Abstract
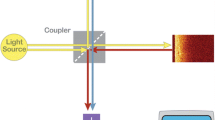
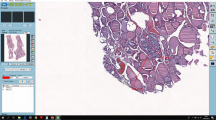
The purpose of this study is twofold: (1) to determine the feasibility of optical coherence tomography (OCT) to differentiate normal and diseased tissue of the neck region intraoperatively and (2) to evaluate how accurately a cohort of test subjects can identify various tissue types when shown a sample set of OCT images. In this in vivo, prospective, single institutional study, an OCT imaging system (Niris, Imalux, Cleveland, OH) was used to image parathyroid, thyroid, lymph node, and fat tissue in 76 patients during neck surgery. Biopsies were performed for comparison of OCT images with histology in select cases (n = 20). Finally, a group of either surgeons or scientists familiar with OCT (n = 17) were shown a sample of OCT images and asked to identify the tissue. A total of 437 OCT images were analyzed, and characteristic features of each tissue type were identified. OCT demonstrated distinct differences in structural architecture and signal intensity that allows differentiation between thyroid and parathyroid tissues, lymph nodes, and fat. OCT images were also compared with histology with good correlation. There was no difference in correctly identifying OCT-imaged tissue type between surgeons and scientists. This study is the first in vivo OCT imaging study to evaluate both normal and diseased tissues that may be encountered during neck surgery. OCT has the potential to become a valuable intraoperative tool to differentiate diseased and normal thyroid tissue intraoperatively to obtain an “optical biopsy” in real time without fixation, staining, or tissue resection.




Similar content being viewed by others
References
Thompson NW, Eckhauser FE, Harness JK (1982) The anatomy of primary hyperparathyroidism. Surgery 92:814–821
Ritter K, Elfenbein D, Schneider DF et al (2015) Hypoparathyroidism after total thyroidectomy: incidence and resolution. J Surg Res 197:348–353. https://doi.org/10.1016/j.jss.2015.04.059
Damadi A, Harkema J, Kareti R, Saxe A (2007) Use of pre-operative Tc99m-Sestamibi scintigraphy and intraoperative parathyroid hormone monitoring to eliminate neck exploration in mediastinal parathyroid adenocarcinoma. J Surg Educ 64:108–112. https://doi.org/10.1016/j.jsurg.2006.10.005
Derom AF, Wallaert PC, Janzing HM, Derom FE (1993) Intraoperative identification of parathyroid glands with methylene blue infusion. Am J Surg 165:380–382. https://doi.org/10.1016/s0002-9610(05)80850-5
McWade MA, Paras C, White LM et al (2013) A novel optical approach to intraoperative detection of parathyroid glands. Surgery 154:1371–1377. https://doi.org/10.1016/j.surg.2013.06.046
Huang D, Swanson E, Lin C et al (1991) Optical coherence tomography. Science 254(80):1178–1181. https://doi.org/10.1126/science.1957169
Fujimoto JG, Brezinski ME, Tearney GJ et al (1995) Optical biopsy and imaging using optical coherence tomography. Nat Med 1:970–972. https://doi.org/10.1038/nm0995-970
Wong BJF, Jackson RP, Guo S et al (2005) In vivo optical coherence tomography of the human larynx: normative and benign pathology in 82 patients. Laryngoscope 115:1904–1911. https://doi.org/10.1097/01.MLG.0000181465.17744.BE
Hirano K, Ito Y, Suzuki T et al (2001) Optical coherence tomography for the noninvasive evaluation of the cornea. Cornea 20:281–289. https://doi.org/10.1097/00003226-200104000-00009
Welzel J (2001) Optical coherence tomography in dermatology: a review. Skin Res Technol 7:1–9
McLaughlin RA, Scolaro L, Robbins P et al (2010) Imaging of human lymph nodes using optical coherence tomography: potential for staging cancer. Cancer Res 70:2579–2584. https://doi.org/10.1158/0008-5472.CAN-09-4062
Kala P, Cervinka P, Jakl M et al (2018) OCT guidance during stent implantation in primary PCI: a randomized multicenter study with nine months of optical coherence tomography follow-up. Int J Cardiol 250:98–103. https://doi.org/10.1016/j.ijcard.2017.10.059
