Abstract
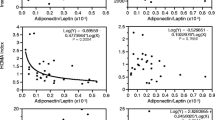
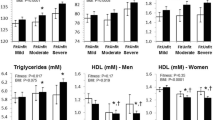
Adiposopathy, or sick fat, refers to adipose tissue dysfunction that can lead to several complications such as dyslipidemia, insulin resistance, and hyperglycemia. The relative contribution of adiposopathy in predicting insulin resistance remains unclear. We investigated the relationship between adiposopathy, as assessed as a low plasma adiponectin/leptin ratio, with anthropometry, body composition (hydrostatic weighing), insulin sensitivity (hyperinsulinemic-euglycemic clamp), inflammation, and fitness level (ergocycle VO2max, mL/kgFFM/min) in 53 men (aged 34–53 years) from four groups: sedentary controls without obesity (body mass index [BMI] <25 kg/m2), sedentary with obesity (BMI > 30 kg/m2), sedentary with obesity and glucose intolerance, and endurance trained active without obesity. The adiponectin/leptin ratio was the highest in trained men (4.75 ± 0.82) and the lowest in glucose intolerant subjects with obesity (0.27 ± 0.06; ANOVA p < 0.0001) indicating increased adiposopathy in those with obesity. The ratio was negatively associated with adiposity (e.g., waist circumference, r = −0.59, p < 0.01) and positively associated with VO2max (r = 0.67, p < 0.01) and insulin sensitivity (M/I, r = 0.73, p < 0.01). Multiple regression analysis revealed fitness as the strongest independent predictor of insulin sensitivity (partial R 2 = 0.61). While adiposopathy was also an independent and significant contributor (partial R 2 = 0.10), waist circumference added little power to the model (partial R 2 = 0.024). All three variables remained significant independent predictors when trained subjects were excluded from the model. Plasma lipids were not retained in the model. We conclude that low fitness, adiposopathy, as well as adiposity (and in particular abdominal obesity) are independent contributors to insulin resistance in men without diabetes.
Similar content being viewed by others
References
Alberti KG, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 15:539–553
Bays H (2005) Adiposopathy: role of adipocyte factors in a new paradigm. Expert Rev Cardiovasc Ther 3:187–189
Bays HE (2011) Adiposopathy is “sick fat” a cardiovascular disease? J Am Coll Cardiol 57:2461–2473
Bays H (2014) Adiposopathy, “sick fat,” Ockham’s razor, and resolution of the obesity paradox. Curr Atheroscler Rep 16:409
Bays H, Stein EA (2003) Pharmacotherapy for dyslipidaemia—current therapies and future agents. Expert Opin Pharmacother 4:1901–1938
Bays H, Abate N, Chandalia M (2005) Adiposopathy: sick fat causes high blood sugar, high blood pressure and dyslipidemia. Future Cardiol 1:39–59
Bays HE, Gonzalez-Campoy JM, Bray GA, Kitabchi AE, Bergman DA, Schorr AB, Rodbard HW, Henry RR (2008) Pathogenic potential of adipose tissue and metabolic consequences of adipocyte hypertrophy and increased visceral adiposity. Expert Rev Cardiovasc Ther 6:343–368
Borg GA (1982) Psychophysical bases of perceived exertion. Med Sci Sports Exerc 14:377–381
Bouchard C, Leon AS, Rao DC, Skinner JS, Wilmore JH, Gagnon J (1995) The HERITAGE family study. Aims, design, and measurement protocol. Med Sci Sports Exerc 27:721–729
Bruce CR, Dyck DJ (2004) Cytokine regulation of skeletal muscle fatty acid metabolism: effect of interleukin-6 and tumor necrosis factor-alpha. Am J Physiol Endocrinol Metab 287:E616–621
Caselli C (2014) Role of adiponectin system in insulin resistance. Mol Genet Metab 113:155–160
Desbuquois B, Aurbach GD (1971) Use of polyethylene glycol to separate free and antibody-bound peptide hormones in radioimmunoassays. J Clin Endocrinol Metab 33:732–738
Fletcher GF, Balady GJ, Amsterdam EA, Chaitman B, Eckel R, Fleg J, Froelicher VF, Leon AS, Pina IL, Rodney R, Simons-Morton DA, Williams MA, Bazzarre T (2001) Exercise standards for testing and training: a statement for healthcare professionals from the American Heart Association. Circulation 104:1694–1740
Fox CS, Massaro JM, Hoffmann U, Pou KM, Maurovich-Horvat P, Liu CY, Vasan RS, Murabito JM, Meigs JB, Cupples LA, D’Agostino RB Sr, O’Donnell CJ (2007) Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation 116:39–48
Galic S, Oakhill JS, Steinberg GR (2010) Adipose tissue as an endocrine organ. Mol Cell Endocrinol 316:129–139
Inoue M, Maehata E, Yano M, Taniyama M, Suzuki S (2005) Correlation between the adiponectin-leptin ratio and parameters of insulin resistance in patients with type 2 diabetes. Metabolism 54:281–286
Inoue M, Yano M, Yamakado M, Maehata E, Suzuki S (2006) Relationship between the adiponectin-leptin ratio and parameters of insulin resistance in subjects without hyperglycemia. Metabolism 55:1248–1254
Jung CH, Rhee EJ, Choi JH, Bae JC, Yoo SH, Kim WJ, Park CY, Mok JO, Kim CH, Lee WY, Oh KW, Park SW, Kim SW (2010) The relationship of adiponectin/leptin ratio with homeostasis model assessment insulin resistance index and metabolic syndrome in apparently healthy korean male adults. Korean Diabetes J 34:237–243
