Abstract
Purpose
Questions remain about the polysomnographic findings and the predictors for sleep desaturation in cystic fibrosis (CF) patients. Our study aimed to evaluate sleep parameters in a sample of adult CF patients comparing them with healthy controls and to determine the best predictors of sleep desaturation in CF patients with awake resting peripheral oxygen saturation (SpO2) ≥90%.
Methods
In a cross-sectional study, with data collected prospectively, 51 clinically stable adult CF patients (mean age 25.1 ± 6.7 years) and 25 age-matched controls underwent an overnight polysomnography and answered sleep questionnaires. CF patients had their pulmonary function, 6-min walk test, and echocardiography assessed.
Results
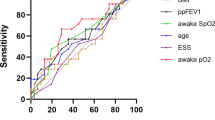
CF patients and control subjects had similar sleep architecture. However, CF patients had impaired subjective sleep quality and a higher arousal index than controls. The apnea–hypopnea index was similar in both groups, and only two CF patients (3.9%) fulfilled the criteria for obstructive sleep apnea syndrome. Sleep desaturation was more common in CF patients (29.4% vs 0%; p < 0.001). In a logistic regression model, we observed that awake resting SpO2 was the single best variable associated with sleep desaturation in CF population (p < 0.001). The awake SpO2 <94% had a sensitivity, specificity, positive and negative predictive value for sleep desaturation of, respectively, 93.3%, 100%, 100%, and 97.3%.
Conclusions
CF patients had a worse subjective sleep quality and small changes in sleep architecture. In nonhypoxic, adult CF patients, sleep desaturation is common, is not associated with obstructive sleep events, and can be accurately predicted by awake resting SpO2 <94%.

Similar content being viewed by others
References
Ratjen F, Doring G (2003) Cystic fibrosis. Lancet 361:681–689
Yankaskas JR, Marshall BC, Sufian B, Simon RH, Rodman D (2004) Cystic fibrosis adult care: consensus conference report. Chest 125:1S–39S
Milross MA, Piper AJ, Dobbin CJ, Bye PT, Grunstein RR (2004) Sleep disordered breathing in cystic fibrosis. Sleep Med Rev 8:295–308
Fraser KL, Tullis DE, Sasson Z, Hyland RH, Thornley KS, Hanly PJ (1999) Pulmonary hypertension and cardiac function in adult cystic fibrosis: role of hypoxemia. Chest 115:1321–1328
Dancey DR, Tullis ED, Heslegrave R, Thornley K, Hanly PJ (2002) Sleep quality and daytime function in adults with cystic fibrosis and severe lung disease. Eur Respir J 19:504–510
Milross MA, Piper AJ, Norman M, Becker HF, Willson GN, Grunstein RR, Sullivan CE, Bye PT (2001) Low-flow oxygen and bilevel ventilatory support: effects on ventilation during sleep in cystic fibrosis. Am J Respir Crit Care Med 163:129–134
Young AC, Wilson JW, Kotsimbos TC, Naughton MT (2008) Randomised placebo controlled trial of non-invasive ventilation for hypercapnia in cystic fibrosis. Thorax 63:72–77
Bradley S, Solin P, Wilson J, Johns D, Walters EH, Naughton MT (1999) Hypoxemia and hypercapnia during exercise and sleep in patients with cystic fibrosis. Chest 116:647–654
Frangolias DD, Wilcox PG (2001) Predictability of oxygen desaturation during sleep in patients with cystic fibrosis: clinical, spirometric, and exercise parameters. Chest 119:434–441
Milross MA, Piper AJ, Norman M, Willson GN, Grunstein RR, Sullivan CE, Bye PT (2001) Predicting sleep-disordered breathing in patients with cystic fibrosis. Chest 120:1239–1245
Versteegh FG, Bogaard JM, Raatgever JW, Stam H, Neijens HJ, Kerrebijn KF (1990) Relationship between airway obstruction, desaturation during exercise and nocturnal hypoxaemia in cystic fibrosis patients. Eur Respir J 3:68–73
Shwachman H, Kulczycki LL (1958) Long-term study of one hundred five patients with cystic fibrosis; studies made over a five- to fourteen-year period. Am J Dis Child 96:6–15
Brasfield D, Hicks G, Soong S, Tiller RE (1979) The chest roentgenogram in cystic fibrosis: a new scoring system. Pediatrics 63:24–29
Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, Crapo R, Enright P, van der Grinten CP, Gustafsson P, Jensen R, Johnson DC, MacIntyre N, McKay R, Navajas D, Pedersen OF, Pellegrino R, Viegi G, Wanger J (2005) Standardisation of spirometry. Eur Respir J 26:319–338
Pereira CA, Sato T, Rodrigues SC (2007) New reference values for forced spirometry in white adults in Brazil. J Bras Pneumol 33:397–406
American Thoracic Society (2002) ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med 166:111–117
Quinones MA, Otto CM, Stoddard M, Waggoner A, Zoghbi WA (2002) Recommendations for quantification of Doppler echocardiography: a report from the Doppler Quantification Task Force of the Nomenclature and Standards Committee of the American Society of Echocardiography. J Am Soc Echocardiogr 15:167–184
Chemla D, Castelain V, Herve P, Lecarpentier Y, Brimioulle S (2002) Haemodynamic evaluation of pulmonary hypertension. Eur Respir J 20:1314–1331
Buysse DJ, Reynolds CF III, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28:193–213
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Bertolazi AN, Fagondes SC, Hoff LS, Pedro VD, Menna Barreto SS, Johns MW (2009) Portuguese-language version of the Epworth sleepiness scale: validation for use in Brazil. J Bras Pneumol 35:877–883
Bertolazi AN, Fagondes SC, Hoff LS, Dartora EG, da Silva Miozzo IC, de Barba ME, Barreto SS (2011) Validation of the Brazilian Portuguese version of the Pittsburgh Sleep Quality Index. Sleep Med 12:70–75
Iber C, Ancoli-Israel S, Chesson A, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. AASM, Westchester
Fletcher EC, Miller J, Divine GW, Fletcher JG, Miller T (1987) Nocturnal oxyhemoglobin desaturation in COPD patients with arterial oxygen tensions above 60 mmHg. Chest 92:604–608
Fletcher EC, Donner CF, Midgren B, Zielinski J, Levi-Valensi P, Braghiroli A, Rida Z, Miller CC (1992) Survival in COPD patients with a daytime PaO2 greater than 60 mmHg with and without nocturnal oxyhemoglobin desaturation. Chest 101:649–655
Braghiroli A (2002) Nocturnal Desaturations in COPD: still an open question ? Sleep Breath 6:25–26
American Academy of Sleep Medicine (2005) International classification of sleep disorders. Diagnostic and coding manual (ICSD-2), 2nd edn. American Academy of Sleep Medicine, Westchester
Becker HF, Piper AJ, Flynn WE, McNamara SG, Grunstein RR, Peter JH, Sullivan CE (1999) Breathing during sleep in patients with nocturnal desaturation. Am J Respir Crit Care Med 159:112–118
Block AJ, Boysen PG, Wynne JW, Hunt LA (1979) Sleep apnea, hypopnea and oxygen desaturation in normal subjects. A strong male predominance. N Engl J Med 300:513–517
Stokes DC, McBride JT, Wall MA, Erba G, Strieder DJ (1980) Sleep hypoxemia in young adults with cystic fibrosis. Am J Dis Child 134:741–743
Laaban JP, Diebold B, Zelinski R, Lafay M, Raffoul H, Rochemaure J (1989) Noninvasive estimation of systolic pulmonary artery pressure using Doppler echocardiography in patients with chronic obstructive pulmonary disease. Chest 96:1258–1262
Acknowledgments
This study was funded by Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul and Fundo de Incentivo à Pesquisa do Hospital de Clínicas de Porto Alegre. We thank Ms Vânia Naomi Hirakata for statistical analyses and the medical, administrative, and nursing staff of the HCPA Adult CF Program for their collaboration.
Financial disclosures
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
This research was performed at Hospital de Clinicas de Porto Alegre, Porto Alegre, Rio Grande do Sul, Brazil.
Rights and permissions
About this article
Cite this article
Perin, C., Fagondes, S.C., Casarotto, F.C. et al. Sleep findings and predictors of sleep desaturation in adult cystic fibrosis patients. Sleep Breath 16, 1041–1048 (2012). https://doi.org/10.1007/s11325-011-0599-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-011-0599-5