Abstract
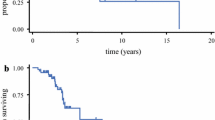
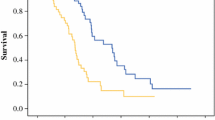
The extent of surgical resection (EOR) has been recorded as conditioning outcome in glioblastoma multiforme (GBM) patients but no significant improvements were recorded in survival. The study aimed to evaluate the impact of EOR on survival, investigating the role of fluid-attenuated inversion recovery (FLAIR) abnormalities removal. 282 newly diagnosed GBM patients were treated with surgery followed by concurrent and adjuvant chemo-radiotherapy. The EOR was defined as: SUPr, in case of resection amounting to 100% of enhanced and FLAIR areas; gross total (GTR) in case of resection between 90 and 100% of enhanced areas with variable amount of FLAIR abnormalities; sub-total (STR), between 10 and 89%; biopsy (B) <10%. FLAIR-RTV was dichotomized in percentage values to identify the best separation threshold for progression free survival (PFS) and overall survival (OS). SUPr was obtained in 21 patients (7.4%), GTR in 60 (21.3%), STR in 143 (50.7%) and biopsy only in 58 (20.6%). The median, 1, 2-year PFS were 10.4 ± 0.4 months, 39.0 ± 3.0, and 17.0 ± 2.0%; the median, 1, 2-year OS were 14.5 ± 0.5 months, 63.3 ± 3.0, and 23.1 ± 3.1%. EOR was significantly influencing survival (p < 0.001). The median, 1, 2-year OS were 28.6 ± 5.2 months, 90.0 ± 6.0, 71.0 ± 10.0% for patients underwent SUPr vs. 16.2 ± 1.2 months, 81.0 ± 5.0, 24.0 ± 6.0% for GTR. The FLAIR removal threshold conditioning survival was 45%. Minor complications were recorded in 14 (5%) patients and major in 8 (2.8%). surgical resection beyond contrast-enhancing boundaries could represent a promising strategy to improve outcome in GBM patients. The identification of a FLAIR-RTV threshold can be useful in clinical practice and it was recorded as factor influencing survival.


Similar content being viewed by others
References
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352(10):987–996
Johnson DR, O’Neill BP (2012) Glioblastoma survival in the United States before and during the temozolomide era. J Neurooncol 107(2):359–364
Wick W, Hartmann C, Engel C et al (2009) NOA-04 randomized phase III trial of sequential radiochemotherapy of anaplastic glioma with PCV or temozolomide. J Clin Oncol 27(35):5874–5880
Yamaguchi S, Kobayashi H, Terasaka S et al (2012) The Impact of Extent of Resection and Histological Subtype on the Outcome of Adult Patients with High-grade Gliomas. Jpn J Clin Oncol 42(4):270–277
Mc Girt MJ, Chaichana KL, Gathinji M et al (2009) Independent association of extent of resection with survival in patients with malignant brain astrocytoma. J Neurosur 110(1):156–162
Lamborn KR, Chang SM, Prados MD (2004) Prognostic factors for survival of patients with glioblastoma: recursive partitioning analysis. Neuro Oncol 6(3):227–235
Oppenlander ME, Wolf AB, Snyder LA et al (2014) An extent of resection threshold for recurrent glioblastoma and its risk for neurological morbidity. J Neurosurg 120(4):846–853
Chaichana KL, Jusue-Torres I, Navarro-Ramirez R et al (2014) Establishing percent resection and residual volume thresholds affecting survival and recurrence for patients with newly diagnosed intracranial glioblastoma. Neuro Oncol 16(1):113–122
Chaichana KL, Cabrera-Aldana EE, Jusue-Torres I et al (2014) When gross total resection of a glioblastoma is possible, how much resection should be achieved? World Neurosurg 82(1–2):257–265
Sanai N, Polley MY, McDermott MW, Parsa AT, Berger MS (2011) An extent of resection threshold for newly diagnosed glioblastomas. J Neurosurg 115(1):3–8
Li YM, Suki D, Hess K, Sawaya R (2016) The influence of maximum safe resection of glioblastoma on survival in 1229 patients: Can we do better than gross-total resection? J Neurosurg 124(4):977–988
Duffau H (2014) Is supratotal resection of glioblastoma in noneloquent areas possible? World Neurosurg 82(1–2):101–103
Wilson TA, Karajannis MA, Harter DH (2014) Glioblastoma multiforme: State of the art and future therapeutics. Surg Neurol Int 5:64
