Abstract
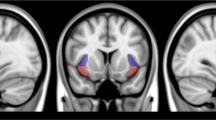
Compared to nonsmokers, smokers exhibit a number of potentially important differences in regional brain function. However, little is known about the associations between the local spontaneous brain activity and smoking cessation treatment outcomes. In the present analysis, we aimed to evaluate whether the local features of spontaneous brain activity prior to the target quit date was associated with the smoking cessation outcomes. All the participants underwent magnetic resonance imaging scans and smoking-related behavioral assessments. After a 12-week treatment with varenicline, 23 smokers succeeded in quitting smoking and 32 failed. Smokers underwent functional magnetic resonance imaging (fMRI) scanning prior to an open label smoking cessation treatment trial. Regional homogeneity (ReHo) was used to measure spontaneous brain activity, and whole-brain voxel-wise comparisons of ReHo were performed to detect brain regions with altered spontaneous brain activity between relapser and quitter groups. After controlling for potentially confounding factors including years of education, years smoked, cigarettes smoked per day and FTND score as covariates, compared to quitters, relapsers displayed significantly decreased ReHo in bilateral posterior cingulate cortex (PCC), as well as increased ReHo in left superior temporal gyrus (STG). These preliminary results suggest that regional brain function variables may be promising predictors of smoking relapse. This study provided novel insights into the neurobiological mechanisms underlying smoking relapse. A deeper understanding of the neurobiological mechanisms associated with relapse may result in novel pharmacological and behavioral interventions.


Similar content being viewed by others
References
Bentley, P., Husain, M., & Dolan, R. J. (2004). Effects of cholinergic enhancement on visual stimulation, spatial attention, and spatial working memory. Neuron, 41, 969–982.
Brody, A. L., Mandelkern, M. A., Jarvik, M. E., Lee, G. S., Smith, E. C., Huang, J. C., et al. (2004). Differences between smokers and nonsmokers in regional gray matter volumes and densities. Biological Psychiatry, 55, 77–84.
Buckner, R. L., Andrews-Hanna, J. R., & Schacter, D. L. (2008). The brain’s default network: anatomy, function, and relevance to disease. Annals of the New York Academy of Sciences, 1124, 1–38.
Coe, J. W., Brooks, P. R., Vetelino, M. G., Wirtz, M. C., Arnold, E. P., Huang, J., et al. (2005). Varenicline: an alpha4beta2 nicotinic receptor partial agonist for smoking cessation. Journal of Medicinal Chemistry, 48, 3474–3477.
Costello, M. R., Mandelkern, M. A., Shoptaw, S., Shulenberger, S., Baker, S. K., Abrams, A. L., et al. (2010). Effects of treatment for tobacco dependence on resting cerebral glucose metabolism. Neuropsychopharmacology: official publication of the American College of Neuropsychopharmacology, 35, 605–612.
David, S. P., Munafo, M. R., Johansen-Berg, H., Smith, S. M., Rogers, R. D., Matthews, P. M., & Walton, R. T. (2005). Ventral striatum/nucleus accumbens activation to smoking-related pictorial cues in smokers and nonsmokers: a functional magnetic resonance imaging study. Biological Psychiatry, 58, 488–494.
Dome, P., Lazary, J., Kalapos, M. P., & Rihmer, Z. (2010). Smoking, nicotine and neuropsychiatric disorders. Neuroscience and Biobehavioral Reviews, 34, 295–342.
Due, D. L., Huettel, S. A., Hall, W. G., & Rubin, D. C. (2002). Activation in mesolimbic and visuospatial neural circuits elicited by smoking cues: evidence from functional magnetic resonance imaging. The American Journal of Psychiatry, 159, 954–960.
Engelmann, J. M., Versace, F., Robinson, J. D., Minnix, J. A., Lam, C. Y., Cui, Y., et al. (2012). Neural substrates of smoking cue reactivity: a meta-analysis of fMRI studies. NeuroImage, 60, 252–262.
Fiore, M.C., Jaén, C. R., Baker, T. B., Bailey, W. C., Benowitz, N. L., Curry, S. J., et al. (2008) Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guideline PhD thesis, US Department of Health and Human Services Public Health Service, Rockville, MD.
Franklin, T.R., Wang, Z., Wang, J., Sciortino, N., Harper, D., Li, Y., et al. (2007). Limbic activation to cigarette smoking cues independent of nicotine withdrawal: a perfusion fMRI study. Neuropsychopharmacology: official publication of the American College of Neuropsychopharmacology, 32, 2301–2309.
Franklin, T., Wang, Z., Suh, J. J., Hazan, R., Cruz, J., Li, Y., et al. (2011). Effects of varenicline on smoking cue-triggered neural and craving responses. Archives of General Psychiatry, 68, 516–526.
Froeliger, B., Kozink, R. V., Rose, J. E., Behm, F. M., Salley, A. N., & McClernon, F. J. (2010). Hippocampal and striatal gray matter volume are associated with a smoking cessation treatment outcome: results of an exploratory voxel-based morphometric analysis. Psychopharmacology, 210, 577–583.
