Abstract
Purposes
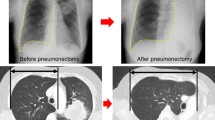
The purpose of this study was to investigate the compensatory phenomena after lung resection in clinical cases by evaluating the spirometric and radiological parameters.
Methods
Forty patients undergoing lobectomy for stage IA lung cancer were divided into the following groups: (A) patients with <10 (n = 20) and (B) patients with ≥10 resected subsegments (n = 20). Comparisons were made of the predicted and observed postoperative values of spirometry and radiological parameters, such as lung volumetry and the “estimated lung weight”. Predicted values were based on the number of resected subsegments. The postoperative time to re-evaluation was at least 1 year for both groups.
Results
The predicted postoperative values of spirometry underestimated the actual values, and the differences were more significant in group B (forced vital capacity, p = 0.006, forced expiratory volume in 1 s, p = 0.011). Focusing on the remnant lungs on the surgical side, group B had significantly larger % postoperative lung volumes (161 ± 6.0 %) and % estimated lung weight (124 ± 5.4 %) than did group A (114 ± 3.8 %, p < 0.0001; 89.5 ± 4.4 %, p < 0.0001, respectively).
Conclusions
Major lung resection in clinical cases causes a compensatory restoration of the pulmonary function and tissue.








Similar content being viewed by others
References
Nakahara K, Monden Y, Ohno K, Miyoshi S, Maeda H, Kawashima Y. A method for predicting postoperative lung function and its relation to postoperative complications in patients with lung cancer. Ann Thorac Surg. 1985;39(3):260–5.
Koizumi K, Tanaka S, Shioda M, Haraguchi S, Masaki Y, Morota T, et al. Simplified prediction of postoperative lung function by plain chest roentgenogram in patients with primary lung cancer–in correlation to postoperative respiratory complications. Nihon Kyobu Geka Gakkai Zasshi. 1991;39(9):1758–64.
Zeiher BG, Gross TJ, Kern JA, Lanza LA, Peterson MW. Predicting postoperative pulmonary function in patients undergoing lung resection. Chest. 1995;108(1):68–72.
Chen F, Kubo T, Shoji T, Fujinaga T, Bando T, Date H. Comparison of pulmonary function test and computed tomography volumetry in living lung donors. J Heart Lung Transpl. 2011;30(5):572–5.
American Thoracic Society. Mechanisms and limits of induced postnatal lung growth. Am J Respir Crit Care Med. 2004;170(3):319–43.
Wada H, Yoshida S, Suzuki H, Sakairi Y, Mizobuchi T, Komura D, et al. Transplantation of alveolar type II cells stimulates lung regeneration during compensatory lung growth in adult rats. J Thorac Cardiovasc Surg. 2012;143(3):711–9.
Kubo H. Molecular basis of lung tissue regeneration. Gen Thorac Cardiovasc Surg. 2011;59(4):231–44.
Sakamaki Y, Matsumoto K, Mizuno S, Matsuda H, Nakamura T. Hepatocyte growth factor stimulates proliferation of respiratory epithelial cells during postpneumonectomy compensatory lung growth in mice. Am J Repir Cell Mol Biol. 2002;26(5):525–33.
Matsumoto K, Nagayasu T, Hishikawa Y, Tagawa T, Yamayoshi T, Abo T, et al. Keratinocyte growth factor accelerates compensatory growth in the remaining lung after trilobectomy in rats. J Thorac Cardiovasc Surg. 2009;137(6):1499–507.
Sakurai MK, Lee S, Arsenault DA, Nose V, Wilson JM, Heymach JV, et al. Vascular endothelial growth factor accelerates compensatory lung growth after unilateral pneumonectomy. Am J Physiol Lung Cell Mol Physiol. 2007;292(3):L742–7.
Kaza AK, Kron IL, Kern JA, Long SM, Fiser SM, Nguyen RP, et al. Retinoic acid enhances lung growth after pneumonectomy. Ann Thorac Surg. 2001;71(5):1645–50.
Akira M, Toyokawa K, Inoue Y, Arai T. Quantitative CT in chronic obstructive pulmonary disease: inspiratory and expiratory assessment. AJR Am J Roentgenol. 2009;192(1):267–72.
Yamashiro T, Matsuoka S, Bartholmai BJ, San José Estépar R, Ross JC, et al. Collapsibility of lung volume by paired inspiratory and expiratory CT scans: correlations with lung function and mean lung density. Acad Radiol. 2010;17(4):489–95.
ARDS Definition Task Force. Acute respiratory distress syndrome: the Berlin definition. JAMA. 2012;307(23):2526–33.
Gattinoni L, Caironi P, Pelosi P. What has computed tomography taught us about the acute respiratory distress syndrome? Am J Respir Crit Care Med. 2001;164(9):1701–11.
Endoh H, Yamamoto R, Satoh Y, Kuwano H, Nishizawa N. Risk analysis of pulmonary resection for elderly patients with lung cancer. Surg Today. 2013;43(5):514–20.
Ueda K, Tanaka T, Hayashi M, Li TS, Kaneoka T, Tanaka N, et al. Compensation of pulmonary function after upper lobectomy versus lower lobectomy. J Thorac Cardiovasc Surg. 2011;142(4):762–7.
Ibla JC, Shamberger RC, DiCanzio J, Zurakowski D, Koka BV, Lillehei CW. Lung growth after reduced size transplantation in a sheep model. Transplantation. 1999;67(2):233–40.
Butler JP, Loring SH, Patz S, Tsuda A, Yablonskiy DA, Mentzer SJ. Evidence for adult lung growth in humans. N Engl J Med. 2012;367:244–7.
Toyooka S, Sano Y, Yamane M, Oto T, Okazaki M, Kusano KF, et al. Long-term follow-up of living-donor single lobe transplantation for idiopathic pulmonary arterial hypertension in a child. J Thorac Cardiovasc Surg. 2008;135(2):451–2.
Mizobuchi T, Chen F, Yoshino I, Iwata T, Yoshida S, Bando T, et al. Radiological evaluation for volume and weight of remnant lung in living lung donors. J Thorac Cardiovasc Surg. 2013;. doi:10.1016/j.jtcvs.2013.05.038 (in Press).
Ueda K, Tanaka T, Hayashi M, Li TS, Tanaka N, Hamano K. Computed tomography-defined functional lung volume after segmentectomy versus lobectomy. Eur J Cardiothorac Surg. 2010;37(6):1433–7.
Nagamatsu Y, Maeshiro K, Kimura NY, Nishi T, Shima I, Yamana H, et al. Long-term recovery of exercise capacity and pulmonary function after lobectomy. J Thorac Cardiovasc Surg. 2007;134(5):1273–8.
Acknowledgments
This study was supported by Grants-in-Aid for Scientific Research (C) 23592054 (to T.M.) from the Japan Society for the Promotion of Science (JSPS KAKENHI Grant Number 23592054).
Conflict of interest
Teruaki Mizobuchi and the co-authors have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mizobuchi, T., Wada, H., Sakairi, Y. et al. Spirometric and radiological evaluation of the remnant lung long after major pulmonary resection: can compensatory phenomena be recognized in clinical cases?. Surg Today 44, 1735–1743 (2014). https://doi.org/10.1007/s00595-013-0702-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-013-0702-6