Abstract
Introduction
Radiosurgery (RS) and fractionated radiotherapy (FRT) are part of the therapeutic armamentarium for the management of cavernous sinus meningiomas. We propose a systematic review of the local tumor control and clinical outcomes after monofractionated radiosurgical treatment, including gamma knife radiosurgery (GKRS) and linear accelerator (Linac RS), or fractionated radiotherapy.
Materials and Methods
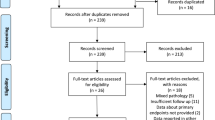
The current review and meta-analysis adhered to the PRISMA guidelines. We performed a search in PubMed, Embase, and Medline based on the following mesh terms, used alone or in diverse combinations, in both title and abstract: “cavernous sinus,” “meningioma,” “radiosurgery,” “gamma knife,” “linac,” “cyberknife,” and “radiotherapy”. We screened 425 studies. We selected 36 studies, matching all selection criteria: 24 for GK, 5 for Linac, and 7 for FRT.
Results
Were included 2817 patients (GKRS, n = 2047, LinacRS, n = 350, FRT, n = 420). Half of patients benefited from upfront RS or FRT; the other half benefited from adjuvant RS or FRT (combined approach or tumor recurrence). The mean gross target volume (GTV) was smaller for RS as compared to FRT (p = 0.07). The median marginal doses were 13.9 Gy (range, 11 to 28) for GKRS and 14 Gy (range, 12.8 to 17.7) for LinacRS. For FRT, patients received a mean dose of 51.2 Gy (25.5 fractions, 1.85 Gy each). The mean overall follow-up values were 48 months (range, 15 to 89) for GKRS, 69 months (range, 46 to 87) for Linac, and 59.5 months (range, 33 to 83) for FRT. PFS at 5 years for GKRS, LinacRS, and FRT were respectively 93.6%, 95.6%, and 97.4% (p = 0.32, the Kruskal-Wallis). Monofractionated treatments (GKRS and LinacRS) induced more tumor volume regression than FRT (p = 0.001). Tumor recurrence or progression ranged between 3 and 5.8%, without statistically significant differences between modalities (p > 0.05). Trigeminal symptoms improved in approximately 54%, and III-IV-VI cranial nerves (CN) palsies improved in approximately 45%. After GKRS, visual acuity improved in 21% (not enough data available for other modalities). De novo deficits occurred in 5 to 7.5%. Adverse radiation effects appeared in 4.6 to 9.3% (all techniques pooled).
Conclusion
RS achieved a twice-higher rate of tumor volume regression than FRT. GKRS series reported an improvement in visual acuity in 21% of the cases. GKRS, Linac, and FRT provided similar clinical post therapeutic outcomes for the trigeminal and oculomotor CN.




Similar content being viewed by others
References
Wiemels J, Wrensch M, Claus EB (2010) Epidemiology and etiology of meningioma. J Neuro-Oncol 99:307–314
Goldbrunner R, Minniti G, Preusser M, Jenkinson MD, Sallabanda K, Houdart E, von Deimling A, Stavrinou P, Lefranc F, Lund-Johansen M, Moyal EC, Brandsma D, Henriksson R, Soffietti R, Weller M (2016) EANO guidelines for the diagnosis and treatment of meningiomas. Lancet Oncol 17:e383–e391
Simpson D (1957) The recurrence of intracranial meningiomas after surgical treatment. J Neurol Neurosurg Psychiatry 20:22–39
DeMonte F, Smith HK, al-Mefty O (1994) Outcome of aggressive removal of cavernous sinus meningiomas. J Neurosurg 81:245–251
O’Sullivan MG, van Loveren HR, Tew JM Jr (1997) The surgical resectability of meningiomas of the cavernous sinus. Neurosurgery 40:238–244 discussion 245–237
Sindou M, Wydh E, Jouanneau E, Nebbal M, Lieutaud T (2007) Long-term follow-up of meningiomas of the cavernous sinus after surgical treatment alone. J Neurosurg 107:937–944
