Abstract
Background
The objective of breast reconstruction (BR) is to erase the after-effects of total mastectomy by allowing patients to restore their breast shape. The aim of our study was to investigate the body map integration of different types of BR using functional magnetic resonance (fMRI).
Patients and Methods
We prospectively enrolled all women undergoing BR for breast cancer to the Remasco study (NCT02553967). Participants were categorized into four groups according to the standard of care they required: immediate BR (IBR), delayed BR (DBR), flap (autologous), or implant BR. Each patient performed sensorimotor tasks during the fMRI acquisition.
Results
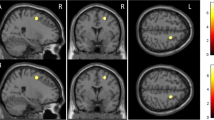
Data of 38 patients were analyzed. We identified the cingulate region as the area of interest in the brain. In the case of DBR, the brain area activated during palpation of the total mastectomy scar (before BR) was different from the brain area activated during palpation of the reconstructed breast (Brodmann areas 31 versus 32). Palpation of the native breast and reconstructed breast activated the same Brodmann area 32. Comparing the brain activation signal during palpation of the native breast and the reconstructed breast did not reveal any significant difference in the overall population (P = 0.41) or in the groups: autologous (P = 0.32), implant (P = 0.10), IBR (P = 0.72), or DBR (P = 0.10).
Conclusions
This experimental study allowed us to describe and understand the brain plasticity processes that accompany BR. The results suggest that the reconstructed breast is integrated into the body schema, regardless of the type of BR or the timing.





Similar content being viewed by others
References
Ferlay J, Colombet M, Soerjomataram I, Dyba T, Randi G, Bettio M, et al. Cancer incidence and mortality patterns in Europe: eestimates for 40 countries and 25 major cancers in 2018. Eur J Cancer. 2018;103:356–87. https://doi.org/10.1016/j.ejca.2018.07.005.
Kiebert GM, de Haes JC, van de Velde CJ. The impact of breast-conserving treatment and mastectomy on the quality of life of early-stage breast cancer patients: a review. J Clin Oncol. 1991;9:1059–70. https://doi.org/10.1200/JCO.1991.9.6.1059.
Pusic AL, Klassen AF, Scott AM, Klok JA, Cordeiro PG, Cano SJ. Development of a new patient-reported outcome measure for breast surgery: the BREAST-Q. Plast Reconstr Surg. 2009;124:345–53. https://doi.org/10.1097/PRS.0b013e3181aee807.
Popowich B, Kostaras X, Temple-Oberle C. Breast reconstruction after therapeutic or prophylactic mastectomy for breast cancer: a comparison of guideline recommendations. Eur J Surg Oncol. 2020;46:1046–51. https://doi.org/10.1016/j.ejso.2020.01.024.
Régis C, Le J, Chauvet M-P, Le Deley M-C, Le Teuff G. Variations in the breast reconstruction rate in France: a nationwide study of 19,466 patients based on the French medico-administrative database. The Breast. 2018;42:74–80. https://doi.org/10.1016/j.breast.2018.07.009.
Caterson SA, Fox SE, Tobias AM, Lee BT. Functional MRI To evaluate “Sense of Self” following perforator flap breast reconstruction. PLoS ONE. 2012;7:e49883. https://doi.org/10.1371/journal.pone.0049883.
Santosa KB, Qi J, Kim HM, Hamill JB, Wilkins EG, Pusic AL. Long-term patient-reported outcomes in postmastectomy breast reconstruction. JAMA Surg. 2018;153:891. https://doi.org/10.1001/jamasurg.2018.1677.
Nelson JA, Allen RJ, Polanco T, Shamsunder M, Patel AR, McCarthy CM, et al. Long-term patient-reported outcomes following postmastectomy breast reconstruction: an 8-year examination of 3268 patients. Ann Surg. 2019;270:473–83. https://doi.org/10.1097/SLA.0000000000003467.
Yousaf T, Dervenoulas G, Politis M. Chapter Two - Advances in MRI Methodology. In: Politis M, editor. Int Rev Neurobiol., vol. 141, Academic Press; 2018, p. 31–76. https://doi.org/10.1016/bs.irn.2018.08.008.
Anderson SR, Sieffert MR, Talarczyk CMR, Johnson RM, Fox MJP. Geographic variation in breast reconstruction modality use among women undergoing mastectomy. Ann Plast Surg. 2019;82:382–5. https://doi.org/10.1097/SAP.0000000000001746.
Reinders FCJ, Young-Afat DA, Batenburg MCT, Bruekers SE, van Amerongen EA, Macaré van Maurik JFM, et al. Higher reconstruction failure and less patient-reported satisfaction after post mastectomy radiotherapy with immediate implant-based breast reconstruction compared to immediate autologous breast reconstruction. Breast Cancer. 2020;27:435–44. https://doi.org/10.1007/s12282-019-01036-4.
Zhong T, Hu J, Bagher S, Vo A, O’Neill AC, Butler K, et al. A comparison of psychological response, body image, sexuality, and quality of life between immediate and delayed autologous tissue breast reconstruction: a prospective long-term outcome study. Plast Reconstr Surg. 2016;138:772–80. https://doi.org/10.1097/PRS.0000000000002536.
Matthews H, Turner A, Williamson I, Clyne W. ‘It’s a silver lining’: a template analysis of satisfaction and quality of life following post-mastectomy breast reconstruction. Br J Health Psychol. 2018;23:455–75. https://doi.org/10.1111/bjhp.12299.
Lagergren J, Edsander-Nord Å, Wickman M, Hansson P. Long-term sensibility following nonautologous, immediate breast reconstruction. Breast J. 2007;13:346–51. https://doi.org/10.1111/j.1524-4741.2007.00441.x.
Puonti HK, Broth TA, Soinila SO, Hallikainen HK, Jääskeläinen SK. How to assess sensory recovery after breast reconstruction surgery? Clin Breast Cancer. 2017;17:471–85. https://doi.org/10.1016/j.clbc.2017.04.011.
Shridharani S, Magarakis M, Stapleton S, Basdag B, Seal S, Rosson G. Breast Sensation after breast reconstruction: a systematic review. J Reconstr Microsurg. 2010;26:303–10. https://doi.org/10.1055/s-0030-1249313.
Alderman AK, Kuhn LE, Lowery JC, Wilkins EG. Does patient satisfaction with breast reconstruction change over time? Two-year results of the Michigan breast reconstruction outcomes study. J Am Coll Surg. 2007;204:7–12. https://doi.org/10.1016/j.jamcollsurg.2006.09.022.
Acknowledgements
The authors are particularly grateful to Delphine Hudry, Céline Renaudeau, and Julie Quemener who participated to the surgical management. Special thanks to Jessica Isaert, Communication department, Oscar Lambret Centre, who created the illustration for the visual abstract. We also thank the data managers from the Centre de Traitement des Données du Cancéropôle Nord-Ouest (CTD-CNO), who were in charge of the trial data management. The CTD-CNO clinical research platform was funded by the French National Cancer Institute (INCa) and La Ligue Nationale Contre le Cancer.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors declare that they have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 138290 kb)
Rights and permissions
About this article
Cite this article
Régis, C., Le Deley, MC., Bogart, E. et al. Functional Cerebral MRI Evaluation of Integration of Breast Reconstruction into the Body Schema. Ann Surg Oncol 29, 2652–2661 (2022). https://doi.org/10.1245/s10434-021-11048-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-11048-0