Abstract
Purpose
The objective of this study was to evaluate the delivery of nasally administered aerosols to the lungs during noninvasive ventilation using controlled condensational growth techniques.
Methods
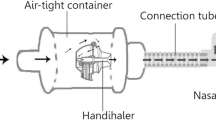
An optimized mixer, combined with a mesh nebulizer, was used to generate submicrometer aerosol particles using drug alone (albuterol sulfate) and with mannitol or sodium chloride added as hygroscopic excipients. The deposition and growth of these particles were evaluated in an adult nose-mouth-throat (NMT) model using in vitro experimental methods and computational fluid dynamics simulations.
Results
Significant improvement in the lung dose (3–4× increase) was observed using excipient enhanced growth (EEG) and enhanced condensational growth (ECG) delivery modes compared to control studies performed with a conventional size aerosol (~5 μm). This was due to reduced device retention and minimal deposition in the NMT airways. Increased condensational growth of the initially submicrometer particles was observed using the ECG mode and in the presence of hygroscopic excipients. CFD predictions for regional drug deposition and aerosol size increase were in good agreement with the observed experimental results.
Conclusions
These controlled condensational growth techniques for the delivery of submicrometer aerosols were found to be highly efficient methods for delivering nasally-administered drugs to the lungs.







Similar content being viewed by others
Abbreviations
- ACI:
-
Andersen cascade impactor
- AS:
-
albuterol sulfate
- CFD:
-
computational fluid dynamics
- DF:
-
deposition fraction
- ECG:
-
enhanced condensational growth
- EEG:
-
excipient enhanced growth
- GSD:
-
geometric standard deviation
- HFT:
-
high flow therapy
- HPLC:
-
high performance liquid chromatography
- LRN:
-
low Reynolds number
- MMAD:
-
mass median aerodynamic diameter
- MN:
-
mannitol
- NaCl:
-
sodium chloride
- NIV:
-
noninvasive ventilation
- NMT:
-
nose-mouth-throat model
- NPPV:
-
noninvasive positive pressure ventilation
- RH:
-
relative humidity
- SD:
-
standard deviation
References
Mehta S, Hill NS. Noninvasive ventilation. Am J Respir Crit Care Med. 2001;163:540–77.
Dhand R. Aerosol therapy in patients receiving noninvasive positive pressure ventilation. J Aerosol Med and Pulm Drug Deliv. 2012;25(2):63–78.
Hess DR. The mask of noninvasive ventilation: principles of design and effects on aerosol delivery. J Aerosol Med. 2007;20:S85–99.
Dysart K, Miller TL, Wolfson MR, Shaffer TH. Research in high flow therapy: mechanisms of action. Respir Med. 2009;103:1400–5.
Dhand R. Inhalation therapy in invasive and noninvasive mechanical ventilation. Curr Opin Crit Care. 2007;13:27–38.
Bhashyam AR, Wolf MT, Marcinkowski AL, Saville A, Thomas K, Carcillo JA, et al. Aerosol delivery through nasal cannulas: an in vitro study. J Aerosol Med Pulm Drug Deliv. 2008;21:181–7.
Fink JB. Aerosol delivery to ventilated infant and pediatric patients. Respir Care. 2004;49:653–65.
Parkes SN, Bersten AD. Aerosol kinetics and bronchodilator efficacy during continuous positive airway pressure delivered by face mask. Thorax. 1997;52:171–5.
Ari A, Fink JB, Dhand R. Inhalation therapy in patients receiving mechanical ventilation: an update. J Aerosol Med and Pulm Drug Deliv. 2012;25(6):319–32.
O’Riordan TG, Greco MJ, Perry RJ, Smaldone GC. Nebulizer function during mechanical ventilation. Am Rev Respir Dis. 1992;145:1117–22.
Diot P, Morra L, Smaldone GC. Albuterol delivery in a model of mechanical ventilation. Comparison of metered-dose inhaler and nebulizer efficiency. Am J Respir Crit Care Med. 1995;152(Pt 1):1391–4.
Longest PW, Tian G, Hindle M. Improving the lung delivery of nasally administered aerosols during noninvasive ventilation- an application of enhanced condensational growth (ECG). J Aerosol Med Pulm Drug Deliv. 2011;24(2):103–18.
Longest PW, Walenga R, Son YJ, Hindle M. High efficiency generation and delivery of aerosols through nasal cannula during noninvasive ventilation. J Aerosol Med Pulm Drug Deliv. 2013. doi:10.1089/jamp.2012.1006.