Turani Z, Fatemizadeh E, Blumetti T et al (2019) Optical radiomic signatures derived from optical coherence tomography images improve identification of melanoma. Cancer Res 79:2021–2030. https://doi.org/10.1158/0008-5472.CAN-18-2791
Adabi S, Hosseinzadeh M, Noei S et al (2017) Universal in vivo textural model for human skin based on optical coherence tomograms. Sci Rep 7:17912. https://doi.org/10.1038/s41598-017-17398-8
Garcia Garrido M, Beck SC, Mühlfriedel R et al (2014) Towards a quantitative OCT image analysis. PLoS One 9. https://doi.org/10.1371/journal.pone.0100080
Djalilian HR, Ridgway J, Tam M et al (2008) Imaging the human tympanic membrane using optical coherence tomography in vivo. Otol Neurotol 29:1091–1094. https://doi.org/10.1097/MAO.0b013e31818a08ce
Djalilian HR, Rubinstein M, Wu EC et al (2010) Optical coherence tomography of cholesteatoma. Otol Neurotol 31:932–935
Mahmood U, Ridgway J, Jackson R et al In vivo optical coherence tomography of the nasal mucosa. Am J Rhinol 20:155–159
Englhard AS, Wiedmann M, Ledderose GJ et al (2018) In vivo imaging of the internal nasal valve during different conditions using optical coherence tomography. Laryngoscope 128:E105–E110. https://doi.org/10.1002/lary.26962
Englhard AS, Wiedmann M, Ledderose GJ et al (2016) Imaging of the internal nasal valve using long-range Fourier domain optical coherence tomography. Laryngoscope 126:E97–E102. https://doi.org/10.1002/lary.25785
Jerjes W, Upile T, Conn B et al (2010) In vitro examination of suspicious oral lesions using optical coherence tomography. Br J Oral Maxillofac Surg 48:18–25. https://doi.org/10.1016/j.bjoms.2009.04.019
Ridgway JM, Armstrong WB, Guo S et al (2006) In vivo optical coherence tomography of the human oral cavity and oropharynx. Arch Otolaryngol Neck Surg 132:1074. https://doi.org/10.1001/archotol.132.10.1074
Wang Y, Bachman M, Li G-P et al (2005) Low-voltage polymer-based scanning cantilever for in vivo optical coherence tomography. Opt Lett 30:53–55. https://doi.org/10.1364/ol.30.000053
Kimbell JS, Basu S, Garcia GJM et al (2019) Upper airway reconstruction using long-range optical coherence tomography: effects of airway curvature on airflow resistance. Lasers Surg Med 51:150–160. https://doi.org/10.1002/lsm.23005
Jing JC, Chou L, Su E et al (2016) Anatomically correct visualization of the human upper airway using a high-speed long range optical coherence tomography system with an integrated positioning sensor. Sci Rep 6:39443. https://doi.org/10.1038/srep39443
Jing J, Zhang J, Loy AC et al (2012) High-speed upper-airway imaging using full-range optical coherence tomography. J Biomed Opt 17:110507
Ridgway JM, Ahuja G, Guo S et al (2007) Imaging of the pediatric airway using optical coherence tomography. Laryngoscope 117:2206–2212. https://doi.org/10.1097/MLG.0b013e318145b306
Ridgway JM, Su J, Wright R et al (2008) Optical coherence tomography of the newborn airway. Ann Otol Rhinol Laryngol 117:327–334
Lazarow FB, Ahuja GS, Chin Loy A et al (2015) Intraoperative long range optical coherence tomography as a novel method of imaging the pediatric upper airway before and after adenotonsillectomy. Int J Pediatr Otorhinolaryngol 79:63–70. https://doi.org/10.1016/j.ijporl.2014.11.009
Armstrong WB, Ridgway JM, Vokes DE et al (2006) Optical coherence tomography of laryngeal cancer. Laryngoscope 116:1107–1113. https://doi.org/10.1097/01.mlg.0000217539.27432.5a
Sepehr A, Armstrong WB, Guo S et al (2008) Optical coherence tomography of the larynx in the awake patient. Otolaryngol Neck Surg 138:425–429. https://doi.org/10.1016/j.otohns.2007.12.005
Kraft M, Glanz H, von Gerlach S et al (2008) Clinical value of optical coherence tomography in laryngology. Head Neck 30:1628–1635. https://doi.org/10.1002/hed.20914
Coughlan CA, Chou L, Jing JC et al (2016) In vivo cross-sectional imaging of the phonating larynx using long-range Doppler optical coherence tomography. Sci Rep 6:22792. https://doi.org/10.1038/srep22792
Rubinstein M, Fine EL, Sepehr A et al (2010) Optical coherence tomography of the larynx using the Niris system. J Otolaryngol Head Neck Surg 39:150–156
