Abstract
Background
Atrial fibrillation (AF) is a major risk factor for stroke. Cost-effectiveness studies of anticoagulants for stroke prevention in AF rarely utilise AF-stroke-specific cost data in their analyses, as data are limited. Data that exist do not account for AF found on prolonged cardiac monitoring after stroke, further underestimating the clinical and economic burden of AF-stroke.
Objective
Our objective was to investigate differences in direct medical costs of acute stroke care among patients with and without AF.
Methods
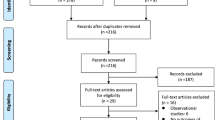
Data were prospectively collected from 213 consecutive patients with confirmed stroke (196 ischaemic [IS], 17 intracranial haemorrhage [ICH]), admitted to a UK district general hospital between November 2011 and October 2012. Sociodemographic, clinical and cardiac monitoring characteristics were recorded, and resource use was calculated using a ‘bottom-up’ approach. Univariate and multivariate stepwise regressions were performed to identify predictors of direct cost.
Results
Among patients with IS, 73 had AF (37 %). These patients were older, experienced greater stroke severity, lengths of hospitalisation, inpatient mortality and discharge to institutionalised care than those without AF. Mean acute care costs for the year 2012 were £6,978 (standard deviation [SD] 6,769, range 510–36,952). Mean (SD) costs were significantly higher for patients with AF than for those without (£9,083 [7,381] vs. £5,729 [6,071], p = <0.001). AF independently predicted acute care cost along with history of heart failure and stroke severity. The adjusted independent effect of having AF on costs was an additional £2,173 (95 % confidence interval 91–4,254; p = 0.041). Costs for patients with an ICH did not differ according to cardiac rhythm.
Conclusion
Direct medical costs of acute stroke care for patients with AF may be 50 % greater than for patients without. Economic studies should take this into account to ensure the benefits of anticoagulants are not underestimated.
Similar content being viewed by others
References
Stroke Association. Available at: http://www.strokecenter.org/patients/about-stroke/stroke-statistics. Accessed July 2014.
Saka O, McGuire A, Wolfe C. Cost of stroke in the United Kingdom. Age Ageing. 2009;38(1):27–32.
Singer D, Albers G, Dalen J, Go A, Helperin J, Manning W. Antithrombotic therapy in atrial fibrillation: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126(S3):429S–56S.
Hannon N, Sheehan O, Kelly L, Marnane M, Merwick A, Moore A, Kyne L, Duggan J, Moroney J, McCormack P, Daly L, Fitz-Simon N, Harris D, Horgan G, Williams E, Furie K, Kelly P. Stroke associated with atrial fibrillation—incidence and early outcomes in the North Dublin population stroke study. Cerebrovasc Dis. 2010;29:43–9.
Hart R, Pearce L, Aguilar M. Meta-analysis: antithrombotic therapy to prevent stroke in patients who have non-valvular atrial fibrillation. Ann Intern Med. 2007;146:857–67.
Ruff C, Guigliano R, Braunwald E, et al. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a metanalysis of randomised trials. Lancet. 2014;383:955–62.
Freeman J, Zhu R, Owens D, Garber A, Hutton D, Go A, Wang P, Turakhla M. Cost-effectiveness of dabigatran compared with warfarin for stroke prevention in atrial fibrillation. Ann Intern Med. 2011;154:1–11.
Edwards S, Hamilton V, Nherera L, Trevor N, Barton S. Rivaroxaban for the prevention of stroke and systemic embolism in people with atrial fibrillation: a single Technology Appraisal. London: BMJ-TAG; 2011.
Gonzalez-Juanatey J, Alvarez-Sabin J, Lobos J, Martinez-rubio A, Reverter J, Oyaguez I, Gonzalez-Rojas N, Becerra V. Cost-effectiveness of dabigatran for stroke prevention in non-valvular atrial fibrillation in Spain. Rev Esp Cardiol. 2012;65:901–10.
Kansal A, Sharma M, Bradley-Kennedy C, Clemens A, Monz B, Peng S, Roskell N, Sorensen S. Dabigatran versus rivaroxaban for the prevention of stroke and systematic embolism in atrial fibrillation in Canada. Comparative efficacy and cost-effectiveness. Thromb Haemost. 2012;108:672–82.
Kamel H, Johnston S, Easton J, Kim A. Cost-effectiveness of dabigatran compared with warfarin for stroke prevention in patients with atrial fibrillation and prior stroke or transient ischaemic attack. Stroke. 2012;43:881–3.
Lee S, Anglade M, Meng J, Hagstrom K, Kluger J. Cost-effectiveness of apixaban compared with aspirin for stroke prevention in atrial fibrillation among patients unsuitable for warfarin. Circ Cardiovasc Qual Outcomes. 2012;5:472–9.
Lee S, Anglade M, Piscane R, Kluger J, Coleman C. Cost-effectiveness of rivaroxaban compared to warfarin for stroke prevention in atrial fibrillation. Am J Cardiol. 2012;110:845–51.
Lee S, Mullikn R, Blazawski J, Coleman C. Cost-effectiveness of apixaban compared with warfarin for stroke prevention in atrial fibrillation. Plos One. 2012;7:e47473.