Longest PW, Golshahi L, Hindle M. Improving pharmaceutical aerosol delivery during noninvasive ventilation: effects of streamlined components. Annals Biomed Eng. 2013. doi:10.1007/s10439-013-0759-9.
Hindle M, Longest PW. Condensational growth of combination drug-excipient submicrometer particles for targeted high-efficiency pulmonary delivery: evaluation of formulation and delivery device. J Pharm Pharmacol. 2012;64:1254–63.
Longest PW, Hindle M. Numerical model to characterize the size increase of combination drug and hygroscopic excipient nanoparticle aerosols. Aerosol Sci Technol. 2011;45:884–99.
Longest PW, Hindle M. Condensational growth of combination drug-excipient submicrometer particles: comparison of CFD predictions with experimental results. Pharm Res. 2012;29:707–21.
Tian G, Longest PW, Li X, Hindle M. Targeting aerosol deposition to and within the lung airways using excipient enhanced growth. J Aerosol Med Pulm Drug Deliv. 2013. doi:10.1089/jamp.2012.0997.
Longest PW, Tian G, Li X, Son YJ, Hindle M. Performance of combination drug and hygroscopic excipient submicrometer particles from a softmist inhaler in a characteristic model of the airways. Annals Biomed Eng. 2012;40(12):2596–610.
Hindle M, Longest PW. Evaluation of enhanced condensational growth (ECG) for controlled respiratory drug delivery in a mouth-throat and upper tracheobronchial model. Pharm Res. 2010;27:1800–11.
Guilmette RA, Wicks JD, Wolff RK. Morphometry of human nasal airways in vivo using magnetic resonance imaging. J Aerosol Med. 1989;2(4):365–77.
Kelly JT, Asgharian B, Kimbell JS, Wong B. Particle deposition in human nasal airway replicas manufactured by different methods. Part I: Inertial regime particles. Aerosol Sci Technol. 2004;38:1063–71.
Kelly JT, Asgharian B, Kimbell JS, Wong B. Particle deposition in human nasal airway replicas manufactured by different methods. Part II: Ultrafine particles. Aerosol Sci Technol. 2004;38:1072–9.
Kimbell JS, Segal RA, Asgharian B, Wong BA, Schroeter JD, Southal JP, et al. Characterization of deposition from nasal spray devices using a computational fluid dynamics model of the human nasal passages. J Aerosol Med. 2007;20(1):59–74.
Schroeter JD, Garcia GJM, Kimbell JS. Effects of surface smoothness on inertial particle deposition in human nasal models. J Aerosol Sci. 2011;42:52–63.
Xi J, Longest PW. Transport and deposition of micro-aerosols in realistic and simplified models of the oral airway. Ann Biomed Eng. 2007;35(4):560–81.
Delvadia RR, Longest PW, Hindle M, and Byron PR. In vitro tests for aerosol deposition. III: effect of inhaler insertion angel on aerosol deposition. J Aerosol Med Pulm Drug Del. 2013 doi: 10.1089/jamp.2012.0989.
Longest PW, Vinchurkar S. Validating CFD predictions of respiratory aerosol deposition: effects of upstream transitions and turbulence. J Biomech. 2007;40:305–16.
Xi J, Longest PW, Martonen TB. Effects of the laryngeal jet on nano- and microparticle transport and deposition in an approximate model of the upper tracheobronchial airways. J Appl Physiol. 2008;104:1761–77.
Longest PW, Xi J. Condensational growth may contribute to the enhanced deposition of cigarette smoke particles in the upper respiratory tract. Aerosol Sci Technol. 2008;42:579–602.
Longest PW, Hindle M, Das Choudhuri S, Byron PR. Numerical simulations of capillary aerosol generation: CFD model development and comparisons with experimental data. Aerosol Sci Technol. 2007;41:952–73.
Acknowledgments and Disclosures
This study was supported by Award R01 HL107333 from the National Heart, Lung, and Blood Institute. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Heart, Lung, And Blood Institute or the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Golshahi, L., Tian, G., Azimi, M. et al. The Use of Condensational Growth Methods for Efficient Drug Delivery to the Lungs during Noninvasive Ventilation High Flow Therapy. Pharm Res 30, 2917–2930 (2013). https://doi.org/10.1007/s11095-013-1123-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-013-1123-3