Abstract
Objective and design
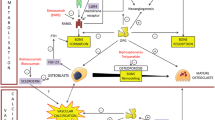
Evaluating the pro-/anti-inflammatory activity of the C-terminal cleavage product of osteopontin in comparison to angiotensin 1–7.
Material and subjects
Human coronary endothelial cells (hcEC) treated with conditioned media from human U937 macrophages.
Treatment
Macrophages were (pre)treated with C-terminal, full-length or N-terminal osteopontin (OPN-C, OPN-FL, OPN-N, respectively), angiotensin II, angiotensin 1–7 or TNF-α. OPN-C modulatory capacity was compared to that of Ang1–7 in inhibiting subsequent Ag II, OPN-FL or OPN-N-induced macrophage-mediated endothelial inflammation.
Methods
Protein expression of NFκB, IκB, vCAM-1 and iCAM-1 was assessed using western blot. Promotor activation by NFκB was also assessed by dual-luciferase reporter assay.
Results
Conditioned media of macrophages treated with OPN-C induced hcECs’ NfκB activation to a lower degree than OPN-FL or OPN-N. Priming of macrophages with angiotensin 1–7 attenuated the endothelial pro-inflammatory effect induced by subsequent exposure of the macrophages to angiotensin II, OPN-FL or OPN-N. This was evidenced by both NfκB activation and vCAM and iCAM expression. In contrast, priming macrophages with OPN-C did not significantly attenuate the subsequent response to the pro-inflammatory cytokines.
Conclusions
OPN-C induces lower macrophage-induced endothelial inflammation compared to OPN-FL or OPN-N, but unlike angiotensin 1–7, fails to prevent endothelial inflammation induced by subsequent pro-inflammatory macrophage stimulation.







Similar content being viewed by others
References
Hansson GK. Inflammation, atherosclerosis, and coronary artery disease. N Engl J Med. 2005;352:1685–95.
Bremner P, Heinrich M. Natural products as targeted modulators of the nuclear factor-kappaB pathway. J Pharm Pharmacol. 2002;54:453–72.
Min JK, Kim YM, Kim SW, Kwon MC, Kong YY, Hwang IK, et al. TNF-related activation-induced cytokine enhances leukocyte adhesiveness: induction of ICAM-1 and VCAM-1 via TNF receptor-associated factor and protein kinase C-dependent NF-kappaB activation in endothelial cells. J Immunol. 2005;175:531–40.
Liu J, Ren Y, Kang L, Zhang L. Oxidized low-density lipoprotein increases the proliferation and migration of human coronary artery smooth muscle cells through the upregulation of osteopontin. Int J Mol Med. 2014;33:1341–7.
Bruemmer D, Collins AR, Noh G, Wang W, Territo M, Arias-Magallona S, et al. Angiotensin II-accelerated atherosclerosis and aneurysm formation is attenuated in osteopontin-deficient mice. J Clin Investig. 2003;112:1318–31.
Ogawa D, Stone JF, Takata Y, Blaschke F, Chu VH, Towler DA, et al. Liver x receptor agonists inhibit cytokine-induced osteopontin expression in macrophages through interference with activator protein-1 signaling pathways. Circ Res. 2005;96:e59–e67.
Ding Y, Chen J, Cui G, Wei Y, Lu C, Wang L, et al. Pathophysiological role of osteopontin and angiotensin II in atherosclerosis. Biochem Biophys Res Commun. 2016;471:5–9.
Wolak T, Kim H, Ren Y, Kim J, Vaziri ND, Nicholas SB. Osteopontin modulates angiotensin II-induced inflammation, oxidative stress, and fibrosis of the kidney. Kidney Int. 2009;76:32–43.
Golledge J, Cullen B, Rush C, Moran CS, Secomb E, Wood F, et al. Peroxisome proliferator-activated receptor ligands reduce aortic dilatation in a mouse model of aortic aneurysm. Atherosclerosis. 2010;210:51–6.