National Institute of Clinical Excellence. Dabigatran etixilate for the prevention of stroke and systemic embolism in atrial fibrillation. 2012. Available at: http://www.nice.org.uk/guidance/ta249/resources/guidance-dabigatran-etexilate-for-the-prevention-of-stroke-and-systemic-embolism-in-atrial-fibrillation-pdf. Accessed Nov 2014.
National Institute of Clinical Excellence. Rivaroxaban for the prevention of stroke and systemic embolism in atrial fibrillation. 2012. Available at: http://www.nice.org.uk/guidance/ta256/resources/guidance-rivaroxaban-for-the-prevention-of-stroke-and-systemic-embolism-in-people-with-atrial-fibrillation-pdf. Accessed Nov 2014.
Lin H, Wolf P, Kelly-Hayes M, Beiser A, Kase C, Benjamin E, D’Agostino R. Stroke severity in atrial fibrillation. The Framingham Study. Stroke. 1996;27:1760–4.
Saxena R, Lewis S, Berge E, Sandercock P, Coastal P. Risk of early death and recurrent stroke and effect of heparin in 3,169 patients with acute ischaemic stroke and atrial fibrillation in the International Stroke Trial. Stroke. 2001;32(10):2333–7.
Jorgensen H, Nakayama H, Reith J, Raaschou H, Olsen T. Acute stroke with atrial fibrillation. The Copenhagen Stroke Study. Stroke. 1996;27:1765–9.
Bruggenjurgen B, Rossnagel K, Roll S, Andersson F, Selim D, Muller-Nordhorn J, Nolte C, Jungehulsing G, Villringer A, Willisch S. The impact of atrial fibrillation on the cost of stroke: The Berlin Acute Stroke Study. Value Health. 2007;10:137–43.
Ghatnekar O, Glader E. The effect of atrial fibrillation on stroke—related inpatient costs in Sweden: a 3-year analysis of registry data from 2001. Value Health. 2008;11:862–8.
Department of Health. NHS reference costs 2011–2012. Available at: https://www.gov.uk/government/publications/nhs-reference-costs-financial-year-2011-to-2012. Accessed July 2012.
Curtis L, Netten A. Unit costs of health and social care. Canterbury: Personal Social Services Research Unit; 2012. Available at: http://www.pssru.ac.uk/project-pages/unit-costs/2012/. Accessed July 2012.
British National Formulary 61, 2011. Available at: http://www.bnf.org. Accessed Nov 2012 to Oct 2013.
Rotherham General Hospital Foundation Trust: private patient list tariff; 2012.
Qureshi H, Lowe D, Dobson P, Grant-Casey J, Parris E, Dalton D, Hickling K, Waller F, Howell C, Murphy M. National comparative audit of the use of platelet transfusions in the UK. Transfus Clin Biol. 2007;14:509–13.
Pamphilon D, Griffin C, Gerrard R, Neuberger J, Norfolk D, Richardson P, Rooney P, Webster R. Blood and transplant matters. Information for hospitals served by the NHS Blood and Transplant. NHS Blood and Transplant, 2011, Issue 34. Available at: http://www.blood.co.uk/pdf/publications/blood_matters_34.pdf. Accessed Oct 2012.
Luengo-Fernandez R, Gray A, Rothwell P. Population-based study of determinants of initial secondary care costs of acute stroke in the United Kingdom. Stroke. 2006;37:2579–87.
Arboix A, Alio J. Cardioembolic stroke: clinical features, specific cardiac disorders and prognosis. Curr Cardiol Rev. 2010;6:150–61.
Rosner B. Fundamentals of biostatistics. 7th ed. Boston: Brooks/Cole; 2011.
Briggs A, Gray A. The distribution of healthcare costs and their statistical analysis for economic evaluation. J Health Res Policy. 1998;3:233–45.
Afifi A, Kotlerman J, Ettner S, Cowan M. Methods for improving regression analysis for skewed continuous or counted responses. Annu Rev Public Health. 2007;28:95–111.
Diringer M, Edwards D, Mattson D, Akins P, Sheedy C, Hsu C, Dromerick A. Predictors of acute hospital costs for treatment of ischaemic stroke in an academic centre. Stroke. 1998;30:724–8.
Christensen L, Krieger D, Hojberg S, Pedersen O, Karlsen F, Jacobsen M, Worck R, Nielsen H, Aegidius K, Jeppesen L, Rosenbaum S, Marstrand J, Christensen H. Paroxysmal atrial fibrillation occurs in cryptogenic ischaemic stroke. Final results from the SURPRISE study. Eur J Neurol. 2014;21:884–9.
Acknowledgments
Neither the data nor the models or methodology within the study are proprietary. No financial support for this study was sought. Publication of the study is not contingent on any sponsor approval.
The authors acknowledge Jeanette Harris for help with data collection and Caroline Leggot from the finance department at Rotherham General Hospital. This study was completed without any funding support. No conflicts of interest existed for any of the named authors of this study.
Author contributions
Ms Joanne Howe undertook data collection and manuscript editing. Dr Ali Ali undertook study design, assisted in data collection, performed data analysis and manuscript writing and submission. Dr Abdel-Hafiz assisted in study design, data analysis and manuscript editing and acts as guarantor for the study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ali, A.N., Howe, J. & Abdel-Hafiz, A. Cost of Acute Stroke Care for Patients with Atrial Fibrillation Compared with Those in Sinus Rhythm. PharmacoEconomics 33, 511–520 (2015). https://doi.org/10.1007/s40273-015-0263-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-015-0263-1