Yordanova YN, Moritz-Gasser S, Duffau H (2011) Awake surgery for WHO Grade II gliomas within “noneloquent” areas in the left dominant hemisphere: toward a “supratotal” resection. J Neurosurg 115(2):232–239
Bello L, Riva M, Fava E et al (2014) Tailoring neurophysiological strategies with clinical context enhances resection and safety and expands indications in gliomas involving motor pathways. Neuro Oncol 16(8):1110–1128
Sawaya R, Hammoud M, Schoppa D et al (1998) Neurosurgical outcomes in a modern series of 400 craniotomies for treatment of parenchymal tumors. Neurosurgery 42(5):1044–1055
Lacroix M, Abi-Said D, Fourney DR et al (2001) A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg 95(2):190–198
Sanai N, Berger MS (2008) Glioma extent of resection and its impact on patient outcome. Neurosurgery 62(4):753–766
Smith JS, Chang EF, Lamborn KR et al (2008) Role of extent of resection in the long-term outcome of low-grade hemispheric gliomas. J Clin Oncol 26(8):1338–1345
Chaichana KL, Jusue-Torres L, Navarro-Ramirez R et al (2014) Establishing percent resection and residual volume thresholds affecting survival and recurrence for patients with newly diagnosed intracranial glioblastoma. Neuro Oncol 16(1):113–122
Grabowski MM, Recinos PF, Nowacki AS et al (2014) Residual tumor volume versus extent of resection: predictors of survival after surgery for glioblastoma. J Neurosurg 121(5):1115–1123
Pessina F, Navarria P, Cozzi L et al (2016) Value of surgical resection in patients with newly diagnosed grade iii glioma treated in a multimodal approach: surgery, chemotherapy and radiotherapy. Ann Surg Oncol 23(9):3040–3046
Swanson KR, Rostomily RC, Alvord EC Jr (2008) A mathematical modelling tool for predicting survival of individual patients following resection of glioblastoma: a proof of principle. Br J Cancer 98(1):113–119
Swanson KR, Bridge C, Murray JD, Alvord EC Jr (2003) Virtual and real brain tumors: using mathematical modeling to quantify glioma growth and invasion. J Neurol Sci 216(1):1–10
Petrecca K, Guiot MC, Panet-Raymond V (2013) Failure pattern following complete resection plus radiotherapy and temozolomide is at the resection margin in patients with glioblastoma. J Neurooncol 111(1):19–23
Dobelbower MC, Burnet OL III, Nordal RA et al (2011) Patterns of failure for glioblastoma multiforme following concurrent radiation and temozolomide. J Med Imaging Radiat Oncol 55(1):77–81
McDonald MW, Shu HKS, Curran WJ Jr, Crocker IR (2011) Pattern of failure after limited radiotherapy and temozolomide for glioblastoma. Int J Radiat Oncol Biol Phys 79(1):130–136
Oh J, Sahgal A, Sanghera P et al (2011) Gliobastoma: patterns of recurrence and efficacy of salvage treatments. Can J Neurol Sci 38(4):621–625
Rahman M, Abbatematteo J, De Leo EK et al (2016) The effects of new or worsened postoperative neurological deficits on survival of patients with glioblastoma. J Neurosurg 30:1–9
Senft C, Bink A, Franz K et al (2011) Intraoperative MRI guidance and extent of resection in glioma surgery: a randomised, controlled trial. Lancet Oncol 12(11):997–1003
Pitter KL, Tamagno I, Alikhanyan K (2016) Corticosteroids compromise survival in glioblastoma. Brain 139(pt 5):1458–1471
Slotman BJ, Eppinga WS, Reijneveld JC et al (2009) Impact of extent of resection of glioblastoma multiforme (GBM) in the era of chemoradiation. J Clin Oncol 27:e13029
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
L. Cozzi acts as Scientific Advisor to Varian Medical Systems and is Clinical Research Scientist at Humanitas Cancer Center. All other co-authors have no conflicts of interest. No other conflict or source should be disclosed.
Rights and permissions
About this article
Cite this article
Pessina, F., Navarria, P., Cozzi, L. et al. Maximize surgical resection beyond contrast-enhancing boundaries in newly diagnosed glioblastoma multiforme: is it useful and safe? A single institution retrospective experience. J Neurooncol 135, 129–139 (2017). https://doi.org/10.1007/s11060-017-2559-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-017-2559-9