Abstract
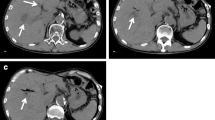
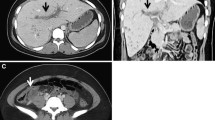
Spontaneous hemoperitoneum is an uncommon condition, which may be critical even if treated appropriately. The paraumbilical vein is a portosystemic collateral vein that develops in patients with portal hypertension, and is rarely found to be a source of bleeding. Here we present a case report of spontaneous hemoperitoneum due to rupture of the paraumbilical vein successfully treated with balloon-occluded retrograde transvenous obliteration (B-RTO). A 69-year-old man with cirrhosis due to nonalcoholic steatohepatitis was admitted to our hospital with abdominal distention and pain. Computed tomography revealed hemoperitoneum with a dilated paraumbilical vein, and rupture of the paraumbilical vein was diagnosed to be the cause of anemia. B-RTO was performed via the left femoral vein with upstream embolization using microcoils, and thrombosis of the paraumbilical vein was confirmed after B-RTO. The patient was discharged without complications 20 days after B-RTO and he experienced no further episodes of bleeding during the subsequent 6-month period.



Similar content being viewed by others
References
Lucey BC, Varghese JC, Anderson SW, Soto JA. Spontaneous hemoperitoneum: a bloody mess. Emerg Radiol. 2007;14:65–75.
Ellis H, Griffiths PW, MacIntyre A. Haemoperitoneum; a record of 129 consecutive patients with notes on some unusual cases. Br J Surg. 1958;45:606–10.
Goldstein AM, Gorlick N, Gibbs D, Fernandez-del Castillo C. Hemoperitoneum; a record of 129 consecutive patients with notes on some unusual cases. Am J Gastroenterol. 1995;90:315–7.
Ross AP. Portal hypertension presenting with haemoperitoneum. Br Med J. 1970;28:544.
Paizis B, Krespis E, Filiotou A, Kalochairetis P, Golematis B. Rupture of a periumbilical vein causing hemoperitoneum in a cirrhotic patient. Mt Sinai J Med. 1986;53:123–5.
Sato H, Kamibayashi S, Tatsumura T, Yamamoto K. Intraabdominal bleeding attributed to ruptured periumbilical varices. A case report and a review of the literature. Jpn J Surg. 1987;17:33–6.
Lee JM, Kim HL, Lee YH, Lee SH, Kim JK. Hemoperitoneum due to ruptured paraumbilical vein in a cirrhotic patient with portal hypertension: treatment by means of coil embolization. J Korean Radiol Soc. 2000;42:751–5.
Fox L, Crane SA, Bidari C, Jones A. Intra-abdominal hemorrhage from ruptured varices. Arch Surg. 1982;117:953–6.
Akriviadis EA. Hemoperitoneum in patients with ascites. Am J Gastroenterol. 1997;92:567–75.
Vallalta Morales M, Cano B, Morata Aldea C, Calabuig Alborch JR. Hemoperitoneum secondary to spontaneous rupture of the umbilical vein (in Spanish with English abstract). Gastroenterol Hepatol. 2004; 27: 414–6.
Sincos IR, Mulatti G, Mulatti S, Sincos IC, Belczak SQ, Zamboni V. Hemoperitoneum in a cirrhotic patient due to rupture of retroperitoneal varix. HPB Surg. 2009;2009:240780.
Hoevels J, Lunderquist A, Tylén U, Simert G. Porto-systemic collaterals in cirrhosis of the liver. Selective percutaneous transhepatic catheterization of the portal venous system in portal hypertension. Acta Radiol Diagn (Stockh). 1979; 20: 65–77.
Schabel SI, Rittenberg GM, Javid LH, Cunningham J, Ross P. The “bull’s-eye” falciform ligament: a sonographic finding of portal hypertension. Radiology. 1980;136:157–9.
McCain AH, Bernardino ME, Sones PJ Jr, Berkman WA, Casarella WJ. Varices from portal hypertension: correlation of CT and angiography. Radiology. 1985;154:63–9.
Cho KC, Patel YD, Wachsberg RH, Seeff J. Varices in portal hypertension: evaluation with CT. Radiographics. 1995;15:609–22.
Ohhira M, Ohta H, Ohhira M, Matsumoto A, Ohtake T, Fujimoto Y, et al. Altered intrahepatic pathway of para-umbilical vein in portal hypertension. J Gastroenterol Hepatol. 1998;13:691–5.
Zardi EM, Uwechie V, Caccavo D, Pellegrino NM, Cacciapaglia F, Di Matteo F, et al. Portosystemic shunts in a large cohort of patients with liver cirrhosis: detection rate and clinical relevance. J Gastroenterol. 2009;44:76–83.
Horton KM, Fishman EK. Paraumbilical vein in the cirrhotic patient: imaging with 3D CT angiography. Abdom Imaging. 1998;23:404–8.
Aagaard J, Jensen LI, Sorensen TI, Christensen U, Burcharth F. Recanalized umbilical vein in portal hypertension. AJR. 1982;139:1107–10.
Lafortune M, Constantin A, Breton G, Legare AG, Lavoie P. The recanalized umbilical vein in portal hypertension: a myth. AJR. 1985;144:549–53.
Lubner M, Menias C, Rucker C, Bhalla S, Peterson CM, Wang L, et al. Blood in the belly: CT findings of hemoperitoneum. Radiographics. 2007;27:109–25.
Shanmuganathan K, Mirvis SE, Sover ER. Value of contrast-enhanced CT in detecting active hemorrhage in patients with blunt abdominal or pelvic trauma. AJR. 1993;161:65–9.
Assis DN, Pollak J, Schilsky ML, Emre S. Successful treatment of a bleeding umbilical varix by percutaneous umbilical vein embolization with sclerotherapy. J Clin Gastroenterol. 2012;46:115–8.
Ohta M, Hashizume M, Kawanaka H, Akazawa K, Ueno K, Tomikawa M, et al. Complications of percutaneous transhepatic catheterization of the portal venous system in patients with portal hypertension. J Gastroenterol Hepatol. 1996;11:630–4.
Abraham AS, Atkinson M. The disappearance of ascites in alcoholic cirrhosis with the development of the Cruveilhier-Baumgarten syndrome. Ann Intern Med. 1965;62:1045–9.
Burchell AR, Panke WF, Moreno AH, Rousselot LM. The patent umbilical vein in portal hypertension. Surg Gynecol Obstet. 1970;130:77–86.
Gibson RN, Gibson PR, Donlan JD, Clunie DA. Identification of a patent paraumbilical vein by using Doppler sonography: importance in the diagnosis of portal hypertension. AJR. 1989;153:513–6.
Morin C, Lafortune M, Pomier G, Robin M, Breton G. Patent paraumbilical vein: anatomic and hemodynamic variants and their clinical importance. Radiology. 1992;185:253–6.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kitagawa, S., Sato, T., Yamazaki, K. et al. Spontaneous hemoperitoneum due to rupture of the paraumbilical vein successfully treated with balloon-occluded retrograde transvenous obliteration. Clin J Gastroenterol 6, 75–79 (2013). https://doi.org/10.1007/s12328-012-0349-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-012-0349-7