Abstract
Objective
This systematic review sought to evaluate the clinical outcomes of vitrification at the cleavage stage and blastocyst stage for embryo transfer in patients undergoing assisted reproductive technology (ART) treatment.
Methods
We searched for related comparative studies published in the PubMed, EMBASE, and Cochrane Library databases up to July 2017. The primary outcomes were clinical pregnancy rate (CPR) and embryo implantation rate (IR). Secondary outcomes were multiple pregnancy rate (MPR), miscarriage rate (MR), live birth rate (LBR), and ongoing pregnancy rate (OPR). The Mantel-Haenszel fixed effects model and random effects model were used to analyze the summary risks ratios (RRs) with 95% confidence intervals (CIs).
Results
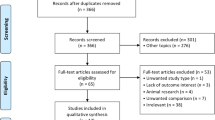
Eight studies with more than 6590 cycles were included in our meta-analysis. Seven studies were observational retrospective comparative studies. One was a prospective study. Overall, the current study summarizes information from 6590 vitrification warming cycles (cleavage stage n = 4594; blastocysts n = 1996). There was no difference in the primary outcome clinical pregnancy rate (RR = 0.97, 95% CI = 0.90–1.04; fixed effects model; I 2 = 21%), whereas vitrified blastocyst transfer was significantly superior to vitrified cleavage-stage embryo transfer regarding the implantation rate (RR = 0.85, 95% CI = 0.74–0.97; random effects model; I 2 = 43). Regarding the secondary outcomes, no differences were found in the multiple pregnancy rate (RR = 1.20, 95% CI = 0.79–1.82; fixed effects model; I 2 = 22), live birth rate (RR = 1.07, 95% CI = 0.98–1.16; fixed effects model; I 2 = 0), and ongoing pregnancy rate (RR = 1.01, 95% CI = 0.92–1.120; fixed effects model; I 2 = 0), whereas a higher miscarriage rate was observed with vitrified blastocyst transfer (RR = 0.65, 95% CI = 0.45–0.93; random effects model; I 2 = 23).
Conclusion
In summary, this meta-analysis shows that vitrification at any stage has no detrimental effect on clinical outcome. Blastocyst transfer will still remain a favorable and promising option in ART. Due to the small sample evaluated in the pool of included studies, large-scale, prospective, and randomized controlled trials are required to determine if these small effects are clinically relevant.








Similar content being viewed by others
References
Trounson A, Mohr L. Human pregnancy following cryopreservation, thawing and transfer of an eight-cell embryo. Nature. 1998;3(305):707–9.
Ozgur K, et al. Perinatal outcomes after fresh versus vitrified-warmed blastocyst transfer: retrospective analysis. Fertil Steril. 2015;104(4):899–907.
Li Z, et al. Clinical outcomes following cryopreservation of blastocysts by vitrification or slow freezing: a population-based cohort study. Hum Reprod. 2014;29:2794–801.
Wikland M, et al. Obstetric outcomes after transfer of vitrified blastocysts. Hum Reprod. 2010;25:1699–707.
Wong KM, Mastenbroek S, Repping S. Cryopreservation of human embryos and its contribution to in vitro fertilization success rates. Fertil Steril. 2014;102:19–26.
Zhu HY, et al. Slow freezing should not be totally substituted by vitrification when applied to day 3 embryo cryopreservation: an analysis of 5613 frozen cycles. J Assist Reprod Genet. 2015;32:1371–7.
Kolibianakis EM, Venetis CA, Tarlatzis BC. Cryopreservation of human embryos by vitrification or slow freezing: which one is better? Curr Opin Obstet Gynecol. 2009;21:270–4.
Rezazadeh Valojerdi M, et al. Vitrification versus slow freezing gives excellent survival, post warming embryo morphology and pregnancy outcomes for human cleaved embryos. J Assist Reprod Genet. 2009;26(6):347–54.
Balaban B, et al. A randomized controlled study of human day 3 embryo cryopreservation by slow freezing or vitrification: vitrification is associated with higher survival, metabolism and blastocyst formation. Hum Reprod. 2008;23:1976–82.
Rall WF, Fahy GM. Ice-free cryopreservation of mouse embryos at -196 C by vitrification. Nature. 1985;313:573–5.
Wong YY, Wong YK. Phasing-in of vitrification into routine practice: why, how, and what. Hong Kong Med J. 2011;17:119–26.