Franzin A, Vimercati A, Medone M, Serra C, Marzoli SB, Forti M, Gioia L, Valle M, Picozzi P (2007) Neuroophthalmological evaluation after Gamma Knife surgery for cavernous sinus meningiomas. Neurosurg Focus 23
Kano H, Park K-JJ, Kondziolka D, Iyer A, Liu X, Tonetti D, Flickinger JC, Lunsford LD (2013) Does prior microsurgery improve or worsen the outcomes of stereotactic radiosurgery for cavernous sinus meningiomas? Neurosurgery 73:401–410
Pollock BE, Stafford SL, Link MJ, Garces YI, Foote RL (2013) Single-fraction radiosurgery of benign cavernous sinus meningiomas. J Neurosurg 119:675–682
Dufour H, Muracciole X, Métellus P, Régis J, Chinot O, Grisoli F (2001) Long-term tumor control and functional outcome in patients with cavernous sinus meningiomas treated by radiotherapy with or without previous surgery: is there an alternative to aggressive tumor removal? Neurosurgery 48:285
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6:e1000100
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8:336–341
Duma CM, Lunsford LD, Kondziolka D, Harsh GR, Flickinger JC (1993) Stereotactic radiosurgery of cavernous sinus meningiomas as an addition or alternative to microsurgery. Neurosurgery 32:699
Hafez RF, Morgan MS, Fahmy OM (2015) Stereotactic Gamma Knife surgery safety and efficacy in the management of symptomatic benign confined cavernous sinus meningioma. Acta Neurochir 157:1559–1564
Hasegawa T, Kida Y, Yoshimoto M, Koike J, Iizuka H, Ishii D (2007) Long-term outcomes of Gamma Knife surgery for cavernous sinus meningioma. J Neurosurg 107:745–751
Hayashi M, Chernov M, Tamura N, Tamura M, Horiba A, Konishi Y, Okada Y, Muragaki Y, Iseki H, Takakura K (2012) Gamma knife radiosurgery for benign cavernous sinus tumors: treatment concept and outcomes in 120 cases. Neurol Med Chir 52:714–723
Iwai Y, Yamanaka K, Ishiguro T (2003) Gamma knife radiosurgery for the treatment of cavernous sinus meningiomas. Neurosurgery 52:517
Kobayashi T, Kida Y, Mori Y (2001) Long-term results of stereotactic gamma radiosurgery of meningiomas. Surg Neurol 55:325–331
Lee JY, Niranjan A, McInerney J, Kondziolka D, Flickinger JC, Lunsford LD (2002) Stereotactic radiosurgery providing long-term tumor control of cavernous sinus meningiomas. J Neurosurg 97:65–72
Liscák R, Simonová G, Vymazal J, Janousková L, Vladyka V (1999) Gamma knife radiosurgery of meningiomas in the cavernous sinus region. Acta Neurochir 141:473–480
Liu ALL, Wang C, Sun S, Wang M, Liu P (2005) Gamma knife radiosurgery for tumors involving the cavernous sinus. Stereotact Funct Neurosurg 83:45–51
Malik I, Rowe JG, Walton L, Radatz MW, Kemeny AA (2005) The use of stereotactic radiosurgery in the management of meningiomas. Br J Neurosurg 19:13–20
Maruyama K, Shin M, Kurita H, Kawahara N, Morita A, Kirino T (2004) Proposed treatment strategy for cavernous sinus meningiomas: a prospective study. Neurosurgery 55:1068–1075
Nicolato A, Foroni R, Alessandrini F, Bricolo A, Gerosa M (2002) Radiosurgical treatment of cavernous sinus meningiomas: experience with 122 treated patients. Neurosurgery 51:1153
Pollock BE, Stafford SL (2005) Results of stereotactic radiosurgery for patients with imaging defined cavernous sinus meningiomas. Int J Radiat Oncol Biol Phys 62:1427–1431
Roche PH, Régis J, Dufour H, Fournier HD, Delsanti C, Pellet W, Grisoli F, Peragut JC (2000) Gamma knife radiosurgery in the management of cavernous sinus meningiomas. J Neurosurg 93(Suppl 3):68–73
