Abstract
Background
Admissions for ambulatory care sensitive conditions (ACSCs) are considered preventable and indicators of poor access to primary care. We wondered whether per-capita rates of admission for ACSCs in France demonstrated geographic variation, were changing, were related to other independent variables, or were comparable to those in other countries; further, we wanted to quantify the resources such admissions consume.
Methods
We calculated per-capita rates of admission for five categories (chronic, acute, vaccination preventable, alcohol-related, and other) of ACSCs in 94 departments in mainland France in 2009 and 2010, examined measures and causes of geographic variation in those rates, computed the costs of those admissions, and compared rates of admission for ACSCs in France to those in several other countries.
Results
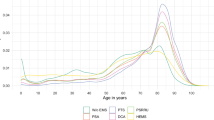
The highest ACSC admission rates generally occurred in the young and the old, but rates varied across French regions. Over the 2-year period, rates of most categories of ACSCs increased; higher ACSC admission rates were associated with lower incomes and a higher supply of hospital beds. We found that the local supply of general practitioners was inversely associated with rates of chronic and total ACSC admission rates, but that this relationship disappeared if we accounted for patients’ use of general practitioners in neighboring departments. ACSC admissions cost 4.755 billion euros in 2009 and 5.066 billion euros in 2010; they consumed 7.86 and 8.74 million bed days of care, respectively. France had higher rates of ACSC admissions than most other countries examined.
Conclusions
Because admissions for ACSCs are generally considered a failure of outpatient care, cost French taxpayers substantial monetary and hospital resources, and appear to occur more frequently in France than in other countries, policymakers should prioritize targeted efforts to reduce them.





Similar content being viewed by others
References
McCulloch, P., Nagendran, M., Campbell, W.B., Price, A., Jani, A., Birkmeyer, J.D., Gray, M.: Strategies to reduce variation in the use of surgery. Lancet 382(9898), 1130–1139 (2013)
Wennberg, J.E.: Tracking medicine: a researcher’s quest to understand health care. Oxford University Press, New York (2010)
Wennberg, J.E.: The Dartmouth atlas project. http://www.dartmouthatlas.org (2012). Accessed July 11 2014
Birkmeyer, J.D., Sharp, S.M., Finlayson, S.R., Fisher, E.S., Wennberg, J.E.: Variation profiles of common surgical procedures. Surgery 124, 917–923 (1998)
Corallo, A.N., Croxford, R., Goodman, D.C., Bryan, E.L., Srivastava, D., Stukel, T.A.: A systematic review of medical practice variation in OECD countries. Health Policy 114(1), 5–14 (2014)
Weeks, W.B., Paraponaris, A., Ventelou, B.: Geographic variation in rates of common surgical procedures in France in 2008–2010, and comparison to the US and Britain. Health Policy 118(2), 215–221 (2014)
Freund, T., Campbell, S.M., Geissler, S., Kunz, C.U., Mabler, C., Peters-Klimm, F., Szecsenyi, J.: Strategies for reducing potentially avoidable hospitalizations for ambulatory care sensitive conditions. Ann Fam Med 11(4), 363–370 (2013)
Ambulatory care-sensitive conditions. http://www.dartmouthatlas.org/data/table.aspx?ind=198. Accessed July 11 2014. In: The Dartmouth atlas of health care, The Dartmouth Institute for Health Policy and Clinical Practice: Lebanon, NH
Chen, L.W., Zhang, W., Sun, J., Mueller, K.J.: The magnitude, variation, and determinants of rural hospital resource utilization associated with hospitalization due to ambulatory care sensitive conditions. J. Public Health Manag. Prac. 15(3), 216–222 (2009)
