Abstract
Background
Thyroid cancer is the most common endocrine malignancy with relatively good prognosis in children. However, unlike adults, children usually present with more advanced disease and have a higher local recurrence and distant metastases. Thus surveillance for recurrence is a major goal of long-term follow-up.
Objective
This retrospective study evaluates the diagnostic value of ultrasound (US) imaging in the post-therapy surveillance of children with differentiated thyroid cancer.
Materials and methods
We reviewed the charts of 54 children (40 girls; mean age 14.3 ± 3.6 years) with differentiated thyroid cancer treated with total or near-total thyroidectomy. Forty children (29 girls and 11 boys) who had routine follow-up US examinations (112 studies) were included for the evaluation of US accuracy in the follow-up of pediatric differentiated thyroid cancer. Histopathology, stimulated thyroglobulin determination, post-therapy whole-body iodine scan and clinical follow-up were used as the standards of reference.
Results
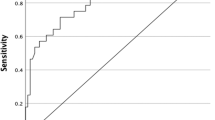
Mean period of follow-up was 34 months. The frequency of recurrence was 42% (17/40). Seventeen percent of the children had lung metastases either at presentation or on follow-up. In all cases of lung metastases, stimulated thyroglobulin level was greater than 10 ng/ml. The sensitivity was 85.7%, specificity 89.4%, negative predictive value 94.4% and positive predictive value 75% for US in detecting loco-regional recurrence in follow-up studies of pediatric differentiated thyroid cancer. In 17.3% (18/104) of studies, the results of stimulated thyroglobulin and US were discordant.
Conclusion
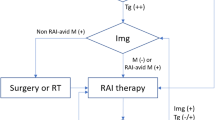
US showed very good sensitivity and specificity and a high negative predictive value for evaluation of loco-regional involvement in follow-up of pediatric differentiated thyroid cancer. Diagnostic whole-body iodine scan is indicated when serum anti-thyroglobulin Ab is high, or in cases of discordant findings between US and stimulated thyroglobulin levels, or when stimulated thyroglobulin levels are >10 ng/ml (to evaluate for lung metastasis).


Similar content being viewed by others
References
National Cancer Institute (2014) The survival, epidemiology, and end result program: SEER stats fact sheet: thyroid cancer. http://seer.cancer.gov/statfacts/html/thyro.html. Accessed 7 Nov 2014
Hogan AR, Zhuge Y, Perez EA et al (2009) Pediatric thyroid carcinoma: incidence and outcomes in 1,753 patients. J Surg Res 156:167–172
Davies L, Welch HG (2006) Increasing incidence of thyroid cancer in the United States, 1973–2002. JAMA 295:2164–2167
Hundahl SA, Fleming ID, Fremgen AM et al (1998) A national cancer database report on 53,856 cases of thyroid carcinoma treated in the U.S., 1985–1995. Cancer 83:2638–2648
Mazzaferri EL, Massoll N (2002) Management of papillary and follicular (differentiated) thyroid cancer: new paradigms using recombinant human thyrotropin. Endocr Relat Cancer 9:227–247
Jones MK (2002) Management of papillary and follicular thyroid cancer. J R Soc Med 95:325–326
Hay ID, Gonzalez-Losada T, Reinalda MS et al (2010) Long-term outcome in 215 children and adolescents with papillary thyroid cancer treated during 1940 through 2008. World J Surg 34:1192–1202
Parisi MT, Mankoff D (2007) Differentiated pediatric thyroid cancer: correlates with adult disease, controversies in treatment. Sem Nucl Med 37:340–356
Cooper DS, Doherty GM, Haugen BR et al (2009) Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
O’Gorman CS, Hamilton J, Rachmiel M et al (2010) Thyroid cancer in childhood: a retrospective review of childhood course. Thyroid 20:375–380
Ko MS, Lee JH, Shong YK et al (2010) Normal and abnormal sonographic findings at the thyroidectomy sites in postoperative patients with thyroid malignancy. AJR Am J Roentgenol 194:1596–1609
Torlontano M, Attard M, Crocetti U et al (2004) Follow-up of low risk patients with papillary thyroid cancer: role of neck ultrasonography in detecting lymph node metastases. J Clin Endocrinol Metab 89:3402–3407
Antonelli A, Miccoli P, Fallahi P et al (2003) Role of neck ultrasonography in the follow-up of children operated on for thyroid papillary cancer. Thyroid 13:479–484
Sohn YM, Kwak JY, Kim EK et al (2010) Diagnostic approach for evaluation of lymph node metastasis from thyroid cancer using ultrasound and fine-needle aspiration biopsy. AJR Am J Roentgenol 194:38–43