Shin M, Kurita H, Sasaki T, Kawamoto S, Tago M, Kawahara N, Morita A, Ueki K, Kirino T (2001) Analysis of treatment outcome after stereotactic radiosurgery for cavernous sinus meningiomas. J Neurosurg 95:435–439
Skeie BS, Enger PO, Skeie GO, Thorsen F, Pedersen PHH (2010) Gamma knife surgery of meningiomas involving the cavernous sinus: long-term follow-up of 100 patients. Neurosurgery 66:661
Williams BJ, Yen CP, Starke RM, Basina B, Nguyen J, Rainey J, Sherman JH, Schlesinger D, Sheehan JP (2011) Gamma Knife surgery for parasellar meningiomas: long-term results including complications, predictive factors, and progression-free survival. J Neurosurg 114:1571–1577
Zada G, Pagnini PG, Yu C, Erickson KT, Hirschbein J, Zelman V, Apuzzo ML (2010) Long-term outcomes and patterns of tumor progression after gamma knife radiosurgery for benign meningiomas. Neurosurgery 67:322
Correa SFF, Marta GN, Teixeira MJ (2014) Neurosymptomatic carvenous sinus meningioma: a 15-years experience with fractionated stereotactic radiotherapy and radiosurgery. Radiation oncology (London, England) 9:27
Chang D, Adler R, Martin DP (1998) LINAC Radiosurgery for Cavernous Sinus Meningiomas. Stereotact Funct Neurosurg 71:43–50
dos Santos MA, de Salcedo JBB, Gutiérrez Diaz JAA, Calvo FA, Samblás J, Marsiglia H, Sallabanda K (2011) Long-term outcomes of stereotactic radiosurgery for treatment of cavernous sinus meningiomas. Int J Radiat Oncol Biol Phys 81:1436–1441
Kimball MM, Friedman WA, Foote KD, Bova FJ, Chi YY (2009) Linear accelerator radiosurgery for cavernous sinus meningiomas. Stereotact Funct Neurosurg 87:120–127
Spiegelmann R, Cohen ZR, Nissim O, Alezra D, Pfeffer R (2010) Cavernous sinus meningiomas: a large LINAC radiosurgery series. J Neuro-Oncol 98:195–202
Brell M, Villà S, Teixidor P, Lucas A, Ferrán E, Marín S, Acebes J (2006) Fractionated stereotactic radiotherapy in the treatment of exclusive cavernous sinus meningioma: functional outcome, local control, and tolerance. Surg Neurol 65:28–33
Haghighi N, Seely A, Paul E, Dally M (2015) Hypofractionated stereotactic radiotherapy for benign intracranial tumours of the cavernous sinus. J Clin Neurosci 22:1450–1455
Litré C, Colin P, Noudel R, Peruzzi P, Bazin A, Sherpereel B, Bernard M, Rousseaux P (2009) Fractionated stereotactic radiotherapy treatment of cavernous sinus meningiomas: a study of 100 cases. Int J Radiat Oncol Biol Phys 74:1012–1017
Metellus P, Batra S, Karkar S, Kapoor S, Weiss S, Kleinberg L, Rigamonti D (2010) Fractionated conformal radiotherapy in the management of cavernous sinus meningiomas: long-term functional outcome and tumor control at a single institution. Int J Radiat Oncol Biol Phys 78:836–843
Milker-Zabel S, Bois A, Huber P, Schlegel W, Debus J (2006) Fractionated stereotactic radiation therapy in the management of benign cavernous sinus meningiomas : long-term experience and review of the literature. Strahlenther Onkol 182:635–640
Selch MT, Ahn E, Laskari A, Lee SP, Agazaryan N, Solberg TD, Cabatan-Awang C, Frighetto L, Desalles A (2004) Stereotactic radiotherapy for treatment of cavernous sinus meningiomas. International Journal of Radiation Oncology*Biology*Physics 59:101–111
Soldà F, Wharram B, De Ieso PB, Bonner J, Ashley S, Brada M (2013) Long-term efficacy of fractionated radiotherapy for benign meningiomas. Radiother Oncol 109:330–334
Kuo JS, Chen JC, Yu C, Zelman V, Giannotta SL, Petrovich Z, MacPherson D, Apuzzo ML (2004) Gamma knife radiosurgery for benign cavernous sinus tumors: quantitative analysis of treatment outcomes. Neurosurgery 54:1385
