Abstract
Background
We investigate the outcomes of pregnancy in women who undergone restrictive–malabsorptive procedure at Centro da Obesidade Mórbida–Hospital São Lucas (COM HSL-PUCRS), Porto Alegre, Brazil.
Methods
All pregnancies started after the bariatric surgery and with estimated due date until June 2008 were eligible for the study. Only the first pregnancy of each patient was included in the data analysis. Data was collected from medical records.
Results
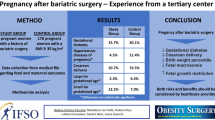
Forty seven pregnancies were identified in 41 women. Eight of them were ineligible. There were 30 complete pregnancies and nine miscarriages (23%). Cesarean delivery was performed in 69% of the complete pregnancies. Mature infants occurred in 93.1%. Twelve pregnancies (30.8%) occurred in the first year after surgery. Vitamin B12 was low in 53.4% patients; folic acid in 16.1%, iron in 6.7%, ferritin in 41.7%, calcium in 16.7%, and albumin in 10.3% of the patients. Nineteen women (79.2%) had no complication during the pregnancy and two (8.3%) presented with internal hernia. The average of newborns weight and length on delivery were 3,037 g and 48.07 cm, respectively. Children from pregnancies started in the first year of post operatory had similar outcomes of children from pregnancies started after 1 year of surgery.
Conclusions
Pregnancy after bariatric surgery is safe and has fewer complications than pregnancy in morbidly obese women. However, the recommendation to delay the pregnancy for at least 12–18 months post-operatively should be kept.


Similar content being viewed by others
References
Bar-Zohar D et al. Pregnancy after laparoscopic adjustable gastric banding: perinatal outcome is favorable also for women with relatively high gestacional weight gain. Surg Endosc. 2006;20:1580–3.
World Health Organization (2009). Health topics—obesity. Available at www.wpro.who.int/health_topics/obesity/. Accessed date January 12, 2009.
Instituto Brasileiro de Geografia e Estatística—IBGE. 2ª Etapa da Pesquisa de Orçamentos Familiares–POF 2002–2003.
Marceu P et al. Outcome of pregnancies after biliopancreatic diversion. Obes Surg. 2004;14:318–24.
Raymond RH. Hormonal status, fertility, and pregnancy before and after bariatric surgery. Crit Care Nurs Q. 2005;28(3):263–8.
Weiss JL et al. Obesity, obstetric complications and cesarean delivery rate—a population-based screening study. Am J Obstet Gynecol. 2004;190:1091–7.
Buchwald H. Consensus conference statement bariatric surgery for morbid obesity: health implications for patients, health professionals, and third-party payers. Surg Obes Relat Dis. 2005;1:371–81.
Dao T et al. Pregnancy outcomes after gastric-bypass surgery. Am J Surg. 2006;192:762–6.
Woodard C. Pregnancy following bariatric surgery. J Perinat Neonatal Nurs. 2004;18:329–40.
Deitel M. Pregnancy after bariatric surgery. Obes Surg. 1998;8:465–6.
Martin LF et al. Pregnancy after adjustable gastric banding. Obstet Gynecol. 2000;95:927–30.
Wittgrove AC et al. Pregnancy following gastric bypass for morbid obesity. Obes Surg. 1998;8:461–6.
Sheiner E et al. Pregnancy after bariatric surgery is not associated with adverse perinatal outcome. Am J Obstet Gynecol. 2004;190:1335–40.
Karmon A, Sheiner E. Pregnancy after bariatric surgery: a comprehensive review. Arch Gynecol Obstet. 2008;277:381–8.
Poobalan AS et al. Obesity as an independent risk factor for elective and emergency Caesarean delivery in nulliparous women—systematic review and meta-analysis of cohort studies. Obes Rev. 2009;10:28–35.
Sheiner E et al. Maternal obesity as an independent risk factor for Caesarean delivery. Paediatr Perinat Epidemiol. 2004;18:196–201.
Charles A et al. Small bowel ischemia after Roux-en-Y gastric bypass complicated by pregnancy: a case report. Am Surg. 2005;71(3):231–4.
Baker MT, Kothari SN. Successful surgical treatment of a pregnancy-induced Petersen’s hernia after laparoscopic gastric bypass. Surg Obes Relat Dis. 2005;1:506–8.
Kakarla N et al. Pregnancy after gastric bypass surgery and internal hernia formation. Obstet Gynecol. 2005;105(5pt2):1195–8.
Conflict of interest disclosure
Drs. Bebber, Rodrigues, Padoin, and Repetto and Nut Casagrande have no conflict of interest which would include funding for the research. Dr. Rizzolli has contracted research from Takeda Pharmaceutical Co. and Dr. Mottim is the principal investigator of Brazilian Health Ministry and Brazilian Science and Technology Ministry and principal and co-investigator of Johnson & Johnson.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bebber, F.E., Rizzolli, J., Casagrande, D.S. et al. Pregnancy after Bariatric Surgery: 39 Pregnancies Follow-up in a Multidisciplinary Team. OBES SURG 21, 1546–1551 (2011). https://doi.org/10.1007/s11695-010-0263-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-010-0263-3