Guo S, Yu L, Sepehr A et al (2009) Gradient-index lens rod based probe for office-based optical coherence tomography of the human larynx. J Biomed Opt 14:014017. https://doi.org/10.1117/1.3076198
Burns JA, Kim KH, Kobler JB et al (2009) Real-time tracking of vocal fold injections with optical coherence tomography. Laryngoscope 119:2182–2186. https://doi.org/10.1002/lary.20654
Burns JA, Zeitels SM, Anderson RR et al (2005) Imaging the mucosa of the human vocal fold with optical coherence tomography. Ann Otol Rhinol Laryngol 114:671–676. https://doi.org/10.1177/000348940511400903
Yu L, Liu G, Rubinstein M et al (2009) Office-based dynamic imaging of vocal cords in awake patients with swept-source optical coherence tomography. J Biomed Opt 14:064020. https://doi.org/10.1117/1.3268442
Guo S, Hutchison R, Jackson RP et al (2006) Office-based optical coherence tomographic imaging of human vocal cords. J Biomed Opt 11:030501. https://doi.org/10.1117/1.2200371
Vokes DE, Jackson R, Guo S et al (2008) Optical coherence tomography—enhanced microlaryngoscopy: preliminary report of a noncontact optical coherence tomography system integrated with a surgical microscope. Ann Otol Rhinol Laryngol 117:538–547. https://doi.org/10.1177/000348940811700713
Jing JC, Chen JJ, Chou L et al (2017) Visualization and detection of ciliary beating pattern and frequency in the upper airway using phase resolved Doppler optical coherence tomography. Sci Rep 7:8522. https://doi.org/10.1038/s41598-017-08968-x
Pantanowitz L, Hsiung P-L, Ko TH et al (2004) High-resolution imaging of the thyroid gland using optical coherence tomography. Head Neck 26:425–434. https://doi.org/10.1002/hed.10392
Zhou C, Wang Y, Aguirre AD et al (2010) Ex vivo imaging of human thyroid pathology using integrated optical coherence tomography and optical coherence microscopy. J Biomed Opt 15:016001. https://doi.org/10.1117/1.3306696
Ladurner R, Hallfeldt KKJ, Al Arabi N et al (2013) Optical coherence tomography as a method to identify parathyroid glands. Lasers Surg Med 45:654–659. https://doi.org/10.1002/lsm.22195
Conti de Freitas LC, Phelan E, Liu L et al (2013) Optical coherence tomography imaging during thyroid and parathyroid surgery: a novel system of tissue identification and differentiation to obviate tissue resection and frozen section. Head Neck 36:n/a–n/a. https://doi.org/10.1002/hed.23452
Hou F, Yu Y, Liang Y (2017) Automatic identification of parathyroid in optical coherence tomography images. Lasers Surg Med 49:305–311. https://doi.org/10.1002/lsm.22622
Sommerey S, Al Arabi N, Ladurner R et al (2015) Intraoperative optical coherence tomography imaging to identify parathyroid glands. Surg Endosc 29:2698–2704. https://doi.org/10.1007/s00464-014-3992-x
Yang N, Boudoux C, De Montigny E et al (2019) Rapid head and neck tissue identification in thyroid and parathyroid surgery using optical coherence tomography. Head Neck. https://doi.org/10.1002/hed.25972
Armstrong WB, Naemi K, Keel S et al (2010) Intraoperative use of OCT in endocrine surgery. Otolaryngol Neck Surg 143:P63–P63. https://doi.org/10.1016/j.otohns.2010.06.075
Tyshlek D, Aubry J-F, Ter Haar G et al (2014) Focused ultrasound development and clinical adoption: 2013 update on the growth of the field. J Ther ultrasound 2:2. https://doi.org/10.1186/2050-5736-2-2
Funding
This work was supported by the National Institutes of Health (DC 006026, CA 91717, EB 00293, RR 01192, RR00827), Flight Attendant Medical Research Institute (32456), State of California Tobacco Related Disease Research Program (12RT-0113), Air Force Office of Scientific Research (F49620_00_1_0371), and the Arnold and Mabel Beckman Foundation.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rubinstein, M., Hu, A.C., Chung, PS. et al. Intraoperative use of optical coherence tomography to differentiate normal and diseased thyroid and parathyroid tissues from lymph node and fat. Lasers Med Sci 36, 269–278 (2021). https://doi.org/10.1007/s10103-020-03024-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-020-03024-z