Leboulleux S, Girard E, Rose M et al (2007) Ultrasound criteria of malignancy for cervical lymph nodes in patients followed up for differentiated thyroid cancer. J Clin Endocrinol Metab 92:3590–3594
Cailleux AF, Baudin E, Travagli JP et al (2000) Is diagnostic iodine-131 scanning useful after total thyroid ablation for differentiated thyroid cancer? J Clin Endocrinol Metab 85:175–178
Lin JD, Chao TC, Hsueh C et al (2009) High recurrent rate of multicentric papillary thyroid carcinoma. Ann Surg Oncol 16:2609–2616
Cirocchi R, Trastulli S, Sanguinetti A et al (2011) Recurrent differentiated thyroid cancer: to cut or burn. World J Surg Oncol 9:89
Brassard M, Borget I, Edet-Sanson A et al (2011) Long-term follow-up of patients with papillary and follicular thyroid cancer: a prospective study on 715 patients. J Clin Endocrinol Metab 96:1352–1359
Collini P, Mattavelli F, Pellegrinelli A et al (2006) Papillary carcinoma of the thyroid gland of childhood and adolescence: morphologic subtypes, biologic behavior and prognosis: a clinicopathologic study of 42 sporadic cases treated at a single institution during a 30-year period. Am J Surg Pathol 30:1420–1426
Merrick Y, Hansen HS (1989) Thyroid cancer in children and adolescents in Denmark. Eur J Surg Oncol 15:49–53
Chow SM, Law SC, Mendenhall WM et al (2004) Differentiated thyroid carcinoma in childhood and adolescence—clinical course and role of radioiodine. Pediatr Blood Cancer 42:176–183
Newman KD, Black T, Heller G et al (1998) Differentiated thyroid cancer: determinants of disease progression in patients <21 years of age at diagnosis: a report from the Surgical Discipline Committee of the Children’s Cancer Group. Ann Surg 227:533–541
Zimmerman D, Hay ID, Gough IR et al (1988) Papillary thyroid carcinoma in children and adults: long-term follow-up of 1,039 patients conservatively treated at one institution during three decades. Surgery 104:1157–1166
Palmer BA, Zarroug AE, Poley RN et al (2005) Papillary thyroid carcinoma in children: risk factors and complications of disease recurrence. J Pediatr Surg 40:1284–1288
Choi JW, Lee JH, Baek JH et al (2010) Diagnostic accuracy of ultrasound and 18-F-FDG PET or PET/CT for patients with suspected recurrent papillary thyroid carcinoma. Ultrasound Med Biol 36:1608–1615
Park EK, Chung JK, Lim IH et al (2009) Recurrent/metastatic thyroid carcinomas false negative for serum thyroglobulin but positive by posttherapy I-131 whole body scans. Eur J Nucl Med Mol Imaging 36:172–179
Ma C, Kuang A, Xie J et al (2005) Possible explanations for patients with discordant findings of serum thyroglobulin and 131I whole-body scanning. J Nucl Med 46:1473–1480
Spencer C, Petrovic I, Fatemi S (2011) Current thyroglobulin autoantibody (TgAb) assays often fail to detect interfering TgAb that can result in the reporting of falsely low/undetectable serum Tg IMA values for patients with differentiated thyroid cancer. J Clin Endocrinol Metab 96:1283–1291
Siddiqi A, Foley RR, Britton KE et al (2001) The role of 123I-diagnostic imaging in the follow-up of patients with differentiated thyroid carcinoma as compared to 131I-scanning: avoidance of negative therapeutic uptake due to stunning. Clin Endocrinol 55:515–521
Brendel AJ, Lambert B, Guyot M et al (1990) Low levels of serum thyroglobulin after withdrawal of thyroid suppression therapy in the follow up of differentiated thyroid carcinoma. Eur J Nucl Med 16:35–38
Bachelot A, Cailleux AF, Klain M et al (2002) Relationship between tumor burden and serum thyroglobulin level in patients with papillary and follicular thyroid carcinoma. Thyroid 12:707–711
Torrens JI, Burch HB (2001) Serum thyroglobulin measurement. Utility in clinical practice. Endocrinol Metab Clin North Am 30:429–467
Acknowledgments
We thank Dr. Rahim Moineddin for providing statistical analysis and Dr. Lianna Kyriakopoulou for laboratory and thyroglobulin interpretation. The authors also thank the editor and reviewers of this manuscript for their insightful comments and suggestions.
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vali, R., Rachmiel, M., Hamilton, J. et al. The role of ultrasound in the follow-up of children with differentiated thyroid cancer. Pediatr Radiol 45, 1039–1045 (2015). https://doi.org/10.1007/s00247-014-3261-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-014-3261-0