Abstract
Background
Locoregional recurrence rates after definitive chemoradiotherapy (dCRT) for locally advanced esophageal cancer (EC) are high. Salvage surgery (SALV) is considered the best treatment option in case of persistent or recurrent disease for operable patients, but SALV has been associated with increased morbidity and mortality. The aim of this study is to identify factors linked to outcomes after SALV to better select candidates and to optimize perioperative care.
Study Design
We retrospectively analyzed data from 308 consecutive SALV patients from a large multicenter European cohort. Univariate and multivariate analyses were performed to identify factors associated with in-hospital postoperative morbidity, anastomotic leakage (AL), and overall survival (OS).
Results
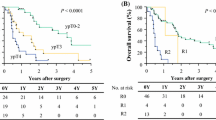
The in-hospital postoperative mortality and morbidity rates were 8.4 and 34.7%, respectively. Squamous cell histology (p = 0.040) and radiation dose ≥ 55 Gy (p = 0.047) were independently associated with major morbidity. The AL rate was 12.7%, and cervical anastomosis was independently associated with AL (p = 0.002). OS at 5 years was 34.0%. Radiation dose ≥ 55 Gy (p = 0.003), occurrence of postoperative complications (p = 0.006), ypTNM stage 3 (p = 0.019), and positive surgical margins (p < 0.001) were linked to poor prognosis.
Conclusions
SALV is a valuable option for patients with persistent or recurrent disease after dCRT and offers long-term survival. Factors such as radiation dose and anastomosis location identified here will help to optimize outcomes after SALV, which may be considered a standard treatment in the EC therapeutic armamentarium.
Similar content being viewed by others
References
Siegel R, DeSantis C, Virgo K, et al. Cancer treatment and survivorship statistics, 2012. CA Cancer J Clin. 2012;62:220–41.
Mariette C, Piessen G, Briez N, et al. Oesophagogastric junction adenocarcinoma: which therapeutic approach? Lancet Oncol. 2011;12:296–305.
Stahl M, Stuschke M, Lehmann N, et al. Chemoradiation with and without surgery in patients with locally advanced squamous cell carcinoma of the esophagus. J Clin Oncol. 2005;23:2310–17.
Bedenne L, Michel P, Bouche O, et al. Randomized phase III trial in locally advanced esophageal cancer: radiochemotherapy followed by surgery versus radiochemotherapy alone (FFCD 9102). J Clin Oncol. 2007;25:1160–8.
Stahl M, Mariette C, Haustermans K, et al. Oesophageal cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2013;24 Suppl 6:vi52–56.
Thésaurus National de Cancerologie Digestive. Société nationale française de gastroenterologie. Chapitre 1: Cancer de l’oesophage. http://www.tncd.org. Accessed 21 Aug 21 2015.
Gardner-Thorpe J, Hardwick R, Dwerryhouse S. Salvage esophagectomy after local failure of definitive chemoradiotherapy. Br J Surg. 2007;94:1059–66.
Jamel S, Markar S. Salvage esophagectomy: safe therapeutic strategy? J Thorac Dis. 2017;9:S799–808.
Rice TW. Esophageal nightmare: cancer recurrence after definitive chemoradiation. Is salvage esophagectomy possible? Semin Thorac Cardiovasc Surg. 2013;25:83–6.
Piessen G, Messager M, Mirabel X, et al. Is there a role for surgery for patients with a complete clinical response after chemoradiation for esophageal cancer? An intention to-treat case-control study. Ann Surg. 2013;258:793–9.
Mariette C, Piessen G, Briez N, Triboulet JP. The number of metastatic lymph nodes and the ratio between metastatic and examined lymph nodes are independent prognostic factors in esophageal cancer regardless of neoadjuvant chemoradiation or lymphadenectomy extent. Ann Surg. 2008;247:365–71.
Briez N, Piessen G, Bonnetain F, et al. Open versus laparoscopically-assisted oesophagectomy for cancer: a multicenter randomized controlled phase III trial-the MIRO trial. BMC Cancer. 2011;11:310.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Edge SB, Byrd DR, Compton CC, eds. AJCC Cancer Staging Manual. 7th ed. New York: Springer; 2010:103–115.
Akutsu Y, Kono T, Uesato M, et al. Is outcome of salvage surgery for T4 thoracic esophageal squamous cell carcinoma really poor? World J Surg. 2014;38:2891–7.