Metellus P, Regis J, Muracciole X, Fuentes S, Dufour H, Nanni I, Chinot O, Martin P-MM, Grisoli F (2005) Evaluation of fractionated radiotherapy and gamma knife radiosurgery in cavernous sinus meningiomas: treatment strategy. Neurosurgery 57:873
Fariselli L, Biroli A, Signorelli A, Broggi M, Marchetti M, Biroli F (2016) The cavernous sinus meningiomas’ dilemma: Surgery or stereotactic radiosurgery? Rep Pract Oncol Radiother 21:379–385
Sughrue ME, Rutkowski MJ, Aranda D, Barani IJ, McDermott MW, Parsa AT (2010) Factors affecting outcome following treatment of patients with cavernous sinus meningiomas. J Neurosurg 113:1087–1092
Kaprealian T, Raleigh DR, Sneed PK, Nabavizadeh N, Nakamura JL, McDermott MW (2016) Parameters influencing local control of meningiomas treated with radiosurgery. J Neuro-Oncol 128:357–364
Sandstrom H, Nordstrom H, Johansson J, Kjall P, Jokura H, Toma-Dasu I (2014) Variability in target delineation for cavernous sinus meningioma and anaplastic astrocytoma in stereotactic radiosurgery with Leksell Gamma Knife Perfexion. Acta Neurochir 156:2303–2312 discussion 2312–2303
Kondziolka D, Flickinger JC, Perez B (1998) Judicious resection and/or radiosurgery for parasagittal meningiomas: outcomes from a multicenter review. Gamma Knife Meningioma Study Group. Neurosurgery 43:405–413 discussion 413-404
Rogers L, Barani I, Chamberlain M, Kaley TJ, McDermott M, Raizer J, Schiff D, Weber DC, Wen PY, Vogelbaum MA (2015) Meningiomas: knowledge base, treatment outcomes, and uncertainties. A RANO review J Neurosurg 122:4–23
Kaul D, Badakhshi H, Gevaert T, Pasemann D, Budach V, Tuleasca C, Gruen A, Prasad V, Levivier M, Kufeld M (2015) Dosimetric comparison of different treatment modalities for stereotactic radiosurgery of meningioma. Acta Neurochir 157:559–563 discussion 563–554
Kaul D, Badakhshi H, Gevaert T, Pasemann D, Budach V, Tuleasca C, Gruen A, Prasad V, Levivier M, Kufeld M (2015) Erratum to: dosimetric comparison of different treatment modalities for stereotactic radiosurgery of meningioma. Acta Neurochir 157:565
Leavitt JA, Stafford SL, Link MJ, Pollock BE (2013) Long-term evaluation of radiation-induced optic neuropathy after single-fraction stereotactic radiosurgery. Int J Radiat Oncol Biol Phys 87:524–527
Marchetti M, Bianchi S, Pinzi V, Tramacere I, Fumagalli ML, Milanesi IM, Ferroli P, Franzini A, Saini M, DiMeco F, Fariselli L (2016) Multisession radiosurgery for sellar and parasellar benign meningiomas: long-term tumor growth control and visual outcome. Neurosurgery 78:638–646
Navarria P, Pessina F, Cozzi L, Clerici E, Villa E, Ascolese AM, De Rose F, Comito T, Franzese C, D’Agostino G, Lobefalo F, Fogliata A, Reggiori G, Fornari M, Tomatis S, Bello L, Scorsetti M (2015) Hypofractionated stereotactic radiation therapy in skull base meningiomas. J Neuro-Oncol 124:283–289
Stieler F, Wenz F, Abo-Madyan Y, Schweizer B, Polednik M, Herskind C, Giordano FA, Mai S (2016) Adaptive fractionated stereotactic Gamma Knife radiotherapy of meningioma using integrated stereotactic cone-beam-CT and adaptive re-planning (a-gkFSRT). Strahlenther Onkol
Nakazawa H, Mori Y, Komori M, Tsugawa T, Shibamoto Y, Kobayashi T, Hashizume C, Uchiyama Y, Hagiwara M (2014) Simulational study of a dosimetric comparison between a Gamma Knife treatment plan and an intensity-modulated radiotherapy plan for skull base tumors. J Radiat Res 55:518–526
