Abstract
Background
Hepatocellular carcinoma (HCC) occasionally occurs in non-cirrhotic patients; however, outcomes for these patients are not extensively documented.
Methods
We performed an institutional review of patients without cirrhosis who underwent resection for HCC. Clinical data were evaluated to identify factors impacting recurrence-free survival (RFS) and overall survival (OS).
Results
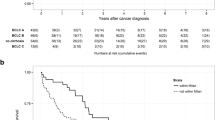
Forty-two patients underwent hepatectomy for HCC in the absence of cirrhosis over a 10-year period. Median follow-up was 22 months. For the entire cohort, 1-, 3-, and 5-year RFS was 62%, 42%, and 38% and 1-, 3-, and 5-year OS was 78%, 60%, and 49%, respectively. On univariate analysis, RFS was significantly worse for patients with a disrupted/absent tumor capsule (p = 0.027), vascular invasion (p = 0.030), elevated alkaline phosphatase (p = 0.004), and tumor size > 10 cm (p = 0.016). OS was significantly worse for patients with a disrupted/absent tumor capsule (p = 0.044), obesity (p = 0.036), and elevated alkaline phosphatase (p = 0.007) with a trend towards decreased OS for tumor size > 10 cm (p = 0.07).
Conclusions
Patients undergoing resection for HCC in the absence of cirrhosis have fairly high recurrence and modest survival rates. Pre-operative alkaline phosphatase, tumor size, tumor encapsulation, and vascular invasion are important prognostic factors.

Similar content being viewed by others
References
Chacko S, Samanta S. Hepatocellular carcinoma: a life-threatening disease. Biomed Pharmacother. 2016;84:1679–88.
Yoo HY, Patt CH, Geschwind JF, Thuluvath PJ. The outcome of liver transplantation in patients with hepatocellular carcinoma in the United States between 1988 and 2001: 5-year survival has improved significantly with time. J Clin Oncol. 2003;21(23):4329–35.
Figueras J, Jaurrieta E, Valls C, Benasco C, Rafecas A, Xiol X, et al. Survival after liver transplantation in cirrhotic patients with and without hepatocellular carcinoma: a comparative study. Hepatology. 1997;25(6):1485–9.
Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, Bozzetti F, et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med. 1996;334(11):693–9.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–96.
Edge S, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A. editors AJCC cancer staging manual. 7th ed. New York, Springer; 2009. p. 19–199.
Zhou Y, Lei X, Wu L, Wu X, Xu D, Li B. Outcomes of hepatectomy for noncirrhotic hepatocellular carcinoma: a systematic review. Surg Oncol. 2014;23(4):236–42.
Cabibbo G, Craxì A. Epidemiology, risk factors and surveillance of hepatocellular carcinoma. Eur Rev Med Pharmacol Sci. 2010;14(4):352–5.
Yeh CN, Chen MF, Lee WC, Jeng LB. Prognostic factors of hepatic resection for hepatocellular carcinoma with cirrhosis: univariate and multivariate analysis. J Surg Oncol. 2002;81(4):195–202.
Dahiya D, Wu TJ, Lee CF, Chan KM, Lee WC, Chen MF. Minor versus major hepatic resection for small hepatocellular carcinoma (HCC) in cirrhotic patients: a 20-year experience. Surgery. 2010;147(5):676–85.
Menahem B, Lubrano J, Duvoux C, Mulliri A, Alves A, Costentin C, et al. Liver transplantation versus liver resection for hepatocellular carcinoma in intention to treat: attempt to perform an ideal meta-analysis. Liver Transpl. 2017;23:836–44. https://doi.org/10.1002/lt.24758.
Arnaoutakis DJ, Mavros MN, Shen F, Alexandrescu S, Firoozmand A, Popescu I, et al. Recurrence patterns and prognostic factors in patients with hepatocellular carcinoma in noncirrhotic liver: a multi-institutional analysis. Ann Surg Oncol. 2014;21(1):147–54.
Bismuth H, Chiche L, Castaing D. Surgical treatment of hepatocellular carcinomas in noncirrhotic liver: experience with 68 liver resections. World J Surg. 1995;19(1):35–41.
Dupont-Bierre E, Compagnon P, Raoul JL, Fayet G, de Lajarte-Thirouard AS, Boudjema K. Resection of hepatocellular carcinoma in noncirrhotic liver: analysis of risk factors for survival. J Am Coll Surg. 2005;201(5):663–70.
Yu MC, Chan KM, Lee CF, Lee YS, Eldeen FZ, Chou HS, et al. Alkaline phosphatase: does it have a role in predicting hepatocellular carcinoma recurrence? J Gastrointest Surg. 2011;15(8):1440–9.
Yip VS, Gomez D, Tan CY, Staettner S, Terlizzo M, Fenwick S, et al. Tumour size and differentiation predict survival after liver resection for hepatocellular carcinoma arising from non-cirrhotic and non-fibrotic liver: a case-controlled study. Int J Surg. 2013;11(10):1078–82.
