Abstract
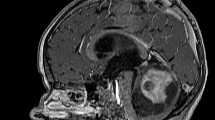
The aim of this study is to identify possible risks factors for the occurrence of cerebellar mutism syndrome (CMS) in children with posterior cranial fossa tumours. Children diagnosed with posterior fossa tumours consecutively admitted to our institution between 2006 and 2008 were the subjects of this prospective study. Besides standard neurological and radiological evaluations, all children underwent thorough neuropsychological assessments at admission and following surgery. Children under two or older than 16 years of age and those with a severe pre-operative clinical condition precluding neuropsychological assessment were excluded. Thirty-four children met the inclusion criteria. They were divided into two groups. Group I consisted of 23 children with normal language on admission and group II had 11 children showing pre-operative language impairment (PLI). PLI was observed in 11 children (32.4%: group II). Post-operatively, seven out of 34 children developed CMS (20.6%), all of them belonging to group II. In group II, indeed, the incidence of CMS was 63%. No case of CMS was observed in group I. PLI regressed after the operation in three out of the four subjects belonging to group II who did not develop CMS. PLI remained unchanged in the last child of this group. Posterior fossa tumour resection can have different effects on children with pre-existing language impairment (PLI). PLI can be considered a subclinical state of CMS in some children with posterior fossa tumour. However, in some children with PLI, the tumour resection may improve the linguistic abilities, as well as the other neurocognitive performances. In the present series, children with normal pre-operative language function did not develop post-operative mutism.


Similar content being viewed by others
References
Hirsch JF, Renier D, Czernichow P, Benveniste L, Pierre-Khan A. Medulloblastoma in childhood. Survival and functional results. Acta Neurochir (Wien). 1979;48:1–15.
Rekate HL, Grubb RL, Aram DM, Hahn JF, Ratcheson RA. Muteness of cerebellar origin. Arch Neurol. 1985;42(7):697–8.
Yonemasu Y: Cerebellar mutism and speech disturbance as a complication of posterior fossa surgery in children. 13th Annual Meeting of the Japanese Society for Pediatric Neurosurgery, Tsukuba, Japan, 1985.
Gelabert-Gonzalez M, Fernandez-Villa J. Mutism after posterior fossa surgery. Review of the literature. Clin Neurol Neurosurg. 2001;103:111–4.
Doxey D, Bruce D, Sklar F, Swift D, Shapiro K. Posterior fossa syndrome: identifiable risk factors and irreversible complications. Pediatr Neurosurg. 1999;31(3):131–6.
Van Calenbergh F, Van de Laar A, Plets C, Goffin J, Casaer P. Transient cerebellar mutism after posterior fossa surgery in children. Neurosurg. 1995;37(5):894–8.
Pollack IF, Polinko P, Albright LA, Towbin R, Fitz C. Mutism and pseudobulbar symptoms after resection of posterior fossa tumours in children: incidence and pathophysiology. Neurosurg. 1995;37:885–93.
Vandeinse D, Hornyak JE. Linguistic and cognitive deficits associated with cerebellar mutism. Pediatr Rehabil. 1997;1(1):41–4.
Crutchfeld JS, Sawaya R, Meyers CA, Moore III BD. Postoperative mutism in neurosurgery. J Neurosurg. 1994;81:115–21.
Dietze DD, Mickle JP. Cerebellar mutism after posterior fossa surgery. Pediat Neurosurg. 1990–1991;16:25–31.
Ersahin Y, Yararbas U, Duman Y, Mutluer S. Single photon emission tomography following posterior fossa surgery in patients with and without mutism. Child's Nerv Syst. 2002;18:318–25.
Frim DM, Ogilvy CS. Mutism and cerebellar dysarthria after brainstem surgery: case report. Neurosurg. 1995;36:854–7.
Robertson PL, Muraszko KM, Holmes E, Sposto R, Packer RJ, Gajjar A, et al. Incidence and severity of postoperative cerebellar mutism syndrome in children with medulloblastoma: a prospective study by the Children's Oncology Group. J Neurosurg. 2006;105:444–51. 6 Suppl Pediatrics.
Ammirati M, Mirzai S, Samii M. Transient mutism following removal of a cerebellar tumour: a case report and review of the literature. Childs Nerv Syst. 1989;5:12–4.
Fraioli B, Guidetti B. Effect of stereotactic lesions of the dentate nucleus of the cerebellum in man. Appl Neurophysiol. 1975;38:81–90.