Froeliger, B., Modlin, L. A., Kozink, R. V., Wang, L., Garland, E. L., Addicott, M. A., & McClernon, F. J. (2013). Frontoparietal attentional network activation differs between smokers and nonsmokers during affective cognition. Psychiatry Research, 211, 57–63.
Gallinat, J., Meisenzahl, E., Jacobsen, L. K., Kalus, P., Bierbrauer, J., Kienast, T., et al. (2006). Smoking and structural brain deficits: a volumetric MR investigation. The European Journal of Neuroscience, 24, 1744–1750.
Giessing, C., Thiel, C. M., Rosler, F., & Fink, G. R. (2006). The modulatory effects of nicotine on parietal cortex activity in a cued target detection task depend on cue reliability. Neuroscience, 137, 853–864.
Greicius, M. D., Krasnow, B., Reiss, A. L., & Menon, V. (2003). Functional connectivity in the resting brain: a network analysis of the default mode hypothesis. Proceedings of the National Academy of Sciences of the United States of America, 100, 253–258.
Hahn, B., Ross, T. J., Yang, Y., Kim, I., Huestis, M. A., & Stein, E. A. (2007). Nicotine enhances visuospatial attention by deactivating areas of the resting brain default network. The Journal of Neuroscience, 27, 3477–3489.
Hartwell, K. J., Johnson, K. A., Li, X., Myrick, H., LeMatty, T., George, M. S., & Brady, K. T. (2011). Neural correlates of craving and resisting craving for tobacco in nicotine dependent smokers. Addiction Biology, 16, 654–666.
Heatherton, T. F., Kozlowski, L. T., Frecker, R. C., & Fagerstrom, K. O. (1991). The fagerstrom test for nicotine dependence: a revision of the fagerstrom tolerance questionnaire. British Journal of Addiction, 86, 1119–1127.
Hegemann, S., Fitzek, S., Fitzek, C., & Fetter, M. (2004). Cortical vestibular representation in the superior temporal gyrus. Journal of Vestibular Research: Equilibrium & Orientation, 14, 33–35.
Hong, L. E., Gu, H., Yang, Y., Ross, T. J., Salmeron, B. J., Buchholz, B., et al. (2009). Association of nicotine addiction and nicotine’s actions with separate cingulate cortex functional circuits. Archives of General Psychiatry, 66(4), 431–441.
Janse Van Rensburg, K., Taylor, A., Hodgson, T., & Benattayallah, A. (2009). Acute exercise modulates cigarette cravings and brain activation in response to smoking-related images: an fMRI study. Psychopharmacology, 203, 589–598.
Jiang, L., Xu, T., He, Y., Hou, X. H., Wang, J., Cao, X. Y., et al. (2015a). Toward neurobiological characterization of functional homogeneity in the human cortex: regional variation, morphological association and functional covariance network organization. Brain Structure & Function, 220, 2485–2507.
Jiang, L., & Zuo, X.N., (2015b). Regional homogeneity: a multimodal, multiscale neuroimaging marker of the human connectome. Neuroscientist, 7,1–20.
Jorenby, D. E., Hays, J. T., Rigotti, N. A., Azoulay, S., Watsky, E. J., Williams, K. E., et al. (2006). Efficacy of varenicline, an α4β2 nicotinic acetylcholine receptor partial agonist, vs placebo or sustained-release bupropion for smoking cessation: a randomized controlled trial. JAMA, 296, 56–63.
Karnath, H. O. (2001). New insights into the functions of the superior temporal cortex. Nature Reviews Neuroscience, 2, 568–576.
Lee, J. H., Lim, Y., Wiederhold, B. K., & Graham, S. J. (2005). A functional magnetic resonance imaging (FMRI) study of cue-induced smoking craving in virtual environments. Applied Psychophysiology and Biofeedback, 30, 195–204.
Liao, Y., Tang, J., Liu, T., Chen, X., & Hao, W. (2012). Differences between smokers and non-smokers in regional gray matter volumes: a voxel-based morphometry study. Addiction Biology, 17, 977–980.
Lin, F., Wu, G., Zhu, L., & Lei, H. (2015). Altered brain functional networks in heavy smokers. Addiction Biology, 20(4), 809–819.
Liu, D., Yan, C., Ren, J., Yao, L., Kiviniemi, V. J., & Zang, Y. (2010). Using coherence to measure regional homogeneity of resting-state FMRI signal. Frontiers in Systems Neuroscience, 4, 24.
Luijten, M., Veltman, D. J., van den Brink, W., Hester, R., Field, M., Smits, M., & Franken, I. H. (2011). Neurobiological substrate of smoking-related attentional bias. NeuroImage, 54, 2374–2381.
Mathers, C. D., & Loncar, D. (2006). Projections of global mortality and burden of disease from 2002 to 2030. PLoS Medicine, 3, e442.
May, J. C., Delgado, M. R., Dahl, R. E., Stenger, V. A., Ryan, N. D., Fiez, J. A., & Carter, C. S. (2004). Event-related functional magnetic resonance imaging of reward-related brain circuitry in children and adolescents. Biological Psychiatry, 55(4), 359–366.