Borghesi S, Hawkins M, Tait D. Esophagectomy after definitive chemoradiation in patients with locally advanced esophageal cancer. Clin Oncol. 2008;20:221–6.
Yoo C, Park JH, Yoon DH, et al. Salvage esophagectomy for locoregional failure after chemoradiotherapy in patients with advanced esophageal cancer. Ann Thorac Surg. 2012;94:1862–8.
Chao YK, Chan SC, Chang HK, et al. Salvage surgery after failed chemoradiotherapy in squamous cell carcinoma of the esophagus. Eur J Surg Oncol. 2009;35:289–94.
Chen Y, Lu Y, Wang Y, et al. Comparison of salvage chemoradiation versus salvage surgery for recurrent esophageal squamous cell carcinoma after definitive radiochemotherapy or radiotherapy alone. Dis Esophagus. 2014;27:134–40.
D’Journo XB, Michelet P, Dahan L, et al. Indications and outcome of salvage surgery for esophageal cancer. Eur J Cardiothorac Surg. 2008;33:1117–23.
Farinella E, Safar A, Nasser H, et al. Salvage esophagectomy after failure of definitive radiochemotherapy for esophageal cancer. J Surg Oncol. 2016; 114:833–7.
Marks J, Hofstetter W, Correa A, et al. Salvage esophagectomy after failed definitive chemoradiation for esophageal adenocarcinoma. Ann Thorac Surg. 2012;94:1126–33.
Miyata R, Yamasaki M, Takiguchi S, et al. Salvage esophagectomy after definitive chemoradiotherapy for thoracic esophageal cancer. J Surg Oncol. 2009;100:442–6.
Morita M, Kumashiro R, Hisamatsu Y, et al. Clinical significance of salvage esophagectomy for remnant or recurrent cancer following definitive chemoradiotherapy. J Gastroenterol. 2011;46:1284–91.
Nakamura T, Hayashi K, Ota M, et al. Salvage esophagectomy after definitive chemotherapy and radiotherapy for advanced esophageal cancer. Am J Surg. 2004;188:261–6.
Oki E, Morita M, Kakeji Y, et al. Salvage esophagectomy after definitive chemoradiotherapy for esophageal cancer. Dis Esophagus. 2007;20:301–4.
Piessen G, Briez N, Triboulet JP, Mariette C. Patients with locally advanced esophageal carcinoma nonresponder to radiochemotherapy: who will benefit from surgery? Ann Surg Oncol. 2007;14:2036–44.
Pinto CE, de Souza Fernandes D, Moura Sà E, Mello ELR. Salvage esophagectomy after exclusive chemoradiotherapy: results at the Brazilian Cancer Institute. Dis Esophagus. 2009;22:682–6.
Schieman C, Wigle DA, Deschamps C, et al. Salvage resections for recurrent or persistent cancer of the proximal esophagus after chemoradiotherapy. Ann Thorac Surg. 2013;95:459–63.
Smithers BM, Cullinan M, Thomas JM, et al. Outcomes from salvage esophagectomy post definitive chemoradiotherapy compared with resection following preoperative neoadjuvant chemoradiotherapy. Dis Esophagus. 2007;20:471–7.
Sohda M, Kumakura Y, Saito H, et al. Clinical significance of salvage esophagectomy for patients with esophageal cancer and factors of influencing long-term survival. Anticancer Res. 2017;37:5045–51.
Swisher SG, Wynn P, Putnam JB, et al. Salvage esophagectomy for recurrent tumors after definitive chemotherapy and radiotherapy. J Thorac Cardiovasc Surg. 2002;123:175–83.
Tachimori Y, Kanamori N, Uemura N, et al. Salvage esophagectomy after high-dose chemoradiotherapy for esophageal squamous cell carcinoma. J Thorac Cardiovasc Surg. 2009;137:49–54.
Takeuchi H, Saikawa Y, Oyama T, et al. Factors influencing the long-term survival in patients with esophageal cancer who underwent esophagectomy after chemoradiotherapy. World J Surg. 2010;34:277–84.
Tomimaru Y, Yano M, Takachi K, et al. Factors affecting the prognosis of patients with esophageal cancer undergoing salvage surgery after definitive chemoradiotherapy. J Surg Oncol. 2006;93:422–8.
