Abstract
Background context
Traumatic thoracolumbar discoligamentous injuries and partial burst fractures are commonly managed through posterior-only stabilization. Many cases present later with failure of posterior implant and progressive kyphotic deformities that necessitates major surgeries. Anterior interbody fusion saves the patients unnecessary long-segment fixation and provides a stable definitive solution for the injured segment.
Purpose
The purpose of this study is to assess the clinical and radiographic outcomes of combined minimal invasive short-segment posterior percutaneous instrumentation and anterior thoracoscopic-assisted fusion in thoracolumbar partial burst fractures or discoligamentous injuries.
Study design
Prospective observational study.
Patient sample
Thirty patients with acute thoracic or thoracolumbar injuries operated upon between December 2007 and January 2009.
Outcome measures
Oswestry Disability Index (ODI), clinical and neurological examination for clinical assessment. Plain X-ray for radiological evaluation.
Methods
Preoperative evaluation included clinical and neurological examination, plain X-rays, computed tomography (CT), and magnetic resonance imaging (MRI). Posterior short-segment percutaneous stabilization plus anterior thoracoscopically assisted fusion in prone position were done. The minimum follow-up period was 2 years (range 24–48 months).
Results
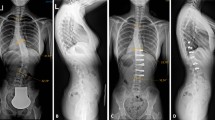
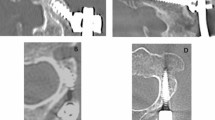
The mean age was 44 years. The commonest affected segment was between T10 and L1 (22 patients, 73 %). The mean total operative time was 103 min. The mean operative blood loss was 444 ml. Interbody fusion cage was used in 28 patients while iliac graft in two cases. Fusion rate at the final follow-up was 97 % (29 patients); one patient did not show definitive fusion although he was clinically satisfied. The mean final follow-up ODI was 12 %. The mean preoperative kyphosis angle was 22° improved to 6.5° postoperatively and was 7.5° at final follow-up. There were no major intraoperative or postoperative complications.
Conclusion
Combined anterior thoracoscopic fusion and short-segment posterior percutaneous instrumentation showed good clinical and radiographic outcomes in cases of thoracolumbar injuries through limiting the instrumented levels and preventing progress of posttraumatic kyphosis.


Similar content being viewed by others
References
Patel AA, Vaccaro AR (2010) Thoracolumbar spine trauma classification. J Am Acad Orthop Surg 18(No. 2):63–71
Oner FCW, Kirkham B, Smith JS, Shaffrey C (2010) Therapeutic decision making in thoracolumbar spine trauma. Spine 35(21S):S235–S244
Jansson KA, Svedmark P, Buskens E, Larsson M, Blomqvist P, Adami J (2009) Epidemiology of thoracolumbar spine fractures—a nationalwide study in Sweden. J Bone Joint Surg (Br) 91(SUPP I):22–23
McCormack T, Karaikovic E, Gaines RW (1994) The load sharing classification of spine fractures. Spine 19(15):1741–1744
Knop C, Fabian H, Bastian L et al (2002) Fate of the transpedicular intervertebral bone graft after posterior stabilisation of thoracolumbar fractures. Eur Spine J 11(3):251–257
Vaccaro AR, Lehman RA Jr, Hurlbert RJ et al (2005) A new classification of thoracolumbar injuries: the importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine 30:2325–2333
Shawky A et al (2013) Thoracoscopically assisted corpectomy and percutaneous transpedicular instrumentation in management of burst thoracic and thoracolumbar fractures. Eur Spine J Oct 22(10):2211–8. doi:10.1007/s00586-013-2835-0
Wiesner L, Kothe R, Ruther W (1999) Anatomical evaluation of two different techniques for the percutaneous insertion of pedicle screws in the lumbar spine. Spine 24:1599–1603
Wiesner L, Kothe R, Schulitz K-P, Ruether W (2000) Clinical evaluation and computed tomography scan analysis of screw tracts after percutaneous insertion of pedicle screws in the lumbar spine. Spine 25(5):615–621
Gullung G, Theiss SM (2008) Thoracolumbar spine: surgical treatment of thoracolumbar fractures: fusion versus nonfusion. Curr Orthop Pract 19(4):383–387
Alanay A, Acaroglu E, Yazici M et al (2001) Short-segment pedicle instrumentation of thoracolumbar burst fractures: does transpedicular intracorporeal grafting prevent early failure. Spine 26(2):213–217
Wood KB, Bohn D, Mehbod A (2005) Anterior versus posterior treatment of stable thoracolumbar burst fractures without neurologic deficit: a prospective, randomized study. J Spinal Disord Tech 18:15–23
DiMarco AF, Oca O, Renston JP (1995) Lung herniation. A cause of chronic chest pain following thoracotomy. Chest 107:877–879
Smith WD, Dakwar E, Le TV, Christian G, Serrano S, Uribe JS (2010) Minimally invasive surgery for traumatic spinal pathologies: a mini-open, lateral approach in the thoracic and lumbar. Spine 35(26S):S338–S346
Tofuku KK, Koga H, Ijiri K, Ishidou Y, Yamamoto T, Zenmyo M, Yone K, Komiya S (2012) Combined posterior and delayed staged mini-open anterior short-segment fusion for thoracolumbar burst fractures. J Spinal Disord Tech 25(1):38–46
Lieberman IH, Salo PT, Orr D et al (2000) Prone position endoscopic trans-thoracic release simultaneous with posterior instrumentation for spinal deformity. Spine 25:2251–2257
King AG, Mills TE, Loe WA, Chutkan NB, Revels TS (2000) Video-assisted thoracoscopic surgery in the prone position. Spine 18:2403–2406
Teitelbaum GP, Shaolian S, McDougall CG, Preul MC, Crawford NR, Sonntag VKH (2004) New percutaneously inserted spinal fixation system. Spine 29(6):703–709
Khoo LT, Palmer S, Laich DT et al (2002) Minimally invasive percutaneous posterior lumbar interbody fusion. Neurosurgery 51(suppl 2):166–181
Disclosures
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
(WMV 104,492 kb)
Rights and permissions
About this article
Cite this article
Shawky, A., El-Meshtawy, M. & Boehm, H. Thoracoscopic interbody fusion with percutaneous posterior stabilization for thoracic and thoracolumbar injuries. Eur Orthop Traumatol 5, 299–303 (2014). https://doi.org/10.1007/s12570-014-0251-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12570-014-0251-5