Abstract
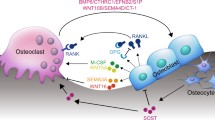
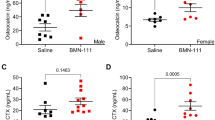
The taste receptor type 1 (TAS1R) family of heterotrimeric G protein-coupled receptors participates in monitoring energy and nutrient status. TAS1R member 3 (TAS1R3) is a bi-functional protein that recognizes amino acids such as L-glycine and L-glutamate or sweet molecules such as sucrose and fructose when dimerized with TAS1R member 1 (TAS1R1) or TAS1R member 2 (TAS1R2), respectively. It was recently reported that deletion of TAS1R3 expression in Tas1R3 mutant mice leads to increased cortical bone mass but the underlying cellular mechanism leading to this phenotype remains unclear. Here, we independently corroborate the increased thickness of cortical bone in femurs of 20-week-old male Tas1R3 mutant mice and confirm that Tas1R3 is expressed in the bone environment. Tas1R3 is expressed in undifferentiated bone marrow stromal cells (BMSCs) in vitro and its expression is maintained during BMP2-induced osteogenic differentiation. However, levels of the bone formation marker procollagen type I N-terminal propeptide (PINP) are unchanged in the serum of 20-week-old Tas1R3 mutant mice as compared to controls. In contrast, levels of the bone resorption marker collagen type I C-telopeptide are reduced greater than 60% in Tas1R3 mutant mice. Consistent with this, Tas1R3 and its putative signaling partner Tas1R2 are expressed in primary osteoclasts and their expression levels positively correlate with differentiation status. Collectively, these findings suggest that high bone mass in Tas1R3 mutant mice is due to uncoupled bone remodeling with reduced osteoclast function and provide rationale for future experiments examining the cell-type-dependent role for TAS1R family members in nutrient sensing in postnatal bone remodeling.



Similar content being viewed by others
References
Allendorph GP, Vale WW, Choe S (2006) Structure of the ternary signaling complex of a TGF-beta superfamily member. Proc Natl Acad Sci U S A 103:7643–7648. https://doi.org/10.1073/pnas.0602558103
Berasi SP, Varadarajan U, Archambault J, Cain M, Souza TA, Abouzeid A, Li J, Brown CT, Dorner AJ, Seeherman HJ, Jelinsky SA (2011) Divergent activities of osteogenic BMP2, and tenogenic BMP12 and BMP13 independent of receptor binding affinities. Growth Factors. https://doi.org/10.3109/08977194.2011.593178
Black DM, Bauer DC, Schwartz AV, Cummings SR, Rosen CJ (2012) Continuing bisphosphonate treatment for osteoporosis—for whom and for how long? N Engl J Med. https://doi.org/10.1056/NEJMp1202623
Bouxsein ML, Boyd SK, Christiansen BA, Guldberg RE, Jepsen KJ, Muller R (2010) Guidelines for assessment of bone microstructure in rodents using micro-computed tomography. J Bone Miner Res 25:1468–1486. https://doi.org/10.1002/jbmr.141
Dempster DW, Compston JE, Drezner MK, Glorieux FH, Kanis JA, Malluche H, Meunier PJ, Ott SM, Recker RR, Parfitt AM (2013) Standardized nomenclature, symbols, and units for bone histomorphometry: a 2012 update of the report of the ASBMR Histomorphometry Nomenclature Committee. J Bone Miner Res 28:2–17. https://doi.org/10.1002/jbmr.1805
El Hajj Dib I, Gallet M, Mentaverri R, Sevenet N, Brazier M, Kamel S (2006) Imatinib mesylate (Gleevec) enhances mature osteoclast apoptosis and suppresses osteoclast bone resorbing activity. Eur J Pharmacol 551:27–33. https://doi.org/10.1016/j.ejphar.2006.09.007
Heinecke K, Seher A, Schmitz W, Mueller TD, Sebald W, Nickel J (2009) Receptor oligomerization and beyond: a case study in bone morphogenetic proteins. BMC Biol 7:59. https://doi.org/10.1186/1741-7007-7-59
