Abstract
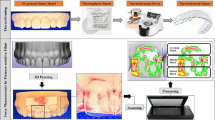
This in vitro study investigated the fracture behaviour of implant–implant-supported and implant–tooth-supported all-ceramic fixed dental prostheses (FDP) using zirconium dioxide implant abutments (FRIADENT® CERCON® abutments, DENTSPLY Friadent). Six different test groups (n = 8) were prepared. Groups 1, 2, 4, and 5 represented an implant–implant-supported FDP condition, whereas groups 3 and 6 simulated an implant–tooth-supported FDP condition. The second right premolar of the mandible was replaced with a pontic tooth. In groups 2 and 5, implant abutments were individualised by circumferential preparation. XiVe® S plus screw implants (DENTSPLY Friadent) that were 4.5 mm (first molar) and 3.8 mm (first premolar) in diameter and 11 mm in length and metal tooth analogues with simulated periodontal mobility, representing the first right premolar, were mounted in a polymethyl methacrylate block. The FDPs were cemented with KetacCem (3 M Espe GmbH, Germany). Groups 4, 5, and 6 were thermomechanically loaded (thermal and mechanical cycling (TCML) = 1.2 × 106; 10,000 × 5°/55°) and subjected to static loading until failure. Statistical analysis of data obtained for the force at fracture was performed using non-parametric tests. All samples tested survived TCML. In the implant–implant-supported groups, circumferential abutment preparation resulted in a tendency to lower fracture forces compared to groups with unprepared abutments (group 1, 472.75 ± 24.71 N; group 2, 423.75 ± 48.48 N; group 4, 647.13 ± 39.10 N; group 5, 555.86 ± 30.34 N). The implant–tooth-supported restorations exhibited higher fracture loads (group 3, 736.25 ± 82.23 N; group 6, 720.75 ± 48.99 N) than the implant–implant-supported restorations which did not possess circumferentially individualised abutments. Statistically significant differences were found when comparing the non-artificially aged groups. Implant–tooth-supported FDP restorations did exhibit an increased fracture load compared to implant–implant-supported FDP restorations.















Similar content being viewed by others
References
Barboza EP, Caula AL, Carvalho WR (2002) Crestal bone loss around submerged and exposed unloaded dental implants: a radiographic and microbiological descriptive study. Implant Dent 11:162–169
Misch CE, Dietsh-Misch F, Hoar J, Beck G, Hazen R, Misch CM (1999) A bone quality-based implant system: first year of prosthetic loading. J Oral Implantol 25:185–197
Abrahamsson I, Berglundh T, Lindhe J (1997) The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol 24:568–572
Welander M, Abrahamsson I, Berglundh T (2008) The mucosal barrier at implant abutments of different materials. Clin Oral Implants Res 19:635–641
Abrahamsson I, Berglundh T, Glantz PO, Lindhe J (1998) The mucosal attachment at different abutments. An experimental study in dogs. J Clin Periodontol 25:721–727
Watkin A, Kerstein RB (2008) Improving darkened anterior peri-implant tissue color with zirconia custom implant abutments. Compend Contin Educ Dent 29(238–240):242
Linkevicius T, Apse P (2008) Influence of abutment material on stability of peri-implant tissues: a systematic review. Int J Oral Maxillofac Implants 23:449–456
Degidi M, Artese L, Scarano A, Perrotti V, Gehrke P, Piattelli A (2006) Inflammatory infiltrate, microvessel density, nitric oxide synthase expression, vascular endothelial growth factor expression, and proliferative activity in peri-implant soft tissues around titanium and zirconium oxide healing caps. J Periodontol 77:73–80
Brodbeck U (2003) The ZiReal post: a new ceramic implant abutment. J Esthet Restor Dent 15:10–23 discussion 24
Butz F, Heydecke G, Okutan M, Strub JR (2005) Survival rate, fracture strength and failure mode of ceramic implant abutments after chewing simulation. J Oral Rehabil 32:838–843
Gehrke P, Dhom G, Brunner J, Wolf D, Degidi M, Piattelli A (2006) Zirconium implant abutments: fracture strength and influence of cyclic loading on retaining-screw loosening. Quintessence Int 37:19–26
Glauser R, Sailer I, Wohlwend A, Studer S, Schibli M, Scharer P (2004) Experimental zirconia abutments for implant-supported single-tooth restorations in esthetically demanding regions: 4-year results of a prospective clinical study. Int J Prosthodont 17:285–290
Kolbeck C, Behr M, Rosentritt M, Handel G (2008) Fracture force of tooth–tooth- and implant–tooth-supported all-ceramic fixed partial dentures using titanium vs. customised zirconia implant abutments. Clin Oral Implants Res 19:1049–1053
Andersson B, Glauser R, Maglione M, Taylor A (2003) Ceramic implant abutments for short-span FPDs: a prospective 5-year multicenter study. Int J Prosthodont 16:640–646
Zembic A, Sailer I, Jung RE, Hammerle CH (2009) Randomized-controlled clinical trial of customized zirconia and titanium implant abutments for single-tooth implants in canine and posterior regions: 3-year results. Clin Oral Implants Res 20:802-808