Mesulam, M. M. (1998). From sensation to cognition. Brain, 121, 1013–1052.
Nides, M., Oncken, C., Gonzales, D., Rennard, S., Watsky, E. J., Anziano, R., & Reeves, K. R. (2006). Smoking cessation with varenicline, a selective α4β2 nicotinic receptor partial agonist: results from a 7-week, randomized, placebo-and bupropion-controlled trial with 1-year follow-up. Archives of Internal Medicine, 166, 1561–1568.
Picciotto, M. R., & Zoli, M. (2008). Neuroprotection via nAChRs: the role of nAChRs in neurodegenerative disorders such as Alzheimer’s and Parkinson’s disease. Frontiers In Bioscience, 13, 492–504.
Rose, J.E., Behm, F.M., Salley, A.N., Bates, J.E., Coleman, R.E., Hawk, T.C., & Turkington, T.G., (2007). Regional brain activity correlates of nicotine dependence. Neuropsychopharmacology: official publication of the American College of Neuropsychopharmacology, 32, 2441–2452.
Song, X. W., Dong, Z. Y., Long, X. Y., Li, S. F., Zuo, X. N., Zhu, C. Z., et al. (2011). REST: a toolkit for resting-state functional magnetic resonance imaging data processing. PloS One, 6, e25031.
Sutherland, M. T., Carroll, A. J., Salmeron, B. J., Ross, T. J., Hong, L. E., & Stein, E. A. (2013a). Down-regulation of amygdala and insula functional circuits in abstinent cigarette smokers by varenicline and nicotine. Biological Psychiatry, 74, 538–546.
Sutherland, M. T., Carroll, A. J., Salmeron, B. J., Ross, T. J., Hong, L. E., & Stein, E. A. (2013b). Individual differences in amygdala reactivity following nicotinic receptor engagement in abstinent smokers. NeuroImage, 66, 585–593.
Sutherland, M. T., Carroll, A. J., Salmeron, B. J., Ross, T. J., & Stein, E. A. (2013c). Insula’s functional connectivity with ventromedial prefrontal cortex mediates the impact of trait alexithymia on state tobacco craving. Psychopharmacology, 228, 143–155.
Tanabe, J., Nyberg, E., Martin, L. F., Martin, J., Cordes, D., Kronberg, E., & Tregellas, J. R. (2011). Nicotine effects on default mode network during resting state. Psychopharmacology, 216, 287–295.
Tang, J., Liao, Y., Deng, Q., Liu, T., Chen, X., Wang, X., et al. (2012). Altered spontaneous activity in young chronic cigarette smokers revealed by regional homogeneity. Behavioral and Brain Functions, 8, 44.
Thiel, C. M., & Fink, G. R. (2008). Effects of the cholinergic agonist nicotine on reorienting of visual spatial attention and top-down attentional control. Neuroscience, 152, 381–390.
Thiel, C. M., Zilles, K., & Fink, G. R. (2005). Nicotine modulates reorienting of visuospatial attention and neural activity in human parietal cortex. Neuropsychopharmacology, 30, 810–820.
Tregellas, J. R., Shatti, S., Tanabe, J. L., Martin, L. F., Gibson, L., Wylie, K., & Rojas, D. C. (2007). Gray matter volume differences and the effects of smoking on gray matter in schizophrenia. Schizophrenia Research, 97, 242–249.
Wu, G., Yang, S., Zhu, L., & Lin, F. (2015). Altered spontaneous brain activity in heavy smokers revealed by regional homogeneity. Psychopharmacology, 232(14), 2481–2489.
Yu, R., Zhao, L., & Lu, L. (2011). Regional grey and white matter changes in heavy male smokers. PloS one, 6, e27440.
Yu, R., Zhao, L., Tian, J., Qin, W., Wang, W., Yuan, K., Li, Q., & Lu, L. (2013). Regional homogeneity changes in heavy male smokers: a resting-state functional magnetic resonance imaging study. Addiction Biology, 18, 729–731.
Zang, Y., Jiang, T., Lu, Y., He, Y., & Tian, L. (2004). Regional homogeneity approach to fMRI data analysis. NeuroImage, 22, 394–400.
Zhang, D., & Raichle, M. E. (2010). Disease and the brain's dark energy. Nature Reviews Neurology, 6, 15–28.
Zhang, X., Salmeron, B. J., Ross, T. J., Geng, X., Yang, Y., & Stein, E. A. (2011). Factors underlying prefrontal and insula structural alterations in smokers. NeuroImage, 54, 42–48.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the Natural Science Foundation of China surface project (grant nos. 81171310) and science and technology planning project of Zhejiang Province (grant 2011C23094).
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Wang, C., Shen, Z., Huang, P. et al. Altered spontaneous activity of posterior cingulate cortex and superior temporal gyrus are associated with a smoking cessation treatment outcome using varenicline revealed by regional homogeneity. Brain Imaging and Behavior 11, 611–618 (2017). https://doi.org/10.1007/s11682-016-9538-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-016-9538-1