Wang S, Tachimori Y, Hokamura N, et al. Prognosis analysis of salvage esophagectomy following definitive chemoradiotherapy for esophageal squamous cell carcinoma: the importance of lymphadenectomy. J Thorac Cardiovasc Surg. 2014;147:1805–11.
Watanabe M, Mine S, Nishida K et al. Salavage esophagectomy after definitive chemoradiotherapy for patients with esophageal squamous cell carcinoma: who really benefits from this high risk surgery? Ann Surg Oncol. 2015;22:4438–44.
Ghaly G, Kamel M, Nasar A, et al. Locally advanced esophageal cancer: what becomes of 5-year survivors? J Thorac Cardiovasc Surg. 2016;151:726–32.
Gronnier C, Tréchot B, Duhamel A, et al. Impact of neoadjuvant chemoradiotherapy on postoperative outcomes after esophageal cancer resection: results of a European multicenter study. Ann Surg. 2014;260:764–70.
Minsky BD, Pajak TF, Ginsberg RJ, et al. INT 0123 (Radiation Therapy Oncology Group 94-05) phase III trial of combined-modality therapy for esophageal cancer: high-dose versus standard-dose radiation therapy. J Clin Oncol. 2002;20:1167–74.
NCCN esophageal cancer guidelines. http://www.nccn.org/professionals/physician_gls/pdf/esophageal.pdf. Accessed 20 Aug 2015.
Girard E, Messager M, Sauvanet A, et al. Anastomotic leakage after gastrointestinal surgery: diagnosis and management. J Visc Surg. 2014;151:441–50.
Markar S, Gronnier C, Duhamel A, et al. Salvage surgery after chemotherapy in the management of esophageal cancer: is it a viable therapeutic option? J Clin Oncol. 2015; 33:3866–73.
Vincent J, Mariette C, Pezet D, et al. Early surgery for failure after chemoradiation in operable thoracic oesophageal cancer. Analysis of the non-randomised patients in FFCD 9102 phase III trial: Chemoradiation followed by surgery versus chemoradiation alone. Eur J Cancer. 2015;51:1683–93.
Acknowledgment
Collaborators for the FREGAT (French Eso-Gastric Tumors working group) – FRENCH (Fédération de Recherche en Chirurgie) – AFC (Association Française de Chirurgie) Working Groups
Abdennahceur Dhahri, MD, PhD, Delphine Lignier, MD, Cyril Cossé, MD, Jean-Marc Regimbeau, MD, PhD, Department of Digestive Surgery, Amiens, France; Guillaume Luc, MD, Department of Digestive Surgery, Bordeaux, France; Magalie Cabau, MD, Jacques Jougon MD, PhD, Department of Thoracic Surgery, Bordeaux, France; Bogdan Badic, MD, Patrick Lozach, MD, Jean Pierre Bail, MD, Department of Digestive Surgery, Brest, France; Serge Cappeliez, MD, PhD, Issam El Nakadi, MD, PhD, Department of Digestive Surgery, Brussel ULB, Erasme Bordet University, Brussel, Belgium; Gil Lebreton, MD, Arnaud Alves, MD, PhD, Department of Digestive Surgery, Caen, France; Renaud Flamein, MD, Denis Pezet, MD, PhD, Department of Digestive Surgery, Clermont-Ferrand, France; Federica Pipitone, MD, Bogdan Stan-Iuga, MD, Nicolas Contival, MD, Eric Pappalardo, MD, Xaviera Coueffe, MD, Simon Msika, MD, PhD, Department of Digestive Surgery, Louis Mourier University Hospital, Colombes, France; Styliani Mantziari, MD, Nicolas Demartines, MD, Department of Digestive Surgery, Lausanne University Hospital, Lausanne, Switzerland; Flora Hec, MD, Marguerite Vanderbeken, MD, Nicolas Briez, MD, Department of Digestive Surgery, Lille, France; Fabien Fredon, MD, Alain Gainant, MD, Muriel Mathonnet, MD, PhD, Department of Digestive Surgery, Limoges, France; Jean Marc Bigourdan, MD, Salim Mezoughi, MD, Christian Ducerf, MD, Jacques Baulieux, MD, Jean-Yves Mabrut, MD, PhD, Department of