Yousif MH, Benter IF, Diz DI, Chappell MC. Angiotensin-(1–7)-dependent vasorelaxation of the renal artery exhibits unique angiotensin and bradykinin receptor selectivity. Peptides. 2017;90:10–6.
Sullivan J, Blair L, Alnajar A, Aziz T, Ng CY, Chipitsyna G, et al. Expression of a prometastatic splice variant of osteopontin, OPNC, in human pancreatic ductal adenocarcinoma. Surgery. 2009;146:232–40.
Scatena M, Liaw L, Giachelli CM. Osteopontin: a multifunctional molecule regulating chronic inflammation and vascular disease. Arterioscler Thromb Vasc Biol. 2007;27:2302–9.
Denhardt DT, Noda M, O’Regan AW, Pavlin D, Berman JS. Osteopontin as a means to cope with environmental insults: regulation of inflammation, tissue remodeling, and cell survival. J Clin Investig. 2001;107:1055–61.
Uchinaka A, Hamada Y, Mori S, Miyagawa S, Saito A, Sawa Y, et al. SVVYGLR motif of the thrombin-cleaved N-terminal osteopontin fragment enhances the synthesis of collagen type III in myocardial fibrosis. Mol Cell Biochem. 2015;408:191–203.
Hamias R, Volvich L, Paran E, Sion-Vardi N, Novack V, Szendro G, et al. Low osteopontin N-terminal fragment and carotid plaque stability associated with statin or antiplatelet therapy. Curr Vasc Pharmacol. 2016;14(3):288–94.
Wolak T, Sion-Vardi N, Novack V, Greenberg G, Szendro G, Tarnovscki T, et al. N-terminal rather than full-length osteopontin or its C-terminal fragment is associated with carotid-plaque inflammation in hypertensive patients. American journal of hypertension. 2013;26:326–33.
Ozaki S, Kurata M, Kumon Y, Matsumoto S, Tagawa M, Watanabe H, et al. Plasma thrombin-cleaved osteopontin as a potential biomarker of acute atherothrombotic ischemic stroke. Hypertens Res. 2017;40(1):61–6.
Lai CF, Seshadri V, Huang K, Shao JS, Cai J, Vattikuti R, et al. An osteopontin-NADPH oxidase signaling cascade promotes pro-matrix metalloproteinase 9 activation in aortic mesenchymal cells. Circ Res. 2006;98:1479–89.
Takahashi K, Takahashi F, Tanabe KK, Takahashi H, Fukuchi Y. The carboxyl-terminal fragment of osteopontin suppresses arginine-glycine-asparatic acid-dependent cell adhesion. Biochem Mol Biol Int. 1998;46:1081–92.
Maeda K, Takahashi K, Takahashi F, Tamura N, Maeda M, Kon S, et al. Distinct roles of osteopontin fragments in the development of the pulmonary involvement in sarcoidosis. Lung. 2001;179:279–91.
Shao Z, Morser J, Leung LL. Thrombin cleavage of osteopontin disrupts a pro-chemotactic sequence for dendritic cells, which is compensated by the release of its pro-chemotactic C-terminal fragment. J Biol Chem. 2014;289:27146–58.
Plumer A, Duan H, Subramaniam S, Lucas FL, Miesfeldt S, Ng AK, et al. Development of fragment-specific osteopontin antibodies and ELISA for quantification in human metastatic breast cancer. BMC Cancer. 2008;8:38.
Ridruechai C, Sakurada S, Yanai H, Yamada N, Kantipong P, Piyaworawong S, et al. Association between circulating full-length osteopontin and IFN-gamma with disease status of tuberculosis and response to successful treatment. Southeast Asian J Trop Med Public Health. 2011;42:876–89.
Christensen B, Klaning E, Nielsen MS, Andersen MH, Sorensen ES. C-terminal modification of osteopontin inhibits interaction with the alphaVbeta3-integrin. J Biol Chem. 2012;287:3788–97.