Katsuki A, Sumida Y, Murashima S, Murata K, Takarada Y, Ito K, Fujii M, Tsuchihashi K, Goto H, Nakatani K, Yano Y (1998) Serum levels of tumor necrosis factor-alpha are increased in obese patients with noninsulin-dependent diabetes mellitus. J Clin Endocrinol Metab 83:859–862
Khan M, Joseph F (2014) Adipose tissue and adipokines: the association with and application of adipokines in obesity. Scientifica (Cairo) 2014:328592
Kitahara CM, Trabert B, Katki HA, Chaturvedi AK, Kemp TJ, Pinto LA, Moore SC, Purdue MP, Wentzensen N, Hildesheim A, Shiels MS (2014) Body mass index, physical activity, and serum markers of inflammation, immunity, and insulin resistance. Cancer Epidemiol Biomarkers Prev 23:2840–2849
Kohno S, Ueji T, Abe T, Nakao R, Hirasaka K, Oarada M, Harada-Sukeno A, Ohno A, Higashibata A, Mukai R, Terao J, Okumura Y, Nikawa T (2011) Rantes secreted from macrophages disturbs skeletal muscle regeneration after cardiotoxin injection in Cbl-b-deficient mice. Muscle Nerve 43:223–229
Kwon H, Pessin JE (2013) Adipokines mediate inflammation and insulin resistance. Front Endocrinol (Lausanne) 4:13
Lee MJ, Wu Y, Fried SK (2013) Adipose tissue heterogeneity: implication of depot differences in adipose tissue for obesity complications. Mol Aspects Med 34:1–11
Mauriege P, Joanisse DR, CasparBauguil S, Cartier A, Lemieux I, Bergeron J, Biron S, Marceau P, Richard D (2015) Gene expression of different adipose tissues of severely obese women with or without a dysmetabolic profile. J Physiol Biochem 71:719–732
Mikines KJ, Sonne B, Farrell PA, Tronier B, Galbo H (1988) Effect of physical exercise on sensitivity and responsiveness to insulin in humans. Am J Physiol 254:E248–259
Oppert JM, Nadeau A, Tremblay A, Despres JP, Theriault G, Bouchard C (1997) Negative energy balance with exercise in identical twins: plasma glucose and insulin responses. Am J Physiol 272:E248–254
Piche ME, Weisnagel SJ, Corneau L, Nadeau A, Bergeron J, Lemieux S (2005) Contribution of abdominal visceral obesity and insulin resistance to the cardiovascular risk profile of postmenopausal women. Diabetes 54:770–777
Pigeon E, Riou ME, St-Onge J, Couillard E, Tremblay A, Marette A, Weisnagel SJ, Joanisse DR (2009) Validation of a simple index (SIisOGTT) of insulin sensitivity in a population of sedentary men. Diabetes Metab 35:398–403
Pradhan AD, Manson JE, Rifai N, Buring JE, Ridker PM (2001) C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA 286:327–334
Rice B, Janssen I, Hudson R, Ross R (1999) Effects of aerobic or resistance exercise and/or diet on glucose tolerance and plasma insulin levels in obese men. Diabetes Care 22:684–691
Richterich R, Dauwalder H (1971) Determination of plasma glucose by hexokinase-glucose-6-phosphate dehydrogenase method. Schweizerische medizinische Wochenschrift 101:615–618
Riou ME, Pigeon E, St-Onge J, Tremblay A, Marette A, Weisnagel J, Joanisse DR (2009) Cardiorespiratory fitness and components of the metabolic syndrome in sedentary men. Obes Facts 2:318–324
Sell H, Dietze-Schroeder D, Kaiser U, Eckel J (2006) Monocyte chemotactic protein-1 is a potential player in the negative cross-talk between adipose tissue and skeletal muscle. Endocrinology 147:2458–2467
Vega GL, Grundy SM (2013) Metabolic risk susceptibility in men is partially related to adiponectin/leptin ratio. J Obes 2013:409679
Wei M, Gibbons LW, Mitchell TL, Kampert JB, Lee CD, Blair SN (1999) The association between cardiorespiratory fitness and impaired fasting glucose and type 2 diabetes mellitus in men. Ann Intern Med 130:89–96
White MD, Bouchard G, Buemann B, Almeras N, Despres JP, Bouchard C (1985) Tremblay A (1996) reproducibility of 24-h energy expenditure and macronutrient oxidation rates in an indirect calorimeter. J Appl Physiol 80:133–139
Acknowledgments
We would like to express our heartfelt gratitude to the study participants. We would also like to thank Guy Fournier, Jean Doré, Marc Brunet, Linda Drolet, Nancy Parent, Marie Tremblay, Rollande Couture, Valérie-Ève Julien, Rachelle Duchesne, and Ginette Lapierre for their expert technical assistance in recruiting subjects and carrying out the clinical aspects of the study. This study was supported by grants from the Canadian Institutes of Health Research grant (MOP-68846) to DRJ and from the Fondation du Centre de Recherche de l’Institut Universitaire de Cardiologie et Pneumologie de Québec (CRIUCPQ) to DRJ and AM.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The research protocol was approved by the ethics committees of Université Laval (CERUL, approval 2004–2007) and the Centre de Recherche de l’Institut Universitaire de Cardiologie et Pneumologie de Québec (CRIUCPQ; approval 2013–2151), and all subjects provided written informed consent.
Rights and permissions
About this article
Cite this article
Huth, C., Pigeon, É., Riou, MÈ. et al. Fitness, adiposopathy, and adiposity are independent predictors of insulin sensitivity in middle-aged men without diabetes. J Physiol Biochem 72, 435–444 (2016). https://doi.org/10.1007/s13105-016-0488-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-016-0488-2