Abstract
Purpose
To evaluate high-dose intravenous glucocorticoid treatment on tear inflammatory cytokines and ocular surface parameters in patients with active TED. Correlations between tear inflammatory cytokines and clinical parameters were also investigated.
Methods
This prospective pilot study included 15 moderate-to-severe and active TED patients. Control group consist of 15 sex and age-matched healthy subjects. All TED patients were treated with high-dose intravenous methylprednisolone with cumulative dose of 4.5 g during the therapy subdivided into 12 weekly infusions. Tear concentrations of interleukin (IL)-1β, IL-6, IL-8, IL-10, IL-17A, tumor necrosis factor (TNF)-α, and vascular endothelial growth factor (VEGF) were measured by multiplex bead analysis in TED patients at baseline and 12 weeks after treatment. Ocular surface disease index (OSDI), tear break-up time (TBUT), corneal fluorescent staining, and Schirmer’s test were obtained from TED and controls.
Results
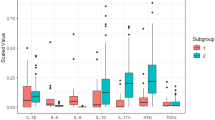
All baseline cytokine levels except for IL-17A were significantly elevated in active TED patients compared with controls. Concentrations of IL-1β, IL-6, IL-8, TNF-α, and VEGF were significantly decreased at 12 weeks compared with baseline. OSDI and TBUT showed significant improvement at 6 and 12 weeks. There were significant positive correlations between IL-6, IL-8, and CAS, and negative correlation was found between IL-6 level and TED duration before methylprednisolone treatment. The reduction of IL-6, IL-8, and VEGF were positive correlated with the reduction in CAS at 12 weeks.
Conclusions
High-dose glucocorticoids treatment improved ocular surface symptom, increased the tear film stability, and decreased tear inflammatory cytokines in active TED. The reduction of the inflammatory cytokines is consistent with the improvement of clinical parameters.





Similar content being viewed by others
References
Bruscolini A, Abbouda A, Locuratolo N, Restivo L, Trimboli P, Romanelli F (2015) Dry eye syndrome in non-exophthalmic Graves’ disease. Semin Ophthalmol 30(5–6):372–376. https://doi.org/10.3109/08820538.2013.874491
Versura P, Campos EC (2010) The ocular surface in thyroid diseases. Curr Opin Allergy Clin Immunol 10(5):486–492. https://doi.org/10.1097/ACI.0b013e32833e1749
Gilbard JP, Farris RL (1983) Ocular surface drying and tear film osmolarity in thyroid eye disease. Acta Ophthalmol (Copenh) 61(1):108–116
Gupta A, Sadeghi PB, Akpek EK (2009) Occult thyroid eye disease in patients presenting with dry eye symptoms. Am J Ophthalmol 147(5):919–923. https://doi.org/10.1016/j.ajo.2008.12.007
Eckstein AK, Finkenrath A, Heiligenhaus A, Renzing-Kohler K, Esser J, Kruger C, Quadbeck B, Steuhl KP, Gieseler RK (2004) Dry eye syndrome in thyroid-associated ophthalmopathy: lacrimal expression of TSH receptor suggests involvement of TSHR-specific autoantibodies. Acta Ophthalmol Scand 82(3 Pt 1):291–297. https://doi.org/10.1111/j.1395-3907.2004.00268.x
Villani E, Viola F, Sala R, Salvi M, Mapelli C, Curro N, Vannucchi G, Beck-Peccoz P, Ratiglia R (2010) Corneal involvement in Graves’ orbitopathy: an in vivo confocal study. Invest Ophthalmol Vis Sci 51(9):4574–4578. https://doi.org/10.1167/iovs.10-5380
Wu LQ, Mou P, Chen ZY, Cheng JW, Le QH, Cai JP, Wei RL (2019) Altered corneal nerves in Chinese thyroid-associated ophthalmopathy patients observed by in vivo confocal microscopy. Med Sci Monit Int Med J Exp Clin Res 25:1024–1031. https://doi.org/10.12659/MSM.912310
