Abstract
Background
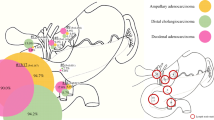
T2 intrahepatic cholangiocarcinoma (ICC) is defined as a solitary tumors with vascular invasion or multifocal tumors including satellite lesions, multiple lesions, and intrahepatic metastases. This study aimed to evaluate the prognosis associated with multifocal tumors.
Methods
The National Cancer Database was queried from 2004 to 2017 for patients with non-metastatic ICC. The patients were grouped based on T2 staging, multifocality, and lymph node involvement.
Results
The study enrolled and classified 4887 patients into clinical (c) stage groups as follows: 15.2% with solitary T2N0 (sT2N0) tumors, 21.3% with multifocal T2N0 (mT2N0) tumors, and 63.5% with node-positive (TxN1) disease. Patients with (c)sT2N0 tumors had higher rates of surgical resection than those with (c)mT2N0 or (c)TxN1 disease (33.5% vs 19.7% vs 15.0%; p < 0.01). Median overall survival (OS) was better for the patients with (c)sT2N0 tumors than for those with multifocal and node-positive disease (15.4 vs 10.4 vs 10.4 months; p < 0.01). On multivariate analysis, (c)sT2N0 tumors were associated with better OS than (c)mT2N0 tumors [hazard ratio (HR), 1.31; 95% confidence interval (CI), 1.17–1.46; p < 0.01] or (c)TxN1 disease (HR,1.41; 95% CI 1.28–1.56; p < 0.01). In a subset analysis based on pathologic (p) staging of patients who underwent surgical resection with regional lymphadenectomy, multivariate analysis demonstrated that (p)sT2N0 tumors were associated with better OS than (p)mT2N0 tumors (HR,1.40; 95% CI 1.03–1.92; p = 0.03) or (p)TxN1 disease (HR, 2.05; 95% CI 1.62–2.58; p < 0.01).
Conclusions
Multifocal T2N0 ICC is associated with poor OS and has a disparate prognosis compared with solitary T2N0 disease, even among patients who undergo resection. Future staging criteria should account for the poor outcomes associated with multifocal ICC.




Similar content being viewed by others
References
Zhang H, Yang T, Wu M, Shen F. Intrahepatic cholangiocarcinoma: epidemiology, risk factors, diagnosis, and surgical management. Cancer Lett. 2016;379:198–205.
Singal AK, Vauthey JN, Grady JJ, Stroehlein JR. Intra-hepatic cholangiocarcinoma—frequency and demographic patterns: thirty-year data from the M.D. Anderson Cancer Center. J Cancer Res Clin Oncol. 2011;137:1071–8.
Buettner S, Galjart B, van Vugt JLA, et al. Performance of prognostic scores and staging systems in predicting long-term survival outcomes after surgery for intrahepatic cholangiocarcinoma. J Surg Oncol. 2017;116:1085–95.
Tabrizian P, Jibara G, Hechtman JF, et al. Outcomes following resection of intrahepatic cholangiocarcinoma. HPB Oxford. 2015;17:344–51.
Weber SM, Ribero D, O’Reilly EM, Kokudo N, Miyazaki M, Pawlik TM. Intrahepatic cholangiocarcinoma: expert consensus statement. HPB Oxford. 2015;17:669–80.
Buettner S, Ten Cate DWG, Bagante F, et al. Survival after resection of multiple tumor foci of intrahepatic cholangiocarcinoma. J Gastrointest Surg. 2019;23:2239–46.
Addeo P, Jedidi I, Locicero A, et al. Prognostic impact of tumor multinodularity in intrahepatic cholangiocarcinoma. J Gastrointest Surg. 2019;23:1801–9.
Amin MB, Edge S, Greene F, Byrd DR, Brookland RK, Washington MK, et al editors. AJCC Cancer Staging Manual. 8th edn. Berlin: Springer; 2017.
Wang Y, Li J, Xia Y, et al. Prognostic nomogram for intrahepatic cholangiocarcinoma after partial hepatectomy. J Clin Oncol. 2013;31:1188–95.
Hyder O, Marques H, Pulitano C, et al. A nomogram to predict long-term survival after resection for intrahepatic cholangiocarcinoma: an Eastern and Western experience. JAMA Surg. 2014;149:432–8.
de Jong MC, Nathan H, Sotiropoulos GC, et al. Intrahepatic cholangiocarcinoma: an international multi-institutional analysis of prognostic factors and lymph node assessment. J Clin Oncol. 2011;29:3140–5.
Mavros MN, Economopoulos KP, Alexiou VG, Pawlik TM. Treatment and prognosis for patients with intrahepatic cholangiocarcinoma: systematic review and meta-analysis. JAMA Surg. 2014;149:565–74.
Zhang XF, Chakedis J, Bagante F, et al. Trends in use of lymphadenectomy in surgery with curative intent for intrahepatic cholangiocarcinoma. Br J Surg. 2018;105:857–66.
Jutric Z, Johnston WC, Hoen HM, et al. Impact of lymph node status in patients with intrahepatic cholangiocarcinoma treated by major hepatectomy: a review of the National Cancer Database. HPB Oxford. 2016;18:79–87.
National Cancer Database. American College of Surgeons. https://www-facs-org.proxy.libraries.uc.edu/quality-programs/cancer/ncdb. (2020)
Raoof M, Dumitra S, Ituarte PHG, et al. Development and validation of a prognostic score for intrahepatic cholangiocarcinoma. JAMA Surg. 2017;152:e170117.
Chen Y, Weng S. Reappraisal of the T category for solitary intrahepatic cholangiocarcinoma by tumor size in 611 early-stage (T1-2N0M0) patients after hepatectomy: a surveillance, epidemiology, and end results (SEER) analysis. J Gastrointest Surg. 2020;25:1989–99.
Yamamoto Y, Sugiura T, Okamura Y, et al. The Evaluation of the eight edition of the AJCC/UICC staging system for intrahepatic cholangiocarcinoma: a proposal of a modified new staging system. J Gastrointest Surg. 2020;24:786–95.
Wright GP, Perkins S, Jones H, et al. Surgical resection does not improve survival in multifocal intrahepatic cholangiocarcinoma: a comparison of surgical resection with intra-arterial therapies. Ann Surg Oncol. 2018;25:83–90.
Zhang XF, Xue F, He J, et al. Proposed modification of the eighth edition of the AJCC staging system for intrahepatic cholangiocarcinoma. Surg Oncol. 2021;23:1456–66.
Conci S, Ruzzenente A, Viganò L, et al. Patterns of distribution of hepatic nodules (single, satellites or multifocal) in intrahepatic cholangiocarcinoma: prognostic impact after surgery. Ann Surg Oncol. 2018;25:3719–27.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Davendra Sohal: Speakers Bureau–Incyte; Consulting–Astra Zeneca; Funding–Ability Pharma, Amgen, Apexigen, Astra Zeneca, Bristol-Myers Squibb, FibroGen, Genentech, Merck, Rafael, Roche.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Turner, K.M., Delman, A.M., Kharofa, J. et al. A National Assessment of T2 Staging for Intrahepatic Cholangiocarcinoma and the Poor Prognosis Associated with Multifocality. Ann Surg Oncol 29, 5094–5102 (2022). https://doi.org/10.1245/s10434-022-11762-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-11762-3