Digestive Surgery, Croix Rousse University Hospital, Lyon, France; Oussama Baraket, MD, Gilles Poncet, MD, Mustapha Adam, MD, PhD, Department of Digestive Surgery, Edouard Herriot University Hospital, Lyon, France; Delphine Vaudoyer, MD, Peggy Jourdan Enfer, MD, Laurent Villeneuve, MD, Olivier Glehen, MD, PhD, Department of Digestive Surgery, Lyon Sud University Hospital, Lyon, France; Thibault Coste, MD, Jean-Michel Fabre, MD, Department of Digestive Surgery, Montpellier, France; Frédéric Marchal, MD, Department of Digestive Surgery, Institut de cancérologie de Lorraine, Nancy, France; Romain Frisoni, MD, Ahmet Ayav, MD, PhD, Laurent Brunaud, MD, PhD, Laurent Bresler, MD, Department of Digestive Surgery, Nancy, France; Olivier Aze, MD, Nicolas Venissac, MD, Daniel Pop, MD, Jérôme Mouroux, MD, Department of Thoracic Surgery, Nice, France; Ion Donici, MD, Michel Prudhomme, MD, PhD, Department of Digestive Surgery, Nîmes, France; Emanuele Felli, MD, Stéphanie Lisunfui, MD, Marie Seman, MD, Gaelle Godiris Petit, MD, Mehdi Karoui, MD, PhD, Christophe Tresallet, MD, PhD, Fabrice Ménégaux, MD, PhD, Jean-Christophe Vaillant, MD, Laurent Hannoun, MD, Department of Digestive Surgery, Pitié-Salpétrière University Hospital, Paris, France; Brice Malgras, MD, Denis Lantuas, MD, Karine Pautrat, MD, Marc Pocard, MD, PhD, Patrice Valleur, MD, Department of Digestive Surgery, Lariboisière University Hospital, Paris, France; Jérémie H Lefevre, MD, PhD, Najim Chafai, MD, Pierre Balladur, MD, Magalie Lefrançois, MD, Yann Parc, MD, PhD, François Paye, MD, PhD Emmanuel Tiret, MD Department of Digestive Surgery, Saint-Antoine University Hospital, Paris, France; Marius Nedelcu, MD, Letizia Laface, MD, Thierry Perniceni, MD, Brice Gayet, MD, Department of Digestive Surgery, Institut Mutualiste Montsouris, Paris, France; Kathleen Turner, MD, Department of Digestive Surgery, Rennes, France; Alexandre Filipello, MD, Jack Porcheron, MD, Olivier Tiffet, MD, PhD, Department of Digestive Surgery, Saint-Etienne, France; Noémie Kamlet, MD, Rodrigue Chemaly, MD, Amandine Klipfel, MD, Patrick Pessaux, MD, PhD, Cecile Brigand, MD, PhD, Serge Rohr MD, Department of Digestive Surgery, Strasbourg, France; Nicolas Carrère, MD, PhD, Department of Digestive Surgery, Toulouse, France; Chiara Da Re, MD, Frédéric Dumont, MD, Diane Goéré, MD, PhD, Dominique Elias, MD, Department of Digestive Surgery Institut Gustave-Roussy, Villejuif, France; Claude Bertrand, MD, Mont-Godinne University Hospital, Yvoir, Belgium.
Author Contribution
Study conception and design: Williams TESSIER and Christophe MARIETTE; Acquisition of data: All authors; Analysis and interpretation of data: Charlotte COHEN, Williams TESSIER, Caroline GRONNIER, Guillaume PIESSEN, and Christophe MARIETTE; Drafting of manuscript: Charlotte COHEN, Williams TESSIER, and Christophe MARIETTE; Critical revision: All authors.
Disclosure
None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Collaborators of the FREGAT (French Eso-Gastric Tumors working group) – FRENCH (Fédération de Recherche en Chirurgie) – AFC (Association Française de Chirurgie) Working Groups are listed in “Acknowledgment”.
Rights and permissions
About this article
Cite this article
Cohen, C., Tessier, W., Gronnier, C. et al. Salvage Surgery for Esophageal Cancer: How to Improve Outcomes?. Ann Surg Oncol 25, 1277–1286 (2018). https://doi.org/10.1245/s10434-018-6365-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-018-6365-1