Xu N, Huang DP, Yang HS, Lai ZG, Luo Q (2012) Ocular surface characteristics and impression cytology in patients with active versus inactive thyroid eye disease. Eye Sci 27(2):64–68. https://doi.org/10.3969/j.issn.1000-4432.2012.02.003
Gurdal C, Sarac O, Genc I, Kirimlioglu H, Takmaz T, Can I (2011) Ocular surface and dry eye in Graves’ disease. Curr Eye Res 36(1):8–13. https://doi.org/10.3109/02713683.2010.526285
Wei YH, Chen WL, Hu FR, Liao SL (2015) In vivo confocal microscopy of bulbar conjunctiva in patients with Graves’ ophthalmopathy. J Formos Med Assoc Taiwan 114(10):965–972. https://doi.org/10.1016/j.jfma.2013.10.003
Wang CY, Ho RW, Fang PC, Yu HJ, Chien CC, Hsiao CC, Kuo MT (2018) The function and morphology of Meibomian glands in patients with thyroid eye disease: a preliminary study. BMC Ophthalmol 18(1):90. https://doi.org/10.1186/s12886-018-0763-9
Ujhelyi B, Gogolak P, Erdei A, Nagy V, Balazs E, Rajnavolgyi E, Berta A, Nagy EV (2012) Graves’ orbitopathy results in profound changes in tear composition: a study of plasminogen activator inhibitor-1 and seven cytokines. Thyroid 22(4):407–414. https://doi.org/10.1089/thy.2011.0248
Matheis N, Grus FH, Breitenfeld M, Knych I, Funke S, Pitz S, Ponto KA, Pfeiffer N, Kahaly GJ (2015) Proteomics differentiate between thyroid-associated orbitopathy and dry eye syndrome. Invest Ophthalmol Vis Sci 56(4):2649–2656. https://doi.org/10.1167/iovs.15-16699
Bahn RS (2010) Graves’ ophthalmopathy. N Engl J Med 362(8):726–738. https://doi.org/10.1056/NEJMra0905750
Shen J, Li Z, Li W, Ge Y, Xie M, Lv M, Fan Y, Chen Z, Zhao D, Han Y (2015) Th1, Th2, and Th17 cytokine involvement in thyroid associated ophthalmopathy. Dis Markers 2015:609593. https://doi.org/10.1155/2015/609593
Hiromatsu Y, Yang D, Bednarczuk T, Miyake I, Nonaka K, Inoue Y (2000) Cytokine profiles in eye muscle tissue and orbital fat tissue from patients with thyroid-associated ophthalmopathy. J Clin Endocrinol Metab 85(3):1194–1199. https://doi.org/10.1210/jcem.85.3.6433
Huang D, Xu N, Song Y, Wang P, Yang H (2012) Inflammatory cytokine profiles in the tears of thyroid-associated ophthalmopathy. Graefes Arch Clin Exp Ophthalmol 250(4):619–625. https://doi.org/10.1007/s00417-011-1863-x
Yang M, Chung Y, Lang S, Yawata N, Seah LL, Looi A (2018) The tear cytokine profile in patients with active Graves’ orbitopathy. Endocrine 59(2):402–409. https://doi.org/10.1007/s12020-017-1467-2
Kishazi E, Dor M, Eperon S, Oberic A, Turck N, Hamedani M (2018) Differential profiling of lacrimal cytokines in patients suffering from thyroid-associated orbitopathy. Sci Rep 8(1):10792. https://doi.org/10.1038/s41598-018-29113-2
Bartalena L, Baldeschi L, Boboridis K, Eckstein A, Kahaly GJ, Marcocci C, Perros P, Salvi M, Wiersinga WM, European Group on Graves O (2016) The 2016 European thyroid association/European group on Graves’ orbitopathy guidelines for the Management of Graves’ Orbitopathy. Eur Thyroid J 5(1):9–26. https://doi.org/10.1159/000443828
Bartley GB, Gorman CA (1995) Diagnostic criteria for Graves’ ophthalmopathy. Am J Ophthalmol 119(6):792–795
Mourits MP, Prummel MF, Wiersinga WM, Koornneef L (1997) Clinical activity score as a guide in the management of patients with Graves’ ophthalmopathy. Clin Endocrinol (Oxf) 47(1):9–14
Iskeleli G, Karakoc Y, Abdula A (2008) Tear film osmolarity in patients with thyroid ophthalmopathy. Jpn J Ophthalmol 52(4):323–326. https://doi.org/10.1007/s10384-008-0545-7
Khurana AK, Sunder S, Ahluwalia BK, Malhotra KC (1992) Tear film profile in Graves’ ophthalmopathy. Acta Ophthalmol (Copenh) 70(3):346–349