Morris EB, Phillips NS, Laningham FH, Patay Z, Gajjar A, Wallace D, et al. Proximal dentatothalamocortical tract involvement in posterior fossa syndrome. Brain. 2009;132(Pt 11):3087–95.
Frassanito P, Massimi L, Caldarelli M, Di Rocco C. Cerebellar mutism after spontaneous intratumoural bleeding involving the upper cerebellar vermis: a contribution to the physiopathogenic interpretation. Childs Nerv Syst. 2009;25(1):7–11.
Marien P, Engelborghs S, Fabbro F, De Deyn PP. The lateralised linguistic cerebellum: a review and new hypothesis. Brain Lang. 2001;79:580–600.
Griffiths R. The abilities of young children. A comprehensive system of mental measure for the first 8 years of life. High Wycombe: The test agency Publisher; 1984. p. 21–245.
Griffiths R. The Griffiths mental development scales: from birth to 2 years. High Wycombe: The test agency Publisher; 1996. p. 32–267.
Orsini A, Picone L. WPPSI: Contributo alla taratura italiana. Florence: Organizzazioni Speciali Publisher; 1993. p. 31–128.
Leiter RG. Leiter International Performance Scale Revised (LIPS-R). Los Angeles: Western Psychological Service Publisher; 2002. p. 12–187.
Axia G. Primary language test. Florence: Organizzazioni Speciali Editor; 1995. p. 1–55.
Caselli MC, Casadio P. Il primo vocabolario del bambino. Milan: Franco Angeli Publisher; 1995. p. 25–76.
Rey A. Reattivo della figura complessa. Florence: Organizzazioni Speciali Publisher; 1959. p. 11–112.
Beery KE. VMI developmental test of visuo-motor integration. Florence: Organizzazioni Speciali Ed; 2000. p. 12–142.
Achenbach TM, Rescorla LA. Manual for the ASEBA preschool forms and profiles. Burlington: Library of Congress; 2000. p. 21–153.
Frigerio A, Cozzi C, Pastore V, Molteni M, Borgatti M, Montirosso R. La valutazione dei problemi emotivo comportamentali in un campione italiano di bambini in età prescolare attraverso la Child behavior Checklist e il Caregiver Teacher Report Form. Infanzia e adolescenza. 2006;5:24–37.
Mercuri E. Movement assessment battery for children second edition (Movement ABC-2) Italian version. Florence: Organizzazioni Speciali Publisher; 2000. p. 14–192.
Wechsler D. Wechsler intelligence scale for children- third edition: psychological corporation. San Antonio: Harcourt Brace Publisher; 2004. p. 14–187.
Orsini A, Picone L. WISC-III: Contributo alla taratura italiana. Florence: Organizzazioni Speciali Publisher; 2006. p. 23–210.
Biancardi A, Stoppa E. The bells test revised: a proposal for the study of attention in childhood. Psich dell'infanzia e dell'adolescenza. 1997;64:73–84.
Krikorian R, Bartok J, Gay N. Tower of London procedure: a standard method and developmental data. J Clin Exp Neuropsychol. 1994;16:840–50.
Luria AR. The working brain. London: Penguin Press Publisher; 1973. p. 12–156.
Vicari S, Pasqualetti P, Marotta L, Carlesimo GA. Word-list learning in normally developing children: effects of semantic organization and retention interval. It J Neurol Sci. 1999;12:119–28.
Reynolds CR, Bigler CR. (TOMAL) Test of memory and learning. Trento: Erickson Publisher; 1996. p. 24–196.
Fenson L, Dale P, Reznick S, Thal D, Bates E, Hartung J, et al. MacArthur communication development inventories. User's guide and technical manual. San Diego: Singular Publ Group Editor; 1993. p. 32–85.
Cipriani P, Bottari P, Chilosi AM, Pfanner L. A longitudinal perspective on the study of specific language impairment: The long term follow up of an Italian child. Int J of Lang and Communication Dis. 1998;3:245–80.
Cianchetti C, Sannio Fancello G. LAT Language assessment test. Trento: Erickson Publisher; 1997. p. 31–282.
Goodglass H, Weintraub S. Boston Naming Test, 2nd edn, Kaplan Ed.; 2002
Stella G, Pizzoli C, Tressoldi P. Il peabody test. Test di vocabolario recettivo. Turin: Omega Publisher; 2000. p. 14-–23.
Dunn LM. Peabody picture vocabulary test. Wilmington: Guidance Association Editor; 1981. p. 27–67.
Riva D, Nichelli F, Devoti M. Developmental aspects of verbal fluency and confrontation naming in children. Brain Lang. 2000;71:267–84.