De Jesus O, Sekhar LN, Parikh HK, Wright DC, Wagner DP (1996) Long-term follow-up of patients with meningiomas involving the cavernous sinus: recurrence, progression, and quality of life. Neurosurgery 39:915–919 discussion 919–920
Abdel-Aziz KM, Froelich SC, Dagnew E, Jean W, Breneman JC, Zuccarello M, van Loveren HR, Tew JM, Jr. (2004) Large sphenoid wing meningiomas involving the cavernous sinus: conservative surgical strategies for better functional outcomes. Neurosurgery 54:1375–1383; discussion 1383–1374
Park HJ, Griffin RJ, Hui S, Levitt SH, Song CW (2012) Radiation-induced vascular damage in tumors: implications of vascular damage in ablative hypofractionated radiotherapy (SBRT and SRS). Radiat Res 177:311–327
Song CW, Kim M-SS, Cho LC, Dusenbery K, Sperduto PW (2014) Radiobiological basis of SBRT and SRS. Int J Clin Oncol 19:570–578
Morita A, Coffey RJ, Foote RL, Schiff D, Gorman D (1999) Risk of injury to cranial nerves after gamma knife radiosurgery for skull base meningiomas: experience in 88 patients. J Neurosurg 90:42–49
Lee C-CC, Sheehan JP (2016) Advances in Gamma Knife radiosurgery for pituitary tumors. Cur Opin Endocrinol Diabetes Obes 23:331–338
Sheehan JP, Starke RM, Mathieu D, Young B, Sneed PK, Chiang VL, Lee JY, Kano H, Park K-JJ, Niranjan A, Kondziolka D, Barnett GH, Rush S, Golfinos JG, Lunsford LD (2013) Gamma Knife radiosurgery for the management of nonfunctioning pituitary adenomas: a multicenter study. J Neurosurg 119:446–456
Xu Z, Ellis S, Lee C-CC, Starke RM, Schlesinger D, Lee Vance M, Lopes MB, Sheehan J (2014) Silent corticotroph adenomas after stereotactic radiosurgery: a case-control study. Int J Radiat Oncol Biol Phys 90:903–910
Pichierri A, Santoro A, Raco A, Paolini S, Cantore G, Delfini R (2009) Cavernous sinus meningiomas: retrospective analysis and proposal of a treatment algorithm. Neurosurgery 64:1090
Abeloos L, Levivier M, Devriendt D, Massager N (2007) Internal carotid occlusion following gamma knife radiosurgery for cavernous sinus meningioma. Stereotact Funct Neurosurg 85:303–306
Niranjan A, Gobbel GT, Kondziolka D, Flickinger JC, Lunsford LD (2004) Experimental radiobiological investigations into radiosurgery: present understanding and future directions. Neurosurgery 55:495–504 discussion 504–495
Larson DA, Flickinger JC, Loeffler JS (1993) The radiobiology of radiosurgery. Int J Radiat Oncol Biol Phys 25:557–561
Colombo F, Casentini L, Cavedon C, Scalchi P, Cora S, Francescon P (2009) Cyberknife radiosurgery for benign meningiomas: short-term results in 199 patients. Neurosurgery 64:A7–A13
Conti A, Pontoriero A, Midili F, Iati G, Siragusa C, Tomasello C, La Torre D, Cardali SM, Pergolizzi S, De Renzis C (2015) CyberKnife multisession stereotactic radiosurgery and hypofractionated stereotactic radiotherapy for perioptic meningiomas: intermediate-term results and radiobiological considerations. Springerplus 4:37
Oermann EK, Bhandari R, Chen VJ, Lebec G, Gurka M, Lei S, Chen L, Suy S, Azumi N, Berkowitz F, Kalhorn C, McGrail K, Collins BT, Jean WC, Collins SP (2013) Five fraction image-guided radiosurgery for primary and recurrent meningiomas. Front Oncol 3:213
McTyre E, Helis CA, Farris M, Wilkins L, Sloan D, Hinson WH, Bourland JD, Dezarn WA, Munley MT, Watabe K, Xing F, Laxton AW, Tatter SB, Chan MD (2017) Emerging indications for fractionated gamma knife radiosurgery. Neurosurgery 80:210–216
