Abstract
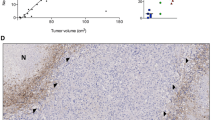
To date, no histopathological vascular investigation focusing on peritumoral brain zone (PBZ) has been reported for glioblastoma. We analyzed 10 newly diagnosed cases of glioblastomas. For these PBZs, histopathological investigation was performed by hematoxylin–eosin (H&E) staining and immunohistochemistry was analyzed for CD31, CD34, Factor VIII, VEGF, VEGFR-1/2, Ki67, p53 and nestin. Although it was difficult to identify PBZ by H&E, Ki67 and p53 staining, there were apparent differences in nestin staining among PBZ, tumor core (TC), and normal zone (NZ). Therefore, in this study, we divided PBZ from TC and NZ by nestin staining. Differences in histological features, microvessel density, expression of VEGF and its receptors were assessed for PBZ, TC and NZ. The microvessel density, as determined by counting CD31, CD34 and VEGF receptors, and VEGF-A expression were lower in PBZ than TC. The expression patterns for CD31, CD34 and VEGF receptors in vessels show dissociation in PBZ. In addition, the vascular characteristics of the PBZ may correlate with findings of radiographic imaging. We provide the first clinicopathological evidence that PBZ exhibits unique angiogenic characteristics. These in situ observations will help to elucidate the mechanisms of tumor recurrence.




Similar content being viewed by others
References
Binder DK, Berger MS (2002) Proteases and the biology of glioma invasion. J Neurooncol 56:149–158
Pope WB, Sayre J, Perlina A, Villablanca JP, Mischel PS, Cloughesy TF (2005) MR imaging correlates of survival in patients with high-grade gliomas. AJNR Am J Neuroradiol 26:2466–2474
Zinn P, Majadan B, Sathyan P, Singh S, Majumder S, Jolesz F, Colen R (2011) Radiogenomic mapping of edema/cellular invasion MRI-phenotypes in Glioblastoma multiforme. PLoS ONE 6:e25451
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996
Stummer W, Pichlmeier U, Meinel T, Wiestler OD, Zanella F, Reulen HJ (2006) ALA-Glioma Study Group. Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. Lancet Oncol 7:392–401
Shaw E, Berkey B, Coons S, Bullard D, Brachman D, Buckner J, Stelzer K, Barger G, Brown P, Gilbert M, Mehta M (2008) Recurrence following neurosurgeon-determined gross-total resection of adult supratentorial low-grade glioma: results of a prospective clinical trial. J Neurosurg 109:835–841
Baumgarten P, Blank A, Franz K, Hattingen E, Dunst M, Zeiner P, Hoffmann K, Bähr O, Mäder L, Goeppert B, Machein M, Seifert V, Steinbach J, Plate K, Harter P, Mittelbronn M (2016) Differential expression of vascular endothelial growth factor A, its receptors VEGFR-1, -2, and -3 and co-receptors neuropilin-1 and -2 does not predict bevacizumab response in human astrocytomas. Neuro Oncol 18:173–183
Folkman J (2007) Angiogenesis: an organizing principle for drug discovery ? Nat Rev Drug Discov 6:273–286
Jain RK, di Tomaso E, Duda DG, Loeffler JS, Sorensen AG, Batchelor TT (2007) Angiogenesis in brain tumours. Nat Rev Neurosci 8:610–622
Shibuya M (2011) Vascular endothelial growth factor (VEGF) and its receptor (VEGFR) signaling in Angiogenesis. Genes Cancer 2:1097–1105
Chaudhry IH, O’Donovan DG, Brenchley PE, Reid H, Roberts IS (2001) Vascular endothelial growth factor expression correlates with tumour grade and vascularity in gliomas. Histopathology 39:409–415
Yao Y, Kubota T, Sato K, Kitai R, Takeuchi H, Arishima H (2001) Prognostic value of vascular endothelial growth factor and its receptors Flt-1 and Flk-1 in astrocytic tumours. Acta Neurochir (Wien) 143:159–166
Kitamura Y, Sasaki H, Kimura T, Miwa T, Takahashi S, Kawase T, Yoshida K (2013) Molecular and clinical risk factors for recurrence of skull base chordomas: gain on chromosome 2p, expression of brachyury, and lack of irradiation negatively correlate with patient prognosis. J Neuropathol Exp Neurol 72:816–823
Ohgaki H, Kleihues P (2011) Genetic profile of astrocytic and oligodendroglial gliomas. Brain Tumor Pathol 28:177–183
Chow LM, Endersby R, Zhu X, Rankin S, Qu C, Zhang J, Broniscer A, Ellison DW, Baker SJ (2011) Cooperativity within and among Pten, p53, and Rb pathways induces high-grade astrocytoma in adult brain. Cancer Cell 19:305–316
Harhouri K, Kebir A, Guillet B, Foucault-Bertaud A, Voytenko S, Piercecchi-Marti (2010) soluble CD146 displays angiogenic properties and promotes neovascularization in experimental hind-limb ischemia. Blood 115:3843–3851
Matsuda Y, Hagio M, Ishiwata T (2013) Nestin: a novel angiogenesis marker and possible target for tumor angiogenesis. World J Gastroenterol 19:42–48
DeLay M, Jahangiri A, Carbonell W, Hu YL, Tsao S, Tom MW, Paquette J, Tokuyasu TA, Aqhi MK (2012) Microarray analysis verifies two distinct phenotypes of glioblastomas resistant to antiangiogenic therapy. Clin Cancer Res 18:2930–2942
