (2020) The accuracy of external calibration markers in digital templating using the double marker and single marker method: a comparative study. Arch Orthop Trauma Surg 140(10):1559–1565. https://doi.org/10.1007/s00402-020-03569-2
Efe T, El Zayat B, Heyse T, Timmesfeld N, Fuchs-Winkelmann S, Schmitt J (2011) Precision of preoperative digital templating in total hip arthroplasty. Acta Orthop Belg 77(5):616–621
Steinberg EL, Shasha N, Menahem A, Dekel S (2010) Preoperative planning of total hip replacement using the TraumaCadTM system. Arch Orthop Trauma Surg 130(12):1429–1432. https://doi.org/10.1007/s00402-010-1046-y
Kumar P, Kirmani S, Humberg H, Kavarthapu V, Li P (2009) Reproducibility and accuracy of templating uncemented THA with digital radiographic and digital TraumaCad templating software. Orthopedics 32(11):815. https://doi.org/10.3928/01477447-20090922-08
Wedemeyer C, Quitmann H, Xu J, Heep H, von Knoch M, Saxler G (2008) Digital templating in total hip arthroplasty with the Mayo stem. Arch Orthop Trauma Surg 128(10):1023–1029. https://doi.org/10.1007/s00402-007-0494-5
King RJ, Makrides P, Gill JA, Karthikeyan S, Krikler SJ, Griffin DR (2009) A novel method of accurately calculating the radiological magnification of the hip. J Bone Jt Surg 91(9):6
Baxter JA, Barlow T, Karthikeyan S, Mayo DJ, King RJ (2012) The accuracy of automatic calibration of digital pelvic radiographs using two different scale markers: a comparative study. Hip Int 22(1):82–89. https://doi.org/10.5301/HIP.2012.9044
Woolson ST, Hartford JM, Sawyer A (1999) Results of a method of leg-length equalization for patients undergoing primary total hip replacement. J Arthroplasty 14(2):159–164. https://doi.org/10.1016/S0883-5403(99)90119-5
Heaver C, St Mart J-P, Nightingale P, Sinha A, Davis ET (2013) Measuring limb length discrepancy using pelvic radiographs: the most reproducible method. Hip Int 23(4):391–394. https://doi.org/10.5301/hipint.5000042
Hananouchi T et al (2007) Preoperative templating of femoral components on plain X-rays: rotational evaluation with synthetic X-rays on ORTHODOC. Arch Orthop Trauma Surg 127(5):381–385. https://doi.org/10.1007/s00402-007-0349-0
Eckrich SGJ, Noble PC, Tullos HS (1994) Effect of rotation on the radiographic appearance of the femoral canal. J Arthroplasty 9(4):419–426. https://doi.org/10.1016/0883-5403(94)90053-1
Sershon R, Diaz A, Bohl D, Levine B (2017) Effect of body mass index on digital templating for total hip arthroplasty. J Arthroplasty 32(3):1024–1026. https://doi.org/10.1016/j.arth.2016.09.020
Konyves A, Bannister GC (2005) The importance of leg length discrepancy after total hip arthroplasty. J Bone Jt Surg Br 87(2):3
Desai AS, Dramis A, Board TN (2013) Leg length discrepancy after total hip arthroplasty: a review of literature. Curr Rev Musculoskelet Med 6(4):336–341. https://doi.org/10.1007/s12178-013-9180-0
Bono JV (2004) Digital templating in total hip arthroplasty. J Bone Jt Surg Am 86-A(Suppl 2):118–122. https://doi.org/10.2106/00004623-200412002-00016
Woolson ST, Harris WH (1985) A method of intraoperative limb length measurement in total hip arthroplasty. Clin Orthop Relat Res 194:207–210. https://doi.org/10.1097/00003086-198504000-00032
Suh KT, Cheon SJ, Kim DW (2004) Comparison of preoperative templating with postoperative assessment in cementless total hip arthroplasty. Acta Orthop Scand 75(1):40–44. https://doi.org/10.1080/00016470410001708070
Acknowledgements
The authors acknowledge the helps from Sohail Nisar, Rana Al-Ashqar.
Funding
We confirm no funding was sought and no funding was received for this research project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There were no conflicts of interest with any of the authors or any of the software used. None of the authors have any financial or personal interests with any of the material or software in the study.
Ethical approval
Ethical approval was not required as all data collection was retrospective, anonymised, and did not affect any patient management or outcomes.
Ethical standards
We confirm that all data collection and analysis were performed in keeping with patient confidentiality protection and complied with local ethical standards.
Informed consent
Informed consent was not needed from patients as all data analysed were retrospective, anonymised, and not traceable to any individual patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Al-Ashqar, M., Aslam, N., Azhar, M.S. et al. KingMark’s dual-marker versus a conventional single-marker templating system: is there a difference in accuracy of predicting final implant sizes and leg lengths?. Eur J Orthop Surg Traumatol 33, 167–175 (2023). https://doi.org/10.1007/s00590-021-03174-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-03174-y