Novaes P, Diniz Grisolia AB, Smith TJ (2016) Update on thyroid-associated Ophthalmopathy with a special emphasis on the ocular surface. Clin Diabet Endocrinol 2:19. https://doi.org/10.1186/s40842-016-0037-5
Yoon JS, Choi SH, Lee JH, Lee SJ, Lee SY (2010) Ocular surface inflammation, and nerve growth factor level in tears in active thyroid-associated ophthalmopathy. Graefes Arch Clin Exp Ophthalmol 248(2):271–276. https://doi.org/10.1007/s00417-009-1215-2
Gurdal C, Genc I, Sarac O, Gonul I, Takmaz T, Can I (2010) Topical cyclosporine in thyroid orbitopathy-related dry eye: clinical findings, conjunctival epithelial apoptosis, and MMP-9 expression. Curr Eye Res 35(9):771–777. https://doi.org/10.3109/02713683.2010.490320
Nichols KK, Nichols JJ, Mitchell GL (2004) The lack of association between signs and symptoms in patients with dry eye disease. Cornea 23(8):762–770
Chen Q (2019) The expression of interleukin-15 and interleukin-17 in tears and orbital tissues of Graves ophthalmopathy patients. J Cell Biochem 120(4):6299–6303. https://doi.org/10.1002/jcb.27916
Mysliwiec J, Kretowski A, Topolska J, Siewko K, Jakubczyk D, Szelachowska M, Mikita A, Kinalska I (2001) Serum Th1 and Th2 profile cytokine level changes in patients with Graves’ ophthalmopathy treated with corticosteroids. Horm Metab Res 33(12):739–743. https://doi.org/10.1055/s-2001-19135
Mysliwiec J, Kretowski A, Szelachowska M, Topolska J, Mikita A, Kinalska I (2001) Serum L-selectin and ICAM-1 in patients with Graves’ ophthalmopathy during treatment with corticosteroids. Immunol Lett 78(3):123–126
Lacka K, Manuszewska E, Korczowska I, Lacki JK (2007) The effect of methylprednisolone pulse treatment on cytokine network in Graves ophthalmopathy. Curr Eye Res 32(3):291–297. https://doi.org/10.1080/02713680601186698
Matos K, Manso PG, Marback E, Furlanetto R, Alberti GN, Nose V (2008) Protein expression of VEGF, IGF-1 and FGF in retroocular connective tissues and clinical correlation in Graves’ ophthalmopathy. Arqu Bras Oftalmol 71(4):486–492
Gortz GE, Horstmann M, Aniol B, Reyes BD, Fandrey J, Eckstein A, Berchner-Pfannschmidt U (2016) Hypoxia-dependent HIF-1 activation impacts on tissue remodeling in Graves’ ophthalmopathy-implications for smoking. J Clin Endocrinol Metab 101(12):4834–4842. https://doi.org/10.1210/jc.2016-1279
Nowak M, Marek B, Karpe J, Kos-Kudla B, Sieminska L, Kajdaniuk D, Treszer M (2014) Serum concentration of VEGF and PDGF-AA in patients with active thyroid orbitopathy before and after immunosuppressive therapy. Exp Clin Endocrinol Diabet 122(10):582–586. https://doi.org/10.1055/s-0034-1383579
Iitaka M, Miura S, Yamanaka K, Kawasaki S, Kitahama S, Kawakami Y, Kakinuma S, Oosuga I, Wada S, Katayama S (1998) Increased serum vascular endothelial growth factor levels and intrathyroidal vascular area in patients with Graves’ disease and Hashimoto’s thyroiditis. J Clin Endocrinol Metab 83(11):3908–3912. https://doi.org/10.1210/jcem.83.11.5281
Mandic JJ, Kozmar A, Kusacic-Kuna S, Jazbec A, Mandic K, Mrazovac D, Vukojevic N (2018) The levels of 12 cytokines and growth factors in tears: hyperthyreosis vs euthyreosis. Graefe’s Arch Clin Exp Ophthalmol 256(4):845–852. https://doi.org/10.1007/s00417-017-3892-6
Cook EB, Stahl JL, Lowe L, Chen R, Morgan E, Wilson J, Varro R, Chan A, Graziano FM, Barney NP (2001) Simultaneous measurement of six cytokines in a single sample of human tears using microparticle-based flow cytometry. J Immunol Methods 254(1-2):109–118. https://doi.org/10.1016/s0022-1759(01)00407-0