Indo Y, Takeshita S, Ishii KA, Hoshii T, Aburatani H, Hirao A, Ikeda K (2013) Metabolic regulation of osteoclast differentiation and function. J Bone Miner Res 28:2392–2399. https://doi.org/10.1002/jbmr.1976
Kokabu S, Gamer L, Cox K, Lowery J, Tsuji K, Raz R, Economides A, Katagiri T, Rosen V (2012) BMP3 suppresses osteoblast differentiation of bone marrow stromal cells via interaction with Acvr2b. Mol Endocrinol 26:87–94. https://doi.org/10.1210/me.2011-1168
Kokabu S, Lowery JW, Toyono T, Seta Y, Hitomi S, Sato T, Enoki Y, Okubo M, Fukushima Y, Yoda T (2015) Muscle regulatory factors regulate T1R3 taste receptor expression. Biochem Biophys Res Commun 468:568–573. https://doi.org/10.1016/j.bbrc.2015.10.142
Laffitte A, Neiers F, Briand L (2014) Functional roles of the sweet taste receptor in oral and extraoral tissues. Curr Opin Clin Nutr Metab Care 17:379–385. https://doi.org/10.1097/MCO.0000000000000058
Li B, Yu S (2003) Genistein prevents bone resorption diseases by inhibiting bone resorption and stimulating bone formation. Biol Pharm Bull 26:780–786
Lowery JW, Intini G, Gamer L, Lotinun S, Salazar VS, Ote S, Cox K, Baron R, Rosen V (2015) Loss of BMPR2 leads to high bone mass due to increased osteoblast activity. J Cell Sci 128:1308–1315. https://doi.org/10.1242/jcs.156737
Morini G, Bassoli A, Temussi PA (2005) From small sweeteners to sweet proteins: anatomy of the binding sites of the human T1R2_T1R3 receptor. J Med Chem 48:5520–5529. https://doi.org/10.1021/jm0503345
Pacheco-Costa R, Hassan I, Reginato RD, Davis HM, Bruzzaniti A, Allen MR, Plotkin LI (2014) High bone mass in mice lacking Cx37 because of defective osteoclast differentiation. J Biol Chem 289:8508–8520. https://doi.org/10.1074/jbc.M113.529735
Simon BR, Learman BS, Parlee SD, Scheller EL, Mori H, Cawthorn WP, Ning X, Krishnan V, Ma YL, Tyrberg B, MacDougald OA (2014) Sweet taste receptor deficient mice have decreased adiposity and increased bone mass. PLoS One 9:e86454. https://doi.org/10.1371/journal.pone.0086454
Wauson EM, Zaganjor E, Lee AY, Guerra ML, Ghosh AB, Bookout AL, Chambers CP, Jivan A, McGlynn K, Hutchison MR, Deberardinis RJ, Cobb MH (2012) The G protein-coupled taste receptor T1R1/T1R3 regulates mTORC1 and autophagy. Mol Cell 47:851–862. https://doi.org/10.1016/j.molcel.2012.08.001
Whitaker M, Guo J, Kehoe T, Benson G (2012) Bisphosphonates for osteoporosis—where do we go from here? N Engl J Med. https://doi.org/10.1056/NEJMp1202619
Zhao GQ, Zhang Y, Hoon MA, Chandrashekar J, Erlenbach I, Ryba NJ, Zuker CS (2003) The receptors for mammalian sweet and umami taste. Cell 115:255–266
Acknowledgements
We gratefully acknowledge the late John Martin (Harvard School of Dental Medicine μCT Core Facility) for his expertise and participation in this study. Histological preparation and staining was performed by Dr. Keith Condon (Indiana University School of Medicine).
Funding
This study was supported by a Marian University College of Osteopathic Medicine Faculty Research Development Award issued to JWL, Iowa Osteopathic Education and Research funds issued to EMW, and other intramural funds.
Author information
Authors and Affiliations
Contributions
JWL, BJD, and LP conceived of, designed, and supervised the study. MSE, NW, JBN, MP, HEF, JWA, SRS, AB, RS, EMW, JN, and HD generated the data and performed the statistical analyses. All authors interpreted the results, and JWL, BJD, NW, and TDW drafted the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Eaton, M.S., Weinstein, N., Newby, J.B. et al. Loss of the nutrient sensor TAS1R3 leads to reduced bone resorption. J Physiol Biochem 74, 3–8 (2018). https://doi.org/10.1007/s13105-017-0596-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-017-0596-7