Kim HJ, Lee HJ, Jun JI, Oh Y, Choi SG, Kim H, et al. Intracellular cleavage of osteopontin by caspase-8 modulates hypoxia/reoxygenation cell death through p53. Proc Natl Acad Sci USA. 2009;106:15326–31.
Boggio E, Dianzani C, Gigliotti CL, Soluri MF, Clemente N, Cappellano G, et al. Thrombin cleavage of osteopontin modulates its activities in human cells in vitro and mouse experimental autoimmune encephalomyelitis in vivo. J Immunol Res. 2016;2016:9345495.
Mi Z, Oliver T, Guo H, Gao C, Kuo PC. Thrombin-cleaved COOH(−) terminal osteopontin peptide binds with cyclophilin C to CD147 in murine breast cancer cells. Cancer Res. 2007;67:4088–97.
Kaartinen MT, El-Maadawy S, Rasanen NH, McKee MD. Tissue transglutaminase and its substrates in bone. J Bone Miner Res. 2002;17:2161–73.
Giachelli CM, Liaw L, Murry CE, Schwartz SM, Almeida M. Osteopontin expression in cardiovascular diseases. Ann N Y Acad Sci. 1995;760:109–26.
Sharif SA, Du X, Myles T, Song JJ, Price E, Lee DM, et al. Thrombin-activatable carboxypeptidase B cleavage of osteopontin regulates neutrophil survival and synoviocyte binding in rheumatoid arthritis. Arthritis Rheum. 2009;60:2902–12.
Agnihotri R, Crawford HC, Haro H, Matrisian LM, Havrda MC, Liaw L. Osteopontin, a novel substrate for matrix metalloproteinase-3 (stromelysin-1) and matrix metalloproteinase-7 (matrilysin). J Biol Chem. 2001;276:28261–7.
Kon S, Nakayama Y, Matsumoto N, Ito K, Kanayama M, Kimura C, et al. A novel cryptic binding motif, LRSKSRSFQVSDEQY, in the C-terminal fragment of MMP-3/7-cleaved osteopontin as a novel ligand for alpha9beta1 integrin is involved in the anti-type II collagen antibody-induced arthritis. PLoS One. 2014;9:e116210.
Christensen B, Zachariae ED, Scavenius C, Thybo M, Callesen MM, Kloverpris S, et al. Identification of transglutaminase reactive residues in human osteopontin and their role in polymerization. PLoS One. 2014;9:e113650.
Das R, Philip S, Mahabeleshwar GH, Bulbule A, Kundu GC. Osteopontin: it’s role in regulation of cell motility and nuclear factor kappa B-mediated urokinase type plasminogen activator expression. IUBMB Life. 2005;57:441–7.
Philip S, Kundu GC. Osteopontin induces nuclear factor kappa B-mediated promatrix metalloproteinase-2 activation through I kappa B alpha /IKK signaling pathways, and curcumin (diferulolylmethane) down-regulates these pathways. J Biol Chem. 2003;278:14487–97.
Matusan-Ilijas K, Damante G, Fabbro D, Dordevic G, Hadzisejdic I, Grahovac M, et al. EGFR expression is linked to osteopontin and Nf-kappaB signaling in clear cell renal cell carcinoma. Clin Transl Oncol. 2013;15:65–71.
Matusan-Ilijas K, Damante G, Fabbro D, Dordevic G, Hadzisejdic I, Grahovac M, et al. Osteopontin expression correlates with nuclear factor-kappaB activation and apoptosis downregulation in clear cell renal cell carcinoma. Pathol Res Pract. 2011;207:104–10.
Raja R, Kale S, Thorat D, Soundararajan G, Lohite K, Mane A, et al. Hypoxia-driven osteopontin contributes to breast tumor growth through modulation of HIF1alpha-mediated VEGF-dependent angiogenesis. Oncogene. 2014;33:2053–64.