Willems F, Marchant A, Delville JP, Gerard C, Delvaux A, Velu T, de Boer M, Goldman M (1994) Interleukin-10 inhibits B7 and intercellular adhesion molecule-1 expression on human monocytes. Eur J Immunol 24(4):1007–1009. https://doi.org/10.1002/eji.1830240435
Pawlowski P, Mysliwiec J, Mrugacz M, Zak J, Bakunowicz-Lazarczyk A, Rejdak R, Wysocka J, Gorska M (2014) Elevated percentage of HLA-DR(+) and ICAM-1(+) conjunctival epithelial cells in active Graves’ orbitopathy. Graefe’s Arch Clin Exp Ophthalmol 252(4):641–645. https://doi.org/10.1007/s00417-014-2580-z
Conti P, Kempuraj D, Kandere K, Di Gioacchino M, Barbacane RC, Castellani ML, Felaco M, Boucher W, Letourneau R, Theoharides TC (2003) IL-10, an inflammatory/inhibitory cytokine, but not always. Immunol Lett 86(2):123–129
Dias AC, Modulo CM, Jorge AG, Braz AM, Jordao AA Jr, Filho RB, de Paula JS, Rocha EM (2007) Influence of thyroid hormone on thyroid hormone receptor beta-1 expression and lacrimal gland and ocular surface morphology. Invest Ophthalmol Vis Sci 48(7):3038–3042. https://doi.org/10.1167/iovs.06-1309
Turck N, Eperon S, De Los Angeles Gracia M, Oberic A, Hamedani M (2018) Thyroid-associated orbitopathy and biomarkers: where we are and what we can hope for the future. Dis Markers 2018:7010196. https://doi.org/10.1155/2018/7010196
Huang D, Luo Q, Yang H, Mao Y (2014) Changes of lacrimal gland and tear inflammatory cytokines in thyroid-associated ophthalmopathy. Invest Ophthalmol Vis Sci 55(8):4935–4943. https://doi.org/10.1167/iovs.13-13704
Kahaly GJ, Shimony O, Gellman YN, Lytton SD, Eshkar-Sebban L, Rosenblum N, Refaeli E, Kassem S, Ilany J, Naor D (2011) Regulatory T-cells in Graves’ orbitopathy: baseline findings and immunomodulation by anti-T lymphocyte globulin. J Clin Endocrinol Metab 96(2):422–429. https://doi.org/10.1210/jc.2010-1424
Leszczynska A, Molins B, Fernandez E, Adan A, Ortiz-Perez S (2019) Cytokine production in thyroid eye disease: in vitro effects of dexamethasone and IL-6 blockade with tocilizumab. Graefe’s Arch Clin Exp Ophthalmol 5:4. https://doi.org/10.1007/s00417-019-04419-7
Acknowledgements
The authors thank Fayang Lian, a biostatistician from the Fujian Provincial Hospital, for giving us statistical consultation on this study.
Funding
This research was funded by the Fujian Provincial Natural Science Foundation (Grant Numbers 2018J01238; 2019J01152), the Joint Funds for the Innovation of Science and Technology of Fujian province (Grant Number 2018Y9035), the Startup Fund for Scientific Research of Fujian Medical University (Grant Number 2017XQ1022), and the Youth Foundation of Fujian Provincial Health Commission (Grant Number 2019-1-31).
Author information
Authors and Affiliations
Contributions
Conceptualization: NX and YC; Methodology: NX; Formal analysis and investigation: YC and DF; Writing—original draft preparation: NX; Writing—review and editing: YC and FS; Funding acquisition: NX and YC; Resources: YC, DF; Supervision: FS.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was carried out to appropriated ethical standards.
Informed consent
Informed consent was obtained from an individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xu, N., Cui, Y., Fu, D. et al. Tear inflammatory cytokines and ocular surface changes in patients with active thyroid eye disease treated with high-dose intravenous glucocorticoids. J Endocrinol Invest 43, 901–910 (2020). https://doi.org/10.1007/s40618-019-01174-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-019-01174-8