Belva F, et al. Neonatal health including congenital malformation risk of 1072 children born after vitrified embryo transfer. Hum Reprod. 2016;10:1093.
Cobo A, et al. Outcomes of vitrified early cleavage-stage and blastocyst-stage embryos in a cryopreservation program: evaluation of 3,150 warming cycles. Fertil Steril. 2012;98(5):1138–1146.e1.
Wilding MG, et al. Human cleavage-stage embryo vitrification is comparable to slowrate cryopreservation in cycles of assisted reproduction. J Assist Reprod Genet. 2010;27:549–54.
Nakashima A, et al. Optimization of a novel nylon mesh container for human embryo ultrarapid vitrification. Fertil Steril. 2010;93:24052410.
Schoolcraft WB, et al. Clinical application of comprehensive chromosomal screening at the blastocyst stage. Fertil Steril. 2010;94:1700–6.
Raju GA, et al. Vitrification of human early cavitating and deflated expanded blastocysts: clinical outcome of 474 cycles. J Assist Reprod Genet. 2009;26:523–9.
Vanderzwalmen P, et al. Aseptic vitrification of blastocysts from infertile patients, egg donors and after IVM. Reprod BioMed Online. 2009;19:700–7.
van Landuyt L, et al. Outcome of closed blastocyst vitrification in relation to blastocyst quality: evaluation of 759 warming cycles in a single-embryo transfer policy. Hum Reprod. 2011;26:527–34.
Liebermann J. Vitrification of human blastocysts: an update. 2009. Reprod BioMed Online. 2009;19 Suppl 4:4328.
Jacobsen IA, Pegg DE, et al. Effect of cooling and warming rate on glycerolized rabbit kidneys. Cryobiology. 1984;21:637–53.
Pegg DE. Ice crystals in tissues and organs. In: Pegg DE, Karow Jr AM, editors. The biophysics of organ preservation. New York: Plenum; 1987. p. 117–40.
Rubinsky B, Pegg ED. A mathematical model for the freezing process in biological tissue. Proc R Soc Lond. 1988;234:343–58.
De Vos A, et al. Cumulative live birth rates after fresh and vitrified cleavage-stage versus blastocyst-stage embryo transfer in the first treatment cycle. Hum Reprod. 2016;31(11):2442–9.
Desai N, et al. What is the optimal stage for embryo vitrification-a comparison of embryo survival and clinical outcomes with day 3 cleavage versus blastocyst stage vitrification. Fertil Steril. 2010;94(4):S110.
Desai N, et al. The new Rapid-i carrier is an effective system for human embryo vitrification at both the blastocyst and cleavage stage. Reprod Biol Endocrinol. 2013;11(44):2–9.
Lee JH, et al. Effect of day-3 embryo and day-5 blastocyst stage at vitrification on clinical outcome of cryopreserved-embryo transfer cycles. Stockholm: Annual Meeting of ESHRE; 2011.
Shaw SF. Ongoing and cumulative pregnancy rate after cleavage-stage versus blastocyst-stage embryo transfer using vitrification for cryopreservation: impact of age on the results. J Assist Reprod Genet. 2015;32:177–84.
Sugiyama R, et al. Clinical outcomes resulting from the transfer of vitrified human embryos using a new device for cryopreservation (plastic blade). J Assist Reprod Genet. 2010;27(4):161–7.
Tong GQ, et al. Clinical outcome of fresh and vitrified-warmed blastocyst and cleavage-stage embryo transfers in ethnic Chinese ART patients. J Ovarian Res. 2012;5:27.
Kamath M, et al. Comparison of clinical outcomes following vitrified warmed day 5/6 blastocyst transfers using solid surface methodology with fresh blastocyst transfers. J Hum Reprod Sci. 2013;6(1):59.
Zhu D, et al. Vitrified-warmed blastocyst transfer cycles yield higher pregnancy and implantation rates compared with fresh blastocyst transfer cycles—time for a new embryo transfer strategy? Fertil Steril. 2011;95(5):1691–5.
Han AR, et al. Blastocyst transfer in frozen-thawed cycles. Clin Exp Reprod Med. 2012;39(3):114–7.
Blake D, et al. Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology (Review). Cochrane Libr. 2011;10
Papanikolaou EG, et al. In vitro fertilization with single blastocyst-stage versus single cleavage-stage embryos. N Engl J Med. 2006;354:1139–46.