Urtasun R, Lopategi A, George J, Leung TM, Lu Y, Wang X, et al. Osteopontin, an oxidant stress sensitive cytokine, up-regulates collagen-I via integrin alpha(V)beta(3) engagement and PI3K/pAkt/NFkappaB signaling. Hepatology. 2012;55:594–608.
Pandey A, Goru SK, Kadakol A, Malek V, Gaikwad AB. Differential regulation of angiotensin converting enzyme 2 and nuclear factor-kappaB by angiotensin II receptor subtypes in type 2 diabetic kidney. Biochimie. 2015;118:71–81.
Acknowledgements
This study was supported by grant from the Israel Ministry of Health (Grant no. 8736511; 3-9937 for TW and AR).
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: John Di Battista.
Electronic supplementary material
Below is the link to the electronic supplementary material.
11_2017_1120_MOESM1_ESM.tif
Supplementary Figure 1. Ag II, OPN-FL and OPN-N expression in conditioned media. Western blot of AgII, OPN-FL and OPN-N MQ condition media: before PBS wash versus the conditioned media that was applied onto the endothelial cells; after PBS wash and incubated overnight for additional 16 h with fresh medium (TIF 96 KB)
11_2017_1120_MOESM2_ESM.tif
Supplementary Figure 2. NfκB and IκB expression induced by inflammatory stimulation. (A) Macrophages from U937 cells were treated with vehicle, angiotensin II (Ag II), angiotensin 1-7 (Ag 1-7), TNF-α, OPN-FL or vehicle OPN-FL, OPN-N, OPN overnight, then washed and incubated overnight with fresh medium. This medium was transferred onto human coronary endothelial cells for another 16 h. (B) Representative blots of cytoplasmatic NfκB, IκB and nuclear NfκB after stimulation with vehicle, Ag 1-7, Ag II, TNF-α or OPN-FL. Quantification of signals from western blot: column bars (mean±SEM) treated with vehicle, Ag 1-7, Ag II, TNF-α or OPN-FL: for cytoplasmatic NfκB: p<0.001; nuclear NfκB: p=0.0017. One-way Anova with Kruskal–Wallis test. All data are the mean change of n=3 per treatment (TIF 159 KB)
11_2017_1120_MOESM3_ESM.tif
Supplementary Figure 3. The effect of pretreatment with Ag 1-7 and OPN-C on OPN-rFL induced NfκB and IκB endothelial expression. (A) Representative blots of cytoplasmatic NfkB and IkB and nuclear NfkB of control and after pretreatment with vehicle, OPN-C or Ag 1-7 before stimulation with OPN-rFL. (B) Quantification of western blot signals (mean±SEM) bars column treated with control, pretreatment with vehicle, OPN-C, or Ag 1-7 from cytoplasmatic NfκB:p<0.001; IκB: p=0.0014; nuclear NfκB: p<0.001. The effect of pre treatment with Ag 1-7 and OPN-C on OPN-rFL induced vCAM and iCAM endothelial expression. (C) Representative blots of whole cell lysates of vCAM and iCAM of control and after pretreatment with vehicle, OPN-C, or Ag 1-7 before stimulation with OPN-rFL. (D) Quantification of signals from vCAM western blot: column bars (mean±SEM) of control, vehicle, OPN-C, or Ag 1-7: p=0.0014. Quantification of signals iCAM from western blot: column bars (mean±SEM) of control, vehicle, OPN-C or Ag 1-7: p=0.014. One-way Anova with Kruskal–Wallis test. All data are the mean change of n=3 per treatment (TIF 159 KB)
Rights and permissions
About this article
Cite this article
Hamias, R., Rudich, A., Greenberg, G. et al. Angiotensin 1–7, but not the thrombin-cleaved osteopontin C-terminal fragment, attenuates osteopontin-mediated macrophage-induced endothelial-cell inflammation. Inflamm. Res. 67, 265–275 (2018). https://doi.org/10.1007/s00011-017-1120-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-017-1120-9