Sailer I, Zembic A, Jung RE, Siegenthaler D, Holderegger C, Hammerle CH (2009) Randomized controlled clinical trial of customized zirconia and titanium implant abutments for canine and posterior single-tooth implant reconstructions: preliminary results at 1year of function. Clin Oral Implants Res 20:219–225
Canullo L, Morgia P, Marinotti F (2007) Preliminary laboratory evaluation of bicomponent customized zirconia abutments. Int J Prosthodont 20:486–488
Att W, Kurun S, Gerds T, Strub JR (2006) Fracture resistance of single-tooth implant-supported all-ceramic restorations after exposure to the artificial mouth. J Oral Rehabil 33:380–386
Aramouni P, Zebouni E, Tashkandi E, Dib S, Salameh Z, Almas K (2008) Fracture resistance and failure location of zirconium and metallic implant abutments. J Contemp Dent Pract 9:41–48
Adatia ND, Bayne SC, Cooper LF, Thompson JY (2009) Fracture resistance of yttria-stabilized zirconia dental implant abutments. J Prosthodont 18:17–22
Yildirim M, Fischer H, Marx R, Edelhoff D (2003) In vivo fracture resistance of implant-supported all-ceramic restorations. J Prosthet Dent 90:325–331
Lawn BR, Pajares A, Zhang Y, Deng Y, Polack MA, Lloyd IK et al (2004) Materials design in the performance of all-ceramic crowns. Biomaterials 25:2885–2892
Ohlmann B, Marienburg K, Gabbert O, Hassel A, Gilde H, Rammelsberg P (2009) Fracture-load values of all-ceramic cantilevered FPDs with different framework designs. Int J Prosthodont 22:49–52
Ferrario VF, Sforza C, Serrao G, Dellavia C, Tartaglia GM (2004) Single tooth bite forces in healthy young adults. J Oral Rehabil 31:18–22
Nishigawa K, Bando E, Nakano M (2001) Quantitative study of bite force during sleep associated bruxism. J Oral Rehabil 28:485–491
Schwartz-Arad D, Samet N, Samet N (1999) Single tooth replacement of missing molars: a retrospective study of 78 implants. J Periodontol 70:449–454
Nickenig HJ, Schafer C, Spiekermann H (2006) Survival and complication rates of combined tooth–implant-supported fixed partial dentures. Clin Oral Implants Res 17:506–511
Gross M, Laufer BZ (1997) Splinting osseointegrated implants and natural teeth in rehabilitation of partially edentulous patients. Part I: laboratory and clinical studies. J Oral Rehabil 24:863–870
Laufer BZ, Gross M (1998) Splinting osseointegrated implants and natural teeth in rehabilitation of partially edentulous patients. Part II: principles and applications. J Oral Rehabil 25:69–80
Becker CM, Kaiser DA, Jones JD (2000) Guidelines for splinting implants. J Prosthet Dent 84:210–214
Lin CL, Wang JC (2003) Nonlinear finite element analysis of a splinted implant with various connectors and occlusal forces. Int J Oral Maxillofac Implants 18:331–340
Astrand P, Borg K, Gunne J, Olsson M (1991) Combination of natural teeth and osseointegrated implants as prosthesis abutments: a 2-year longitudinal study. Int J Oral Maxillofac Implants 6:305–312
Fugazzotto PA, Kirsch A, Ackermann KL, Neuendorff G (1999) Implant/tooth-connected restorations utilizing screw-fixed attachments: a survey of 3, 096 sites in function for 3 to 14years. Int J Oral Maxillofac Implants 14:819–823
Hosny M, Duyck J, van Steenberghe D, Naert I (2000) Within-subject comparison between connected and nonconnected tooth-to-implant fixed partial prostheses: up to 14-year follow-up study. Int J Prosthodont 13:340–346
Lindh T, Back T, Nystrom E, Gunne J (2001) Implant versus tooth-implant-supported prostheses in the posterior maxilla: a 2-year report. Clin Oral Implants Res 12:441–449
Pesun IJ (1997) Intrusion of teeth in the combination implant-to-natural-tooth fixed partial denture: a review of the theories. J Prosthodont 6:268–277
Nyman SR, Lang NP (1994) Tooth mobility and the biological rationale for splinting teeth. Periodontol 2000 4:15–22
Lin CL, Wang JC, Chang WJ (2008) Biomechanical interactions in tooth–implant-supported fixed partial dentures with variations in the number of splinted teeth and connector type: a finite element analysis. Clin Oral Implants Res 19:107–117
Pjetursson BE, Bragger U, Lang NP, Zwahlen M (2007) Comparison of survival and complication rates of tooth-supported fixed dental prostheses (FDPs) and implant-supported FDPs and single crowns (SCs). Clin Oral Implants Res 18(Suppl 3):97–113
Torbjorner A, Fransson B (2004) A literature review on the prosthetic treatment of structurally compromised teeth. Int J Prosthodont 17:369–376
Heydecke G, Butz F, Hussein A, Strub JR (2002) Fracture strength after dynamic loading of endodontically treated teeth restored with different post-and-core systems. J Prosthet Dent 87:438–445
Piconi C, Maccauro G (1999) Zirconia as a ceramic biomaterial. Biomaterials 20:1–25
Acknowledgements
The authors gratefully acknowledge Dentsply Friadent and DeguDent for contribution of materials, as well as MDT Martin Propson for his support in preparing the tested specimens.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nothdurft, F.P., Merker, S. & Pospiech, P.R. Fracture behaviour of implant–implant- and implant–tooth-supported all-ceramic fixed dental prostheses utilising zirconium dioxide implant abutments. Clin Oral Invest 15, 89–97 (2011). https://doi.org/10.1007/s00784-009-0359-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-009-0359-0