Chang, C.H., Stukel, T.A., Flood, A.B., Goodman, D.C.: Primary care physician workforce and Medicare beneficiaries’ health outcomes. JAMA 305(20), 2096–2105 (2011)
Sanchez, M., Vellanky, S., Herring, J., Liang, J., Jia, H.: Variations in Canadian rates of hospitalization for ambulatory care sensitive conditions. Healthc. Q. 11(4), 20–22 (2008)
Ansari, Z., Carson, N., Serraglio, A., Barbetti, T., Cicuttini, F.: The Victorian ambulatory care sensitive conditions study: reducing demand on hospital services in Victoria. Aust. Health Rev. 25(2), 71–77 (2002)
Ansari, Z., Rowe, S., Ansari, H., Sindall, C.: Small area analysis of ambulatory care sensitive conditions in Victoria, Australia. Popul. Health Manag. 16(3), 190–200 (2013)
Agabiti, N., Pirani, M., Schifano, P., Cesaroni, G., Davoli, M., Bisanti, L., Caranci, N., Costa, G., Forastiere, F., Marinacci, C., Russo, A., Spadea, T., Perucci, C.A.: Income level and chronic ambulatory care sensitive conditions in adults: a multicity population-based study in Italy. BMC Public Health 9, 457 (2009)
Magan, P., Otero, A., Alberquilla, A., Ribera, J.: Geographic variations in avoidable hospitalization in the elderly, in a health system with universal coverage. BMC Health Serv Res 8, 42 (2008)
Sheridan, A., Howell, F., Bedford, D.: Hospitalisations and costs related to ambulatory care sensitive conditions in Ireland. Ir. J. Med. Sci. 181, 527–533 (2012)
Niti, M., Ng, T.P.: Avoidable hospitalisation rates in Singapore, 1991–1998: assessing trends and inequities of quality in primary care. J. Epidemiol. Community Health 57, 17–22 (2003)
Blunt, I.: Focus on preventable admissions—trends in emergency admissions for ambulatory care sensitive conditions, 2001 to 2013. The Health Foundation and the Nuffield Trust: http://www.health.org.uk/publications/focus-on-preventable-admissions (2013). Accessed 11 July 2014
Tian, I., Dixon, A., Gao, H.: Data briefing—emergency hospital admissions for ambulatory care-sensitive conditions: identifying the potential for reductions. The Kingʼs Fund: http://www.kingsfund.org.uk/publications/data-briefing-emergency-hospital-admissions-ambulatory-care-sensitive-conditions (2012). Accessed 11 July 2014
Naylor, C., Imison, C., Addicott, R., Buck, D., Goodwin, N., Harrison, T., Ross, S., Sonola, L., Tian, Y., Curry, N.: The Kingʼs Fund: transforming our health care system. http://www.kingsfund.org.uk/sites/files/kf/field/field_publication_file/10PrioritiesFinal2.pdf (2013). Accessed 11 July 2014, The King’s Fund
Macinko, J., Dourado, I., Aquino, R., Bonolo, P.F., Lima-Costa, M.F., Medina, M.G., Mota, E., de Oliveira, V.B., Turci, M.A.: Major expansion of primary care in Brazil linked to decline in unnecessary hospitalization. Health Aff. 29(12), 2149–2160 (2010)
Junqeira, R.M.P., Duarte, E.C.: Hospitalizations due to ambulatory care-sensitive conditions in the Federal District, Brazil, 2008, R.S. Pública, Editor 2011, Universidade de Brasília. Brasília, DF, Brasil
Eggli, Y., Besquins, B., Seker, E., Halfon, P.: Comparing potentially avoidable hospitalization rates related to ambulatory care sensitive conditions in Switzerland: the need to refine the definition of health conditions and to adjust for population health status. BMC Health Serv. Res. 14, 25 (2014)
Burgdorf, F., Sundmacher, L.: Potentially avoidable hospital admissions in Germany: an analysis of factors influencing rates of ambulatory care sensitive hospitalizations. Deutsches Ärzteblatt Int. 111(13), 215–223 (2014)
Gusmano, M.K., Weisz, D., Rodwin, V.G., Lang, J., Qian, M., Bocquier, A., Moysan, V., Verger, P.: Disparities in access to health care in three French regions. Health Policy 114(1), 31–40 (2014)