Faber W, Sharafi S, Stockmann M, Dennecke T, Bahra M, Klein F, et al. Patient age and extent of liver resection influence outcome of liver resection for hepatocellular carcinoma in non-cirrhotic liver. Hepato-Gastroenterology. 2014;61(135):1925–30.
Grazi GL, Cescon M, Ravaioli M, Ercolani G, Gardini A, Del Gaudio M, et al. Liver resection for hepatocellular carcinoma in cirrhotics and noncirrhotics. Evaluation of clinicopathologic features and comparison of risk factors for long-term survival and tumour recurrence in a single centre. Aliment Pharmacol Ther. 2003;17(Suppl 2):119–29.
Faber W, Sharafi S, Stockmann M, Denecke T, Sinn B, Puhl G, et al. Long-term results of liver resection for hepatocellular carcinoma in noncirrhotic liver. Surgery. 2013;153(4):510–7.
Truant S, Boleslawski E, Duhamel A, Bouras AF, Louvet A, Febvay C, et al. Tumor size of hepatocellular carcinoma in noncirrhotic liver: a controversial predictive factor for outcome after resection. Eur J Surg Oncol. 2012;38(12):1189–96.
Yang LY, Fang F, Ou DP, Wu W, Zeng ZJ, Wu F. Solitary large hepatocellular carcinoma: a specific subtype of hepatocellular carcinoma with good outcome after hepatic resection. Ann Surg. 2009;249(1):118–23.
Yang LY, Wang W, Peng JX, Yang JQ, Huang GW. Differentially expressed genes between solitary large hepatocellular carcinoma and nodular hepatocellular carcinoma. World J Gastroenterol. 2004;10(24):3569–73.
Wu TH, Yu MC, Chen TC, Lee CF, Chan KM, Wu TJ, et al. Encapsulation is a significant prognostic factor for better outcome in large hepatocellular carcinoma. J Surg Oncol. 2012;105(1):85–90.
Ng IO, Lai EC, Ng MM, Fan ST. Tumor encapsulation in hepatocellular carcinoma. A pathologic study of 189 cases. Cancer. 1992;70(1):45–9.
Thorgeirsson SS, Grisham JW. Molecular pathogenesis of human hepatocellular carcinoma. Nat Genet. 2002;31(4):339–46.
El-Refaie A, Savage K, Bhattacharya S, Khakoo S, Harrison TJ, El-Batanony M, et al. HCV-associated hepatocellular carcinoma without cirrhosis. J Hepatol. 1996;24(3):277–85.
Trevisani F, Frigerio M, Santi V, Grignaschi A, Bernardi M. Hepatocellular carcinoma in non-cirrhotic liver: a reappraisal. Dig Liver Dis. 2010;42(5):341–7.
Farazi PA, DePinho RA. Hepatocellular carcinoma pathogenesis: from genes to environment. Nat Rev Cancer. 2006;6(9):674–87.
White DL, Kanwal F, El-Serag HB. Association between nonalcoholic fatty liver disease and risk for hepatocellular cancer, based on systematic review. Clin Gastroenterol Hepatol. 2012;10(12):1342–59.
Perumpail RB, Wong RJ, Ahmed A, Harrison SA. Hepatocellular carcinoma in the setting of non-cirrhotic nonalcoholic fatty liver disease and the metabolic syndrome: US experience. Dig Dis Sci. 2015;60(10):3142–8.
Siegel AB, Zhu AX. Metabolic syndrome and hepatocellular carcinoma: two growing epidemics with a potential link. Cancer. 2009;115(24):5651–61.
Guzman G, Brunt EM, Petrovic LM, Chejfec G, Layden TJ, Cotler SJ. Does nonalcoholic fatty liver disease predispose patients to hepatocellular carcinoma in the absence of cirrhosis? Arch Pathol Lab Med. 2008;132(11):1761–6.
Liu C, Sun L, Xu J, Zhao Y. Clinical efficacy of postoperative adjuvant transcatheter arterial chemoembolization on hepatocellular carcinoma. World J Surg Oncol. 2016;14:100.
Mergental H, Adam R, Ericzon BG, Kalicinski P, Mühlbacher F, Höckerstedt K, et al. Liver transplantation for unresectable hepatocellular carcinoma in normal livers. J Hepatol. 2012;57(2):297–305.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study did not receive any funding. No author has any financial conflict of interest. This article represents a retrospective review of an institutional experience and does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Lewis, R.H., Glazer, E.S., Bittenbinder, D.M. et al. Outcomes Following Resection of Hepatocellular Carcinoma in the Absence of Cirrhosis. J Gastrointest Canc 50, 808–815 (2019). https://doi.org/10.1007/s12029-018-0152-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-018-0152-x