SILLS ES, Palermo DG. Human blastocyst culture in IVF: current laboratory applications in reproductive medicine practice. Morphol Embryol. 2010;51(3):441–5.
Fanchin R, et al. Uterine contractility decreases at the time of blastocyst transfers. Hum Reprod. 2001;16:1115–9.
Ata B, et al. Array CGH analysis shows that aneuploidy is not related with the number of embryos generated. Reprod BioMed Online. 2012;24:614–20.
Carvalho BR, et al. Embryo stage of development is not decisive for reproductive outcomes in frozen-thawed embryo transfer cycles. JBRA Assist Reprod. 2017;21(1):23–6.
Fatemi HM, Popovic-Todorovic B. Implantation in assisted reproduction: a look at endometrial receptivity. Reprod BioMed Online. 2013;27:530–8.
Glujovsky D, et al. Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology. Cochrane Database Syst Rev. 2012;7:CD002118.
Berkkanoglu M, et al. Optimal embryo transfer strategy in poor response may include freeze-all. J Assist Reprod Genet. 2016;34(1):79–87.
Marek D, et al. Introduction of blastocyst culture and transfer for all patients in an in vitro fertilization program. Fertil Steril. 1999;72:1035e40.
Papanikolaou EG, et al. Live birth rates after transfer of equal number of blastocysts or cleavage-stage embryos in IVF. A systematic review and meta-analysis. Hum Reprod. 2008;23:91e9.
Practice Committee of the American Society for Reproductive Medicine.Practice Committee of the Society for Assisted Reproductive Technology. Blastocyst culture and transfer in clinical-assisted reproduction. Fertil Steril. 2006;86:S89e92.
Dar S, et al. Increased risk of preterm birth in singleton pregnancies after blastocyst versus day 3 embryo transfer: Canadian ART Register (CARTR) analysis. Hum Reprod. 2013;28:924e8.
Niemitz EL, Feinberg AP. Epigenetics and assisted reproductive technology: a call for investigation. Am J Hum Genet. 2004;74:599e609.
Chang HJ, et al. Impact of blastocyst transfer on offspring sex ratio and the monozygotic twinning rate: a systematic review and meta-analysis. Fertil Steril. 2009;91:2381e90.
Blake D, et al. Cleavage stage versus blastocyst stage embryo transfer in assisted conception. Cochrane Collab. 2005;4:CD002118.
Hreinsson J, et al. Embryo transfer is equally effective at cleavage stage and blastocyst stage: a randomized prospective study. Eur J Obstet Gynecol Reprod Biol. 2004;117(2):194–200.
Seki S, Mazur P. The dominance of warming rate over cooling rate in the survival of mouse oocytes subjected to a vitrification procedure. Cryobiology. 2009;59:75–82.
Desai N, et al. Artificial collapse of blastocysts before vitrification: mechanical vs. laser technique and effect on survival, cell number, and cell death in early and expanded blastocysts. Biopreserv Biobank. 2008;6:181–90.
Martins WP, et al. Assisted hatching of human embryos: a systematic review and meta-analysis of randomized controlled trials. Hum Reprod Update. 2011;17(4):438–53.
Zhu L, et al. Blastocyst culture and cryopreservation to optimize clinical outcomes of warming cycles. Reprod BioMed Online. 2013;27(2):154–60.
Feng GX, et al. Comparable clinical outcomes and live births after single vitrified–warmed and fresh blastocyst transfer. Reprod BioMed Online. 2012;25:466–73.
Ku P-Y, et al. Comparison of the clinical outcomes between fresh blastocyst and vitrified-thawed blastocyst transfer. J Assist Reprod Genet. 2012;29(12):1353–6.
Edi-Osagie E, Hooper L, Seif MW. The impact of assisted hatching on live birth rates and outcomes of assisted conception: a systematic review. Hum Reprod. 2003;18(9):1828–35.
Maheshwari A, Bhattacharya S. Elective frozen replacement cycles for all: ready for prime time? Hum Reprod. 2013;28:6–9.
Barsky M, et al. Are perinatal outcomes affected by blastocyst vitrification and warming? Am J Obstet Gynecol. 2016;215:603.e1–5.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zeng, M., Su, S. & Li, L. Comparison of pregnancy outcomes after vitrification at the cleavage and blastocyst stage: a meta-analysis. J Assist Reprod Genet 35, 127–134 (2018). https://doi.org/10.1007/s10815-017-1040-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-017-1040-1