Thygesen, L.C., Christiansen, T., Garcia-Armesto, S., Angulo-Pueyo, E., Martinez-Lizaga, N., Bernal-Delgado, E.: Potentially avoidable hospitalizations in five European countries in 2009 and time trends from 2002 to 2009 based on administrative data. Eur. J. Public Health 25(Suppl 1), 35–43 (2015)
Agence Technique de l’Information sur l’Hospitalisation (ATIH). http://www.atih.sante.fr/echelle-nationale-de-couts-par-ghm (2014). Accessed 22 October 2014
WHO mental health atlas: World Health Organization: Geneva (2011)
World Health Organization. Projections of mortality and burden of disease, 2004–2030 for 2008 by World Bank income groups, standard DALYs, (3 % discounting, age weights). http://www.who.int/healthinfo/global_burden_disease/projections2004/en/. [cited 2014 September 19]
Gustavsson, A., Svensson, M., Jacobi, F., Allgulander, C., Alonso, J., Beghi, E., Dodel, R., Ekman, M., Faravelli, C., Fratiglioni, L., Gannon, B., Jones, D.H., Jennum, P., Jordanova, A., Jonsson, L., Karampampa, K., Knapp, M., Kobelt, G., Kurth, T., Lieb, R., Linde, M., Ljungcrantz, C., Maercker, A., Melin, B., Moscarelli, M., Musayev, A., Norwood, F., Preisig, M., Pugliatti, M., Rehm, J., Salvador-Carulla, L., Schlehofer, B., Simon, R., Steinhausen, H.C., Stovner, L.J., Vallat, J.M., Van den Bergh, P., van Os, J., Vos, P., Xu, W., Wittchen, H.U., Jonsson, B., Olesen, J., C.D. Group: Cost of disorders of the brain in Europe 2010. Eur. Neuropsychopharmacol. 21(10), 718–779 (2011). .[Erratum appears in Eur Neuropsychopharmacol. 2012 Mar;22(3):237–8 Note: den Bergh, Peter Van [corrected to Van den Bergh, Peter]]
The Dartmouth atlas of health care: indirect adjustment. http://www.dartmouthatlas.org/downloads/methods/indirect_adjustment.pdf. Accessed 11 July 2014
Résultats du recensement de la population—2009: POP1B—population par sexe et âge. http://www.recensement.insee.fr/basesTableauxDetaillesTheme.action?idTheme=12 (2009). Accessed 11 July 2014. INSEE—Institut national de la statistique et des études économiques: Paris, France
The Dartmouth atlas of health care: research methods. http://www.dartmouthatlas.org/downloads/methods/research_methods.pdf. Accessed 11 July 2014: Hanover, NH
Statistique annuelle des établissements de santé exercice—2010. http://www.data.gouv.fr/content/search?SortBy=Pertinence&SortOrder=0&SearchText=sae+statistique (2012). Accessed 11 July 2014, Ministère du Travail, de l’Emploi et de la Santé
Eco-Santé 2013: Offre de biens et services medicaux; Démographie professions de santé et Distances accès; Médecins; Psychiatres et Neuro-psychiatres Ensemble; effectif http://www.ecosante.fr/. Accessed 22 October 2014
Appleby, J., Raleigh, V., Frosini, F., Bevan, G., Gao, H., Lyscom, T.: Variations in health care: the good, the bad and the inexplicable, The Kingʼs Fund: London (2011)
Birkmeyer, J.D., Reames, B.N., McCulloch, P., Carr, A.J., Campbell, W.B., Wennberg, J.E.: Understanding of regional variation in the use of surgery. Lancet 382(9898), 1121–1129 (2013)
McPherson, K., Wennberg, J.E., Hoving, O.B., Clifford, P.: Small-area variations in the use of common surgical procedures: an international comparison of New England, England, and Norway. N. Engl. J. Med. 307, 1310–1314 (1982)
Annuaire ANDASS des données sociales et de santé 2008 des Conseils généraux, Édition n 15, 2010, Association Nationale des Directeurs d’Action Sociale et de Santé des Conseils généraux: Paris
Peters, D.J.: American income inequality across economic and geographic space, 1970–2010. Soc. Sci. Res. 42(6), 1490–1594 (2013)
Berrigan, D., Tatalovich, Z., Pickle, L.W., Ewing, R., Ballard-Barbash, R.: Urban sprawl, obesity, and cancer mortality in the United States: cross-sectional analysis and methodological challenges. Int. J. Health Geogr. 13(1), 3 (2014)
Anselin, L., Syabri, I., Kho, Y.: GeoDa: an introduction to spatial data analysis. Geogr. Anal. 38(1), 5–22 (2006)