American Psychiatric Association . DSM-IV-TR: Diagnostic and statistical manual of mental disorders, 4th ed. Text revision. Milan, Masson (ed.); 2000. pp. 31–291
Oldfield RC. The assessment and analysis of handedness: The Edinburgh Inventory. Neuropsychologia. 1971;9:97–113.
Crisante F, Lis A, Sambia M. Statistical analysis for psychologist. Florence: Giunti Barbera Publisher; 1992. p. 16–54.
VanDongen HR, Catsman-Berrevoets CE, VanMourik M. The syndrome of ‘cerebellar’ mutism and subsequent dysarthria. Neurology. 1994;44:2040–6.
Baillieux H, Weyns F, Paquier P, De Deyn PP, Marien P. Posterior fossa syndrome after a vermian stroke: a new case and review of the literature. Pediatr Neurosurg. 2007;43:386–95.
Riva D. The cerebellar contribution to language and sequential functions: evidence from a child with cerebellitis. Cortex. 1998;34(2):279–87.
Al-Anazi A, Hassounah M, Sheikh B, Barayan S. Cerebellar mutism by arteriovenous malformation of the vermis. Br J Neurosurg. 2001;15:47–50.
Akil H, Statham PFX, Gotz M, Bramley P, Whittle IR. Adult cerebellar mutism and cognitive-affective syndrome caused by cystic hemangioblastoma. Acta neurochir (Wien). 2006;148:597–8.
Drost G, Verrips A, Thijssen HO, Gabreëls. Cerebellar involvement as a rare complication of pneumococcal meningitis. Neuropediatrics. 2000;31(2):97–9.
Catsman-Berrevoets CE, VanDongen HR, Mulder PGH, Paz y Geuze M, Paquier PF, Lequin MH. Tumour type and size are high risk factors for the syndrome of cerebellar mutism and subsequent dysarthria. J Neurol Neurosurg Psychiatry. 1999;67:755–7.
Dailey AT, McKhann GM, Berger MS. The pathophysiology of oral pharyngeal apraxia and mutism following posterior fossa tumour resection in children. J Neurosurg. 1995;83:467–75.
Baillieux H, De Smet HJ, Paquier PF, De Deyn PP, Marien P. Cerebellar neurocognition: insights into the bottom of the brain. Clin Neurol Neuros. 2008;110:763–73.
Jansen A, Floel A, Van Randenborgh J, Konrad C, Rotte M, Forster AF, et al. Crossed cerebro-cerebellar dominance. Hum Brain Mapp. 2005;24:165–72.
Nicolson RI, Fawcett AJ, Dean P. Association of abnormal cerebellar activation with motor learning difficulties in dyslexic adults. Lancet. 1999;353:1662–7.
Thier P, Dicke PW, Haas R, Barash S. Encoding of movement time by population of cerebellar Purkinje cells. Nature. 2000;405:72–6.
Di Rocco C, Chieffo D, Pettorini BL, Massimi L, Caldarelli M, Tamburrini G. Preoperative and postoperative neurological, neuropsychological and behavioral impairment in children with posterior cranial fossa astrocytomas and medulloblastomas: the role of the tumor and the impact of the surgical treatment. Childs Nerv Syst. 2010;26:1173–88.
Humphreys RP. Mutism after posterior fossa surgery. In: Marlin AE, editor. Concepts in pediatric neurosurgery, vol. 9. Basel: Karger; 1989. p. 57–64.
Ferrante L, Mastronardi L, Acqui M, Fortuna A. Mutism after posterior fossa in children. J Neurosurg. 1990;72:959–63.
Ildan F, Tuna M, Erman T, Goçer AI, Zeren M, Cetinalp E. The evaluation and comparison of cerebellar mutism in children and adults after posterior fossa surgery: report of two adult cases and review of the literature. Acta Neuroch (Wien). 2002;144:463–73.
Souweidane MM. Posterior fossa syndrome. J Neurosurg Pediatr. 2010;5(4):326–8.
Acknowledgement
The authors would like to thank Federazione GENE for its constant support.
Disclosure
The authors declare that this paper has not been submitted elsewhere. The authors have not received financial assistance or inducement and declare that they have no known conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Di Rocco, C., Chieffo, D., Frassanito, P. et al. Heralding Cerebellar Mutism: Evidence for Pre-surgical Language Impairment as Primary Risk Factor in Posterior Fossa Surgery. Cerebellum 10, 551–562 (2011). https://doi.org/10.1007/s12311-011-0273-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-011-0273-2