Abstract
Background
Obesity is a risk factor for colorectal cancer, and colonoscopy can be technically challenging in obese patients. It has been proposed (with little supporting data) that prone positioning of obese patients might facilitate a difficult colonoscopy.
Aim
The aim of this study was to determine if starting colonoscopy in the prone position for obese patients decreases cecal intubation times.
Methods
This was a prospective, randomized study conducted at the North Texas VA Medical Center. Patients with a body mass index of ≥30 kg/m2 undergoing elective colonoscopy were randomized 1:1 to either initial prone positioning or standard, left-lateral positioning. The outcome measurements were cecal intubation time, frequency of repositioning, sedative medications used, reports of pain, complications, and procedure tolerability.
Results
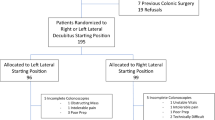
Fifty patients were randomized to have colonoscopy starting in the standard, left-lateral decubitus position, and 51 to the prone position. The average cecal intubation time for the standard group was 550 vs. 424 s in the prone group (p = 0.03). Patient repositioning was used in 28 % of patients in the standard group versus 8 % in the prone group (p = 0.009). There was no difference in subjective reports of pain between groups (p = 0.95) or in average pain scores (p = 0.79). Follow-up interviews were conducted in 93 % of patients, all of whom said that they would be willing to have repeat colonoscopy in the same position.
Conclusions
Performance of colonoscopy in the prone position for obese patients results in significantly shorter cecal intubation times and decreased need for patient repositioning. Prone positioning is well accepted and does not significantly increase procedure-related discomfort.

Similar content being viewed by others
References
Ogden CL, Carroll ME, Kit BK, et al. Prevalence of obesity in the United States, 2009–2010. NCHS Data Brief. 2012;82:1–8.
Moghaddam AA, Woodward M, Huxley R. Obesity and risk of colorectal cancer: a meta-analysis of 31 studies with 70,000 events. Cancer Epidemiol Biomarkers Prev. 2007;16:2533–2547.
Haggar FA, Boushey RP. Colorectal cancer epidemiology: incidence, mortality, survival, and risk factors. Clin Colon Rectal Surg. 2009;22:191–197.
Phillips KA, Liang SY, Ladabaum U, et al. Trends in colonoscopy for colorectal cancer screening. Med Care. 2007;45:160–167.
Schreiner MA, Fennerty MB. Endoscopy in the obese patient. Gastroenterol Clin N Am. 2010;39:87–97.
Borg BB, Gupta NK, Zukerman GR, et al. Impact of obesity on bowel preparation for colonoscopy. Clin Gastroenterol Hepatol. 2009;7:670–675.
Hansel SL, Prechel JA, Horn B, et al. Observational study of the frequency of use and perceived usefulness of ancillary maneuvers to facilitate colonoscopy completion. Dig Liv Dis. 2009;41:812–816.
Roberts-Thomson IC, Teo E. Colonoscopy: art or science? J Gastroenterol Hepatol. 2009;24:180–184.
Waye JD, Yessayan SA, Lewis BS, et al. The technique of abdominal pressure in total colonoscopy. Gastrointest Endosc. 1991;37:147–151.
Desormeaux M, Scicluna M, Friedland S. Colonoscopy in obese patients: a growing problem. Gastrointest Endosc. 2008;67:AB89.
De Silva AP, Kumarasena RS, Perera Keragala SD, et al. The prone 12 o’clock position reduces ileal intubation time during colonoscopy compared to the left lateral 6 o’clock (standard) position. BMC Gastroenterol. 2011;11:89.
Chutkan R. Colonoscopy issues related to women. Gastrointest Endoscopy Clin N Am. 2006;16:153–163.
Tishler PV, Larkin EK, Schluchter MD, et al. Incidence of sleep-disordered breathing in an urban adult population. JAMA. 2003;289:2230–2237.
Chung SA, Yuan H, Chung F. A systemic review of obstructive sleep apnea and its implications for anesthesiologists. Anesth Analg. 2008;107:1543–1563.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Uddin, F.S., Iqbal, R., Harford, W.V. et al. Prone Positioning of Obese Patients for Colonoscopy Results in Shortened Cecal Intubation Times: A Randomized Trial. Dig Dis Sci 58, 782–787 (2013). https://doi.org/10.1007/s10620-012-2468-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-012-2468-x