Welch, H.G., Sharp, S.M., Gottlieb, D.J., Skinner, J.S., Wennberg, J.E.: Geographic variation in diagnosis frequency and risk of death among Medicare beneficiaries. JAMA 305(11), 1113–1118 (2011)
Song, Y., Skinner, J., Bynum, J., Sutherland, J., Wennberg, J.E., Fisher, E.S.: Regional variations in diagnostic practices.[Erratum appears in N Engl J Med. 2010 Jul 8;363(2):198]. N. Engl. J. Med. 363(1), 45–53 (2010)
Lucas, F.L., Sirovich, B.E., Gallagher, P.M., Siewers, A.E., Wennberg, D.E.: Variation in cardiologists’ propensity to test and treat: is it associated with regional variation in utilization? Circul. Cardiovasc. Qual. Outcomes 3(3), 253–260 (2010)
Sirovich, B., Gallagher, P.M., Wennberg, D.E., Fisher, E.S.: Discretionary decision making by primary care physicians and the cost of U.S. health care. Health Aff. 27(3), 813–823 (2008)
Sirovich, B.E., Gottlieb, D.J., Welch, H.G., Fisher, E.S.: Variation in the tendency of primary care physicians to intervene. Arch. Intern. Med. 165(19), 2252–2256 (2005)
Thomson, S., Osborn, R., Squires, D., Jun, M.: International profiles of health care systems, 2013. http://www.commonwealthfund.org/~/media/Files/Publications/FundReport/2013/Nov/1717_Thomson_intl_profiles_hlt_care_sys_2013_v2.pdf, (2013), The Commonwealth Fund: New York, NY
Fenina, A., Le Carrec, M., Koubi, M.: Comptes nationaux de la santé, 2010. N 161—Septembre 2011. http://www.drees.sante.gouv.fr/IMG/pdf/seriestat161.pdf (2011), Direction de la recherche, des études, de l’évaluation et des statistiques (DREES)
Bocquier, A., Cortarendona, S., Nauleau, S., Jardin, M., Verger, P.: Prevalence of treated diabetes: geographical variations at the small-area level and their association with area-level characteristics. A multilevel analysis in southeastern France. Diabetes Metab. 37(1), 39–46 (2011)
Conflict of interest
The authors have no conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Appendix: an example of bed reassignment
Appendix: an example of bed reassignment
In 2009 and 2010, hospitals in the Ain department (department 01) used 581 medical beds to provide 14,399 hospitalizations for ACSCs. Although 12,968 admissions were for patients who lived in Ain, the balance of patients lived in 66 different French departments; for example, 437 admissions were for patients from the neighboring Jura department (department 39). Those 437 bed days represented 3.1 % of all 14,092 admissions for ACSCs that were provided by hospitals in Jura, a department with 549 medical beds. Therefore, we reallocated 17.02 medical beds from Ain to Jura for the purposes of determining bed supply for Jura patients. However, 12,140 admissions for patients who lived in Ain occurred in hospitals outside of Ain, 6683 of which were obtained in Rhône (department 69). Using its 3759 medical beds, Rhône hospitals provided 90,073 hospitalizations for ACSCs in 2009–2010. Therefore, we reallocated 7.4 % of these beds, or 278.9 surgical beds from Rhône to Ain. After allocation from and to other French departments, we calculated that Ain had an adjusted supply of 1033 medical beds, while Jura had an adjusted supply of 614 medical beds, and Rhône had an adjusted supply of 3053 surgical beds.
Rights and permissions
About this article
Cite this article
Weeks, W.B., Ventelou, B. & Paraponaris, A. Rates of admission for ambulatory care sensitive conditions in France in 2009–2010: trends, geographic variation, costs, and an international comparison. Eur J Health Econ 17, 453–470 (2016). https://doi.org/10.1007/s10198-015-0692-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10198-015-0692-y
Keywords
- Ambulatory care sensitive conditions
- Preventable admissions
- Potential cost savings
- International comparisons