Abstract
Background
Cardiovascular risk factors are classically associated with coronary atherosclerosis. We sought to investigate whether risk factors are also associated with left ventricular (LV) dilatation, contractile impairment and reduced myocardial blood flow (MBF) in patients with non-ischemic LV dysfunction.
Methods
We studied 81 patients (59 males, age 60 ± 9 years) with mild-to-severe LV dysfunction (mean ejection fraction 37%, range 19%-50%), no history of diabetes and normal coronary arteries. Absolute MBF was measured by positron emission tomography and 13N-ammonia at rest and after dipyridamole (0.56 mg/kg I.V. over 4 min).
Results
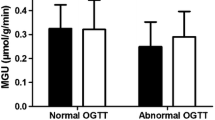
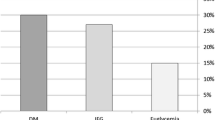
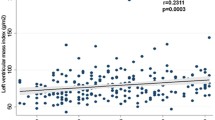
Overt LV dysfunction (LV end-diastolic diameter >60 mm associated with LV ejection fraction <45%) was present in 42 patients (52%); severely depressed hyperemic MBF (<1.09 mL · min−1 · g−1) was present in 41 patients (51%). Using multivariate logistic regression analysis, low high-density lipoprotein cholesterol (HDL-C, P < .036), newly diagnosed non-insulin-dependent diabetes or insulin-resistance (NIDD/IR, P < .019) and the use of diuretics (P = .001) were independently associated with overt LV dysfunction. Low HDL-C (P = .015) and NIDD/IR (P = .048) were also independently associated with severely depressed hyperemic MBF.
Conclusions
Low HDL-C and NIDD/IR are associated with more severe LV impairment and reduced hyperemic MBF in non-ischemic LV dysfunction.

Similar content being viewed by others
References
Camici PG, Crea F. Coronary microvascular dysfunction. N Engl J Med 2007;356:830-40.
Sambuceti G, Marzullo P, Giorgetti A, Neglia D, Marzilli M, Salvadori P, et al. Global alteration in perfusion response to increasing oxygen consumption in patients with single-vessel coronary artery disease. Circulation 1994;90:1696-705.
Kaufmann PA, Gnecchi-Ruscone T, Schäfers KP, Lüscher TF, Camici PG. Low density lipoprotein cholesterol and coronary microvascular dysfunction in hypercholesterolemia. J Am Coll Cardiol 2000;36:103-9.
Liga R, Marini C, Coceani M, Filidei E, Schlueter M, Bianchi M, et al. Structural abnormalities of the coronary arterial wall—in addition to luminal narrowing—affect myocardial blood flow reserve. J Nucl Med 2011;52:1704-12.
Murthy VL, Naya M, Foster CR, Hainer J, Gaber M, Di Carli G, et al. Improved cardiac risk assessment with non invasive measures of coronary flow reserve. Circulation 2011;124:2215-24.
Neglia D, Parodi O, Gallopin M, Sambuceti G, Giorgetti A, Pratali L, et al. Myocardial blood flow response to pacing tachycardia and to dipyridamole infusion in patients with dilated cardiomyopathy without overt heart failure. A quantitative assessment by positron emission tomography. Circulation 1995;92:796-804.
Neglia D, Michelassi C, Trivieri MG, Sambuceti G, Giorgetti A, Pratali L, et al. Prognostic role of myocardial blood flow impairment in idiopathic left ventricular dysfunction. Circulation 2002;105:186-93.
Rigo F, Gherardi S, Galderisi M, Pratali L, Cortigiani L, Sicari R, et al. The prognostic impact of coronary flow reserve assessed by Doppler echocardiography in non-ischemic dilated cardiomyopathy. Eur Heart J 2006;27:1319-23.
Tsagalou EP, Anastasiou-Nana M, Agapitos E, Gika A, Drakos SG, Terrovitis JV, et al. Depressed coronary flow reserve is associated with decreased myocardial capillary density in patients with heart failure due to idiopathic dilated cardiomyopathy. J Am Coll Cardiol 2008;52:1391-8.
Sampietro T, Neglia D, Bionda A, Dal Pino B, Bigazzi F, Puntoni M, et al. Inflammatory markers and serum lipids in idiopathic dilated cardiomyopathy. Am J Cardiol 2005;96:1718-20.
Bertoni AG, Tsai A, Kasper EK, Brancati FL. Diabetes and idiopathic cardiomyopathy: A nationwide case-control study. Diabetes Care 2003;26:2791-5.