Messerer M, Dubourg J, Saint-Pierre G, Jouanneau E, Sindou M (2012) Percutaneous biopsy of lesions in the cavernous sinus region through the foramen ovale: diagnostic accuracy and limits in 50 patients. J Neurosurg 116:390–398
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (name of institute/committee) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent was obtained from all individual participants included in the study.
Additional information
Comments
The authors should be commended for the large scale literature review of this challenging pathology. As one would expect, they found the literature varied in terms of the quality and quantity of provided material useful for such meta-analysis. They found that, Gamma Knife technology was used for smaller tumours, fractionated radiotherapy for large lesions and linear accelerator radiosurgery for those in between. Of note, CyberKnife publications did not meet their, in my view fair, criteria. It was also of note that fractionated radiotherapy publications included a wide range of protocols,e.g. the number of fractions ranged between 15 and 30, while the radiosurgery treatments were more similar to each other. Nevertheless, as the authors point out in Discussion, technology is constantly improving. This makes a retrospective review of often retrospective publications that require long follow-up for outcome to be demonstrated always less pertinent for current practice.
In terms of radiological outcome, they noted a significantly larger proportion of tumour shrinkage after gamma knife treatment than in the other groups, while local progression free survival did not significantly differ between the groups. Clinically, the outcomes appeared similar, with functional improvement whichever technology was used, although probably owing to the superior conformity and gradient index of gamma knife treatments there was more improvement of visual acuity when using GK. The authors found scarcity of data in this respect after linear accelerator radiosurgery compared with the more extensively detailed gamma knife publications. Published adverse radiation effects were also similar between the three modalities.
This paper, therefore, supports the perception prevalent amongst clinicians these days. Radiation therapy for cavernous sinus meningiomas is a well-tolerated and successful treatment and it seems to achieve better progression free survival than surgery alone. For smaller lesions, even those with visual impairment, gamma knife treatment is worthwhile and clinical improvement as well as tumour shrinkage is the norm. It is noteworthy that the vast majority of patients, three-quarters in these publications, were treated by gamma knife. The practice, if one goes by publications summarised here, is that larger tumours are treated with fractionated radiotherapy although visual improvement is less expected and in terms of adverse reactions it is not "safer". One will have to await publications upon results of using newer approaches, e.g. volume staging or even fractionation of larger tumours using the latest model of the gamma knife.
Andras Kemeny
Sheffiled, UK
This article is part of the Topical Collection on Tumor - Meningioma
Appendix 1
Appendix 1
Rights and permissions
About this article
Cite this article
Leroy, HA., Tuleasca, C., Reyns, N. et al. Radiosurgery and fractionated radiotherapy for cavernous sinus meningioma: a systematic review and meta-analysis. Acta Neurochir 160, 2367–2378 (2018). https://doi.org/10.1007/s00701-018-3711-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-018-3711-9