Tamura R, Tanaka T, Miyake K, Tabei Y, Ohara K, Sampetrean O, Kono M, Mizutani K, Yamamoto Y, Murayama Y, Tamiya T, Yoshida K, Sasaki H (2016) Histopathological investigation of glioblastomas resected under bevacizumab treatment. Oncotarget 7:52423–52435
Jin X, Jin X, Jung JE, Beck S, Kim H (2013) Cell surface Nestin is a biomarker for glioma stem cells. Biochem Biophys Res Commun 433:496–501
Ishiwata T, Matsuda Y, Naito Z (2011) Nestin in gastrointestinal and other cancers: effects on cells and tumor angiogenesis. World J Gastroenterol 17:409–418
Onisim A1, Achimas-Cadariu A, Vlad C, Kubelac P, Achimas-Cadariu P (2015) Current insights into the association of Nestin with tumor angiogenesis. J BUON 20:699–706
Tamagno I, Schiffer D. Nestin expression in reactive astrocytes of human pathology. (2006) J Neurooncol 80:227–233
Schmidt NO, Westphal M, Hagel C, Ergün S, Stavrou D, Rosen EM, Lamszus K (1999) Levels of vascular endothelial growth factor, hepatocyte growth factor/scatter factor and basic fibroblast growth factor in human gliomas and their relation to angiogenesis. Int J Cancer 84:10–18
Uesaka T, Shono T, Suzuki S, Nakamizo A, Niiro H, Mizoguchi M, Iwaki T, Sasaki T (2007) Expression of VEGF and its receptor genes in intracranial schwannomas. J Neurooncol 83:259–266
Lin C, McGough R, Aswad B, Block JA, Terek R (2004) Hypoxia induces HIF-1alpha and VEGF expression in chondrosarcoma cells and chondrocytes. J Orthop Res 22:1175–1181
Asahara T, Murohara T, Sullivan A, Silver M, van der Zee R, Li T, Witzenbichler B, Schatteman G, Isner JM (1997) Isolation of putative progenitor endothelial cells for angiogenesis. Science 275:964–967
Miettinen M, Rikala MS, Rys J, Lasota J, Wang ZF (2012)Vascular endothelial growth factor receptor 2 as a marker for malignant vascular tumors and mesothelioma: an immunohistochemical study of 262 vascular endothelial and 1640 nonvascular tumors. Am J Surg Pathol 36:629–639
Huang H, Held-Feindt J, Buhl R, Mehdorn HM, Mentlein R (2005) Expression of VEGF and its receptors in different brain tumors. Neurol Res 27:371–377
Hellström M, Phng LK, Hofmann JJ, Wallgard E, Coultas L, Lindblom P, Alva J, Nilsson AK, Karlsson L, Gaiano N, Yoon K, Rossant J, Iruela-Arispe ML, Kalén M, Gerhardt H, Betsholtz C (2007) Dll4 signalling through Notch1 regulates formation of tip cells during angiogenesis. Nature 445:776–780
Phng LK, Gerhardt H (2009) Angiogenesis: a team effort coordinated by notch. Dev Cell 16:196–208
Brat DJ, Van Meir EG (2001) Glomeruloid microvascular proliferation orchestrated by VPF/VEGF: a new world of angiogenesis research. Am J Pathol 158:789–796
Batchelor T, Duda D, Tomaso E, Ancukiewicz M, Plotkin S, Gerstner E, Eichler A, Drappatz J, Hochberg F, Benner T, Louis D, Cohen K, Chea H, Exarhopoulos A, Loeffler J, Moses M, Ivy P, Sorensen A, Wen P, Jain R (2010) Phase II Study of Cediranib, an oral pan–vascular endothelial growth factor receptor tyrosine kinase inhibitor, in patients with recurrent glioblastoma. J Clin Oncol 28:2817–2823
Batchelor TT, Gerstner ER, Emblem KE, Duda DG, Kalpathy CJ, Snuderl M, Ancukiewicz M, Polaskova P, Pinho MC, Jennings D, Plotkin SR, Chi AS, Eichler AF (2013) Improved tumor oxygenation and survival in glioblastoma patients who show increased blood perfusion after cediranib and chemoradiation. Proc Natl Acad Sci USA 110:19059–19064
Suzuki S, Namiki J, Shibata S, Mastuzaki Y, Okano H (2010) The neural stem/progenitor cell marker nestin is expressed in proliferative endothelial cells, but not in mature vasculature. J Histochem Cytochem 58:721–730
Calabrese C, Poppleton H, Kocak M, Hogg TL, Fuller C, Hamner B, Oh EY, Gaber MW, Finklestein D, Allen M, Frank A, Bayazitov IT, Zakharenko SS, Gajjar A, Davidoff A, Gilbertson RJ (2007) A perivascular niche for brain tumor stem cells. Cancer Cell 11:69–82
Chinot OL, Nishikawa R, Mason W, Henriksson R, Saran F, Cloughesy T, Garcia J, Revil C, Abrey L, Wick W (2016) Upfront bevacizumab may extend survival for glioblastoma patients who do not receive second-line therapy: an exploratory analysis of AVAglio. Neuro Oncol 18:1313–1318
Acknowledgements
The authors greatly thank Ms. Naoko Tsuzaki and Tomoko Muraki at Department of Neurosurgery, Keio University School of Medicine, for technical assistance of laboratory works.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tamura, R., Ohara, K., Sasaki, H. et al. Histopathological vascular investigation of the peritumoral brain zone of glioblastomas. J Neurooncol 136, 233–241 (2018). https://doi.org/10.1007/s11060-017-2648-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-017-2648-9