Treasure CB, Vita JA, Cox DA, Fish RD, Gordon JB, Mudge GH, et al. Endothelium-dependent dilation of the coronary microvasculature is impaired in dilated cardiomyopathy. Circulation 1990;81:772-9.
Rye KA, Bursill CA, Lambert G, Tabet F, Barter PJ. The metabolism and anti-atherogenic properties of HDL. J Lipid Res 2009;50:S195-200.
Prior JO, Schindler TH, Facta AD, Hernandez-Pampaloni M, Campisi R, Dahlbom M, et al. Determinants of myocardial blood flow response to cold pressor testing and pharmacologic vasodilation in healthy humans. Eur J Nucl Med Mol Imaging 2007;34:20-7.
Witteles RM, Fowler MB. Insulin-resistant cardiomyopathy. Clinical evidence, mechanisms, and treatment options. J Am Coll Cardiol 2008;51:93-102.
From AM, Leibson CL, Bursi F, Redfield MM, Weston SA, Jacobsen SJ, et al. Diabetes in heart failure: Prevalence and impact on outcome in the population. Am J Med 2006;119:591-9.
Swan JW, Anker SD, Walton C, Godsland IF, Clark AL, Leyva F, et al. Insulin resistance in chronic heart failure: Relation to severity and etiology of heart failure. J Am Coll Cardiol 1997;30:527-32.
Kim JA, Montagnani M, Koh KK, Quon MJ. Reciprocal relationships between insulin resistance and endothelial dysfunction: Molecular and pathophysiological mechanisms. Circulation 2006;113:1888-904.
Nobécourt E, Tabet F, Lambert G, Puranik R, Bao S, Yan L, et al. Nonenzymatic glycation impairs the antiinflammatory properties of apolipoprotein A-I. Arterioscler Thromb Vasc Biol 2010;30:766-72.
Van Linthout S, Spillmann F, Riad A, Trimpert C, Lievens J, Meloni M, et al. Human apolipoprotein A-I gene transfer reduces the development of experimental diabetic cardiomyopathy. Circulation 2008;117:1563-73.
Chareonthaitawee P, Kaufmann PA, Rimoldi O, Camici PG. Heterogeneity of resting and hyperemic myocardial blood flow in healthy humans. Cardiovasc Res 2001;50:151-61.
Sdringola S, Johnson NP, Kirkeeide RL, Cid E, Gould KL. Impact of unexpected factors on quantitative myocardial perfusion and coronary flow reserve in young, asymptomatic volunteers. JACC Cardiovasc Imaging 2011;4:402-12.
Neglia D, De Maria R, Masi S, Gallopin M, Pisani P, Pardini S, et al. Effects of long-term treatment with carvedilol on myocardial blood flow in idiopathic dilated cardiomyopathy. Heart 2007;93:808-13.
Duvernoy CS, Meyer C, Seifert-Klauss V, Dayanikli F, Matsunari I, Rattenhuber J, et al. Gender differences in myocardial blood flow dynamics: Lipid profile and hemodynamic effects. J Am Coll Cardiol 1999;33:463-70.
Gould KL, Nakagawa Y, Nakagawa K, Sdringola S, Hess MJ, Haynie M, et al. Frequency and clinical implications of fluid dynamically significant diffuse coronary artery disease manifest as graded, longitudinal, base-to-apex myocardial perfusion abnormalities by noninvasive positron emission tomography. Circulation 2000;25:1931-9.
Bellina CR, Parodi O, Camici P, Salvadori PA, Taddei L, Fusani L, et al. Simultaneous in vitro and in vivo validation of nitrogen-13-ammonia for the assessment of regional myocardial blood flow. J Nucl Med 1990;31:1335-43.
Johnson NP, Gould KL. Physiological basis for angina and ST-segment change PET-verified thresholds of quantitative stress myocardial perfusion and coronary flow reserve. JACC Cardiovasc Imaging 2011;4:990-8.
Acknowledgments
We thank Elisa Rizza and Stefano Masi for helping collecting the data. We also thank Silvia Pardini and Danilo Bonora for the production of 13N-Ammonia and Alison Frank for helping editing the manuscript. This study was partly supported by the Genocor FIRB 2005 project of the Italian Ministry of Education, University and Research (Grant N. RBLA05ACJZ).
Conflicts of interest
The authors have indicated that they have no financial conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Neglia, D., Sampietro, T., Vecoli, C. et al. Abnormal glucose and lipid control in non-ischemic left ventricular dysfunction. J. Nucl. Cardiol. 19, 1182–1189 (2012). https://doi.org/10.1007/s12350-012-9609-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-012-9609-7